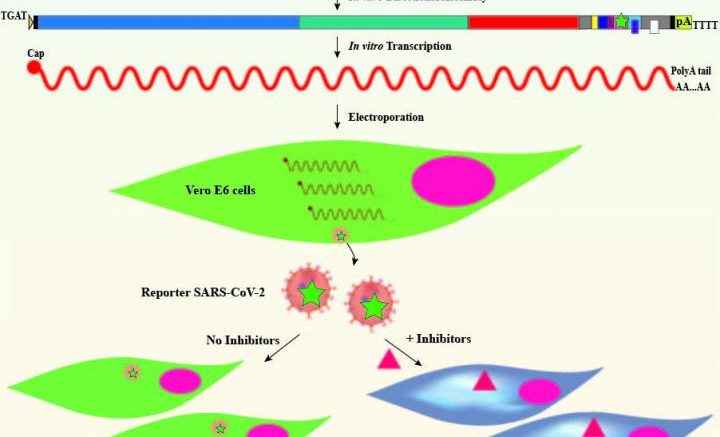
Graphic representation of the reverse genetic system for SARS-CoV-2. Courtesy of the University of Texas Medical Branch at Galveston
A multidisciplinary team at the University of Texas Medical Branch at Galveston working to combat the COVID-19 virus has a system that will unlock researchers' ability to more quickly develop and evaluate developing vaccines, diagnose infected patients and explore whether or how the virus has evolved.
The scientists, led by Pei-Yong Shi, developed the system by engineering a reverse genetic system for SARS coronavirus 2, or SARS-CoV-2, that is causing the current COVID-19 pandemic. The study is currently available in Cell Host & Microbe.
A Reverse genetic system is one of the most useful tools for studying and combatting viruses. The system allows researchers to make the virus in the lab and manipulate it in a petri dish. Using this system, the UTMB team has engineered a version of the SARS-CoV-2 virus that is labeled with neon green. When the labeled virus infects a cell, the infected cell turns green.
"The labeled virus could be used to rapidly determine whether a patient has already been infected by the new coronavirus or evaluate how well developing vaccines are inducing antibodies that block infection of the virus. The level of antibodies induced by a vaccine is the most important parameter in predicting how well a vaccine works," said Shi, I.H. Kempner professor of human genetics at UTMB. "The neon green labeled virus system allows us to test patients' samples in 12 hours in a high-throughput manner that tests many samples at once. In contrast, the conventional method can only test a few specimens at a time with a long turnaround time of a week."
"This technology can significantly reduce how long it takes to evaluate developing vaccines and ultimately bring them to the market," said Xuping Xie, the UTMB research scientist who designed and developed the genetic system. "UTMB will be very happy to make this technology widely available to both academia and industry researchers working to quickly develop countermeasures."
"The genetic system allows us to study the evolution of the new coronavirus. This will help us to understand how the virus jumped from its original host bat species to humans. It remains to be determined if an intermediate host is required for the host switch from the original bats to humans for the new coronavirus," said Vineet Menachery, assistant professor at UTMB, who co-senior-authored the study. "The system has provided a critical tool for the research community."
"This is another example of team science at UTMB," said Dr. Ben Raimer, president ad Interim of UTMB. "The collective effort from teams with complementary expertise worked together to deliver this exciting study. We will expand the team science to areas of clinical care and patient diagnosis by deploying the technology for serological testing."
Shi said, "This will not be the last emerging virus that plagues humanity. In the past two decades, we've seen other coronaviruses like SARS and MERS, as well as other viruses like Zika, Ebola and others. It's critically important to have a system that can be used for any new future or re-emerging viruses so that we can very quickly respond to the pathogens and protect peoples' health."
Other authors include UTMB's Antonio Muruato, Kumari Lokugamage, Krishna Narayanan, Xianwen Zhang, Jing Zou, Jianying Liu, Craig Schindewolf, Nathen Bopp, Patricia Aguilar, Kenneth Plante, Scott Weaver, Shinji Makino and James LeDuc.
To implement the technology for diagnosis and vaccine evaluation, the UTMB team has received grants from National Institutes of Health and philanthropic support from the Robert J. Kleberg, Jr. and Helen C. Kleberg Foundation; John S. Dunn Foundation; Amon G. Carter Foundation; Gillson Longenbaugh Foundation and the Summerfield G. Roberts Foundation.
522380 129223I got what you intend, saved to my bookmarks , quite decent web site . 389035