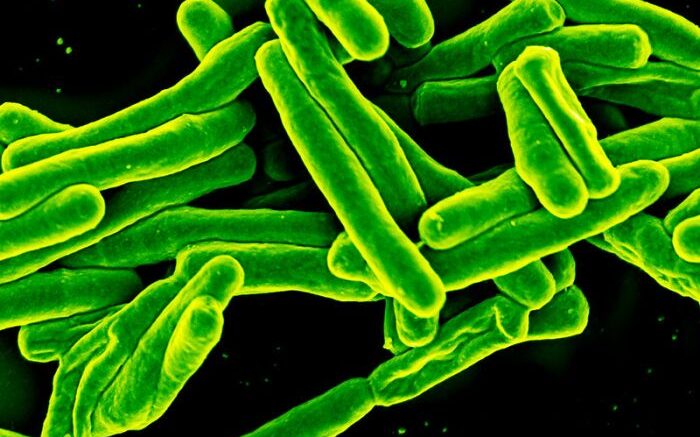
The ability of Mycobacterium tuberculosis (MTB), a serious respiratory infection, to form snake-like cords was first noted nearly 80 years ago. In a study published October 20 in the journal Cell, investigators report the biophysical mechanisms by which these cords form and demonstrate how several generations of dividing bacteria hang together to create these structures that enable resistance to antibiotics.
“Our work clearly showed that cord formation is important for infection and why this highly ordered architecture might be important for pathogenesis,” says senior author Vivek Thacker, who led the work at the Global Health Institute at École Polytechnique Fédérale de Lausannen (EPFL) in Switzerland and is now based at the Department of Infectious Diseases at Heidelberg University in Germany.
The study used a unique combination of technologies to address the role of MTB cord formation. One was a lung-on-chip model, which allowed the researchers to get a direct look at “first contact” between MTB and host cells at the air-liquid interface in the lungs. This revealed that cord formation is prominent in early infection. The researchers also used a mouse model that develops pathologies mimicking human tuberculosis, allowing them to obtain tissue that could be studied using confocal imaging and confirming that cording also occurs early in infection in vivo.
The work yielded several new findings about how these cords interact with and compress the cell nucleus, how this compression affects the immune system and connections between host cells and epithelial cells, and how cord formation affects the alveoli in the lungs. The study also revealed how these cords retain their structural integrity and how they increase tolerance to antibiotic therapy.
“There is an increasing understanding that these mechanical forces influence cellular behavior and responses, but this aspect has been overlooked since traditional cell culture models do not recapitulate the mechanical environment of a tissue,” says Melanie Hannebelle, formerly at EPFL’s Global Health Institute and now at Stanford University. “Understanding how forces at the cellular and tissue level or crowding at the molecular level affects cell and tissue function is therefore important to develop a complete picture of how biosystems work.”
“By thinking of MTB in infection as aggregates and not single bacteria, we can imagine new interactions with host proteins for known effectors of MTB pathogenesis and a new paradigm in pathogenesis where forces from bacterial architectures affect host function,” says Thacker.
Future research will focus on understanding whether cord formation enables new functionality to known effectors of MTB pathogenesis, many of which are located on the MTB cell wall. In addition, it will look at the consequence of tight-packing on the bacteria within the clump and how this may lead to a protective effect against antibiotics.
“Antibiotic therapy is the mainstay of treatment for tuberculosis infections, but therapeutic regimens are long and complicated, with an increasing threat of drug resistance,” says Richa Mishra, the other first author who is currently at EPFL’s Global Health Institute. “There is a recognized need for host-directed therapies or therapies that inhibit specific virulence mechanisms that can shorten and improve antibiotic therapy.”
Source: Cell Press