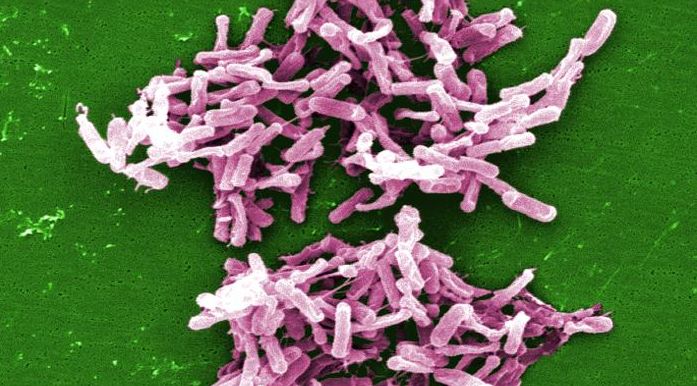
Under a magnification of 3006X, this digitally-colorized scanning electron microscopic (SEM) image depicts a large grouping of rod-shaped, Gram-positive Clostridium difficile bacteria. Courtesy of Janice Carr/CDC
Antibiotics are widely used by all specialties in the hospital setting. Tabak, et al. (2019) evaluated previously defined high-risk antibiotic use in relation to Clostridioides difficile infections (CDIs).
The researchers analyzed 2016–2017 data from 171 hospitals. High-risk antibiotics included second-, third-, and fourth-generation cephalosporins, fluoroquinolones, carbapenems, and lincosamides. A CDI case was a positive stool C. difficile toxin or molecular assay result from a patient without a positive result in the previous eight weeks. Hospital-associated (HA) CDI cases included specimens collected >3 calendar days after admission or ≤3 calendar days from a patient with a prior same-hospital discharge within 28 days. The researchers used the multivariable Poisson regression model to estimate the relative risk (RR) of high-risk antibiotic use on HA CDI, controlling for confounders.
The researchers report that the median days of therapy for high-risk antibiotic use was 241.2 (interquartile range [IQR], 192.6–295.2) per 1,000 days present; the overall HA CDI rate was 33 (IQR, 24–43) per 10,000 admissions. The overall correlation of high-risk antibiotic use and HA CDI was 0.22 (P = .003), and higher correlation was observed in teaching hospitals (0.38; P = .002). For every 100-day (per 1,000 days present) increase in high-risk antibiotic therapy, there was a 12% increase in HA CDI (RR, 1.12; 95% CI, 1.04–1.21; P = .002) after adjusting for confounders.
Tabak, et al. (2019) say their assessment of poststewardship implementation in the United States highlights the importance of tracking trends of antimicrobial use over time as it relates to CDI.
Reference: Tabak YP, et al. Hospital-level high-risk antibiotic use in relation to hospital-associated Clostridioides difficile infections: Retrospective analysis of 2016–2017 data from US hospitals. Published online by Cambridge University Press. Sept. 16, 2019. DOI: https://doi.org/10.1017/ice.2019.236
Be the first to comment on "High-Risk Antibiotic Use is an Independent Predictor of Hospital-Acquired CDI"