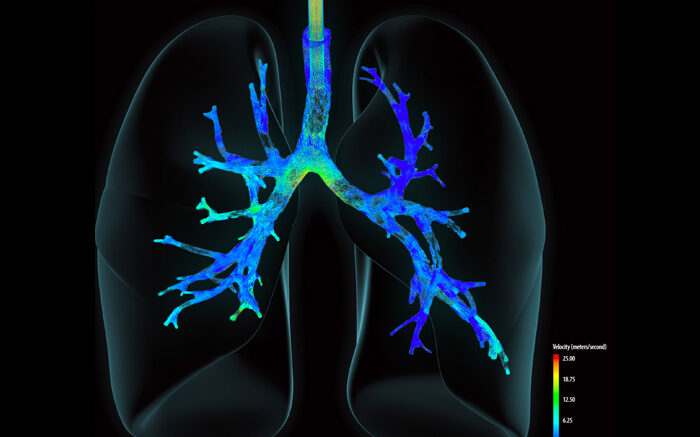
Mathematical visualization shows the velocity of air entering the lungs from a high-frequency pulsating ventilator. Courtesy of Los Alamos National Laboratory
Cross-disciplinary scientists and engineers at Los Alamos National Laboratory are working to learn how Intrapulmonary Percussive Ventilation (IPV) helps clear mucus from blocking the airways of the human lung, a common reaction to SARS-CoV-2.
Researchers, using some of the same modeling and experimental techniques from the Laboratory’s nuclear weapons mission, are working to discover the underlying science and engineering principles behind this process and have developed a preliminary machine learning algorithm that could someday assist pulmonary doctors in treating COVID-19 patients with IPV.
"People who have contracted the SARS-Cov2 virus may develop respiratory distress in which their lungs fill with mucus as a response to the viral infection. As the lungs fill with mucus, the person may ultimately require mechanical ventilation," said John Bernardin, principal investigator for the project in the Laboratory's Mechanical and Thermal Engineering group. "This project is investigating how IPV pulsations of fine aerosols may help clear mucus from the patient's lungs, help them breathe while on a ventilator, and ultimately help them recover from the disease."
IPV is used alongside traditional ventilation to deliver rapid pulses of aerosol, depositing medication and potentially opening up clogged airway passages in the lung. Researchers are merging numerical and experimental approaches to develop a predictive model of lung behavior under these conditions.
The lung is a highly complex system, so the Laboratory is using acoustic measurements, computational fluid dynamics models, structural-fluid interaction models, and optical techniques to model the breathing process and observe aerosol flow and mucus breakup. This is especially challenging because of the complex geometries in lung structure, multifaceted boundary conditions in the deep lung, and non-linear behavior of viscus fluids in the lung. The study requires analysis of how the lung responds to the kinetic energy of variable pressures, rotational flows, and sheer stresses on the lung walls.
To inform the mathematical models, the research team designed, built and tested several experimental devices, including a 3D printed "gas distribution manifold" that mimics the structures of the lung's trachea and bronchial branches. They used sensors to measure pressure, velocity, temperature and humidity, along with a gas analyzer to measure pressure and volume, optical sensors to detect aerosol density and spectrometers to look at particle size distribution. They also used lung tissue harvested from sheep carcasses and dyed aerosol to track the deposition of IPV aerosols during a ventilation-assisted process.
"We have learned that humidity has a strong effect on aerosol concentration," said Bernardin. "Dilution effects in the lung are less apparent with higher humidity, but more pronounced with increased volume flow rate, and aerosol penetration is much better during inhalation. We also discovered new mechanical dynamics and fluid mechanics (patent pending) that may further enhance the aerosol transport and mucus removal.”
The preliminary machine learning algorithm ties all the variables together, with the hope of eventually creating a rapid, patient-specific tool for estimating the proper ventilator and IPV settings for a particular patient before ventilation is begun, responding to and optimizing the treatment for each patient.
"The numerical modeling and experimentation tools required to study IPV are some of the same ones we use to design and test weapon systems, global security devices, and energy harvesting hardware," said Bernardin. "Through the development of new tools to fight COVID-19, we demonstrate first hand how our national laboratory's people and equipment can quickly adapt and overcome to solve a complex problem that threatens our very way of life."
This project is a partnership with Idaho and Sandia National Laboratories, Presbyterian Health Services, Percussionaire (maker of IPV), and several other national experts in infectious disease sciences. The project includes personnel from the Laboratory's Weapons Engineering, Biology, Theoretical, Weapons Modernization, Materials Physics and Applications, Computer, Computational and Statistical Sciences, and Physical Sciences organizations.
The project is funded by the U.S. Department of Energy – Office of Science through the CARES Act.
"The best part of this project was pulling together 20 people from all walks of life to respond to a challenging threat to the health and welfare of the world's population. We are fighting back against Covid-19, trying to find a way to save human lives, including those of our colleagues, friends, family, and people we will never know, what can be more rewarding than that?" said Bernardin.
Source: Los Alamos National Laboratory