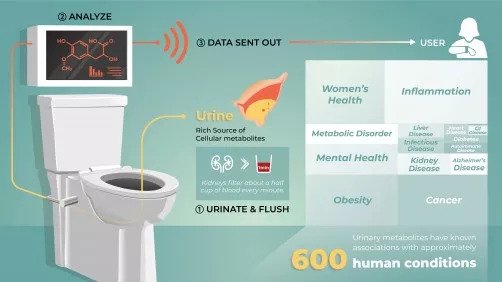
This graphic illustrates how an integrated "smart toilet" system might work as a real-time method of monitoring health. While the application may be years away, proof of principle is being developed in the lab of Professor Joshua Coon. Courtesy of Morgridge Institute for Research
Wearable, smart technologies are transforming the ability to monitor and improve health, but a decidedly low-tech commodity — the humble toilet — may have potential to outperform them all.
That’s the conclusion of a team of metabolism scientists at the University of Wisconsin-Madison and the Morgridge Institute for Research, who are working to put the tremendous range of metabolic health information contained in urine to work for personalized medicine.
Urine contains a virtual liquid history of an individual’s nutritional habits, exercise, medication use, sleep patterns and other lifestyle choices. Urine also contains metabolic links to more than 600 human conditions, including some of the major killers such as cancer, diabetes and kidney disease.
The team has two essential questions. First, can frequent monitoring and testing of urine samples glean useful real-time information about an individual’s health? And second, can a technology platform be adapted to toilets that can make the collection process simple, accurate and affordable?
They received some promising answers to the first question in a small pilot study conducted this year, the results of which were published in the Nov. 11 issue of the journal Nature Digital Medicine. Two research subjects consistently collected all urine samples over a 10-day period, submitted those samples for tests with both gas chromatography and mass spectrometry for a complete readout of metabolic signatures.
The two subjects also happen to be lead authors on the paper: Joshua Coon, the Thomas and Margaret Pyle Chair at the Morgridge Institute and UW-Madison professor of biomolecular chemistry and chemistry; and Ian Miller, data scientist with the Coon Research Group. Collectively they provided 110 samples over the 10-day period, and also used wearable technology to track heart rates and steps, calorie consumption and sleep patterns.
The results? The samples do indeed contain a remarkable health fingerprint that follows the ebbs and flows of daily life. For example, the subjects kept records of coffee and alcohol consumption, and the biomarkers with a known connection to both those drinks were abundantly measured. One subject took acetaminophen, which was measured in urine by a spike in ion intensity. The metabolic outputs from exercise and sleep also could be measured with precision.
The next step: The Coon Research Group is designing a toilet that will incorporate a portable mass spectrometer that can recognize the individual and process samples across a variety of subjects. They plan to install the toilet in their research building and expand the user group to a dozen or more subjects. Coon says the design is “a bit Rube Goldberg-like” but functional.
“We know in the lab we can make these measurements,” says Coon. “And we’re pretty sure we can design a toilet that could sample urine. I think the real challenge is we’re going to have to invest in engineering to make this instrument simple enough and cheap enough. That’s where this will either go far or not happen at all.”
While the pilot experiment didn’t examine health questions, many possibilities exist. For example, testing could show how an individual metabolizes certain types of prescription drugs, in ways that could be healthy or dangerous. Also, as the population gets older with more stay-at-home care, urine tests would indicate whether medications are being taken properly and having their intended effect.
Coon also believes the “smart toilet” concept could have major population health implications, not unlike the National Institutes of Health “All of Us” human genome database. “If you had tens of thousands of users and you could correlate that data with health and lifestyle, you could then start to have real diagnostic capabilities,” he says. It might provide early warning of viral or bacterial outbreaks.
Coon, who runs the National Center for Quantitative Biology of Complex Systems, says the idea of meta-scale urine testing has intrigued him for some time. “Josh mentioned this at a group meeting one time and it was met with laughter,” Miller recalls. “I thought, you know, I kind of like the idea. I already track a lot this stuff in my everyday life.”
Adds Coon: “So we went out and bought a couple coolers and started collecting.”
While the mass spec small-molecule analyses are being done on $300,000 machines, Coon says that portable mass spec technologies exist at a tenth of that cost. He says that with a market this massive, they could eventually hit a reasonable cost threshold.
“Almost every automobile on the road is more complicated than that portable mass spectrometer,” he says.
Source: Morgridge Institute for Research
Be the first to comment on "‘Smart Toilets’ Could be the Next Health Data Source"