Most antibiotics are double-edged swords. Besides killing the pathogen they are prescribed for, they also decimate beneficial bacteria and change the composition of the gut microbiome. As a result, patients become more prone to reinfection, and drug-resistant strains are more likely to emerge.
The answer to this problem might be narrow-spectrum antibiotics that kill only one or a few species of bacteria, minimizing the risk of collateral damage. In a recent study, Rockefeller scientists took a close look at one such antibiotic, fidaxomicin, used to treat Clostridium difficile (C. diff), one of the most common healthcare-associated infections. The researchers demonstrated at a molecular level how fidaxomicin selectively targets C. diff while sparing the innocent bacterial bystanders.
The findings, detailed in Nature, might help scientists in the race to develop new narrow-spectrum antibiotics against other pathogens.
“I want people, scientists, and doctors to think differently about antibiotics,” says Elizabeth Campbell, a research associate professor at Rockefeller. “Since our microbiome is crucial to health, narrow-spectrum approaches have an important part to play in how we treat bacterial infections in the future.”
C. diff is a toxin-producing bacterium that can inflame the colon and cause severe diarrhea. It infects about half a million people in the United States, mostly in a hospital setting, and about one in 11 of those over age 65 who die within a month.
For years, doctors have used broad spectrum antibiotics to treat C. diff. Fidaxomicin is a relatively new alternative that was granted FDA approval in 2011.
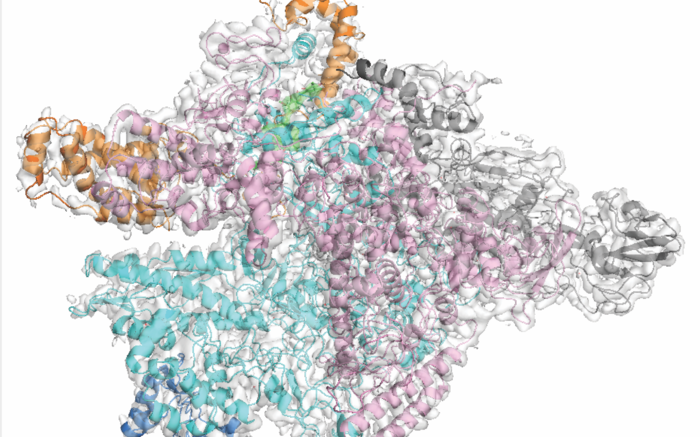
Like several other antibiotics including the tuberculosis drug rifampicin, fidaxomicin targets an enzyme called the RNA polymerase (RNAP), which the bacterium uses to transcribe its DNA code into RNA. To understand exactly why fidaxomicin selectively inhibits RNAP in C. diff and not in most other bacteria, Campbell teamed up with biochemist Robert Landick from the University of Wisconsin-Madison to visualize C. diff RNAP using cryo-electron microscopy, a powerful imaging technique that can reveal the 3D shape of molecules, and capture the drug molecule and its target in action. “Although the overall architecture of RNAP in diverse bacteria is similar, there are still considerable differences,” Campbell says.
One big challenge, however, was to first produce large amounts of C. diff, an anaerobic germ that doesn’t grow in the presence of oxygen. The study’s first author, Xinyun Cao, from the Landick Lab, spent two years developing a system to more easily produce C. diff RNAP using E. Coli, an easy growing bacterium frequently used in the lab.
Using this material, co-first author Hande Boyaci a postdoc on Campbell’s team generated images of C. diff RNAP locked with fidaxomicin at near-atomic resolution. Wedged into a hinge between two subunits of RNAP, fidaxomicin jams open the enzyme’s pincer, preventing it from grabbing on to genetic material and starting the transcription process.
In closely examining the points of contact between RNAP and fidaxomicin, the researchers identified one amino acid on the RNAP that binds to fidaxomicin but is absent in the main groups of gut microbes that are spared by fidaxomicin. A genetically altered version of C. diff that lacked this amino acid was unperturbed by fidaxomicin, just like other commensal bacteria in the gut. Conversely, bacteria that had it added to their RNAP became sensitive to fidaxomicin.
The findings suggest this one amino acid among the 4,000 amino acids of this robust and essential transcription machine is its Achilles heel, responsible for the killing of the bacteria by fidaxomicin.
The approach used in this study proposes a roadmap to developing new and safer antibiotics, the researchers say. By further elucidating RNAP structure of diverse bacteria, scientists can design antibiotics that targets each pathogen more selectively and effectively.
Source: Rockefeller University