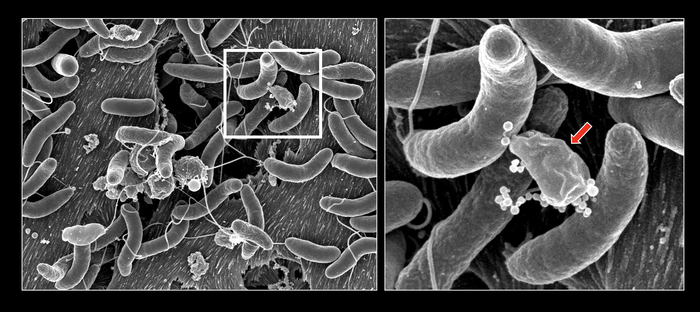
V. cholerae’s growth and competition on natural surfaces (left). The framed area is zoomed-in on the right and shows the killing of a bacterium (indicated by the red arrow) by the two V. cholerae cells. Courtesy of M. Blokesch & G. Knott (EPFL)
Cholera is still an enormous problem. An acute diarrheal disease, there have been seven major pandemics in the last two hundred years. According to the WHO, cholera still kills up to 143,000 people each year and infects up to 4 million others, mostly in poor or underdeveloped countries.
Cholera is caused by the bacterium Vibrio cholerae, a waterborne pathogen that infects the gut of humans when they drink contaminated water. Upon ingestion, Vibrio cholerae begins to colonize the gut’s inner surface, and releases a toxin upon the epithelial cells. The toxin disrupts the ionic balance across the gut’s walls, causing excretion of watery diarrhea. Severe cholera can lead to death due to severe dehydration.
But that’s not all that V. cholerae does. In 2015, researchers led by professor Melanie Blokesch at EPFL published a seminal paper showing that the bacterium uses a spring-loaded spear to stab neighboring bacteria and steal their DNA as it grows in its environmental habitat. This molecular spear known as the “type VI secretion system” or T6SS has previously been described to serve interbacterial competition. “Drinking contaminated water in cholera-endemic areas of the world is expected to contain competition-ready T6SS-active V. cholerae,” says Blokesch.
Previous studies have shown that intestinal pathogens need to interact with the bacteria of the gut microbiome in order to establish themselves in this environment. They do this using a variety of tactics, from competing for nutrients to all-out inter-bacterial warfare. Several studies have suggested that intestinal pathogens use their T6SS spear to clear the intestinal niche and foster their own settling.
But studying how V. cholerae interacts with the gut microbiome is difficult. Normally, scientists would develop a standardized adult animal model, but V. cholerae is notorious for colonizing adult animals relatively poorly compared to humans. This means that researchers have to resort to infant animals, but these lack the mature microbiome with which V. cholerae interacts as soon as it begins to colonize the intestine.
Meanwhile, many studies have shown that resisting colonization by V. cholerae and other infectious bacteria depends to a large extent on so called “commensal” microbes in the gut. Commensal microbes, and especially human gut ones, have not been researched much in terms of interaction with V. cholerae.
In a paper published in Nature Communications, Blokesch’s group has now looked at the way V. cholerae interacts with bacteria of the human microbiota. The scientists looked at a small collection of commensals from human volunteers, which included several bacterial species such as Escherichia coli, Enterobacter cloacae, and various Klebsiella isolates.
Their findings showed that although several species of gut bacteria are depleted following T6SS-mediated attacks by V. cholerae, a significant subset resist it. Specifically, some Klebsiella gut species shield themselves against the T6SS attacks of V. cholerae with a polysaccharide capsule that is characteristic of so-called “encapsulated” bacteria.
Because it is a highly efficient killing device, bacteria like V. cholerae that use T6SS also have ways to protect themselves to avoid self-intoxication. To do this, T6SS-using bacteria produce specific immunity proteins that block the toxic effects of the T6SS.
But the study found that some members of the human microbiota protect themselves from T6SS attacks without going the immunity-protein route. Specifically, the study showed that E. cloacae – itself an opportunistic pathogen – fights back by actually killing V. cholerae first with its own, superior, T6SS weaponry.
“This work provides us with some new insight into bacterial community behavior within the intestinal microbiota and how defense against T6SS intoxication might help bacterial populations to defend themselves against invading pathogens,” says Melanie Blokesch. But she also emphasizes that the study was carried out in vitro, meaning that additional studies are needed if we are to get a more complete picture.
“Nonetheless, our work could serve as a starting point to rationally design T6SS-shielded probiotic strains that are able to restore defective colonization barriers or enhance the barriers’ efficiency,” the authors conclude.
Lastly, Blokesch highlights the generosity of colleagues who shared bacterial strains for this study. She also emphasizes that reaching out into new directions, including Klebsiella biology, would have been much more difficult without the wonderful collaboration with Olaya Rendueles and Eduardo Rocha at the Institute Pasteur in Paris.
“Even more than the scientific message, what I enjoyed the most, was the collaborative aspect (inside and outside the lab) of the story,” agrees Nicolas Flaugnatti, a postdoc in the Blokesch group and first (shared) author of this study.