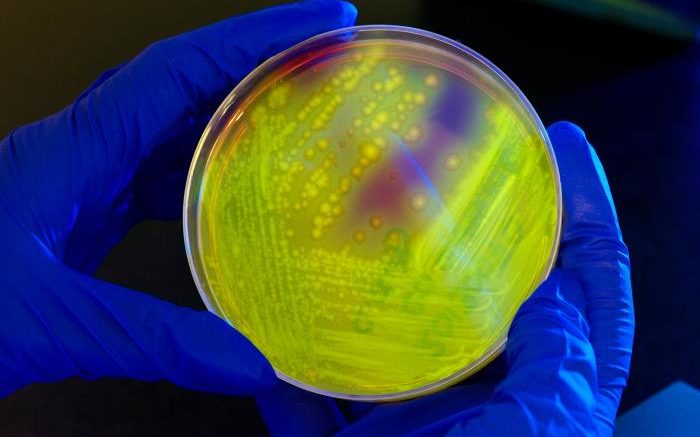
This Petri dish culture plate had contained cycloserine, cefoxitin, and fructose agar (CCFA), which had been inoculated with a Clostridium difficile bacterial culture, and had subsequently given rise to numerous bacterial colonies. In this particular view, the plate had been illuminated using long-wave UV irradiation, hence, the bacterial colonies emitted a yellow-green, or chartreuse fluorescent glow. Courtesy of CDC/ Melissa Dankel
Higher hospital-wide use of four classes of antibiotics thought to increase the risk of the dangerous intestinal illness Clostridioides difficile were associated with increased prevalence of hospital-associated C. difficile, according to a study published today in Infection Control & Hospital Epidemiology.
For every 100 days of facility-wide antibiotic therapy using one of these four antibiotics considered high risk, researchers found a 12 percent increase in hospital-associated C. difficile infection, though when analyzed separately only cephalosporins were significantly correlated with hospital-associated C. difficile.
C. difficile infections, which can cause life-threatening symptoms ranging from diarrhea to inflammation of the colon, affect nearly a half million patients in the United States each year causing approximately 15,000 deaths per year.
The lack of significant results for C. difficile for some classes of antibiotics may reflect reduced use through stewardship, the authors said.
"This highlights the importance of ongoing monitoring of antibiotic use in hospitals for patient safety as it relates to the effect of antibiotics on C. difficile infections. In the future it will also be important to look at the effect of antibiotic use on both C. difficile infection and antibiotic resistance simultaneously, rather than examining each piece as separate endeavors," said L. Clifford McDonald, MD, medical epidemiologist at the Centers for Disease Control and Prevention (CDC) and an author on the study.
"This is possible in our era of electronic medical records because antibiotic usage data has become more available. A facility can use the National Healthcare Safety Network Antibiotic Use and Resistance Module and interpret results using the standardized antibiotic administration ratio (SAAR) to have a better understanding of how antibiotics are being used and identify areas for improvement."
Recent guidelines identified the four classes of antibiotics examined in this study as high risk, though results of previous research evaluating facility-level use of these antibiotics and rates of C. difficile have been inconsistent. Researchers in this study analyzed microbiological and pharmacy data from 171 hospitals included in the BD Insights Research Database to look at the impact of hospital-wide use of these four classes of antibiotics on hospital-acquired C. difficile.
The four high-risk classes were cephalosporins (used for a wide variety of bacterial infections), fluoroquinolones (used for respiratory and urinary tract infections), carbapenems (broad spectrum antibiotics often reserved for unresponsive infections), and lincosamides (used against staph and strep infections).
Higher C. difficile infection rates were also associated with a larger portion of patients over age 65, higher rates of community-onset C. difficile, longer length of stay, and teaching hospitals.
Reference: Ying Tabak, Arjun Srinivasan, Kalvin Yu, Stephen Kurtz, Vikas Gupta, Steven Gelone, Patrick Scoble, L. Clifford McDonald. "Hospital-level High-risk Antibiotic Use in Relation to Hospital-associated Clostridioides difficile Infections: Retrospective Analysis of 2016-2017 Data from US Hospitals." Infection Control & Hospital Epidemiology. Web (September 16, 2019).
Source: Society for Healthcare Epidemiology of America (SHEA)
Be the first to comment on "Hospital-Wide Use of High-Risk Antibiotics Associated With More C. diff Infections"