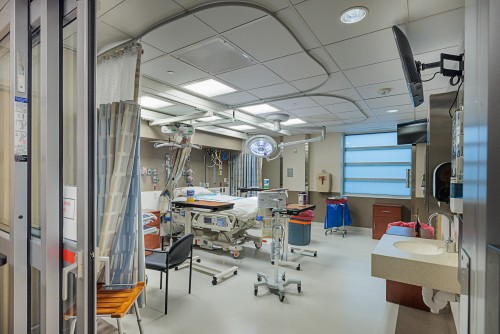
MedStar Washington Hospital Center has opened a state-of-the-art Biocontainment Unit (BCU) that will be used primarily for observation and flexed for respiratory isolation and further flexed to care for patients with highly infectious diseases – including quarantinable diseases such as cholera, diphtheria, infectious tuberculosis, plague, smallpox, yellow fever, viral hemorrhagic fevers (such as Marburg, Ebola, and Crimean-Congo), and severe acute respiratory syndromes.
Development and construction of the new unit with 15 beds have been seven years in the making. “In 2014, there was elevated national concern around Ebola Virus Disease (EVD). To prepare to meet our community’s needs, our plans included converting a large part of our emergency department (ED) into a temporary biocontainment unit, which is a pretty herculean task,” said Shane Kappler, MD, medical director of the newly dedicated Biocontainment Unit at MedStar Washington Hospital Center. “We knew that we needed to find a new way to provide the needed resources to care for these patients with special pathogens. And that is this new unit.”
Physically located adjacent to the hospital’s ED, the 6,800-square-foot space has 10 beds for respiratory isolation and two rooms specifically designated for biocontainment, with an anteroom between them. The anteroom is where team members remove the required personal protective equipment (PPE) they have used to provide patient care for a designated rotation period. The team and patients are continuously monitored by a protector outside the room watching through the glass and a safety officer on a live camera feed. Negative air pressure ensures that infectious particles don’t spread to the hallway or other parts of the hospital, preventing the spread of infection.
Construction of the Biocontainment Unit was supported with grants from the federal and state governments with overall funds supported by MedStar Health. In October 2022, the U.S. Department of Health and Human Services’ Administration for Strategic Preparedness and Response (ASPR) awarded MedStar Washington Hospital Center a $3 million grant to serve as a designated Regional Emerging Special Pathogen Treatment Center (RESPTC). It was one of three sites selected to expand beyond 10 existing RESPTC sites across the country.
“The $3 million ASPR grant provides funding to expand the volume and type of equipment we need to take care of more patients and supports our partnership with the other 12 regional special pathogens treatment centers,” said Craig DeAtley, PA-C, director of emergency preparedness and interim program director who will manage the BCU and grant funds at MedStar Washington Hospital Center. “We’ve become a referral center for FEMA Region 3, which includes Washington, D.C., Delaware, Maryland, Pennsylvania, Virginia, and West Virginia, and we’re partnering with Children’s National Hospital and Johns Hopkins to cover both pediatrics and adult patients.”
When not in use for biocontainment or respiratory isolation, the unit can be configured to observe up to 15 patients who need more extended periods of care than the ED can offer but are not sick enough to warrant inpatient admission. The space also has two special pathogen rooms where operations or labor and delivery procedures can be performed.
MedStar Health's significant investment in the unit underscores the system's commitment to improving and providing safe care for patients who contract pathogen illnesses and is an invaluable addition to MedStar Washington Hospital Center’s suite of existing services such as cardiology, cancer, trauma, and burns.
“This really puts us at the vanguard of health institutions in the U.S. Our Biocontainment Unit is another differentiator that allows us to serve our community and expand our regional and national readiness,” concluded Kappler.
MedStar Washington Hospital Center is part of the National Emerging Special Pathogens Training and Education Center or NETEC, where a consortium of hospitals experienced in treating special pathogens share lessons learned with goals of driving best practices, closing knowledge gaps, and developing innovative resources.
Source: MedStar Washington Hospital Center