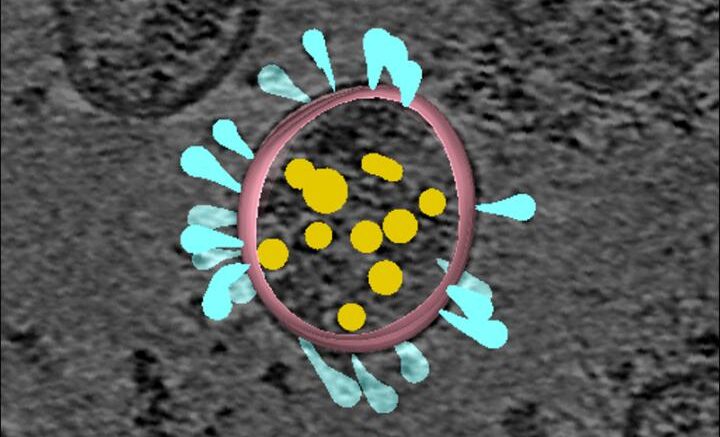
For their experiments determining how spike protein shapes change, Maolin Lu and colleagues used non-infectious corona-like viral particles. This image of those viruses shows the spike proteins colored in light blue. Courtesy of Wenwei Li.
The virus that causes COVID-19 belongs to the family of coronaviruses, "corona" referring to the spikes on the viral surface. These spikes are not static--to infect cells, they change shapes. Maolin Lu, an associate research scientist at Yale University, directly visualized the changing shapes of those spike proteins and monitored how the shapes change when COVID-19 patient antibodies attach. Her work, which was published in Cell Host & Microbe in December 2020 and will be presented at the 65th annual meeting of the Biophysical Society informs the development of COVID-19 vaccines and treatments that target the spikes of the SARS-CoV-2 virus, which causes COVID-19.
When the COVID-19 pandemic hit, Lu was quick to apply her expertise studying the HIV-1 virus to SARS-CoV-2. Prior to the pandemic, Lu studied which shapes of the HIV-1 spikes are most susceptible to antibody attack. Using similar techniques, in March 2020, she turned to SARS-CoV-2.
Because the spike proteins are prominent on the outside of the SARS-CoV-2 virus, they are crucial targets for vaccines and therapeutics. The vaccines that have been approved so far have been designed to help the body generate antibodies that recognize this part of the SARS-CoV-2 virus, blocking its entry into cells. However, Lu says, "the spike protein constantly changes shape, this shape-shifting feature not only allows the virus to enter host cells, it also helps the virus escape from being attacked or recognized by antibodies."
Using an imaging technique to monitor molecular movements, Lu observed that it adopts at least four shapes. She also watched how the spike proteins responded to serum from patients who recovered from COVID-19, which contained antibodies their body made against the SARS-CoV-2 virus. She noticed that some antibodies recognized and attached to the spike protein when it was in an "open" position and ready to stick to cells. Others preferred to attach to a "closed" spike, which is the spike's dominant position when the virus first enters the body.
"This indicates that antibodies can attack or antagonize the SARS-CoV-2 spike two different ways. One way is to directly occupy the spike's open position, then the virus cannot get close or associate with the host cells. The other way is to lock the spike into a closed position. The second locking down strategy has been widely used to develop COVID-19 vaccines," Lu explained.
When it comes to developing new vaccines or treatments, their research shows that targeting the SARS-CoV-2 spike protein when it is in a closed position may be a particularly effective strategy.
Be the first to comment on "Antibodies Recognize and Attack Different SARS-CoV-2 Spike Shapes"