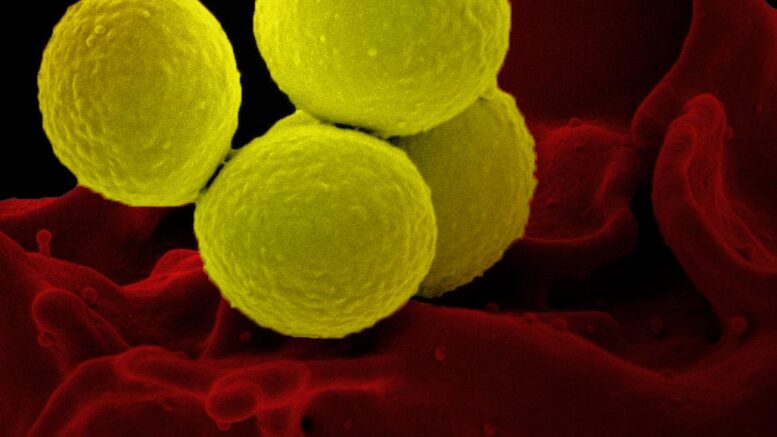
Scanning electron micrograph of a human neutrophil ingesting MRSA (yellow). Courtesy of NIAID
A clinical trial to test the antibiotic dalbavancin for safety and efficacy in treating complicated Staphylococcus aureus (S. aureus) bacteremia has begun. The trial will enroll 200 adults hospitalized with complicated S. aureus infection at approximately 20 trial sites around the United States. The trial is being sponsored by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health.
S. aureus is a leading cause of antibiotic-resistant infection. S. aureus infections led to nearly 20,000 deaths in 2017 in the United States, according to the Centers for Disease Control and Prevention (CDC). This bacterium is of particular concern in healthcare-associated infections. S. aureus bacteremia—an infection of the blood — often requires inserting a central intravenous (IV) catheter to deliver long courses of antibiotics, an invasive procedure that can involve long-term care in healthcare facilities.
“As antibiotic-resistant infections become more widespread, better and easier treatment regimens are needed to ease the burden on both healthcare providers and patients,” said NIAID director Anthony S. Fauci, MD. “By investigating existing antibiotics for their action on a broader array of bacterial infections, we may be able to generate new treatment regimens more efficiently.”
The antibiotic dalbavancin has strong activity against gram-positive bacteria, including methicillin-resistant S. aureus, which suggests it could be an effective treatment for S. aureus bacteremia. Dalbavancin is currently FDA-approved in the United States for treating acute bacterial skin and skin structure infections, including those caused by S. aureus. If the two-dose regimen being tested in this trial proves effective, it could lead to a shorter, less invasive treatment for S. aureus bacteremia that does not require an indwelling IV access for daily therapy.
The Phase 2b trial is being conducted by the NIAID-funded Antibacterial Resistance Leadership Group (ARLG)(link is external) under the leadership of Thomas Holland, MD, of Duke University. It is called the “Dalbavancin as an Option for Treatment of S. aureus Bacteremia (DOTS)” trial. Patients who have stabilized after initial treatment of their bacteremia will be eligible for enrollment in this study.
“Dalbavancin is appealing as a potential option for treatment of these serious S. aureus infections, and we need high quality data to find out if it works,” said Holland, “This trial will provide clinicians and patients with that data.”
One hundred participants will be randomized to receive the standard of care for complicated infections, including appropriate antibiotics, and 100 participants will receive two doses of dalbavancin intravenously. The doses will be given one week apart. Most participants receiving dalbavancin will be given 1500 milligrams (mg) per dose. Participants with signs of kidney dysfunction will be given 1125 mg per dose. All participants will be followed for approximately 70 days after enrollment, and up to six months if they have vertebral osteomyelitis, an infection of the vertebrae.
At the end of the trial, multiple patient outcomes will be assessed: survival; additional complications (such as relapse) or clinical failures; drug-related adverse events; and overall quality of life. The therapeutic regimen will have met the primary endpoint of the trial if participants who received dalbavancin fare better on these metrics than those who received the current standard of care. This trial could validate a dalbavancin regimen of only one dose a week for two weeks, compared to daily doses administered intravenously for four to six weeks with the current standard of care.
The ARLG is a clinical research consortium working to reduce the impact of antimicrobial resistance. It is funded through NIH grant UM1AI104681. For more information about this trial, visit ClinicalTrials.gov and search identifiers NCT04775953.
Source: National Institutes of Health (NIH)
Be the first to comment on "Trial of Existing Antibiotic for Treating Staphylococcus aureus Bacteremia Begins"