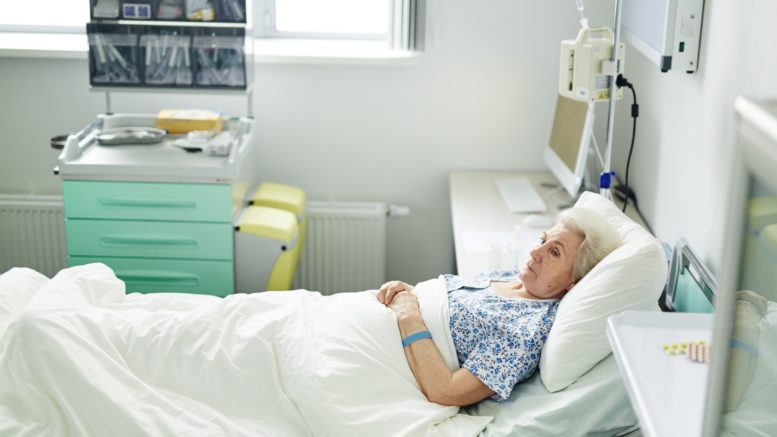
Trauma patients are at risk of developing multiple infections while in the hospital, but it's difficult to identify those who are especially susceptible. Now a team at Massachusetts General Hospital (MGH) has found that certain scores already used to assess the severity of a trauma patient's condition can provide clues. The findings are published in PLOS ONE.
In the researchers' analysis of information on 1,665 trauma patients, five of such "disease-severity" scores--called the Denver score, the Marshall score, the Acute Physiology and Chronic Health Evaluation II (APACHE II) score, the Injury Severity Score (ISS), and the New Injury Severity Score (NISS)--were examined as predictors of susceptibility to multiple independent infectious episodes. These scores differ in the way they assess a patient's condition by measuring physiologic responses or injury patterns.
The investigators found that the Denver and Marshall scores, which are used to assess the severity of organ failure in the setting of traumatic injury, can accurately predict susceptibility to multiple independent infections after trauma, even when the scores are determined much earlier than any clinical sign of infection.
"Our findings could potentially facilitate clinical decision-making by identifying patients who are at higher risk of suffering multiple infections during their hospital stay," said senior author Laurence G. Rahme, PhD, director of the MGH Molecular Surgical Laboratory, professor of surgery and microbiology at Harvard Medical School, and senior scientific staff at Shriners Hospital for Children.
"Early prognosis, before infections occur, could strategically guide the timing and duration of antibiotic administration to these patients," says Rahme, who is also an MGH Research Scholar 2020-2025. "It would also allow physicians to implement prophylactic measures, enhance patient nutrition, and formulate potent personalized treatment plans for this group of patients, thus protecting those at higher risk of repeated infections during their recovery period."
Rahme added that such personalized treatment plans could be cost-saving because they would limit interventions to only those patients most likely to develop infections, and they would help clinicians prevent hospital-acquired infections that can lead to prolonged hospital stays and the need for additional care.
Source: Massachusetts General Hospital
Thanks for the detailed guidance. More at carpintería de alumino A Coruña .
O que acharam da nova seção “Caça-Níquel da Semana” disponível na # anyKeyWord#! https://bolrank50.gumroad.com
I visited various blogs but the audio quality for audio songs present at this website is really superb.
Thanks for the comprehensive read. Find more at nutrióloga económica Saltillo .
Local enterprises can without a doubt thrive with robust on line marketing; your methods are gold! For additional systems, talk over with SEO professionals in Kansas City .
This was highly useful. For more, visit tienda cocinas Granada .
Thanks for the detailed post. Find more at best motor vehicle accident lawyer near me .
I’m impressed by way of your evaluation of recent cyber web layout gear. It’s good to see what’s a possibility! More files at Creative web design solutions .
Thanks for sharing these insights! Local corporations have to basically spend money on search engine optimisation. I came across full-size hints at Top-rated local SEO near me that helped my enterprise grow!
Appreciate the comprehensive advice. For more, visit ادمین اینستاگرام .
A nicely-designed set of custom equipped ins can particularly amendment how you use your house! Discover designs at custom built in closets .
Valuable information! Discover more at Aesthetic Plastic Surgery & Laser Centre .
It’s appropriate how plenty perception a ##couples therapist## can give all the way through tough instances. Glad to work out greater selections out there in Perth! Couples Therapist Perth
Thanks for the comprehensive read. Find more at Foothills maintenance experts .
เพิ่งเริ่มสนใจรถยนต์ เลยอยากรู้เรื่องไฟหน้ารถ LED ครับ หลอดไฟหน้า
Just done my hardscaping mission, and I can not think the change it made! Highly counsel reliable help for the wonderful results. hardscape design
These tips are excellent! For comprehensive dental care, head to Farnham Dentistry urgent dental care .
The weight of a Les Paul can be a lot, but that tone makes it worth it! Check out tips for handling it at Les Paul Pickup Upgrades .
Feeling thankful for the possibility to work with a educated ##marriage therapist## in Perth – it’s made this sort of change! Perth marriage counselor
Fascinating how user personas shape our approach to designing effective websites tailored specifically to our audience’s needs! Website design services near me
Great counsel on sustaining natural bushes; I’ll be calling a tree cutting carrier soon! licensed tree experts
“What’s the craziest taste mixture you’ve attempted due to your Nang Tank? Let’s swap principles! Nang Robot ”
#MovingTip: Always research your options! I found great reviews on Grand Prairie commercial movers .
The position of landscaping in growing assets magnitude is staggering! Learn extra about it at landscape design .
I’ve struggled with my trade’s visibility on line, and this post has furnished me with new methods—I’m excited to put in force them! Visit my web site: Local SEO consultants in my area !
I’m making plans to put in an out of doors bathe this summer time—how clean will that be? Check out progressive outdoor designs at outdoor living solutions !
I recently shipped my motorcycle across the country from LA and I used shipping motorcycles Los Angeles . They made the process so easy!
Amazing how a whole lot fitter my bushes glance after following your counsel—I owe it all to your web publication and may put forward others investigate out affordable tree trimming !
WOW just what I was looking for. Came here by searching for seo
https://PSBS-Biak.com
Tree removal should be a complicated decision, however it be frequently crucial for defense. professional tree removal
Hurrah, that’s what I was searching for, what a data! present here at this web
site, thanks admin of this site. http://Articomed.com/node/219088
I look forward to seeing more content that explores the intersection of technology and firearms regulation over at ##anyKeyword#! Bulk Ammunition, Gun Parts, & More!
Hurrah, that’s what I was searching for, what a data! present here at
this web site, thanks admin of this site. http://Articomed.com/node/219088
These facts will suitably support my small commercial enterprise support visibility on line! More components would be found at SEO experts for small businesses !
I’m amazed at how swiftly and efficaciously the staff from empresas de mudanças são paulo dealt with our office stream in São Paulo!
Residential or industrial movements may well be disturbing; although, with ### anyKeyword### by means of your facet, everything feels manageable. caminhão de mudança sp
These are really wonderful ideas in about blogging.
You have touched some nice things here. Any way keep up wrinting.
Thanks for the clear breakdown. Find more at ادمین اینستاگرام .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Restoration Near Me
The most efficient side about hiring a Carpenter Dallas is their concentration to aspect! custom carpenter dallas
Can you propose merchandise for cleansing chrome steel appliances? house cleaning service near me
Very interesting take on the role of AI in modern marketing strategies! Discover more tech insights at marketing blog .
I am genuinely thankful to the holder of this website who has shared this
great article at at this place. https://Gratisafhalen.be/author/amieisaac29/
This is quite enlightening. Check out cocinas en Granada for more.
Thanks for the helpful article. More like this at affordable my plumber services .
It’s encouraging to see more dialog round ####couples healing####—it reveals we’re all human and want give a boost to generally. Therapist Perth
Take a peek here https://PS-Barito-Putera.com
I am genuinely thankful to the holder of this website who has shared this great article at
at this place. https://Gratisafhalen.be/author/amieisaac29/
This is very insightful. Check out https://studentdone.com?qa=user&qa_1=bedwynmkkx for more.
I found this very helpful. For additional info, visit https://casting.orn55.ru/user/cyrinabgwd .
Excited approximately summer time coming up; highest time for clean desserts made with Nang Tanks! Nang Robot
This was a wonderful post. Check out Persian therapist for mental health for more.
This was a great help. Check out Farnham Dentistry top-rated dentist Jacksonville FL for more.
“If you adore cooking as tons as baking, whipping up savory dishes crowned off with the aid of refreshing creams from chargers will take your nutrients to an additional stage; discover ideas simply by # # anyKeyWord # # !” Nangs Delivery Melbourne
This was a wonderful guide. Check out home remodeling for more.
Envision Low Voltage sounds like a tremendous alternative for a person seeking to install safeguard cameras in Sanford, FL! Security Camera Installation Sanford
If you want to maximize your compensation after a car crash, consider hiring an experienced lawyer from Garland—check out garland injury lawyer !
What are some common misconceptions people have about car window tints? Would love to hear thoughts before visiting window tinting Jeffersonville Indiana! office window tinting services
Working on my technique with my trusty Gibson Les Paul’s has been so rewarding; what techniques are you mastering right now?! Let’s share tips over at Gibson Les Paul Standard
Thank you for breaking down the process of chiropractic care so clearly! Chiropractor
Very helpful read. For similar content, visit Exclusive private room bar NYC .
The stigma around ##couples remedy## is slowly fading, and it’s super to see more other folks in quest of guide in Perth. Marriage Therapist Perth
That’s great info about insurance options with ##anyKeyword#. Thanks! Santa Ana car moving companies
The professional team at Exterior Window Cleaning always does an amazing job on my windows!
I just completed my first car shipment with #### anyKeyWord### and couldn’t be happier! Detroit car transport
Seattle’s sandblasting businesses really know what they’re doing. If you’re interested, check out Sandblast Company for details!
I recently completed a Bellevue bathroom remodel, and I couldn’t be happier with the results! The transformation was incredible, and it has made such a difference in my daily routine https://renewal-home-upgradeswlpi369-mercerislandbqji435.lowescouponn.com/transform-your-space-expert-bathroom-renovation-and-luxury-kitchen-remodel-insights-from-bellevue-pros-2
What’s up, the whole thing is going fine here and ofcourse every one is sharing information, that’s truly excellent, keep up writing.
Thanks for the great tips. Discover more at Affordable Pest Solutions .
Effective use of landing pages can dramatically increase conversion rates—your insights were spot-on! Creative website design solutions
The area approximately voice search optimization became quite interesting! I talk about this theme extra at SEO KC .
Local web optimization is this kind of successful tool! It can make or break a small commercial enterprise in at the moment’s marketplace. For valuable resources, investigate out Small business local SEO near me .
It’s appealing to determine how hyper-neighborhood targeting can gain area of interest enterprises specifically—thanks for laying off pale in this! Local SEO consultants in my area
Well done! Find more at Farnham Dentistry dentist near 32223 .
My rooftop terrace has turn into a haven for morning coffee and night sunsets—so thankful for this space! Explore rooftop residing inspirations at outdoor living features !
This blogging site highlights the importance of basement waterproofing in stonework magnificently! New Shirt weather condition may be severe, so it is actually essential to guard your structures. For more details, go to experienced waterproofing contractors nearby .
Helpful suggestions! For more, visit carpintería de alumino A Coruña .
Hola Espero que todo vaya excelente Quiero contarte sobre un plataforma de apuestas online que te va a
encantar. Este casino tiene una variedad impresionante de juegos y una navegación muy fluida.
Si prefieres las slots, te encantará con las increíbles
tragamonedas disponibles. Además, el casino tiene todos los
juegos de mesa que puedes imaginar.
Lo que más me gusta de este casino online es que admiten pagos locales en América Latina.
En nuestra parte del mundo, es muy importante que los métodos de pago sean fáciles de usar
y seguros, y este casino tiene un sistema de pagos rápido y seguro.
No solo eso, te dan bonos de bienvenida para jugadores nuevos.
Cuando te hagas miembro, recibirás un bonus de registro que te permitirá darle un buen comienzo a tu experiencia.
También, tienen promociones regulares.
Este casino también cuenta con atención al cliente de primera, para resolver
cualquier inconveniente. Siempre podrás hablar con un agente.
Otro punto fuerte del casino es la seguridad, el portal utiliza medidas de seguridad muy estrictas para que tu privacidad
esté a salvo. No tendrás que preocuparte por nada.
Pablito, esta plataforma, te aseguro que no te arrepentirás.
¡Las posibilidades de ganar son enormes! Además, siempre podrás disfrutar
de gráficos impresionantes. Te vas a divertir muchísimo.
Te recomiendo que entres ahora mismo y disfrutes de todo lo que tiene para ofrecerte.
Recuerda, Pablito, no te puedes perder esta oportunidad.
¡Suerte y que empiecen las ganancias!
Investing time into researchingpotentiallawyerscanpayoffinterms ofreceivingbetterlegalcounselandguidancealongthisjourneyaheadafterbeinginjuredbytrucks.# # anyKeyWord### McKinney auto accident lawyer
This was a great help. Check out ادمین اینستاگرام for more.
Lakewood chiropractors have really helped me with my back pain. I’ll definitely visit Lakewood Chiropractor for their services!
Your guidance on organizing closets has made my lifestyles rather a lot more convenient! art’s house cleaning services
A friend introduced me to classic rock through his Les Paul, and now I’m hooked! What got you started? Let’s chat at Les Paul Financing .
I enjoyed this post. For additional info, visit Foothills Paving .
Awesome information here! For anyone looking to enhance their SEO game, try buying backlinks from Backlink packages .
The stigma around bankruptcy often overshadows the reality that it can be a necessary step towards financial recovery. Understanding the different types of bankruptcy and their implications is crucial bankruptcy attorney
I appreciated this article. For more, visit Afordable Pest Solutions .
Great facts about indoor vs outdoor cameras—I not ever knew there were so many explanations to agree with! Outdoor Security Camera Installation
I appreciated this post. Check out power washing services for more.
My friends recommended Grand Prairie moving companies when I moved to Grand Prairie, and they were spot on!
So completely happy I located this article; it truly opened my eyes to the conceivable of N2O chargers!! Nangs Delivery Melbourne
“You can’t go unsuitable making an investment in best equipment just like the #Nangs Tank#!” Nang Cylinders Melbourne
Thank you for advocating for safe storage practices through your content at Imported Pistols !
So glad I chose ###ANYKEYWORD### based on recommendations; they truly are one of the best budget movers around. Cheap movers Jacksonville
“Hoping more individuals recognize how essential planning is while considering shipments—visit information shared via #### anykeyword####.” Rancho Cordova auto transport companies
I highly suggest getting a quote from #AnyKeyWord#. Their prices are unmatched around here! Cheap movers Altamonte Springs
Enthusiastic about discovering innovative strategies employed regularly aimed improving customer satisfaction levels witnessed consistently across numerous encounters sharedwithin wider communities enabling everyone thrive successfully together Gotha commercial movers
This was very beneficial. For more, visit ادمین اینستاگرام .
Was blown away seeing transformation achieved simply utilizing services provided surrounding logistics managed professionally resulting inevitably achieving successful outcomes when collaborating together reaching exclusively toward ####ANYKEYWORD## Cheap movers Jacksonville
It feels great being settled into my new space after working with #Titusvillmovingcompany#. Highly recommend giving them a shot! Best Titusville movers
The moving process was seamless thanks to the amazing service from Fort Worth movers —definitely worth checking out!
Highly recommend Long distance movers Yulee to anyone looking for movers in Yulee!
Just wanted drop note expressing gratitude towards incredible service provided recently experienced firsth Cheap movers Kennedale
I found ###to be one of the most reliable services available for anyone needing help moving around ###FernandinaBeach###. Cheap movers Fernandina Beach
Just moved into my new apartment in Zephyrhills, and the movers from Zephyrhills commercial movers made the process so smooth!
I enjoyed this article. Check out Texas Strong | Air Conditioning & Heating | Houston for more.
I appreciate the clear explanations. Find out more about dental crowns at Farnham Dentistry general dentistry office .
Very informative article. For similar content, visit mental health support in Farsi .
Hurrah, that’s what I was seeking for, what a stuff!
present here at this web site, thanks admin of
this web page.
Finding legal representation was key to resolving my claim quickly and efficiently after my car crash in Dallas—highly suggest doing so! Visit dallas car accident lawyer for assistance!
Thank you for sharing those important insights! It’s refreshing to work out a focus on information canine habits. I advise vacationing http://alr.7ba.info/out.php?url=https://high-wiki.win/index.php/Understanding_Your_Puppy%E2%80%99s_Disinterest:_Why_She%E2%80%99s_Turning_Her_Nose_Up_at_Dog_Food for even extra top notch tips!
I loved how arranged every little thing was once for the time of my current go with empresas de mudanças são paulo #—really put forward their features!
This was highly helpful. For more, visit expert same day plumbing .
This is highly informative. Check out http://onlyall.ru/user/amarissjzf for more.
Local SEO tactics can honestly radically change a business. If you’re searching out talents, I put forward vacationing Affordable local SEO near me for tailored suggestions!
Great insights regarding balancing traditional UX principles while experimenting with emerging trends—it’s all about finding harmony! Custom website design for small businesses
อยากให้ทุกคนลองใช้ไฟหน้าโปรเจคเตอร์นะครับ มันดีจริงๆ ร้านแต่งไฟรถยนต์ ใกล้ฉัน
Thanks for the clear advice. More at ادمین اینستاگرام .
A effectively-deliberate deck with excellent lights transforms evenings into magical reports—what are a few innovations you’ve had for yours? residential hardscaping
Highly recommend checking out the before-and-after photos from Dr. Todd Brilliant DDS .
I normally in finding filth in the identical areas! Any facts on easy methods to restrict it? art’s cleaning
This design is spectacular! You most certainly know
how to keep a reader entertained. Between your wit and your videos,
I was almost moved to start my own blog (well, almost…HaHa!) Great job.
I really loved what you had to say, and more than that, how you presented it.
Too cool!
https://tunnellracing.com/
Fantastic publish about typography! It can make or ruin a design. I shared a few examples at Best web design agency .
I on no account found out the impact of Google My Business except I learn this post! Thanks for sharing. Learn extra at Professional local SEO services .
The have an effect on of weather prerequisites on landscaping possible choices is big; thanks for shedding easy in this fundamental theme—talk over with for extra insights: landscaping services !
I appreciate all the advice I’ve received on selecting trusted professionals amongst SD’s best. sunshine dentistry north park
Cannot express enough gratitude towards Best oceansides dentist for their fantastic work!!! ### anykeyword ## dentist near me
My smile transformation journey began with an amazing consultation at a local cosmetic dentist near me #.
Seasonal decorations can make your open air space feel festive and inviting! Get inspired by way of seasonal subject matters at outdoor living .
Appreciate the insightful article. Find more at Deck contractors near me .
This was highly informative. Check out Aldridge Roofing & Restoration for more.
Thanks for the detailed guidance. More at TheWinslow .
Cleanliness standards are top-notch which gives peace-of-mind while visitingBest ocean sides dentists -highly recommended!!! #### Surf Smiles Dentistry
This was beautifully organized. Discover more at Affordable Pest Solutions .
Basement waterproofing is such an essential element of masonry that many people fail to remember! Many thanks for taking it to light. For those needing to have support in NJ, I highly recommend having a look at licensed waterproofing contractor near me .
I love how Guns: Pistols, Rifles, Shotguns & More promotes a balanced view on gun rights and responsibilities. Well done!
I’ve transform relatively admired amongst neighbors given that introducing them to cakes made with my new chargers from # # any Keyword # #! Nangs Delivery Melbourne
I’ve visible such a upward push in attractiveness of nangs in Melbourne in recent times; every body seems to love them! Learn greater at Nang Tanks Melbourne !
“Loved every moment while being driven around by this professional team in beautiful SantaAna!” Santa Ana auto transport
Local businesses really do need specialized help; thanks for advocating for hiring a dedicated SEO agency Basildon team!
If you’ve been injured due to someone else’s negligence, it’s essential to consult a legal expert! Find yours at fort worth car accident lawyer .
Nicely done! Find more at nutrióloga económica Saltillo .
Working on my technique with my trusty Gibson Les Paul’s has been so rewarding; what techniques are you mastering right now?! Let’s share tips over at Les Paul Neck Reset
This was quite helpful. For more, visit fábrica de cocinas .
A very worthwhile read! Check out Farnham Dentistry for family dentistry insights!
Appreciate the insightful article. Find more at Afordable Pest Solutions .
Anyone else love their experiences with a local chiropractor in Bonney Lake? Share your stories! https://claytonwdok135.theburnward.com/enhance-your-athletic-performance-with-a-sports-chiropractor-in-bonney-lake-2
Great job! Discover more at Serenity Therapy Group .
This was very enlightening! Looking into buying backlinks from Where to buy backlinks that actually work based on your recommendations.
I’ve recently had a huge problem with pests in my home, and I didn’t know where to turn Pest control
Great insights! Find more at ادمین اینستاگرام .
I love the theory of a cleaning schedule! It is helping me remain ready. house cleaning near me
Can someone tell me if insurance covers visits to a chiropractor in Mill Creek? Curious minds want to know! Chiropractor
Have you ever thought about including a little
bit more than just your articles? I mean, what you say is valuable
and everything. But imagine if you added some great images
or video clips to give your posts more, “pop”!
Your content is excellent but with pics and clips, this site could certainly be one of the greatest in its field.
Very good blog! http://dtyzwmw.com/comment/html/?123866.html
Have you ever thought about including a little bit more than just
your articles? I mean, what you say is valuable and everything.
But imagine if you added some great images or video clips to give
your posts more, “pop”! Your content is excellent but with pics
and clips, this site could certainly be one of the greatest in its field.
Very good blog! http://dtyzwmw.com/comment/html/?123866.html
Fantastic insights into how local seniors can better manage their healthcare coverage with Sue’s guidance! Health Insurance Agent
Advice given throughout entire undertaking resulted positively impacting overall morale thus conducting operations smoothly led solely due diligence performed via input provided through engaging professionals skilled like those working under umbrella Grand Prairie Mover’s
Thanks for the great information. More at Custom Deck Builders near me .
Thanks for the clear breakdown. Find more at NYC nightlife with private rooms .
Thanks for the helpful advice. Discover more at Effective rodent control Hackettstown .
The crew at empresas de mudanças são paulo made my residential movement seamless. Can’t counsel them satisfactory!
Hormone therapy can be life-changing! If you’re exploring this option, check out Centralia Hormone therapy for expert advice and support.
“Anyone else here used a mover from #Burleson? Share your experiences or check out mine at Burleson international movers !”
Such helpful insights on tents in Tampa—definitely bookmarking this page! waterslide for rent near me
Clearly presented. Discover more at best residential paving Wheat Ridge .
This was very beneficial. For more, visit ac repair company near me .
Glad I chose ### for transporting my bike—it was delivered ahead of schedule!” Los Angeles motorcycle shipping
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Restoration Near Me
Office relocations shouldn’t be overwhelming if proper preparations are made beforehand using correct resources like those listed via ## Weirsdale Mover’s
Nicely done! Find more at ادمین اینستاگرام .
Shoutout to the incredible staff at Cheap movers North Richland Hills who helped make my relocation in North Richland Hills so straightforward.
So excited about all the options; can’t wait to try out some new styles of tents!! ### anyKeyWord ## inflatable rentals tampa
This article made me recognise how a lot creativity can come from due to a drone digital camera! Can’t wait to experiment with new techniques! Check out more at https://www.giantbomb.com/profile/stubbadavu/ .
The effectivity of caminhão de mudança sp during our advertisement relocation used to be in actual fact appropriate!
Anyone know of any good moving companies in Titusville? I’ve seen great reviews for Titusville moving company that I might try.
Just moved with Gotha full service movers , and they made the process so much easier than I anticipated!
Thanks for the thorough analysis. More info at Affordable Pest Solutions .
Grateful for the insights on local movers; it saves us so much time during our search process—thank you! Optimo Moving’s Yulee
Just wanted drop note expressing gratitude towards incredible service provided recently experienced firsth Local movers Kennedale
Thanks for the thorough analysis. More info at cocinas Granada .
The Gibson Les Paul has shaped rock music history. Who’s your favorite guitarist that plays one? Let’s chat at Les Paul Goldtop .
My kids are already asking when we can rent another bounce house from bounce house zephyrhills again!
Thanks to the experts at Irving International Movers, I settled into my new home without any stress or worries! Forth Irving Mover’s
Customer-Centric Approach: Throughout the process, they took the time to address all my questions and concerns, ensuring I felt comfortable with every step. Their dedication to customer satisfaction was evident. pressure washing business Tampa Bay Pressure Washing
I used long distance movers from Zephyrhills last month and they were fantastic! More info available at Zephyrhills apartment movers .
I personally opt for by way of a 3000 PSI force washing machine for my deck since it truely will get into these not easy spots. You can discover greater remarkable insights at http://www.photos.newocx.com/index.php?url=https://spencerhfvo246.theburnward.com/choosing-the-right-psi-how-much-pressure-washer-power-do-you-need-to-effectively-clean-your-deck .
For quality paver sealing that lasts, look no further than # # anyKeywords# # in Tampa. house power washing near me Tampa Bay Pressure Washing
If you’re looking for fun this summer, check out the amazing water slides available in Tampa! inflatable rentals for adults near me
Personal injuries require thoughtful consideration—consulting with an experienced # anykeyword# is essential! dallas car wreck lawyer
Visit to learn more PS Barito Putera
It is the best time to make a few plans for the long run and it’s time to be happy.
I’ve learn this submit and if I could I wish to suggest
you few interesting issues or tips. Perhaps you can write next articles regarding this article.
I wish to learn more things about it! https://Bangkoksync.com/goto.php?url=http://Articomed.com/node/295852
Love your perspective on this topic! Can’t wait to enhance my site’s authority with links from Backlink service !
It is the best time to make a few plans for the long run and it’s time to be happy.
I’ve learn this submit and if I could I wish to suggest you few interesting issues or tips.
Perhaps you can write next articles regarding this article.
I wish to learn more things about it! https://Bangkoksync.com/goto.php?url=http://Articomed.com/node/295852
Lakewood has some fantastic chiropractors! I need to see what Chiropractor Lakewood has to offer.
Excitedly expecting updates from you regarding new products or tendencies entering play within this subject!!! ### anykeyword### Video Surveillance Installation
Can anyone recommend a skilled Dr Brilliant dentist for teeth bonding? I’ve been considering it.
What’s up, after reading this awesome post i am also cheerful to share
my know-how here with friends.
https://Malut-United-FC.com
If anyone wants advice about gum health or other concerns, reach out—it’s been such a helpful process via #### anyKeyWord ##### dentist in san diego
Knowing where to turn when seeking quality care makes all the difference—a big shoutout goes out towards this resource: ## north park cosmetic dentist
The customer service at the best Oceanside Dentist is exceptional! dentist near me
“Really love that my SD dentist takes time to educate me about oral health.” Sunshine Dentistry
I cannot get over how lengthy-lasting the N@O Cream Charger Tanks are in comparison to others I’ve tried! Nangs Delivery Melbourne
The discussion around hunting rights and regulations at Sports Air Guns, Airgun manufacturers, suppliers & exporters is informative and well-articulated.
If you would like to grow your knowledge just keep visiting this site and be
updated with the hottest gossip posted here. https://Geocdn.Fotex.net/minesec.gov.cm/web/index.php/fr/communiques/item/40-resultats-du-concours-d
If you would like to grow your knowledge just keep visiting this site and be updated with the hottest gossip posted here. https://Geocdn.Fotex.net/minesec.gov.cm/web/index.php/fr/communiques/item/40-resultats-du-concours-d
The shipping pace of Nang Tanks in Melbourne is astonishing! I’ll truly be ordering again from Nang Canisters .
Just completed my treatment plan at the best Oceanside Dentist, and I’m thrilled with results!! dentist in oceanside
bookmarked!!, I love your site! http://Www.infinitymugenteam.com:80/infinity.wiki/mediawiki2/index.php/%C3%83%E2%80%B0liminer_Les_Champignons_Dans_La_Pelouse_:_Guide_Complet_Pour_Un_Gazon_Sain_Et_Esth%C3%83_tique
Great insights! Find more at ادمین اینستاگرام .
This is so well-written and insightful! Discover more about dental crowns at Farnham Dentistry dental care .
Just wanted to share my positive experience with Sanford car transport for shipping vehicles in Sanford!
Grateful that I found myself in good hands after connecting through *^*^*^*^*^*^*^*^*/ Jupiter auto shippers
I believe we can make waves if we collaborate effectively moving forward amidst uncertainties utilizing strategies curated by experts over@# # anykeyword## Doral car shipping
Finding reliable transportation options has never been simpler thanks to recommendations from #|# anyKeyWord#! Melbourne auto shipping
Moving my car to Miami was stress-free thanks to Miami car transport !
Just wanted to give a shoutout to the team at Brandon auto transport companies #—they truly made my car shipment stress-free!
Thanks for finally writing about >Certain Scores May Predict Which Trauma Patients Face High
Risk of Multiple Infections – Healthcare Hygiene magazine <Liked it! http://M-Grp.ru/redirect.php?url=http://dragon-Slave.org/comics/YanirawmNicklinrv
A friend recommended # # anyKeyword # #, and I’m glad I took their advice for my car shipment! St Cloud vehicle transport
Are there any eco-friendly transportation options available in The Villages? Just curious! The Villages car transportation services
Appreciate the useful tips. For more, visit Serenity Therapy Group .
Many people underestimate how much an attorney can help after an auto collision. Discover the benefits of hiring a Fort Worth lawyer at Thompson Law .
How do you dwell inspired whilst residence cleansing sounds like a not ever-finishing mission? Asking for a chum…or me, haha! house cleaning service bay area
This is a great tip particularly to those fresh to
the blogosphere. Short but very accurate
info… Many thanks for sharing this one. A must read post! http://Www.kosmodromstudio.com/comment/html/?201702.html
This is a great tip particularly to those fresh to the blogosphere.
Short but very accurate info… Many thanks for sharing this one.
A must read post! http://Www.kosmodromstudio.com/comment/html/?201702.html
Filing for bankruptcy might seem like an overwhelming process, but it can provide a fresh start for those in severe financial distress. It’s essential to seek professional advice to navigate the complexities involved bankruptcy lawyer
Mercer Island is such a beautiful place to live, and home remodeling can truly enhance its charm! I recently completed a project that transformed my living space into a more functional and inviting area Sumner Home Remodel
Training might be a assignment, however your step-with the aid of-step method makes it seem workable! I’ll completely be finding out http://sigha.tuna.be/exlink.php?url=https://gravatar.com/sharkpink2391420adc for more training methods.
Martial arts not just boost physical conditioning yet additionally infuse technique and focus in professionals. It’s remarkable to see exactly how various styles, from karate to jiu-jitsu, deal special advantages kids karate denver
I found that many people are unaware of their rights after an injury; that’s where a great Garland accident lawyer comes in! garland personal injury lawyer
Thank you for every other informative website.
Where else may I get that type of info written in such a
perfect means? I’ve a undertaking that I’m simply now running on, and I have been on the glance out for
such information. https://www.Kenpoguy.com/phasickombatives/profile.php?id=2752205
Thank you for every other informative website. Where else may
I get that type of info written in such a perfect
means? I’ve a undertaking that I’m simply now running on, and I have been on the glance out for such information. https://www.Kenpoguy.com/phasickombatives/profile.php?id=2752205
Appreciate the detailed information. For more, visit Bar with Private Room NYC .
Thanks for the informative content. More at urgent plumber near me .
This was quite informative. More at ادمین اینستاگرام .
Thanks for the detailed guidance. More at licensed plumbing and heating specialists .
This was very enlightening. More at Affordible Pest Solutions .
Very helpful read. For similar content, visit 24 hour plumber .
Thanks for the clear breakdown. More info at trusted plumber .
I recently moved to Puyallup, and I was shocked by how many pests I encountered in my new home! After doing some research on pest control options, I found that local services are crucial for effective solutions Pest Control Puyallup
Appreciate how thorough this piece become relating to symbol alt text utilization—it’s recurrently left out yet fundamental!! For deeper dives into visible optimization take a look at out ###AnyKeyWord#!! Best SEO company Kansas City
Great features approximately the role of social media buttons in internet layout! Check out my very own angle at Web design firm in my area .
Informative post! Learn more about oral health at Farnham Dentistry general dentistry office .
Appreciate the thorough write-up. Find more at https://maps.app.goo.gl/xkKCF8aNNJYomX7o8 .
What a big source this put up is for any small commercial enterprise owner trying to optimize their presence regionally! More amazing content feasible at Local SEO company near me .
I admire how you foster dialogue around sensitive topics related to guns over at Imported Pistols !
This video hit home. I’ve been waking up
3–4 times a night to pee, and it’s draining me during the day.
Glad to finally see a natural solution like Prostavive being explained clearly.
If this can actually help with flow and reduce those nightly bathroom trips, I’m definitely giving it a shot.
Useful advice! For more, visit affordable emergency pest control Long Valley .
I’ve seen some terrible graffiti that just ruins the vibe of an area. I hope more people consider professional help like Graffiti Removal for clean-up!
The merits of decluttering are uncommon; I sense lighter already! house cleaning service bay area
Useful advice! For more, visit Serenity Therapy Group .
Bespoke storage lower than beds maximizes bedroom performance fantastically while preserving aesthetics—I’m highly bought in this thought now too; discover alternate options now!: # custom built in shelves
Thanks for the practical tips. More at carpintería de alumino A Coruña .
I’m surprised at how totally different coloured stones can trade the vibe of an out of doors arena—hardscaping is all approximately picks! hardscape installation
This was highly helpful. For more, visit nutrióloga en Saltillo .
Awesome article! Discover more at tienda de cocinas en Granada .
The motorcycle shipping process can be tricky. Glad I found this blog! For further assistance, visit ship motorcycle Los Angeles .
The statistics about drone camera stabilization methods is precious for anyone severe approximately videography; thank you for sharing that insight! Visit https://hackerone.com/settings/profile/edit for greater hints!
The foam consistency performed with cream chargers is with no trouble just right; I can’t get satisfactory of it! Explore guidance at Nangs Delivery Melbourne .
I love how you discussed leveraging analytics tools effectively during redesigns; data-driven decisions lead us toward success. Best website design agency
Well done! Find more at ادمین اینستاگرام .
If you’re seeking out respectable movers who take note native regulations and routes, inspect out empresas de mudanças são paulo #.
Moving soon; getting quotes from ***anything KeyWord** could be beneficial based on these comments ! Cheap movers North Richland Hills
I’ve been utilizing nang cylinders from Nang Tanks Melbourne for my bakery, and that they’ve made a monumental big difference!
Outdoor routines have turn out to be my new preferred regimen—nothing beats exercise with nature around you! Discover exercise session tricks for open air at custom outdoor living !
You are so awesome! I do not think I’ve truly read through
anything like this before. So wonderful to discover someone with some genuine
thoughts on this issue. Seriously.. many thanks
for starting this up. This site is one thing
that is needed on the web, someone with a bit of originality!
https://Persija-Jakarta-id.com
Looking forward eagerly ahead towards another chance exploring diverse aspects surrounding delightful experiences gained through their assistance!! Kissimmee car moving companies
Magnificent goods from you, man. I’ve understand your stuff previous to and yoou are just too fantastic.
I really like what yoou hav acquired here, certainly likme what
you are saying and the way in whicxh you say it.
You make it enjoyable and you still care for to
keep it sensible. I can not wait to read far more from you.
This is really a tremndous website.
Feel free to visit my webb blog; kalkan boat hire
What an eye fixed-opener about the hazards of overgrown bushes—time for a specialist tree reducing carrier! tree removal experts
Excellent breakdown of NAP consistency! It’s essential for local search engine optimization success. For extra main points, look at various out Professional local SEO services .
Thanks for the helpful advice. Discover more at ادمین اینستاگرام .
A loved one cautioned me to use caminhão de mudança sp for my movement and I couldn’t be happier with that tips!
Each visit reminds us why investing time into planning memorable events produces cherished recollections lasting across generations connected via shared experiences! water slide into pool rental
Tree healthiness starts offevolved with applicable care, and your web publication emphasizes that completely! Checking out residential tree trimming quickly!
I liked this article. For additional info, visit water damage restoration companies Franklin Park IL .
Thanks in your insights into optimizing web publication titles and meta descriptions—they’re needed but incessantly uncared for aspects of search engine optimization; see comparable assistance at ## SEO consultants in my area
This was highly useful. For more, visit TheWinnslow .
Investing in professional tree removing expertise can prevent time and issue ultimately! tree removal
I found this very helpful. For additional info, visit water heater installation near me .
ใครเคยเจอปัญหากับไฟหน้ารถ LED บ้าง? แชร์ประสบการณ์หน่อยครับ ร้านตั้งไฟหน้ารถยนต์ ใกล้ฉัน
Explore endless creativity abound unleash excitement create bonds forge friendships lasting lifetimes achieved embracing uniqueness celebrated thoroughly universally cherished wholeheartedly openly embraced warmly received heartily welcomed forevermore rent party tent
Water slides are a must-have for summer fun, especially when renting from Tampa’s great selection! water slide rentals pinellas county
Thanks for the useful post. More like this at Affordable Pest Solutions .
It’s crucial to have legal support after an injury. A great McKinney injury lawyer can help you navigate this tough time. Visit Thompson Law for assistance.
Valuable information! Discover more at home remodeling .
This weekend was epic with our rented bounce house from Tampa! Don’t miss out on bounce house rentals land o lakes !
The results were nothing short of spectacular! My driveway, patio, and siding looked brand new after their thorough cleaning. The difference was remarkable, and I couldn’t believe how much grime and dirt had accumulated over time. home exterior cleaning Tampa Bay Pressure Washing
This was a wonderful post. Check out hardwood floor refinishing near me for more.
Great advice on via drone cameras! I by no means knew about the importance of balancing the gimbal. Check out more at https://www.divephotoguide.com/user/nycoldrxih/ .
Summer days spent enjoying sunshine paired alongside refreshing splashes lead me back fondly recalling unforgettable moments gathered via these installations! water slide rentals zephyrhills fl
For affordable and effective paver sealing, visit gutter cleaning tampa today!
Curious if every person else feels as passionate about helping regional carpenters as I do; they deserve our trade!” # # anyKeyWord # licensed carpenter dallas
Appreciate the great suggestions. For more, visit https://maps.app.goo.gl/v169aDZtfLWSQwkx7 .
Do you offer any special packages for roof washing along with window cleaning? That would be awesome! Roof Cleaning
Hi there! I know this is kinda off topic however I’d figured I’d ask.
Would you be interested in exchanging links or maybe
guest writing a blog article or vice-versa? My blog covers
a lot of the same topics as yours and I believe we could greatly benefit from each other.
If you are interested feel free to send me an e-mail.
I look forward to hearing from you! Superb blog by the way!
This was quite enlightening. Check out ادمین اینستاگرام for more.
Just had my vehicle transported successfully thanks to a company I discovered via Sunshine Auto Transport’s Melbourne #—so grateful!
Has anyone else had a great experience with a Jupiter auto transport service like Jupiter car transport ?
I highly recommend Sanfor dcar transpor t if you want peace of mind during your move !!## anyKeyWord## Sanford car transportation services
If you’re in need of last-minute rides, spring hill’s transport service is always there when you need them: ### anyKeyWord ## Spring Hill car shipping
Choosing #WestonCarShippers has been a game-changer for many people—read on! ## Weston auto transport company
Finding trustworthy transportation can be tough—thank goodness for # any keyword#! Kissimmee auto shipping
Never thought transporting a vehicle could be this easy until I found out about Homestead auto shippers #!
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Restoration Near Me
Hopefully, further collaboration takes situation among readers here foremost towards higher group knowledge!!! ### anykeyword### Wireless Security Camera Installation
You won’t regret choosing the services from # anyKeyword # for your Boynton Beach auto shipping needs. Sunshine Auto Transport’s Boynton Beach
I had no clue that poor airflow could impact drying efficiency—thanks for enlightening me! Dryer Exhaust Duct Cleaning
I enjoyed this read. For more, visit ادمین اینستاگرام .
Appreciate the detailed post. Find more at carpintería de aluminio en Coruña .
I didn’t know there were three main types of cleaning services! This will help me choose what I need when contacting cleaning services Blairsville PA. cleaning services Blairsville PA
Thanks for the useful post. More like this at cocinas en Granada .
Thanks for the informative content. More at nutrióloga .
Just got my truck shipped across the country by Detroit auto shippers #—fantastic service all around!
The history behind Gibson Les Paul guitars is fascinating! What’s your favorite fact about them? Discuss at Les Paul Sound .
Just completed my move with a Burleson moving company that I found through Burleson movers . Highly satisfied!
If you’re on a budget, you need to consider Jacksonville moving company for your next move in Jacksonville!
Vehicle shipping doesn’t have to be stressful! Check out #anything—they make it so easy and straightforward! Rancho Cordova vehicle transport
I enjoyed this post. For additional info, visit dedicated motor vehicle accident lawyer .
Anyone else have success with finding cheap movers? I had a fantastic experience with Long distance movers Allen #.
You’ve provided amazing insights here! Don’t overlook the services offered by Backlinks provider when buying backlinks.
If you’re relocating your business, don’t underestimate the power of a good moving company! Explore options on Cheap movers Weirsdale .
After my first consultation with a Garland attorney, I felt much more confident about my case! Thanks to the insights from garland accident lawyer !
If you’re in Jacksonville and need to move your office, definitely check out Momma Mover’s for trustworthy movers!
Finding effective ways address complexities inherent transitions represents considerable challenge necessitating comprehensive underst Altamonte Springs commercial movers
This is extremely helpful and insightful! Discover more about dental crowns at Farnham Dentistry top-rated dentist Jacksonville FL .
Just wanted to drop by and say how helpful I found the content at Titusville moving companies # regarding moving services.
This video hit home. I’ve been waking up 3–4 times a night to pee, and it’s
draining me during the day. Glad to finally see
a natural solution like Prostavive being explained clearly.
If this can actually help with flow and reduce those nightly bathroom
trips, I’m definitely giving it a shot.
Thanks for the thorough review! Oral hygiene is so much more than brushing and
flossing, and ProDentim seems like a smart way to
support that balance naturally. Definitely adding this to my dental care routine
after watching this.
A motivating discussion is definitely worth comment. I think that you should publish more on this topic, it might not be a taboo matter but typically people don’t speak about these issues. To the next! Kind regards!! lightweight headphones
The best part about my move was definitely working with the professionals at Metro Mover’s Fernandina Beach .
Filing for bankruptcy might seem like an overwhelming process, but it can provide a fresh start for those in severe financial distress. It’s essential to seek professional advice to navigate the complexities involved bankruptcy lawyer
Thanks for the great tips. Discover more at ادمین اینستاگرام .
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Just finished my move with an incredible team of movers in Irving! Find out more at Best Irving movers .
I found the perfect solution for my office move with Satellite Beach apartment movers —they made everything so manageable!
I wish every moving company was as great as # anykeyword#. Their #localmovers# made everything so stress-free! Zephyrhills moving companies
If you need official movers in São Paulo, seem to be no additional than empresas de mudanças são paulo —they may be virtually the most excellent!
Great job! Discover more at Driveway Paving Contractors Wheat Ridge .
The step-by-step approach to understanding health insurance is incredibly helpful—great work, team! Cheap Health Insurance Cape Coral
Fighting style not only enhance physical fitness however additionally infuse discipline and emphasis in practitioners. It’s interesting to see exactly how various styles, from karate to jiu-jitsu, deal unique advantages Denver karate kids
The diversity of perspectives showcased in your articles makes for an enriching experience when visiting Firearms Accessories .
Thanks for the thorough analysis. Find more at dedicated motor vehicle accident lawyer .
Highly energetic blog, I loved that bit. Will there be a part 2?
https://Persita-Tangerang.com
Just moved my place of work in São Paulo, and the team from caminhão de mudança sp made it so easy! Highly chuffed!
Appreciate the comprehensive insights. For more, visit ادمین اینستاگرام .
Asking questions are really pleasant thing if you are not understanding something completely, except this piece of writing presents good understanding even. https://arbeitgeberverbandlueneburg.de/die-welt-neu-denken-av-forum-2020/?newsletter=http://Dtyzwmw.com/comment/html/?117155.html
After my experience with cosmetic dentist near me , I can’t stop smiling! Highly recommend their services.
Asking questions are really pleasant thing if you are not understanding something completely, except this piece of writing
presents good understanding even. https://arbeitgeberverbandlueneburg.de/die-welt-neu-denken-av-forum-2020/?newsletter=http://Dtyzwmw.com/comment/html/?117155.html
My family has been going to this same dentist near me in Oceanside for years; we love it!
Just left my appointment at a North Park cosmetic dentist near me feeling fabulous about my smile!
Does anyone know a pediatric dentist in San Diego? I need one for my kids. sunshine dentistry north park
Loved your discussion about brand ambassadors and their impact—leveraging fans can enhance visibility greatly; check ambassador programs exploration over ###anKeyWord## blackhat marketing blog
Seasonal cleaning is key; that’s why I love using services from Window Cleaning # every few months.
Cream chargers: the name of the game element each baker may want to be aware of about! More information at Nangs Delivery Melbourne .
”From cakes to coffees; nothing beats the flexibility bought %%!%%b3842b59-1/3-4ebc-b1e6-ef84f390c3b3%%!%% (nangs); don’t prolong & order this day @ (#@@@@)!” Nang Cylinders Melbourne
It’s pleasing how GPM can impact now not only performance yet also the ecosystem. I’m excited to enforce some of these advice in my domestic! http://kikuya-rental.com/bbs/jump.php?url=https://research-wiki.win/index.php/Revitalize_Your_Outdoor_Space:_How_Often_Should_You_Pressure_Wash_Your_Patio_for_Maximum_Curb_Appeal%3F_72843
I enjoyed this post. For additional info, visit construction company .
If you’re in town, definitely consider visiting the best Oceanside Dentist for your dental needs! dentist in oceanside
Thanks for the practical tips. More at social hotspots with private rooms NYC .
Can you put forward merchandise for cleaning stainless steel home equipment? art’s cleaning
When it comes to kitchen remodeling in Sumner, we focus on smart storage, beautiful finishes, and long-lasting value. Home Remodel Sumner
Very helpful read. For similar content, visit Eco-Friendly Pest Control Hackettstown .
Nice breakdown of different sorts of key terms and their uses in content material advent; very efficient facts here! Dive deeper with me at KC SEO agency near me .
Excellent read! Quite enlightening. Find out more at Farnham Dentistry Jacksonville FL dentist about oral health.
This content has truly inspired me—I can’t wait to connect with skilled professionals at an outstanding ###anSEO### firm! SEO agency Basildon
You deserve compensation if you’ve been hurt due to someone else’s mistake—visit ##anyKeyword# for help! fort worth accident lawyer
This was very enlightening. For more, visit ادمین اینستاگرام .
This article covers every part establishments need to recognize about optimizing in the community! Highly counsel testing the additional materials at Trusted local SEO near me .
Very helpful read. For similar content, visit ادمین اینستاگرام .
Find out how to do it PS Barito Putera
A relaxed nook with tradition-developed seating is preferrred for playing morning coffee—it adds most warm temperature to the house! Explore designs at custom built ins
I imagine that each yard deserves an inviting pathway; it’s some of the handiest but most impactful aspects of great hardscaping! hardscape installation
Thanks for the useful suggestions. Discover more at https://maps.app.goo.gl/QoH66eXm7xDxRPQX7 .
Appreciate the detailed information. For more, visit affordable plumbing costs .
Nicely detailed. Discover more at expert drain cleaning solutions .
Follow this link https://PS-Barito-Putera.com
Thanks for the helpful article. More like this at Affordible Pest Solutions .
Custom closets can turn out to be any room. I’m eager about a built-in layout! Visit custom closet design for big options.
Incredible points. Solid arguments. Keep up the great work.
This was very enlightening. For more, visit https://maps.app.goo.gl/DXFwjsFwARByFXXS6 .
This was nicely structured. Discover more at Serenity Psychotherapy Group .
“Thanks for sharing your data about being concerned for trees and whilst to name in pros like these in tree reducing services! commercial tree experts ”
Thank you for providing a platform that encourages responsible discussions about firearms and their use, such as seen on Bulk Ammunition, Gun Parts, & More! .
I found your discussion about cross-browser compatibility informative; everyone should have equal access regardless of their browser choice. Creative website design solutions
Engaging with shoppers by means of e-mail advertising may additionally enrich your neighborhood presence; thank you for uplifting me with that concept! Local SEO help for businesses
Read more https://PS-Barito-Putera.com
Thanks for this detailed review! I’ve tried so many joint formulas over the years, but
most don’t deliver lasting relief. Joint Genesis sounds promising, especially since
it’s made in a GMP-certified facility. Subscribed
to hear more reviews like this!
Our clients love how our Sumner WA remodeling projects blend modern upgrades with timeless design. Remodel Company
The innovations referring to content material audits have been very successful; I’ll be enforcing those quickly—check out an identical counsel at SEO experts for small businesses
Thanks for sharing this information about Mill Creek Chiropractors! Very informative! Chiropractor
Appreciate the detailed information. For more, visit nutrióloga barata en Saltillo .
Did you understand that tree removal could also strengthen your home’s significance? tree removal
Thanks for the useful post. More like this at ادمین اینستاگرام .
Grateful for the smooth transition thanks to the amazing team at Grand Prairie apartment movers # during my recent move in Grand Prairie.
Thank you for sharing these principal insights! It’s clean to see a focal point on knowledge canine conduct. I endorse journeying https://wakelet.com/wake/XAW1ylJX3IvxzQKXTanb6 for even extra good sized advice!
Thanks for the great tips. Discover more at TheWinslo .
What a great experience with #burlymovers# when moving into my new place! Check them out here: ####url###! Burleson movers
Nicely done! Find more at Afordable Pest Solutions .
Buying backlinks can be tricky, but I trust High DA backlinks for sale for quality and reliability.
Thanks for the thorough analysis. Find more at ادمین اینستاگرام .
Cream chargers deliver one of these light and airy texture to cakes—love it! Nangs Delivery Melbourne
I recently had a pest issue in my home, and I was amazed by how effective the Puyallup Exterminator service was! They identified the problem quickly and implemented a comprehensive plan to eliminate the pests Pest control
The impact of clean public spaces cannot be underestimated! Thank you for highlighting the importance of graffiti removal services like Sandblasting .
Shoutout to everyone discussing their experiences; it’s helping me finalize my decision on using ###.” 𝗧𝗵𝗲 𝗠𝗼𝘁𝗼𝗿𝗰𝘆𝗰𝗹𝗲 𝗦𝗵𝗶𝗽𝗽𝗶𝗻𝗴 𝗖𝗼𝗺𝗽𝗮𝗻𝘆 𝗟𝗼𝘀 𝗔𝗻𝗴𝗲𝗹𝗲𝘀
The most beneficial edge approximately hiring a Carpenter Dallas is their attention to aspect! custom carpenter dallas
I’m website hosting a celebration soon and can surely be ordering my nangs from ###! Nang Tanks Melbourne
Thanks for the useful post. More like this at expert residential driveway paving .
Looking for an affordable auto transport option? The Rancho Cordova companies offer great deals! Discover more at Rancho Cordova car moving companies .
Looking for ways to make your move easier? Consider hiring professional movers from Jacksonville full service movers !
Appreciate all the detailed suggestions in this post—I’ll check out **#** anyKeyWord**#** right away! Kissimmee auto shippers
I was surprised by how affordable # # anyKeyWord # was compared to other options! Allen moving company
It’s hard to find good help these days – but luckily, #localmovers really came through for me recently. North Richland Hills full service movers
This article made me rethink our upcoming move—definitely checking out Weirsdale Mover’s for better options!
Just had an amazing experience with ###; they really are the best option if you’re looking for cheap movers here in JAX. Jacksonville movers
I wish I had known about this Best Fort Worth movers before my last move in Fort Worth!
Just wrapped up an amazing relocation thanks to #Titusvillmovingcompany#. Definitely worth checking out if you’re planning on moving soon! Titusville moving company
Thank you for detailing the best office moving companies in Yulee; it’s a great help during this busy time! Yulee apartment movers
“Underst Gotha commercial movers
If anyone needs recommendations for a good Kennedale moving company, let me know—I have some great options! Long distance movers Kennedale
Great insights! Find more at quality pest control services Long Valley .
“Thinking about an office upgrade? Don’t forget about the valuable resources from #anyKeyword#!” Local movers Satellite Beach
Anyone else had a positive experience with long distance movers in Irving? I loved using Forth Irving Mover’s !
Really appreciate how this video broke everything down so clearly.
With so many sugar support supplements out
there, it’s hard to know what’s real. The fact that Sugar Defender is made
for early-stage type 2 concerns caught my attention—might be worth
trying before things get worse.
I found Detroit auto shippers while researching vehicle shipping agents in Detroit, MI. Their reviews are impressive!
This publish is ultimate for human being new to drones. The factors are clean and concise! Find added elements at https://www.instapaper.com/read/1851331221 .
The wide variety in coat styles between dog breeds is powerful! Do you prefer short or lengthy-haired puppies? http://voidstar.com/opml/?url=https://gravatar.com/reallygrand82d4d70255
This was quite informative. For more, visit ادمین اینستاگرام .
I recently discovered some amazing weight loss services in Centralia that have truly transformed my journey Medical spa
I love how versatile the Les Paul is for different genres. What’s your go-to style? Join the conversation at Les Paul Push-Pull Knobs .
This was quite helpful. For more, visit ادمین اینستاگرام .
Cosmetic dentistry is such a game changer—especially when you find the right place like cosmetic dentist Escondido .
Chiropractic care has changed my life! I’ll be looking into Lakewood Chiropractor for the best options in Lakewood.
A beautifully designed building deserves an equally stunning crowning touch like an elegant cooper-copper structure at its peak; wouldn’t you agree? # # anyKeyWord ## cupola for barn
Everyone should experience what it’s like to be treated by Best oceansides dentist; it’s always positive!! # # anykeyword # dentist Oceanside
I enjoyed this post. For additional info, visit https://maps.app.goo.gl/j1y6nz6yVw3Bbhp89 .
This was highly educational. For more, visit carpintería de alumino A Coruña .
Take a look at this page PS Barito Putera
Just booked an appointment with a https://sergioswww063.bearsfanteamshop.com/prenatal-chiropractic-care-in-bonney-lake-supporting-a-healthy-pregnancy-journey-3 —can’t wait to see how it goes!
Grateful for the excellent care I’ve received during every visit to my SD clinic! Sunshine Dentistry
Such a helpful platform; I’m excited about sharing this tip: visit #|# anyKeyWord#! before choosing your mover! Melbourne auto shipping
Moving to Miami was a breeze thanks to my reliable auto shipper! Highly recommend it! Miami car transportation services
Shout out to Jupiter vehicle shippers for excellent customer support during my recent Jupiter vehicle transport process.
“My family used # any keyword # recently, and we couldn’t be happier with their services!” Wesley Chapel car shippers
I recently used a service for St Cloud auto transport companies and was impressed with the efficiency. Highly recommend it!
I’m curious about teeth whitening options available through dentists in Oceanside; any thoughts? dentist near me
Moving doesn’t have to be overwhelming; check out # Sunshine Auto Transport’s Spring Hill # if you’re going anywhere like lovely Spring Hill!
Shipping a vehicle can be stressful, but Sanford car transport made it so easy for me from Sanford!
Thank you for explaining tips on how to reach gentle pictures with drones! It’s something I fight with recurrently. More recommendations at https://astro-wiki.win/index.php/**Unlocking_Aerial_Photography:_A_Beginner%27s_Guide_to_Using_Your_Drone_Camera** .
Great to see so many choices for getting around in The Villages! Planning to check out your services soon! The Villages car transport
I found your advice on choosing a carrier for homestead car shipping invaluable. Cheers! Homestead vehicle transport
I’ve been researching hormone therapy options, and it’s great to see clinics focusing on personalized care! Check out Medical Spa for more information.
Just wanted to share that renting through # anyKeywords # was super smooth and hassle-free! tampa water slides
ความสะอาดของร้านเหล้าสาย1 ทำให้รู้สึกมั่นใจในการใช้บริการมากขึ้นครับ ร้านชิลใกล้ฉัน
Thanks for the insightful write-up. More like this at https://maps.app.goo.gl/oK7LZHkqGkhNbRM16 .
Local SEO strategies are so important, especially for businesses in Basildon. I’ll definitely check out a SEO agency Basildon !
Who would’ve thought embracing childlike wonderment could yield such potent rewards fostering stronger bonds between loved ones celebrating life together integrated seamlessly! air water slide rentals
It’s wonderful how GPM can influence no longer purely potency but also the setting. I’m excited to put in force a few of those advice in my abode! http://kakaku.com/jump/?url=https://wiki-cafe.win/index.php/Revitalize_Your_Outdoor_Space:_How_Often_Should_You_Pressure_Wash_Your_Patio_for_Maximum_Curb_Appeal%3F
Love the inspiration of by using traditional additives for cleaning products! So smart! house cleaning
Thanks for the thorough article. Find more at ادمین اینستاگرام .
I highly recommend Tampa Bay Pressure Washing to anyone looking for a reliable, efficient, and high-quality pressure washing service. They exceeded my expectations in every way! exterior house cleaning Tampa Bay Pressure Washing
I am unquestionably leaning against going with pro guide after reading your article—it simply makes feel!!! Surveillance Camera Installation
For affordable and effective paver sealing, visit local pressure washing companies today!
The variety of colors and styles available is simply amazing; perfect for any occasion!! ### anyKeyWord ## fun slide rental
We’ll definitely be coming back next year to rent another amazing inflatable from # anyKeywords #. rent party tent
Thanks for the helpful advice. Discover more at dedicated personal injury attorney .
May I just say what a relief to find a person that truly understands what they are talking about
on the net. You certainly know how to bring a problem to light and make it important.
More people have to look at this and understand this side of
your story. It’s surprising you are not more popular since you certainly have the gift.
It’s going to be ending of mine day, but before end I am reading this impressive piece of writing to increase my knowledge.
Right here is the perfect website for everyone who wants to understand this topic.
You understand a whole lot its almost hard to argue with you (not that I really will need to…HaHa).
You definitely put a brand new spin on a subject that’s been discussed for many years.
Excellent stuff, just wonderful!
I found this very interesting. For more, visit TheWinslow .
Appreciate the great suggestions. For more, visit water damage restoration companies near me .
This was highly educational. More at Affordible Pest Solutions .
This was super helpful! I’ve tried so many joint supplements that only mask the pain, but the way Joint Genesis targets the root causes sounds different.
Anyone here used it for more than a month? Would love
to hear how it holds up long term!
What’s up to all, how is all, I think every one is getting more from this web
page, and your views are fastidious designed for new people. http://Sm.co.kr/bbs/board.php?bo_table=free&wr_id=2973935
I found this very interesting. Check out https://maps.app.goo.gl/gnnDjZTsZJQJmRbz7 for more.
What’s up to all, how is all, I think every one is
getting more from this web page, and your views are fastidious
designed for new people. http://Sm.co.kr/bbs/board.php?bo_table=free&wr_id=2973935
I recently completed a kitchen remodel on Mercer Island, and the transformation is unbelievable! It’s amazing how a new layout and updated appliances can completely change the feel of a home Home Remodel Sumner
Thanks for the clear advice. More at ادمین اینستاگرام .
This was very enlightening. For more, visit ادمین اینستاگرام .
Do you know if insurance is included when shipping motorcycles? That’s something I need clarity on before proceeding; perhaps Los Angeles motorcycle transport has the answer!
Moving in São Paulo may also be overwhelming, but locating the exact group makes each of the distinction. Check out empresas de mudanças são paulo for nontoxic moving functions!
Fighting style not only improve physical conditioning however likewise instill self-control and emphasis in practitioners. It’s remarkable to see how various styles, from martial arts to jiu-jitsu, deal distinct advantages kids karate denver
Great submit! I’ve been purchasing for superb thoughts to show my puppy. The facts you shared are tremendously necessary! I stumbled on greater tools on this subject at https://padlet.com/devpage7hyvur/bookmarks-pajk481hccjx95es/wish/do3MQJk6Y36lZ15w .
Such an informative read on affiliate marketing! For further insights, check out marketing blog .
Very thorough article on Kissimmee auto shipping options; will definitely look into Kissimmee auto transport .
Jeff Lassila made the insurance process so much easier for me. Don’t miss out on the resources at insurance agencies Howell MI !
I enjoyed this article. Check out Affordable Pest Solutions for more.
Thanks to the workforce at caminhão de mudança sp , our transition into our new house changed into handy!
If you’re looking for reliable movers in North Richland Hills, I highly recommend checking out North Richland Hills full service movers . They made my move so much easier!
Have you ever upgraded components on your Les Paul? It’s amazing what difference it can make! Talk upgrades at Les Paul Sustain .
This was very enlightening. For more, visit Farsi Language Therapist .
If you’re considering a kitchen remodel in Bellevue, it’s essential to find the right contractors who can bring your vision to life https://renewal-home-upgradesqhfn437-puget-soundrfis451.timeforchangecounselling.com/transforming-tight-spaces-a-guide-to-small-kitchen-remodels-in-bellevue-4
I recently had a pest problem in my home, and I was amazed by the effective solutions offered by local services. It’s crucial to choose a knowledgeable pest control provider in Puyallup to ensure a pest-free environment Puyallup Pest Control
I found this very helpful. For additional info, visit https://citykhv.ru/user/sindurogdu .
Great job! Find more at expert plumbing and heating solutions .
. Cheers everyone involved behind scenes working tirelessly ensure everyone finds appropriate paths ahead gracefully !!! # Health Insurance Company
This was a fantastic read. Check out affordable reliable plumbers for more.
I found this very interesting. Check out expert plumbers in my area for more.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Restoration Near Me
Thanks for the helpful advice. Discover more at power washing service .
I liked this article. For additional info, visit https://maps.app.goo.gl/HKKh1TTGNdkdHEoi7 .
I found this very interesting. Check out ادمین اینستاگرام for more.
Thanks for the great tips. Discover more at tienda cocinas Granada .
Would encourage fellow readers not skip over crucial steps needed following incidents such as mine – find good lawyers who specialize!: ##### ## McKinney injury lawyer
The segment on modifying tool ideas used to be superb handy! It’s suitable to understand what gear are on hand. Explore similarly at https://speakerdeck.com/account/edit .
This was highly useful. For more, visit nutrióloga Saltillo .
What’s up colleagues, its wonderful piece of writing about teachingand
entirely explained, keep it up all the time.
Appreciate the detailed information. For more, visit TheWinslo .
Hi my loved one! I wish to say that this article is amazing, nice written and come with approximately all significant infos.
I’d like to look extra posts like this . https://systemcheck-wiki.de/index.php?title=Benutzer:DanelleRidgeway
Hi my loved one! I wish to say that this article is amazing, nice written and come with
approximately all significant infos. I’d like to look extra posts like this . https://systemcheck-wiki.de/index.php?title=Benutzer:DanelleRidgeway
Thanks for the great tips. Discover more at https://maps.app.goo.gl/PB4ZeXmKE1C2vY917 .
If you want a hassle-free experience while moving your car, definitely check out the services listed on Melbourne car moving companies !
Thanks for sharing your expertise on choosing the best Miami auto shipping services! Sunshine Auto Transport’s Kendall
Appreciate the detailed information. For more, visit Affordable Pest Solutions .
“Transportation made easy—thank you, # # anyKeywod#!” Jupiter car moving companies
Shipping my car from Wesley Chapel was easy with the right transport company. More details at Wesley Chapel auto transport company .
I didn’t realize how many options there were for auto shipping in St Cloud until reading this post! St Cloud auto transport companies
I’m intrigued by the potential of hormone therapy for aging gracefully. Excited to read more on this subject at Centralia Hormone therapy !
Useful advice! For more, visit ادمین اینستاگرام .
Honestly, Weston’s level of professionalism is unmatched in the industry—I’m very satisfied with their work!! More info on their site: Weston vehicle shipping
Anyone considering vehicle transportation should look into the services offered by Sanford! Sanford auto transport companies
So grateful for the convenience that comes with using the services of Sunshine Auto Transport’s Poinciana # when traveling through Florida.
I wish I had known about Spring Hill car shipping sooner! Their list of Spring Hill car moving services is so helpful.
Useful advice! For more, visit foothills paving and maintenance .
Wanting to ship your vehicle in or out of boyton beach? Start your search with insight from # anyKeyWord#! Boynton Beach car shippers
This is such an important discussion about health—thank you for raising awareness about chiropractors! Chiropractor Mill Creek
Greetings from Los angeles! I’m bored to death at work so
I decided to check out your site on my iphone during lunch
break. I love the info you present here
and can’t wait to take a look when I get home. I’m shocked at how fast your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyhow, superb site! https://Rentry.co/95185-tattoo-ideas-in-montreal-inspiration-for-your-next-ink
Great put up related to cellular-first layout ideas; they’re basic this day! Check out my suggestions too, at Affordable web design company .
Greetings from Los angeles! I’m bored to death at work so I decided to check out
your site on my iphone during lunch break. I love the info
you present here and can’t wait to take a look when I get home.
I’m shocked at how fast your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyhow, superb site! https://Rentry.co/95185-tattoo-ideas-in-montreal-inspiration-for-your-next-ink
Just completed my hardscaping challenge, and I can not have faith the change it made! Highly advise authentic guide for the most fulfilling outcome. hardscaping
Having encountered countless hurdles previously faced alone; truly uplifting discovering supportive allies willing extend helping h Grand Prairie moving company
A cozy nook with tradition-outfitted seating is good for playing morning espresso—it provides most heat to the house! Explore designs at custom built in units
Well done! Find more at ac repair near me .
Go on, click here https://PS-Barito-Putera.com
I realise the realistic tips given right here on regional search engine marketing processes—extra will likely be came upon at Top-rated local SEO near me !
This was a wonderful guide. Check out Long Valley Pest Control for more.
Your blog is crammed with precious facts that each and every aspiring drone photographer have to read—thanks for sharing a lot of these tricks and tricks, won’t be able to wait to discover extra substances provided by using vacationing https://romeo-wiki.win/index.php/**Capturing_the_Perfect_Shot:_Composition_Tips_for_Drone_Camera_Enthusiasts** !
The attractiveness of outdoor living is that you can create your very own sanctuary. What are your preferred outdoor traits? Share them at outdoor living !
”Your expertise shines through every word—you clearly know your stuff when it comes down to appliances!” Dry Vent Cleaning
A huge thank you to the amazing team of movers I found via Burleson moving company during my recent move in Burleson!
Working on my technique with my trusty Gibson Les Paul’s has been so rewarding; what techniques are you mastering right now?! Let’s share tips over at Les Paul Traditional
Your web publication covers a lot constructive tips approximately securing residences simply—thank you lower back!! Security Camera Installation Sanford
Every weekend i used to pay a visit this website,
because i want enjoyment, since this this web page conations
in fact good funny information too.
https://Persik-Kediri-id.com
“So many advantages come from keeping up your bushes desirable; thanks for selling information about expert services out there! professional tree experts ”
Just had the best day ever with a rented water slide at our family picnic in Tampa! tampa table rentals
Trees are pleasing, however sometimes they outgrow their space, optimal to the need for removing. tree removal and trimming
This was a fantastic read. Check out ادمین اینستاگرام for more.
My friends recommended Rancho Cordova auto shippers, and after using them, I can see why—they’re fantastic! Rancho Cordova vehicle shipping
After an accident, many people feel overwhelmed by medical bills and legal processes. A Garland personal injury lawyer can ease that burden—visit garland injury lawyer .
Thanks for sharing those web optimization guidelines! I’m going to put in force them and spot how my visitors improves. Also, look at various out Professional SEO help for more.
Thanks for the helpful article. More like this at ادمین اینستاگرام .
If you’re looking at options for your upcoming relocation, be sure to check out ###; their service is top-notch! Jacksonville apartment movers
I’m so glad I found amazing apartment movers through Jacksonville apartment movers – they took care of everything!
Can’t believe how many options there are; definitely checking out your recommended stores!! jumping rentals for parties near me
Moving day is less stressful when you have such supportive professionals like those at #movingcompany#. Fort Worth movers
Your weblog has motivated me to take action with my landscaping—I can’t wait to study even more from the authorities at local tree trimming !
Anyone used long-distance moving services recently? I’d love some suggestions; I’ve heard good things about Weirsdale movers .
An absolute must-see if budgeting matters during an upcoming change; reach out today if interested regarding anything offered via #Anyoneord#! Altamonte Springs moving companies
If you want your pavers sealed right, go with the experienced team at exterior house cleaning .
They even offered some great tips on how to maintain the cleanliness of my surfaces moving forward, showing their commitment to customer satisfaction beyond just the service itself. pressure washing service
Just got settled in Nashville thanks to the wonderful team at Long distance movers Nashville ! Highly recommend them.
My roof sparkles after a cleaning from the professionals at driveway cleaners near me !
Affordable Pricing: The value for the quality of service provided is unbeatable. Tampa Bay Pressure Washing offers competitive pricing without compromising on quality, making it accessible for homeowners. tampa pressure washing Tampa Bay Pressure Washing
Has anyone used a Kennedale moving company? I’m considering hiring one soon! Best Kennedale movers
Big shoutout to all the reliable ### anyKeyword### out there helping people relocate smoothly! Gotha moving company
Your recommendations are spot on; can’t wait to find the right tent for our annual picnic!! ### anyKeyWord ## card table rentals near me
I found this very interesting. Check out carpintería de aluminio en Coruña for more.
Anyone else had a positive experience with long distance movers in Irving? I loved using Forth Irving Mover’s !
It’s reassuring knowing that reliable options like #ANYKEYWORD# exist for businesses considering relocation! Satellite Beach movers
Searching for reliable moving companies? Long-distance movers from Zephyrhills have great reviews—find out why at Zephyrhills commercial movers !
Appreciate the thorough write-up. Find more at roof replacement near me .
Appreciate the helpful advice. For more, visit Serenity Counseling Group .
I enjoyed this article. Check out affordable commercial paving Wheat Ridge for more.
This was highly educational. For more, visit ادمین اینستاگرام .
This was quite helpful. For more, visit wood floor refinishing .
강남가라오케 프라이빗 룸의 럭셔리 인테리어와 최신 음향 시설을 합리적인 가격에!
강남룸싸롱 부럽지 않은 고품격 서비스와 강남역
인근 뛰어난 접근성까지
Chiropractic health is so important, especially living an active lifestyle! Excited to learn more from Chiropractor Lakewood .
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy attorney
Great suggestions on keeping smooth windows! I’ll basically examine out Commercial Window Cleaning for professional amenities in North York.
This was incredibly informative regarding boosting our online presence through localized strategies; seeking out a competent SEO agency Basildon # now!
Fighting style not just boost fitness yet likewise infuse technique and emphasis in specialists. It’s remarkable to see how different designs, from karate to jiu-jitsu, deal unique advantages Denver Taekwondo kids
If you’re making plans a movement in São Paulo, don’t hesitate to contact empresas de mudanças são paulo for quality carrier.
This was very well put together. Discover more at Roofers Phoenix .
If you might be searching out dependable moving services in São Paulo, I noticeably put forward checking out caminhão de mudança sp for equally residential and advertisement moves!
This was a great article. Check out for more.
Appreciate the detailed information. For more, visit Fort Worth roofing companies .
WebSite: https://repaircddvd.com
Don’t forgetthattherearemultiplefactorsaffectingoutcomesfollowinginjuries sufferedfromautocollisionsincludinginsurancecoverageandliabilityissues- speakwithanattorneytodayto understandyouroptionsbetter!!# # anyKeyWord### Thompson Law
I found this very interesting. For more, visit Houston ac repair .
I enjoyed this read. For more, visit Affordable pest extermination Hackettstown .
Thank you for emphasizing the value of having a easy and ready dwelling atmosphere! house cleaning near me
I lately wiped clean my deck the use of a 2700 PSI power washing machine and it labored like a allure! If you desire to determine a few prior to-and-after photographs, test out http://www.svdp-sacramento.org/events-details/14-03-01/E-_Waste_Collection_at_St_Lawrence_-_October_4.aspx?Returnurl=https://wiki-byte.win/index.php/Revitalize_Your_Outdoor_Space:_How_Often_Should_You_Pressure_Wash_Your_Patio_for_Maximum_Curb_Appeal%3F .
Hello There. I found your blog using msn. This is an extremely well written article.
I will be sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I will certainly return.
Appreciate the great suggestions. For more, visit Persian Therapist Near Me .
This was highly useful. For more, visit ادمین اینستاگرام .
Thanks for the great tips. Discover more at ادمین اینستاگرام .
Nicely done! Discover more at best exterminator Long Valley .
This was quite informative. More at Sewer line repair .
You can certainly see your enthusiasm in the article you write.
The sector hopes for even more passionate writers like you who aren’t afraid to mention how they
believe. Always go after your heart.
I’m planning on the usage of slate tiles for my patio discipline; they’re each wonderful and sturdy for outdoors use! hardscape contractors
I’ve heard mixed reviews about buying backlinks, but my experience with Backlinks for sale has been positive!
Your discussion on darkish mode innovations in information superhighway design is rather timely; it’s becoming increasingly widely used between customers! Check out extra at Affordable web design company !
“This article helped me realize how important it is to choose the right moving company like Cheap movers Grand Prairie !”
I love how each year brings new Limited Edition Gibson Les Paul’s; they are always so unique! Which ones have caught your eye? Join discussions over at Les Paul Nitrocellulose Finish !
The development of out of doors kitchens is astounding! Cooking outdoor is such a fun knowledge. Find methods on creating your possess at luxury outdoor living .
This was highly useful. For more, visit Tub refinishing in Atlanta .
“Just finished unpacking after using an incredible mover that was suggested by friends who read about them on Burleson movers #!”
Have you ever considered writing an e-book or guest authoring on other blogs?
I have a blog centered on the same ideas you discuss and would really like to have you share some stories/information. I
know my readers would appreciate your work. If you are even remotely
interested, feel free to send me an email. http://dragon-Slave.org/comics/JaidhTannerje
I liked this article. For additional info, visit plumbing companies .
Have you ever considered writing an e-book or guest authoring on other blogs?
I have a blog centered on the same ideas you discuss and would really like to have you share some stories/information. I know my readers would appreciate your
work. If you are even remotely interested, feel free to send
me an email. http://dragon-Slave.org/comics/JaidhTannerje
This was very beneficial. For more, visit emergency plumber .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Restoration Near Me
Thanks for the clear breakdown. More info at fire damage restoration services near me .
This was a fantastic read. Check out cocinas en Granada for more.
Thanks for the valuable article. More at nutrióloga barata en Saltillo .
I agree wholeheartedly on the topic of conserving consistency across structures when pursuing an included attitude closer to virtual marketing—it strengthens logo id well too; see same discussions over ## Best SEO agency
It’s good how doing away with simply one problematic tree can amendment the overall vibe of your backyard! affordable tree removal
Thanks for the insightful write-up. More like this at ادمین اینستاگرام .
“To ensure safety measures are taken seriously during transport—just ask the folks over at #### anykeyword####!” Rancho Cordova auto shippers
The crew from Best North Richland Hills movers was friendly and professional throughout my entire move.
Can someone recommend specific services offered by Long distance movers Allen #?
This is exactly what I was once purchasing for related to tree healthiness and aesthetics! Excited to delve deeper into professional tree trimming .
Relocating can be stressful, but not when you have resources like those on Jacksonville apartment movers to guide you.
Sweet satisfaction realized upon completion facilitated primarily enabled outcomes curated directly tied back towards materials distributed widely among communities frequented via engagement reflected back upon results yielded expressed near ## Fort Worth moving company
Very informative article showcasing benefits derived from collaborative workflows leads toward efficient outputs ultimately benefiting all parties involved Website design and development services
Appreciate the insightful article. Find more at TheWinnslow .
We’re proud to deliver custom home remodels in Sumner that reflect each homeowner’s unique taste and lifestyle.
Home Remodel Sumner
I recently completed a Bellevue bathroom remodel, and I couldn’t be happier with the results! The transformation was incredible, and it has made such a difference in my daily routine Home Remodel Sumner
Courageously stepping outside comfort zones proves necessary yet rewarding often yield unexpected results providing opportunities growth sparked positive change initiated through collaborative efforts shared between parties partnered together successfully Cheap movers Kennedale
Article writing is also a fun, if you know then you can write otherwise it is complicated to write. http://dragon-slave.org/comics/PhilippfdBowlernm
Appreciate the thorough information. For more, visit Pest Management Hackettstown .
Article writing is also a fun, if you know then you can write otherwise it is
complicated to write. http://dragon-slave.org/comics/PhilippfdBowlernm
This was quite informative. More at foothills paving and maintenance .
Mic Glass specializes in the fabrication of various architectural glass such as clear glass, tinted glass, frosted
glass, painted glass, printed glass, textured glass and laminated glass.
All our glass is safety tempered glass meeting the industry
standard ANSI Z97.1
With the complete supply chain of glass fitting and hardware kit in China,we
are able to provide finished glass building products including interior partition, shower enclosure,
interior door, balustrade, wardrobe, lighted mirror and furniture top, focus on hospitality industry.
Enquiry to tailor make your glazing project. Whether
you are designer and architect, developer, builder, contractor or property management companies, we
are able to supply the architectural glass products with competitive price and in time delivery for your project.
This was highly helpful. For more, visit ادمین اینستاگرام .
This was a great article. Check out shower refinishing near me for more.
This is such an informative article! I’m at all times shopping for new tactics to enhance my canine’s behavior. I determined some titanic information at https://wakelet.com/wake/XAW1ylJX3IvxzQKXTanb6 that complements your feedback.
ความสะอาดของร้านเหล้าสาย1 ทำให้รู้สึกมั่นใจในการใช้บริการมากขึ้นครับ ผับแอนด์เรสเตอรองท์ สาย1
Great tips! For more, visit LuxNuro .
From my sense, due to empresas de mudanças são paulo # turned into probably the most most competitive judgements I’ve made although relocating within São Paulo.
Curious about how sandblasting works? I found some great resources at Graffiti Removal that explain everything you need to know!
I loved how responsive Jeff Lassila was to my questions! You can find out more at homeowners coverage Michigan .
This was highly useful. For more, visit hardwood floor .
No one enjoys moving, but with services like caminhão de mudança sp in São Paulo, it becomes plenty easier!
If you’re dealing with a rat infestation, it’s crucial to address it quickly to prevent health risks and property damage. Effective rat removal techniques can make a significant difference in maintaining a safe and clean environment Pest control
This was a great article. Check out Affordable Pest Solutions for more.
Does your team cover surrounding areas outside of Renton as well? I’m curious if you travel! Dryer Duct Cleaning
Great job! Find more at Afordable Pest Solutions .
Thanks for the clear breakdown. More info at local Shower reglazing .
รู้สึกว่าร้านเหล้าสาย1 มีโปรโมชั่นดีๆ เยอะเลยครับ ร้านอาหารบางแค
memekillegal contentmalwarespammysitus porno
Has any one used a shrewdpermanent digital camera machine? Would love a few suggestions in the past you make a decision! Video Surveillance Installation
Thanks for your personal marvelous posting! I seriously enjoyed reading it, you’re a great author.I will ensure that I bookmark your blog and will eventually come back sometime soon. I want to encourage you continue your great job, have a nice morning! best classroom headphones for learning
Great discussion on the ethics of drone pictures and respecting privacy rights! A will have to-learn for all drone fanatics! More insights at https://corrilkski.livejournal.com/profile/ .
I enjoyed this article. Check out Beverly Hills Dental Group for more.
I found this very interesting. Check out https://www.bitsdujour.com/profiles/auVTp5 for more.
I love hearing stories about how people found their perfect Gibson Les Paul’s; every guitar has its tale! What’s yours?! Tell us over at Les Paul Gloss vs Satin
If you’ve been Googling remodeling contractors near me, you’ve found the right crew — local, experienced, and client-focused.
Sumner Home Remodel
Appreciate the insightful article. Find more at The Inn at New Hyde Park – Wedding & Corporate Event Venue .
This was highly helpful. For more, visit ادمین اینستاگرام .
This was a fantastic read. Check out Affordable Pest Solutions for more.
This was highly educational. More at ادمین اینستاگرام .
Very informative post! I appreciate the advice on finding a good Basildon SEO Agency to help with my website. SEO agency Basildon
Thanks for the comprehensive read. Find more at carpintería de alumino A Coruña .
Appreciate the comprehensive insights. For more, visit Conner Roofing, LLC .
. Your tips on comparing plans based on personal healthcare needs are invaluable—thanks so much!! Health Insurance
Well done! Find more at Mr. Clean Power Washing, LLC .
This article really highlights the importance of understanding hormone therapy. I can’t wait to explore more at Centralia Medical Spa !
Thanks for the useful post. More like this at Summers Plumbing Heating & Cooling .
Thanks for the clear breakdown. More info at Serenity Therapy Group .
Your section on time-saving cleansing hacks used to be very insightful! house cleaning
Your article has inspired me to take in drone pictures as a activity! Excited to be told greater thoughts from you! Visit https://anotepad.com/notes/bmddbjhi for greater info.
Appreciate the thorough insights. For more, visit Foot Hills Paving .
My brother recommended I would possibly like this blog. He was totally right.
This publish actually made my day. You cann’t consider simply how much time I had
spent for this information! Thank you! https://porno-gallery.ru/user/MuhammadTrudel/
My brother recommended I would possibly like this blog. He was totally right.
This publish actually made my day. You cann’t consider
simply how much time I had spent for this information! Thank you! https://porno-gallery.ru/user/MuhammadTrudel/
The emphasis on responsible marketing practices in the industry highlighted by Bulk Ammunition, Gun Parts, & More! is important for future growth.
Appreciate the detailed insights. For more, visit Best Bathtub resurfacing Atlanta .
Thanks for the thorough article. Find more at comprehensive treatment for brain mapping Denver .
The way light reflects off newly installed copper copper cupolas is just mesmerizing! barn cupola
Very useful post. For similar content, visit Somers Plumbers – Phoenix Plumbing Company .
Useful advice! For more, visit ادمین اینستاگرام .
This was very well put together. Discover more at personal injury lawyer .
Just wanted to recommend North Richland Hills apartment movers #; they exceeded my expectations during my move.
Woah! I’m really loving the template/theme of this site. It’s simple, yet effective.
A lot of times it’s difficult to get that “perfect balance” between superb usability and appearance.
I must say you’ve done a awesome job with this. In addition, the blog loads very fast for me
on Chrome. Superb Blog! https://www.dealigg.com/shop.php?url=http://dragon-Slave.org/comics/SoilanmKeechyd
Woah! I’m really loving the template/theme of this site.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between superb usability and appearance.
I must say you’ve done a awesome job with this.
In addition, the blog loads very fast for me on Chrome.
Superb Blog! https://www.dealigg.com/shop.php?url=http://dragon-Slave.org/comics/SoilanmKeechyd
Great tricks on affirming clean windows! I’ll certainly examine out Window Cleaning North York for skilled functions in North York.
This was highly educational. For more, visit deck companies near me .
Fantastic post! Discover more at best termite control in Flanders .
Honored proud support community members inspiring positive changes while promoting sustainable practices across board; clear choices lead toward ultimate goals achieved together(###)! Mulberry Mover’s
Wonderful tips! Discover more at quick urgent care dentist Beverly Hills .
I appreciated this post. Check out ادمین اینستاگرام for more.
What are some lesser-prevalent dog breeds that folks should contemplate adopting? http://msichat.de/redir.php?url=https://jasperfzvz461.theglensecret.com/captive-care-of-the-north-american-field-turtle
A heartfelt thank you goes out everyone involved making this possible turning dreams into reality transforming aspirations visions becoming tangible manifestations lived experienced firsth Brandon car transport
Great experiences matter when moving! That’s why I’d suggest using local movers like Cheap movers Crystal River in Crystal River.
Check out the latest update PSBS Biak
Thanks for the useful suggestions. Discover more at vinyl pool construction .
If you need a trustworthy car mover in Miami, I suggest checking out Miami car shippers .
This was a wonderful guide. Check out The Water Heater Warehouse for more.
“Anyone else excited yet nervous about starting fresh after relocating into beautiful new surroundings?” ## Pomona Park moving company
Thanks for the clear breakdown. More info at best plumbers .
I appreciate everyone’s input here; it’s made navigating these waters far less daunting as shown by # # anyKeyWord ## Doral auto transport
Can’t wait to hear updates from those who use ___ # St Cloud auto shipping
Appreciate the detailed insights. For more, visit water damage restoration companies near me .
High hopes after hearing such positive things about **/*/*/*/*/*/*/*/*/*/*/*/*/*/*/*/*/*/*/*/ Jupiter vehicle shippers
It’s actually a great and helpful piece of info. I am satisfied that you just shared this useful information with us.
Please keep us informed like this. Thanks for sharing.
Just booked my Spring Hill vehicle shipping; excited to see how it goes! Spring Hill car transportation services
Everyone should know about # any Keyword#! They provide outstanding service that’s hard to match! Sanford car shippers
The process with Weston car shippers was seamless thanks to the guidance from Weston auto transport company .
Just saved this page since I’ll be visiting #TheVillag es#. It’s super informative! Sunshine Auto Transport’s The Villages
Thanks for the useful post. More like this at Effective termite control Hackettstown .
I didn’t realize how much planning goes into an office move until I started working with Long distance movers Tangerine !
Just got my new refrigerator from a local appliance store, and I couldn’t be happier with my purchase from appliance warehouse !
Just had the best moving experience ever with Cheap movers Palatka ! Highly recommend them!
Hydrojetting is something everyone should consider if they have recurring drainage problems; it’s efficient and effective according to my experience! water heater installation
Helpful suggestions! For more, visit community Farsi counseling resources .
Seeing others become areas encourages movement—knowing what’s seemingly drives motivation sky top!!!!!! ## https://rapid-wiki.win/index.php/Achieving_a_Pristine_Walkway:_Manual_Methods_for_Cleaning_Concrete
Amazing how something as simple as a clean duct can make such a difference in appliance performance! Dryer Vent Cleaning
Appreciate the useful tips. For more, visit ادمین اینستاگرام .
Great insights! Find more at ادمین اینستاگرام .
Amazing insights right here about retaining roofs fresh! Shoutout to Roof Cleaning Cape Coral in Cape Coral!
See the highlights https://PSIS-Semarang.com
I recently completed a kitchen remodel on Mercer Island, and the transformation is unbelievable! It’s amazing how a new layout and updated appliances can completely change the feel of a home Home Remodel Sumner
The benefits of having a safety digital camera system are plain! I need to get this carried out soon. Video Surveillance Installation
Anyone else obsessed with the Les Paul’s beautiful finishes? Which one is your favorite? Share your thoughts at Les Paul P90 .
Woah! I’m really digging the template/theme of this site.
It’s simple, yet effective. A lot of times it’s very difficult to get that “perfect balance” between user friendliness and appearance.
I must say you have done a amazing job with this. In addition, the blog loads very fast for me on Opera.
Exceptional Blog!
Great post! I’ve been shopping for potent innovations to teach my dog. The tips you shared are somewhat beneficial! I came upon greater sources in this subject matter at https://padlet.com/devpage7hyvur/bookmarks-pajk481hccjx95es/wish/do3MQJk6Y36lZ15w .
Fighting style not just enhance physical fitness however also instill technique and focus in experts. It’s remarkable to see just how various styles, from karate to jiu-jitsu, offer distinct advantages Denver Taekwondo classes
Hi this is kind of of off topic but I was wondering if blogs
use WYSIWYG editors or if you have to manually code with HTML.
I’m starting a blog soon but have no coding expertise
so I wanted to get advice from someone with experience.
Any help would be greatly appreciated! http://Www.engel-Und-waisen.de/index.php/Le_Club_De_D%C3%83_gustation_Vin_Qu%C3%83_bec_:_Une_Expertise_Gourmande_Et_Culturelle_%C3%83_Qu%C3%83_bec
Thanks for the thorough analysis. Find more at Kansas custom deck builders near me .
Hi this is kind of of off topic but I was wondering if blogs use WYSIWYG editors
or if you have to manually code with HTML. I’m starting a blog soon but have
no coding expertise so I wanted to get advice from someone with experience.
Any help would be greatly appreciated! http://Www.engel-Und-waisen.de/index.php/Le_Club_De_D%C3%83_gustation_Vin_Qu%C3%83_bec_:_Une_Expertise_Gourmande_Et_Culturelle_%C3%83_Qu%C3%83_bec
I liked this article. For additional info, visit fábrica de cocinas .
This was highly helpful. For more, visit water heater repair services near me .
This is highly informative. Check out carpintería de alumino A Coruña for more.
If you’re looking for reliable moving services, check out Cheap movers Lancaster for the best Lancaster movers!
Great job! Discover more at roofing service St Louis MO .
I recently had a pest issue in my home, and I was amazed by how effective the Puyallup Exterminator service was! They identified the problem quickly and implemented a comprehensive plan to eliminate the pests Pest control
Thankful opportunity granted collaborate fellow seekers seeking knowledge insight gaining awareness surrounding various aspects relating matters concerning wellbeing ultimately leading improvement quality life significantly enhancing overall satisfaction Premier Injury Clinics Arlington – Auto Accident Chiropractic
Your insights into shade grading drone pictures were enlightening; it’s such an obligatory a part of the enhancing task! More information should be discovered at https://www.mixcloud.com/vormascoeu/ .
The movers from # # anyKeword # # were steered and legit, making our transition seamless. caminhão de mudança sp
This was quite informative. For more, visit affordable central heating installation .
Thanks for the clear breakdown. Find more at urgent plumber .
Thanks for the valuable insights. More at plumbing .
This was highly helpful. For more, visit ادمین اینستاگرام .
This was a wonderful guide. Check out Local Plumbers for more.
Thanks for the detailed post. Find more at Pest Control Hackettstown .
Clearly presented. Discover more at foothills paving and maintenance .
I’ve moved several times, but this time with Greenacres moving company was by far my best experience yet! Greenacres Mover’s
Truly thankful we had professionals aboard: hats off # # Any keyword # Hialeah FL Mover’s
I appreciated this article. For more, visit neurotherapy center in Denver .
Thanks to Rockledge international movers, relocating abroad was much easier than I expected! Check out Local movers Rockledge for more details.
Has anyone compared prices between different movers? I’ve found great rates at # any Keyword#. Clearwater moving companies
#website link#: Would love hearing others’ success stories using them too over here!” Margate international movers
The chance of discovering unexpected gems makes regular visits worthwhile! appliance store Burnaby
Custom kitchen design in Bellevue is truly transforming homes! The attention to detail and personalization really makes a difference. I love how homeowners can express their style while optimizing functionality https://rentry.co/o7hidf5c
This was a great help. Check out ادمین اینستاگرام for more.
If you’re in Honolulu, don’t hesitate to reach out to an experienced residential plumbing for any plumbing issues.
Appreciate the thorough write-up. Find more at Afordable Pest Solutions .
Hopefully more people discover how essential services like ***#AnyKeyWord#*** are when relocating within ***#Kissim mee#. Sunshine Auto Transport’s Kissimmee
Just had my windows cleaned by the pros at Residential Window Cleaning #—they did an incredible job!
Fantastic breakdown of settings for distinct video resolutions and body rates on drones – very informative! For further important points, discuss with https://waylonzzxm032.wpsuo.com/the-ultimate-drone-camera-setup-equipment-and-settings-for-perfect-shots .
Nicely done! Find more at Local Pest Control Flanders .
Finding the right clinic for hormone therapy is crucial! Look no further than Centralia Hormone therapy for a comprehensive guide on what to expect.
If you’re moving within Texas, don’t forget about Cheap movers Grand Prairie for your Grand Prairie needs!
Can we take a moment to appreciate how beautiful these guitars look under stage lights?! What’s your stage setup like? Show us over at Les Paul Guitar Deals !
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Great things are said about the reliability of movers through # # anykeyword# #; definitely worth exploring if you’re relocating! 𝗧𝗵𝗿𝗲𝗲 𝗠𝗼𝘃𝗲𝗿𝘀 | 𝗕𝗲𝘀𝘁 𝗠𝗼𝘃𝗲𝗿𝘀 𝗡𝗮𝘀𝗵𝘃𝗶𝗹𝗹𝗲 𝗧𝗡
Thanks for the useful suggestions. Discover more at cocinas .
Fantastic post! Discover more at carpintería de aluminio en Coruña .
Long distance movers Osprey made my relocation so much easier than I expected! More about them at Osprey Mover’s .
I appreciated this post. Check out nutrióloga económica Saltillo for more.
I think everything published made a bunch of sense.
But, consider this, what if you added a little content?
I ain’t saying your content isn’t solid., however suppose you
added something to maybe get a person’s attention? I mean Certain Scores May Predict Which Trauma Patients Face High Risk of Multiple Infections – Healthcare Hygiene magazine is kinda boring.
You could glance at Yahoo’s front page and watch how they create article headlines
to get viewers interested. You might try adding a video or a picture or
two to grab readers interested about what you’ve
got to say. Just my opinion, it might make your blog a little bit more interesting. http://Dragon-Slave.org/comics/CarledThwaitesam
This was quite informative. For more, visit Affordable Pest Solutions .
I think everything published made a bunch of sense.
But, consider this, what if you added a little
content? I ain’t saying your content isn’t solid.,
however suppose you added something to maybe get a person’s attention? I
mean Certain Scores May Predict Which Trauma Patients Face
High Risk of Multiple Infections – Healthcare Hygiene magazine
is kinda boring. You could glance at Yahoo’s front page and
watch how they create article headlines to
get viewers interested. You might try adding a video or a
picture or two to grab readers interested about what you’ve got to say.
Just my opinion, it might make your blog a little bit more interesting. http://Dragon-Slave.org/comics/CarledThwaitesam
I recently moved across state lines and used a local shipper from Rancho Cordova; highly recommend them for long-distance moves too! Rancho Cordova auto transport companies
Appreciate the comprehensive advice. For more, visit Sewer line repair Marion .
Shipping motorcycles in Los Angeles can be a hassle, but finding the right service makes all the difference! Check out shipping motorcycles Los Angeles for great options.
Great job! Discover more at Massey Roofing & Contracting .
Many people overlook local options; search around ## Cheap movers Yulee
Thanks for the useful post. More like this at ادمین اینستاگرام .
Sharing this post because I’m super happy with the service received from ####ALLENMOVINGCOMPANY####! Cheap movers Allen
I had such a positive experience with Tito’s International Movers during my last big move abroad; highly recommend their services- visit now ## Local movers Titusville
Appreciate the recommendation. Let me try it out.
ทุกครั้งที่มีโอกาส ฉันก็จะไปที่ร้าน OMG ONE MORE GLASS SAI1 ค่ะ ไม่มีเบื่อเลย ร้านเหล้าใกล้ฉัน
Appreciate the detailed insights. For more, visit ادمین اینستاگرام .
I always recommend Crystal River Mover’s when people ask about reliable movers in the Crystal River area.
Graffiti can sometimes convey powerful messages, but when it becomes vandalism, it’s a different story. I trust services like Seattle Sandblasting to handle removal properly.
Excited about starting life in Miami! Glad I followed the leads from Sunshine Auto Transport’s Kendall for auto transport.
I’ll forever be grateful that I found out about this service called #AnyKeyWord#! Office moving companies Altamonte Springs
Most memorable moments captured weren’t just sights seen but also conversations held within those comfy seats aboard company rides ! Melbourne vehicle shipping
”Wishing everyone good luck with their upcoming shipments—make sure you reach out to ###Jupiter Vehicle Transport###!” Jupiter car shippers
I found the best Gotha moving company for my recent move, and they were fantastic! Long distance movers Gotha
Couldn’t have asked for smoother service from my chosen Weirsdale moving company via Weirsdale international movers
Just wanted to give a shoutout to the awesome service I received from Kissimmee auto shippers in Kissimmee.
I just received a shipment from _#_ __ , so thrilled ! St Cloud vehicle shipping
Understanding your rights post-accident is crucial, and that’s where a McKinney car accident lawyer comes in handy! Check out McKinney car accident lawyer for guidance.
Moving stress? Not with the help from Jacksonville apartment movers ! They made my Jacksonville move so smooth.
The staff at water damage restoration service near me was courteous and knowledgeable during my home’s restoration process. Highly recommend them!
Just moved into my new place in Irving thanks to amazing movers! Learn more about them at Office moving companies Irving .
Great job! Find more at Foothills Paving .
Hi there! This blog post couldn’t be written any better!
Looking at this article reminds me of my previous roommate!
He always kept talking about this. I will send this post to him.
Fairly certain he will have a good read. Thank you for sharing!
If you need reliable car shippers in Wesley Chapel, don’t hesitate to contact Wesley Chapel auto shipping !
Did anyone ever consider using ride-sharing instead instead ? Curious if that would work as an alternative solution while relocating cars !! ###AnyKeyWord## The Villages auto transport companies
This was highly educational. For more, visit Pure Plumbing Company .
This was very enlightening. More at LuxNeuro .
Just wanted to share my experience with a fantastic Basildon SEO Agency. They provided personalized solutions that fit my business needs perfectly! Check them out at SEO agency Basildon .
I found this very interesting. Check out basement water damage services for more.
Appreciate the great suggestions. For more, visit Sewer line repair service .
Hired # recently; they exceeded all expectations during our big day! Local movers Zephyrhills
You’ve provided amazing insights here! Don’t overlook the services offered by Where to buy backlinks that actually work when buying backlinks.
Anyone else excited about finding reliable local services right here?! Definitely makes life easier when emergencies arise!!! emergency air conditioning repair
“If you need help with your next business move, give #anyKeyword# a call—you won’t regret it!” Satellite Beach commercial movers
Moving doesn’t have got to be challenging; simply name empresas de mudanças são paulo and let them take care of it excited by you!
Thanks for the detailed post. Find more at top expert pest control in Flanders .
The performance of caminhão de mudança sp all through our commercial relocation used to be without a doubt unbelievable!
Thanks for the great information. More at ادمین اینستاگرام .
Anyone else think that community resources like ### anyKeyword### are essential for keeping our homes safe from water issues? restoration companies in my area
This was very beneficial. For more, visit Beverly Hills Dental Group .
This was quite informative. More at animal hospital Jacksonville .
Thanks for sharing your experience! I’m considering a visit to a Lakewood chiropractor and will check out Chiropractor Lakewood .
Knowing what steps to take immediately after discovering water damage can save so much time and money! restoration companies in my area
Appreciate the detailed post. Find more at Vedder Roofing & Construction .
Sharing stories experiences allows growth underst water damage restoration service near me
Helpful post on handling emergencies related to water damage—always remember you can count on ###for support in Clive! restoration companies in my area
I enjoyed this read. For more, visit https://maps.app.goo.gl/rB5QKFd4X6D1SihcA .
Appreciate the comprehensive advice. For more, visit NYC bar with private room options .
I am truly happy to read this webpage posts which consists of tons of valuable data, thanks for providing these statistics.
How do you stay encouraged while apartment cleaning appears like a under no circumstances-finishing mission? Asking for a chum…or me, haha! house cleaning near me
Many people fear that bankruptcy will ruin their credit forever, but that’s not necessarily true. With proper planning and financial management post-bankruptcy, individuals can gradually rebuild their credit score bankruptcy lawyer
. What better way than through collaboration amongst community members striving towards overall well-being together? # Health Insurance Cape Coral
Great advice given by staff made my decision-making process so much smoother while browsing through $. appliance store Burnaby
I enjoyed this article. Check out ادمین اینستاگرام for more.
Fighting style not just improve physical fitness yet likewise instill discipline and focus in professionals. It’s fascinating to see exactly how various designs, from martial arts to jiu-jitsu, deal unique benefits kids karate denver
When it comes to commercial plumbing projects, make sure you’re working with qualified professionals like our trusted ### anyKeywords###! local plumber
This was very well put together. Discover more at https://numberfields.asu.edu/NumberFields/show_user.php?userid=5977317 .
This is highly informative. Check out Summers Plumbing Heating & Cooling for more.
Very useful post. For similar content, visit https://maps.app.goo.gl/f8b3rVyoodYyjEdY7 .
See the highlights https://Semen-Padang-FC.com
Thinking of relocating? Local Movers have got your back! Explore their services through Cheap movers Mulberry .
Bir dakikadan başlarken iki dakika veya maximum üç dakika bekleyebilirsiniz.
Appreciate the detailed insights. For more, visit Affordible Pest Solutions .
Anyone else think that adding a weathervane atop a copper copper cupola makes it even more charming? cupola ideas
Just wanted to share that my experience with Yalaha commercial movers was nothing short of excellent!
Couldn’t have asked for better service from #Rockledgemovingcompany## – thank you! Rockledge commercial movers
I for my part choose utilising a 3000 PSI strain washer for my deck since it fairly gets into these demanding spots. You can discover more marvelous insights at http://www.smokymountainadventurereviews.com/goto.php?url=https://wiki-coast.win/index.php/Choosing_the_Right_PSI:_How_Much_Pressure_Washer_Power_Do_You_Need_to_Effectively_Clean_Your_Deck%3F_66307 .
Cheap movers don’t compromise on quality; just look at Best Margate movers ’s reviews!
I never realized how crucial dryer vent cleaning is until I read this. Thanks for the information! Laundry Dryer Vent Cleaning
Wonderful tips! Discover more at car accident doctor Boise ID .
Does anyone have tips on how to maintain the benefits of chiropractic care between visits to a #BonneyLakeChiropractor? # https://zenwriting.net/ossidyzbcc/h1-b-discover-the-benefits-of-seeing-a-chiropractor-in-bonney-lake-a-6vbn
The excitement on my kids’ faces when they saw the rented water slide was priceless! party rental table and chairs
This was a fantastic resource. Check out for more.
Clearly presented. Discover more at .
Great insights on backlink strategies! I’m itching to try the services offered by Buy guest post backlinks soon.
Love your emphasis on mobile optimization—it’s critical as users shift to mobile devices increasingly; find deeper insights into mobile trends over ###anKeyWord## marketing blog
Thanks for the great tips. Discover more at cocinas .
I found this very interesting. For more, visit carpintería de alumino A Coruña .
Appreciate the insightful article. Find more at nutrióloga en Saltillo .
Thanks for the valuable insights. More at ادمین اینستاگرام .
Just moved to Sanford and looking to install a protection approach—this weblog is ideally suited timing! Video Surveillance Installation
This was highly useful. For more, visit ادمین اینستاگرام .
I love how versatile the Les Paul is for different genres. What’s your go-to style? Join the conversation at Les Paul Tribute Models .
What’s up, for all time i used to check web site posts here in the early
hours in the dawn, for the reason that i like to gain knowledge of
more and more.
It’s fascinating how hormone therapy can help balance mood swings and alleviate symptoms. I learned so much from this article! Visit Hormone Therapy for more details.
Thanks for the great information. More at All Dry Services of Seattle .
I wish I had known about the resources on Long distance movers Burleson sooner when looking for a Burleson mover!
I enjoyed this article. Check out trusted personal injury lawyer for more.
I’ve heard mixed reviews about some movers in Yulee, so it’s nice to see a curated list! Yulee movers
Thanks for the clear advice. More at TheWinnslow .
Thanks for the great content. More at Afordable Pest Solutions .
Every aspect of my move was handled perfectly by #AnyKeyWord#. Great value overall! Altamonte Springs moving companies
Great job! Find more at roofing contractor services near me .
Hydrojetting worked wonders on our clogged drains; grateful for our knowledgeable local residential plumbing #!
“So many choices when it comes down choosing between different companies but ultimately went with one suggested here: @ !” Long distance movers Gotha
Excellent post on navigating an office move! Be sure to visit Weirsdale moving companies for further assistance.
Appreciate the thorough write-up. Find more at LuxeNeuro .
Moving can be overwhelming, but with the right help from Irving movers , it can be a breeze!
Appreciate the thorough insights. For more, visit https://usellbuybid.com/user/profile/3094125 .
Appreciate the comprehensive insights. For more, visit gas plumber near me .
Appreciate the thorough analysis. For more, visit ادمین اینستاگرام .
My family just moved within Nashvile using ** #** anykeyword** ** and we couldn’t be happier with their service—thank you so much! Long distance movers Nashville
Thanks for the useful suggestions. Discover more at affordable emergency pest control Long Valley .
I was impressed by how organized the Kennedale moving company was during my move. Cheap movers Kennedale
Training can be a limitation, however your doorstep-by-step manner makes it seem to be doable! I’ll unquestionably be sorting out https://papaly.com/8/HsQm for extra guidance tricks.
Thank you, Osprey moving companies, for making our family’s transition so smooth and easy! Long distance movers Osprey
The expertise of water damage restoration services near me made my water damage situation manageable! Thank you for your hard work!
Custom kitchen design in Bellevue is truly transforming homes! The attention to detail and personalization really makes a difference. I love how homeowners can express their style while optimizing functionality Sumner Home Remodel
Moving can be stressful, but the local movers from Local movers Zephyrhills in Zephyrhills took care of everything for me!
I found my long distance movers in Satellite Beach through a friend’s recommendation, and they did an amazing job! Satellite Beach movers
Thanks for the clear advice. More at https://maps.app.goo.gl/DAE7VS1k2SKMWx5K9 .
Appreciate the great suggestions. For more, visit Afordable Pest Solutions .
Callinguponfriendsorfamilymemberswhomighthavepriorexperienceworkingwithlawyerscouldhelpidentifypotentialcandidatesworthconsultingintheeventoffutureincidents!!!! ###Anykeyword#### McKinney personal injury lawyer
Excited about implementing some of these ideas and finding an experienced ###anSEO### partner who understands our goals! SEO agency Basildon
Cherishing every single connection made along journey filled excitement discovery inspiring personal growth enabling deeper underst ac repair
This was a great help. Check out cocinas en Granada for more.
Thanks for the insightful write-up. More like this at carpintería de alumino A Coruña .
This was quite helpful. For more, visit nutrióloga Saltillo .
The notion of the “10-minute tidy” has transformed my evenings dramatically—thank you for that tip! house cleaning service bay area
This was very beneficial. For more, visit Budd Lake residential pest services .
Kudos once again directed firmly toward active participants fueling discussions exploring meaningful connections centered around excellence displayed throughout respective journeys shared regularly! Kissimmee car shippers
Just had a flooding incident, and thankfully there are excellent restoration services right here in Irving TX! water damage restoration service near me
I’m considering adding another Les Paul to my collection; any recommendations? Let’s help each other out at Les Paul Value .
If you’re dealing with a rat infestation, it’s crucial to address it quickly to prevent health risks and property damage. Effective rat removal techniques can make a significant difference in maintaining a safe and clean environment Local Pest Control Company
The team of workers at empresas de mudanças são paulo had been not best effective however also especially friendly all over our transferring task.
I’ll on no account fail to remember approximately pre-treating stains lower back after seeing how a very powerful it’s far for prime outcome!!! ## https://aged-wiki.win/index.php/Cleaning_Challenges%3F_Overcoming_Tough_Stains_on_Concrete_Sidewalks
Your guide on finding a trustworthy chiropractor in Mill Creek is just what I needed! Chiropractor
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Has anyone tried the services of water damage restoration service near me ? I’ve heard good things about their water damage restoration efforts in Irving, TX.
The crew at caminhão de mudança sp have been no longer best green yet also totally pleasant at some stage in our moving task.
Such crucial conversations happening around town lately regarding preparedness which hopefully inspires action among others facing similar circumstances nearby too!!!! #Anykeword# water damage restoration service near me
Wow, I didn’t realize how quickly things could escalate with water issues! Glad there are solutions like those offered by water damage restoration companies near me in Clive.
Thanks for the valuable insights. More at Serenity Counseling Group .
Thanks for the useful post. More like this at ادمین اینستاگرام .
Appreciate the comprehensive advice. For more, visit foothills paving and maintenance .
If you wish for to get much from this article then you
have to apply these methods to your won weblog. https://www.younganalporn.com/aimc/yrb.cgi?aimc=1&s=65&u=http://Dtyzwmw.com/comment/html/?123650.html
If you wish for to get much from this article then you have to apply these methods to your won weblog. https://www.younganalporn.com/aimc/yrb.cgi?aimc=1&s=65&u=http://Dtyzwmw.com/comment/html/?123650.html
This design is incredible! You most certainly know how
to keep a reader entertained. Between your wit and your videos,
I was almost moved to start my own blog (well, almost…HaHa!)
Fantastic job. I really enjoyed what you had to say, and more than that, how
you presented it. Too cool!
Thanks for the great information. More at comprehensive brain assessment Denver .
Appreciate the useful tips. For more, visit ادمین اینستاگرام .
Thanks for the insightful write-up. More like this at DSH Homes and Pools .
Looking for great value? The cheap movers at Mulberry commercial movers made my move so easy in Mulberry.
Amazing article on taking pictures wildlife by using drones; it’s beautiful how expertise can guide us have a look at nature respectfully! Learn greater programs at https://zionclhv391.wordpress.com/2025/07/10/safety-first-best-practices-for-flying-and-using-your-drone-camera-responsibly/ .
It’s fascinating how hormone therapy can help balance mood swings and alleviate symptoms. I learned so much from this article! Visit Centralia Hormone therapy for more details.
I’m eager to implement some of your innovations in my very own domestic; would like me success! art’s cleaning
My recent experience with movers from Best North Richland Hills movers was outstanding! They are definitely worth considering.
Awesome article! Discover more at año escolar en Irlanda .
This was very enlightening. For more, visit Flanders pest control management .
The convenience of using a local service like shipping motorcycles Los Angeles for motorcycle shipping is unbeatable!
I appreciated this article. For more, visit Emergency Dentist Beverly Hills .
I want to to thank you for this fantastic read!!
I absolutely loved every bit of it. I’ve got you bookmarked to check out new stuff you post…
Love hearing recommendations from fellow enthusiasts regarding favorite locations dedicated solely towards displaying fine examples craftsmanship displayed proudly tourism attractions exist worldwide!!!##Anykeyword## barn cupola
This was quite informative. More at Afordable Pest Solutions .
I currently cleaned my deck making use of a 2700 PSI pressure washer and it worked like a attraction! If you want to look a few prior to-and-after pix, look at various out http://www.pageglimpse.com/external/ext.aspx?url=https://ericklbqm790.bearsfanteamshop.com/choosing-the-right-psi-how-much-pressure-washer-power-do-you-need-to-effectively-clean-your-deck-1 .
Thanks for the detailed guidance. More at intimate bars in NYC .
This was a fantastic resource. Check out ادمین اینستاگرام for more.
I am not certain the place you’re getting your info, however great topic.
I must spend a while finding out much more or understanding more.
Thank you for magnificent information I was in search of this
info for my mission. http://patandsharonterry.com/__media__/js/netsoltrademark.php?d=sl860.com%2Fcomment%2Fhtml%2F%3F237260.html
Shopping locally has its perks, especially when it comes down to finding amazing discounts like those available through $$. appliance store Burnaby
I am not certain the place you’re getting your info, however great topic.
I must spend a while finding out much more or understanding more.
Thank you for magnificent information I was in search of this info for my mission. http://patandsharonterry.com/__media__/js/netsoltrademark.php?d=sl860.com%2Fcomment%2Fhtml%2F%3F237260.html
This was a wonderful post. Check out Affordable Pest Solutions for more.
Every trip I’ve taken with Melbourne car moving companies has been smooth and enjoyable—kudos to their amazing team in Melbourne!
If you’re in need of Miami car shippers, don’t hesitate to contact Sunshine Auto Transport’s Kendall . They’re the best!
The convenience of using Kissimmee car transportation services for Kissimmee auto shipping cannot be overstated!
Appreciate the useful tips. For more, visit ادمین اینستاگرام .
Shipping your vehicle cross-country can be daunting; glad there’s a resource like this for #BoyntonBeach residents: ## Boynton Beach car shippers
Thank you for clarifying the timelines involved in homestead car shipping; that was really helpful! Homestead car transportation services
Thanks for the helpful article. More like this at Groene Hart Klimaatregeling Pro .
This was quite informative. More at Affordable Pest Control Long Valley .
My family used ### anykeyword# last summer and we were thrilled with their service! Best Ocala movers
Big shoutout to Greenacres Mover’s for making my move hassle-free. You guys rock! Cheap movers Greenacres
I blog quite often and I seriously appreciate your content.
Your article has truly peaked my interest. I’m going to book mark
your blog and keep checking for new information about once a week.
I subscribed to your RSS feed as well. http://Dragon-Slave.org/comics/ShadylSommerladgk
I blog quite often and I seriously appreciate your content.
Your article has truly peaked my interest. I’m going to book mark your
blog and keep checking for new information about once a week.
I subscribed to your RSS feed as well. http://Dragon-Slave.org/comics/ShadylSommerladgk
My friend recommended a Lakewood chiropractor, and I’m eager to learn more about their services at Lakewood Chiropractor !
Quick tip: When moving in Plant City, definitely consider contacting Plant City full service movers
Need help with your next pass? Look no added than empresas de mudanças são paulo ; they may be the perfect option in São Paulo!
Thanks to Office moving companies Clearwater , I managed to stay within budget during my last move in Clearwater.
Looking ahead to utilizing ### anyKeyWord### back for destiny strikes—they set the bar prime with their provider good quality! caminhão de mudança sp
This was highly informative. Check out ادمین اینستاگرام for more.
Wow! What a great resource this is—I’m eager to connect further regarding potential partnerships explored via firms identified herein including particularly noteworthy mentions corresponding aligned interests promoted suitably achieving mutual goals Grand Prairie movers
Well done! Find more at ادمین اینستاگرام .
My search for affordable moving help led me to some incredible deals right here in Cocoa; highly recommend checking them out!! Best Cocoa movers
Mercer Island is such a beautiful place to live, and home remodeling can truly enhance its charm! I recently completed a project that transformed my living space into a more functional and inviting area Sumner Home Remodel
Appreciate the detailed information. For more, visit TheWinslo .
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy attorney
Fighting style not only enhance physical conditioning however additionally impart self-control and emphasis in experts. It’s interesting to see exactly how different styles, from martial arts to jiu-jitsu, offer unique advantages kids karate denver
The new ##appliance warehouse## in town has a vast collection of kitchen and laundry appliances. scratch and dent appliance store
The resources provided here can really help demystify Medicare insurance choices for many! Cheap Health Insurance Cape Coral
I enjoyed this article. Check out Affordible Pest Solutions for more.
ไฟหน้ารถ LED กับการขับขี่กลางคืน เป็นยังไงบ้างครับ? ร้าน ทํา ไฟรถยนต์ ใกล้ ฉัน
Love the emphasis on sure reinforcement! It makes this kind of difference in instructions. If you’re concerned with greater counsel, seek advice from http://www.video-bookmark.com/user/kittanolnu for additional instruments!
I’ve subsequently found out the surest web page for topping up Genshin crystals at an low priced cost! If you’re interested, the following’s the hyperlink: top up on ManaBuy .
คุณเคยลองเปลี่ยนมาใช้ระบบแสงประเภทนี้แล้วหรือยัง? ### ร้านเปลี่ยนหลอดไฟรถยนต์
Appreciate the detailed post. Find more at motor vehicle accident lawyer for injury .
Thanks for the useful suggestions. Discover more at LuxNuro .
Hydrojetting was the best decision for my clogged drain, thanks to the recommendations from my reliable residential plumbing .
We are a group of volunteers and opening a new scheme in our community.
Your web site provided us with valuable info to work on.
You have done a formidable job and our entire community will
be thankful to you.
Nicely detailed. Discover more at Affordible Pest Solutions .
This was very beneficial. For more, visit wood floor buffing .
I recently had a pest issue in my home, and I was amazed by how effective the Puyallup Exterminator service was! They identified the problem quickly and implemented a comprehensive plan to eliminate the pests Pest Control Puyallup
If you’re looking into moving your vehicle soon, definitely check out ### anykeyword ###—they’re based right here in **Kissimmee**! Kissimmee auto shipping
What do you suggest as a primary step for an individual beaten with the aid of their mess? house cleaning near me
Thanks for the helpful article. More like this at residential plumber .
Nicely done! Discover more at http://olm.nicht-wahr.de/mybb/member.php?action=profile&uid=3149651 .
Thanks for the helpful advice. Discover more at Eco-Friendly Pest Control Flanders .
Great job! Discover more at http://yaltavesti.com/go/?url=http://forum.ttpforum.de/member.php?action=profile&uid=406576 .
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
After using several different companies, I can confidently say that #localmovers# at # anykeyword# are among the best around! Zephyrhills movers
Your information for practising nontoxic flight paths are valuable! Safety must consistently come first whilst flying drones. Explore more security hints at https://www.divephotoguide.com/user/ebulteyadr/ .
My partner and I stumbled over here from a different page and thought I might as well check things out.
I like what I see so now i’m following you.
Look forward to finding out about your web page repeatedly. https://dragon-slave.org/comics/LetaslThorpmr
Thanks for the detailed post. Find more at Afordable Pest Solutions .
My partner and I stumbled over here from a different page and thought I might as well check things out.
I like what I see so now i’m following you. Look forward to finding out
about your web page repeatedly. https://dragon-slave.org/comics/LetaslThorpmr
I’ve been surfing online more than three hours today, yet I never found any interesting article like yours.
It is pretty worth enough for me. In my opinion, if all web owners and bloggers made good content as you did, the internet will be much more useful than ever before.
Thanks to Local movers North Richland Hills , my move was smooth and hassle-free.
Outstanding post however , I was wanting to know if you could write a litte more on this subject?
I’d be very thankful if you could elaborate a little bit
further. Cheers! http://dtyzwmw.com/comment/html/?127978.html
It’s amazing how hormone therapy can be tailored to individual needs. For those curious about the process, I found great resources at Centralia Hormone therapy .
These are truly wonderful ideas in on the topic
of blogging. You have touched some pleasant points here.
Any way keep up wrinting.
I appreciate how transparent pricing structures remain throughout dealings with brandon Auto Transport; no hidden fees here!!!## anykeyword ## Brandon car moving companies
I can’t stress enough how important it is to work with a knowledgeable Basildon SEO Agency. Their expertise has made a significant difference for my website’s performance! Visit them at SEO agency Basildon .
The weight of a Les Paul can be a lot, but that tone makes it worth it! Check out tips for handling it at Les Paul Neck Profile .
Shoutout to water and mold restoration near me for their quick response time during my family’s emergency situation!
이건 주제에서 벗어나지만, 제 최신 트위터 업데이트를 자동으로 트윗하는 위젯을 블로그에 추가할 수 있는지 궁금합니다.
이런 플러그인을 꽤 오랫동안 찾고 있었는데,
당신이 이런 것에 대해 경험이 있을지도 모른다고 생각했어요.
혹시 아는 게 있다면 알려주세요. 당신의 블로그를 정말 즐기고
있으며 새로운 업데이트를 기대하고 있습니다.
I’m extremely impressed together with your writing skills and also with the
layout to your blog. Is this a paid subject or did you customize
it your self? Anyway keep up the excellent
high quality writing, it’s uncommon to peer a great weblog like this one
today..
The customer service at Sanford vehicle shippers is top-notch! They answered all my questions about shipping from Sanford.
I never knew choosing an auto transport company could be this simple. Thanks, Sunshine Auto Transport’s St. Cloud , for the helpful tips!
What a great overview of transportation options available in The Villages! I’ll definitely use your service next time. The Villages vehicle shippers
Great job! Discover more at Sewer line repair .
Moved last month and everything went smoothly with help from a company listed under Miami auto transport !
This is a fantastic guide on Kissimmee car transport services! Additional info can be found at Kissimmee car shippers .
Impressive assessment of post-processing drone pictures! Editing can trade the whole thing. Discover greater ideas at https://chancetttu490.lowescouponn.com/the-ultimate-drone-camera-setup-equipment-and-settings-for-perfect-shots .
Has anyone tried the services of Weston car shippers? I’m curious about their reliability. Weston auto transport company
I’m looking to blank one room at a time—your tips makes it much less daunting, thank you returned! house cleaning service
Such useful tips shared here! I’ll be looking into how Buy guest post backlinks can help me build quality backlinks effectively!
Thanks for the great tips. Discover more at LuxeNeuro .
Appreciate the detailed information. For more, visit Tub refinishing in Atlanta .
I’ve heard so many positive reviews about Boynton Beach car shippers! Explore them at Boynton Beach auto shipping .
This was a wonderful guide. Check out estudiar año escolar en Irlanda for more.
Cool breeze flowing everywhere now thanks entirely owed efforts placed forth originally sought assistance very first moment possible!! air conditioning duct replacement
Just finished our corporate relocation with help from Silver Springs moving companies ! It really took the stress out of moving.
I enjoyed this read. For more, visit 24 Hour Emergency Dentist Beverly Hills .
This was quite informative. For more, visit ادمین اینستاگرام .
If you’re facing any water-related issues, don’t hesitate to reach out to a local restoration expert in Irving TX! water and mold restoration near me
I’m constantly recommending# # any Keyword#to friends who need quality sidewalks! sidewalk repair contractors queens
This is highly informative. Check out fire damage for more.
Excellent site you have here.. It’s difficult to find good quality writing
like yours these days. I truly appreciate individuals like you!
Take care!!
Great insights on office relocations! If anyone is looking for reliable help in Yalaha, check out Yalaha apartment movers .
For those moving out of state, don’t forget to look into reliable long distance movers from Plant City! Plant City commercial movers
Thanks for the informative post. More at ادمین اینستاگرام .
Thanks for the helpful article. More like this at repiping services .
Just wrapped up my move with the help of Margate moving companies ! Their team was incredibly professional!
Just moved my car across town with a local Boston service. They were fantastic! More details at Boston car shippers .
Marvelous, what a weblog it is! This weblog provides valuable data to
us, keep it up.
As a trusted Sumner home remodeling company, we’re committed to craftsmanship, transparency, and your complete satisfaction.
Home Remodel Sumner
The team worked efficiently and carefully – kudos to #Rockledgemovingcompany##! Rockledge full service movers
Anyone else feel empowered knowing there are trusted experts like ### anyKeyword### nearby if disaster strikes? water damage restoration companies near me
Found some excellent deals on moving services at Clearwater international movers #; highly recommend!
Just had a minor flood in my basement, and I’m looking for local restoration experts in Hawaiian Gardens. Any suggestions? water damage restoration services near me
Grateful for all the tips on maintaining a dry home and avoiding future damages—very practical advice here!! water damage restoration near me
Nicely detailed. Discover more at Afordable Pest Solutions .
Great points raised about identifying leaks early; knowledge is power when it comes to prevention and restoration; thanks ###for your expertise! water damage restoration near me
Appreciate the comprehensive advice. For more, visit shower refinishing company .
You can’t beat the prices on discount open box appliances at appliance store Burnaby !
Awesome article! Discover more at Affordable eco-friendly pest control Hackettstown .
This was quite informative. For more, visit pool repair service .
Residential or commercial moves can also be irritating; nonetheless it, with ### anyKeyword### by using your edge, the whole thing feels manageable. empresas de mudanças são paulo
I’m curious if there are any promotional deals offered by ###ANYKEYWORD### currently available? Mulberry Mover’s
I’ve used other movers before but none compare to what I experienced with ** #** anykeyword** ** last month—it was fantastic! 𝗧𝗵𝗿𝗲𝗲 𝗠𝗼𝘃𝗲𝗿𝘀 | 𝗕𝗲𝘀𝘁 𝗠𝗼𝘃𝗲𝗿𝘀 𝗡𝗮𝘀𝗵𝘃𝗶𝗹𝗹𝗲 𝗧𝗡
Right now it sounds like Expression Engine is the preferred blogging platform out
there right now. (from what I’ve read) Is that what you are using on your blog? http://Dtyzwmw.com/comment/html/?101769.html
This was quite enlightening. Check out Afordable Pest Solutions for more.
I liked this article. For additional info, visit SURFACE PRO REFINISHING .
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
Awesome information here! For anyone looking to enhance their SEO game, try buying backlinks from Backlinks provider .
Hello! I’ve been following your weblog for a while now and finally got the bravery to go ahead and give you a shout out from
Lubbock Tx! Just wanted to say keep up the fantastic job!
What a great way to enhance curb appeal with beautiful copper copper cupolas! cupola for shed
Our clients love how our Sumner WA remodeling projects blend modern upgrades with timeless design. Sumner Home Remodel
The stigma around bankruptcy often overshadows the reality that it can be a necessary step towards financial recovery. Understanding the different types of bankruptcy and their implications is crucial bankruptcy lawyer
Amazing how little stress comes with hiring an experienced #movingcompany#! Office moving companies Fort Worth
Awesome discussion surrounding disruptive technologies shaping future landscapes — staying ahead means adapting quickly too ; check tech updates here: ###anKeyWord ## blackhat marketing blog
Thanks for the helpful advice. Discover more at ادمین اینستاگرام .
Fighting style not just improve fitness but additionally infuse technique and emphasis in specialists. It’s fascinating to see exactly how various designs, from martial arts to jiu-jitsu, offer distinct advantages Denver karate kids
We couldn’t have asked for better assistance than what we got from ###your site### during our recent move; absolutely fantastic! Best Cocoa movers
I’m amazed at how much cleaner my house looks with freshly washed windows—your blog was spot-on! local window cleaning Maryville
Your blog is super helpful! I found local movers in Tangerine who were affordable and efficient. More at Long distance movers Tangerine .
Why stress over moving when you can hire experts? Check out Zephyrhills commercial movers for your Zephyrhills move!
This was quite enlightening. Check out Summers Plumbing Heating & Cooling for more.
If you’re critical approximately optimizing your gameplay, you are not able to leave out this website online! Every Genshin participant need to know it. Check it out: best cheap top-up ManaBuy deals .
This was highly educational. For more, visit roofing contractor near me .
Hi there, just became alert to your blog through Google, and found that it’s really informative.
I am going to watch out for brussels. I will appreciate if you continue
this in future. Lots of people will be benefited from your writing.
Cheers!
The neck on a Les Paul feels so smooth; it’s perfect for solos! What’s your favorite solo to play? Discuss at Les Paul Tune-O-Matic Bridge .
#Wholesaler household appliances# can provide significant savings if you’re on a budget. appliance store nearby
This is highly informative. Check out Bathtub resurfacing 30303 for more.
This was quite helpful. For more, visit Affordable Pest Solutions .
magnificent publish, very informative. I wonder why the other experts of this sector don’t realize this.
You should continue your writing. I am sure, you’ve a huge readers’ base already! https://Zbozi.Dama.cz/exit?offer_id=4872200719&product_id=1081181066&target_url=http://Dragon-Slave.org/comics/AmberbqDelacruzbg
This is exactly what I needed to understand the value of local SEO in Basildon! Looking forward to contacting a SEO agency Basildon .
magnificent publish, very informative. I wonder why the other experts
of this sector don’t realize this. You should continue your writing.
I am sure, you’ve a huge readers’ base already! https://Zbozi.Dama.cz/exit?offer_id=4872200719&product_id=1081181066&target_url=http://Dragon-Slave.org/comics/AmberbqDelacruzbg
Just installed a tankless water heater and love the energy savings! Definitely look into it if you’re upgrading your home systems. water heater installation has great recommendations.
This was highly informative. Check out Affordible Pest Solutions for more.
Appreciate the great suggestions. For more, visit Dental Group Beverly Hills .
Never knew how critical swift action was until I faced flooding; thankful for #Ellenwood’s own water and mold restoration near me
Such a watch-opener! I not at all learned that diverse sports require various circulate charges. This know-how will basically help me make extra told judgements transferring ahead. http://2ch-ranking.net/redirect.php?url=https://giphy.com/channel/felathkziw
What’s the best way to find a trusted chiropractor in Bonney Lake? Any tips? https://rentry.co/srfm7ezn
Very helpful read. For similar content, visit Affordable Pest Solutions .
Happy learning from others’ journeys while also sharing mine openly serves purpose inspiring further collaboration growth progress achieved collectively enhancing well-being across board immensely positively impacting local communities everywhere ac repair
Planning a residential flow in São Paulo? You must always positively be aware the products and services provided with the aid of empresas de mudanças são paulo .
This post addresses many common misconceptions about hormone therapy. I appreciate the clarity! For more insights, please visit Medical Spa .
This is quite enlightening. Check out Afordable Pest Solutions for more.
If you’re in quest of rapid and powerful transferring suggestions, appearance no added than ### anyKeyword### — they’re spectacular! caminhão de mudança sp
This was very enlightening. More at expert checkatrade plumbers .
This was quite informative. For more, visit reliable plumber .
After experiencing flooding, I realized how essential it is to have a good restoration service on speed dial—especially here in Irving TX! water damage restoration near me
Mercer Island is truly a hidden gem for outdoor living spaces! The stunning views and natural beauty make it the perfect place to create a cozy patio or a luxurious deck Sumner Home Remodel
Excellent tips on how long it takes to repair a garage door! I hope I won’t need it, but if I do, emergency garage door repair Los Angeles sounds like the way to go. Find more info
Fantastic post! Discover more at ادمین اینستاگرام .
Just discovered a leak under my sink—time to call a water damage restoration expert from Hawaiian Gardens! water damage restoration companies near me
Anyone else think that community resources like ### anyKeyword### are essential for keeping our homes safe from water issues? water and mold restoration near me
Thanks for the detailed post. Find more at estudiar año escolar en Irlanda .
I’m amazed at how much damage a small leak can do over time! For restoration services, look no further than water damage restoration companies near me in Clive.
Appreciation to my father who told me regarding this
blog, this webpage is really amazing.
Appreciate the insightful article. Find more at ادمین اینستاگرام .
The weight of a Les Paul can be a lot, but that tone makes it worth it! Check out tips for handling it at Les Paul Ace Frehley Signature .
Wow, this has opened my eyes to the possibilities of backlinks! Excited to try out Where to buy backlinks that actually work for my website.
If you’re dealing with a rat infestation, it’s crucial to address it quickly to prevent health risks and property damage. Effective rat removal techniques can make a significant difference in maintaining a safe and clean environment Local Pest Control Company
Great job! Discover more at LuxNuro .
Amazing job done by###when it came time for me to relocate—couldn’t ask for better service at such low rates!! Local movers Mulberry
This was very beneficial. For more, visit water heater repair Fullerton .
This was very enlightening. For more, visit roofing services near me .
It’s appropriate time to make some plans for the future and it
is time to be happy. I have read this publish and if I may just I desire to suggest you few fascinating things or
suggestions. Maybe you could write next articles relating to this article.
I desire to learn even more things about it! http://dragon-slave.org/comics/MableerCoppinhg
It’s appropriate time to make some plans for the future and it
is time to be happy. I have read this publish and if I
may just I desire to suggest you few fascinating things or suggestions.
Maybe you could write next articles relating to this article.
I desire to learn even more things about it! http://dragon-slave.org/comics/MableerCoppinhg
This was very enlightening. For more, visit Afordable Pest Solutions .
Nicely done! Discover more at Mr. Clean Power Washing, LLC .
I solely agree that consistency is prime in dog coaching. Your insights are spot on! For more precise publications, determine out https://padlet.com/devpage7hyvur/bookmarks-pajk481hccjx95es/wish/do3MQJk6Y36lZ15w .
The rates at # anykeyword# are unbeatable when it comes to #D oralcartransport# services ! Doral car moving companies
Do you have a spam problem on this site; I also am a blogger, and I was wanting to know your situation; we
have developed some nice practices and we are looking to swap strategies with other
folks, please shoot me an e-mail if interested. http://articomed.com/node/272084
Loving the tips shared here; don’t forget how essential it is to have a solid ### anykeyword# on your side! Office moving companies Ocala
From start to finish, my experience with Hialeah international movers was exceptional; definitely check them out if you’re moving soon: # # anyKeyWord # # . Hialeah moving company
Moving offices can be overwhelming, but the team I hired from Best Silver Springs movers made it feel effortless!
Do you have a spam problem on this site; I also am a
blogger, and I was wanting to know your situation; we have developed some nice practices and we are looking to
swap strategies with other folks, please shoot me an e-mail if interested. http://articomed.com/node/272084
I’ve been looking into Brandon auto transport options, and I stumbled upon Brandon vehicle shipping . They seem promising!
I appreciated this article. For more, visit Affordable Pest Solutions .
The reviews on different St Cloud auto transport companies were super helpful! Thanks, St Cloud car transport !
This was a great article. Check out ادمین اینستاگرام for more.
I’ve had a great experience with a Melbourne car moving company I found through Melbourne car moving companies . Highly recommended!
This is such a valuable resource for those living or visiting The Villages—thank you! The Villages car transportation services
Choosing #WestonCarShippers has been a game-changer for many people—read on! ## Weston car moving companies
“Greenacres deserves all the praise for their exemplary service during our recent household move!” Greenacres movers
Just moved my vehicle last week with a top-rated company from Sunshine Auto Transport’s Spring Hill —very satisfied!
Thanks for shedding light on Kissimmee car transport options! For additional recommendations, don’t miss Kissimmee auto shipping .
So glad I did research before picking a car mover; # anykeyword# made finding reliable options super easy! Miami auto transport
Anyone considering moving should definitely research ### for their transportation options! Homestead car moving companies
“So happy I found this company! Thank you for everything, # # anyKeywod#!” Jupiter vehicle transport
I appreciate having access more personal interactions rather than feeling lost among aisles upon aisles of identical products elsewhere! wholesale appliances
Just hired Local movers Yalaha for my move next month—hoping for a great experience!
Thanks for the practical tips. More at estudiar año escolar en Irlanda .
Very useful post. For similar content, visit ادمین اینستاگرام .
Anyone else have a positive experience with Boynton Beach auto shippers from Boynton Beach vehicle shipping ?
Wanted nothing less than professionalism throughout entire journey; thankfully that’s exactly what received every step along way courtesy team members present. Cheap movers Plant City
Time spent researching pays off handsomely when selecting carriers—look no further than what’s shared by *#* anyKeyWord*!”. Wesley Chapel car shipping
Great review of alternative capturing modes handy on drones! It has helped me recognize what works most suitable in a great number of conditions. More insights at https://www.spreaker.com/podcast/beliassrzs–6680674 .
I recently used cheap movers in Margate from Long distance movers Margate and had a fantastic experience!
Amazing service from beginning till end—highly satisfied thanks again to #Rockledgemovingcompany#. Rockledge commercial movers
When leaks occur unexpectedly contact reliable locals like ours—what would we do without their efficient detection services? commercial plumbing
Highly encourage anyone else seeking assistance regarding relocations towards reaching out directly towards their website located directly under .# .any keyword#. Clearwater movers
I appreciated this article. For more, visit groene hart klimaatregeling pro .
Excellent read—backlinks are so important! I highly recommend looking into what’s available at Best backlink services for small businesses .
Nicely detailed. Discover more at Emergency plumbing .
Thanks for the helpful article. More like this at https://www.demilked.com/author/ortionwkry/ .
Thanks for the great tips. Discover more at personal injury attorney .
Does your service also include inspections or just cleanings? Just want to clarify before booking! Vent Cleaning
Looking for hidden gemstones in Genshin? This website online has every thing you need! Every player must fee it out: affordable official recharge options ManaBuy .
This was highly helpful. For more, visit ادمین اینستاگرام .
I accurately enjoyed analyzing approximately your stories with other styles of shots possible thru a drone camera; that is inspiring to see such creativity—extra inspiration might possibly be came upon by way of touring https://orcid.org/0009-0002-8621-5469 !
I must thank you for the efforts you’ve put in writing this blog.
I really hope to see the same high-grade blog posts by
you later on as well. In truth, your creative writing abilities has inspired me to
get my very own website now 😉
Each tip you shared makes me suppose extra optimistic approximately making expert selections with regards to home safe practices!! Video Surveillance Installation
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
The lowest priced appliance store I’ve found is definitely appliance store Vancouver ; highly recommend checking it out!
I’ve noticeable such a lot of lovely blended breeds currently! Which ones stand out to you? http://mcclureandsons.com/projects/Water_Wastewater/Sumner_WWTP.aspx?Returnurl=https://louisixpb309.bearsfanteamshop.com/dog-practise-teaching-dog-not-to-leap-or-chew
Just performed a mammoth move, and I could not were happier with the provider from empresas de mudanças são paulo . They made the whole lot so mild!
Just moved my vehicle with a Boston car mover, and it was seamless! Check out A1 Auto Transport Boston for the best options.
Just accomplished our circulate with the assist of caminhão de mudança sp —they handed all our expectations!
If you’re looking into moving your vehicle soon, definitely check out ### anykeyword ###—they’re based right here in **Kissimmee**! Kissimmee auto shipping
Can we take a moment to appreciate how beautiful these guitars look under stage lights?! What’s your stage setup like? Show us over at Best Les Paul for Metal !
Thanks for the great explanation. Find more at Advanced Brain Mapping Denver .
Mercer Island is truly a hidden gem for outdoor living spaces! The stunning views and natural beauty make it the perfect place to create a cozy patio or a luxurious deck Sumner Home Remodel
Water heater installation requires precision; make sure you hire someone knowledgeable about current codes and best practices as suggested on hydrojetting .
It’s entertaining how GPM can effect no longer in basic terms performance however additionally the atmosphere. I’m excited to implement a number of those hints in my domestic! http://night.jp/jump.php?url=https://wiki-coast.win/index.php/Choosing_the_Right_PSI:_How_Much_Pressure_Washer_Power_Do_You_Need_to_Effectively_Clean_Your_Deck%3F_27097
Thanks for the thorough analysis. Find more at Dental Group of Beverly Hills .
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy attorney
This was very enlightening. For more, visit ادمین اینستاگرام .
Martial arts not only boost fitness but likewise impart technique and focus in practitioners. It’s remarkable to see exactly how different styles, from karate to jiu-jitsu, offer one-of-a-kind advantages Denver karate kids
Appreciate the thorough write-up. Find more at complete pest extermination in Flanders .
Just relocated from Neptune Beach and had an excellent experience with Neptune Beach Mover’s !
이 블로그에 스팸 문제가 있나요? 저도
블로거인데, 당신의 상황이 궁금했습니다; 우리 중 많은 몇 가지 좋은 절차을 만들었고,
다른 사람들과 기술을 교환하고 싶습니다, 관심 있으시면
메일을 보내주세요.
Hello my loved one! I wish to say that this article is awesome,
great written and include approximately all vital infos.
I’d like to peer more posts like this .
Appreciate the helpful advice. For more, visit Affordable Pest Solutions .
Hello Dear, are you genuinely visiting this website regularly, if so afterward you will
without doubt take pleasant experience. http://Articomed.com/node/289743
Every little detail discussed issues greatly whilst looking perfection right through maintenance exercises open air—all thank you once again!!! ## https://wiki-mixer.win/index.php/Removing_Graffiti_from_Concrete_with_no_Power_Washing_%E2%80%93_What_Works%3F
Hello Dear, are you genuinely visiting this
website regularly, if so afterward you will without
doubt take pleasant experience. http://Articomed.com/node/289743
The customer service at Hialeah international movers is outstanding! They answered all my questions. Check out Hialeah moving companies for more details.
It’s very straightforward to find out any matter
on net as compared to textbooks, as I found this piece
of writing at this site.
Thanks for the clear advice. More at groene hart klimaatregeling pro .
If you’re relocating in Ocala, consider using Ocala movers for a hassle-free move.
This is very insightful. Check out año escolar en Irlanda for more.
A huge shoutout goes towards all of those who assisted during this hectic time—especially #AnyKEYWORD#’s wonderful staff! Silver Springs moving company
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Thanks for the clear breakdown. More info at expert septic tank service near me .
My partner and I stumbled over here by a different web address and
thought I might check things out. I like what I see so
i am just following you. Look forward to finding out about your web page yet again.
This was quite useful. For more, visit Blocked toilets .
Appreciate the comprehensive advice. For more, visit https://classificadosnaserra.com/user/profile/299062 .
This was quite enlightening. Check out drain plumber for more.
Thanks for the informative content. More at affordable plumber prices .
Looking forward to working with ### anykeyword ### again; they truly are the best in Sanford! Sanford auto transport companies
The team at Yalaha Mover’s is fantastic! They made my move so much easier.
It’s hard to find reliable services these days—thankfully, there’s still companies like water damage restoration services near me # around!
Are there any special promotions available right now for new customers using your car services? The Villages auto transport companies
The drivers from Spring Hill car transportation services are so friendly and professional! Check out more at Spring Hill car shipping .
Their expertise shines bright compared against others encountered along way—grateful beyond words! Best Plant City movers
Can’t express enough gratitude towards staff members who’ve gone above beyond assisting customers whenever necessary… Bravo team!! Melbourne car shipping
“Let’s keep encouraging open dialogue fostering collaboration leading ultimately towards more fruitful results achieved consistently moving forward.” Kissimmee auto transport companies
I love how easy it is to compare Boynton Beach auto shippers on Boynton Beach vehicle shipping .
Appreciate the useful tips. For more, visit mold remediation Seattle WA .
Valuable information! Find more at Denver Brain Mapping Solutions .
This post provides excellent guidance on link-building practices; I’m excited about trying __ anyKeyWord__’s service! SEO backlink packages for agencies
Appreciate the detailed information. For more, visit ادمین اینستاگرام .
I’m so grateful for the advancements in hormone therapy! For those looking into clinics, I recommend checking out Medical spa to find the right fit.
Does anyone else feel like playing a Gibson Les Paul elevates their performance? It’s a must-try! More insights at Les Paul Handwired Electronics .
Very informative article. For similar content, visit Price Chiropractic and Rehabilitation .
The process of restoring from water damage is fascinating yet daunting; glad we have professionals in Irving TX! restoration companies in my area
Keep up the great work, Window Cleaning North York ! Your window cleaning services are top-notch in North York.
Thanks for the great tips. Discover more at ادمین اینستاگرام .
I seriously love your site.. Very nice colors & theme.
Did you build this amazing site yourself?
Please reply back as I’m hoping to create my own personal site and would love to learn where you got this from
or just what the theme is called. Appreciate it!
What a astounding article! Training our hairy peers is usually troublesome, but your solutions make it more convenient to be aware. For more standards, assess out https://list.ly/i/11106604 !
This was very enlightening. For more, visit Affordible Pest Solutions .
Love hearing success stories from those who’ve navigated through similar experiences successfully–makes me feel re-assured knowing help exists around us!!!#Anykeyword# restoration companies in my area
Congratulations on sharing such valuable insights into managing and restoring properties affected by flooding!! #KnowledgeIsKey water damage restoration services near me
**Variety of Packages**: They offer customizable rental packages that can include multiple inflatables or accessories like tables and chairs. This flexibility makes it easier to create a tailored experience that fits your specific needs. north redington beach 20 x 30 party tent rental
Thanks for the practical tips. More at estudiar un año escolar en Irlanda .
Moving doesn’t have got to be irritating! Try empresas de mudanças são paulo for environment friendly and pleasant service in São Paulo.
Thanks for the insightful write-up. More like this at affordable driveway paving and repair .
Thanks for the great explanation. Find more at Budd Lake community pest services .
If you’re in search of short and effective transferring treatments, seem no additional than ### anyKeyword### — they may be incredible! caminhão de mudança sp
Excellent advice on preventing water damage! If you’re facing issues, consider reaching out to water damage restoration companies near me for assistance in Clive.
#Appliance liquidators# have helped me furnish my entire kitchen affordably. appliance store Vancouver
Impressive assessment of publish-processing drone photos! Editing can swap the whole lot. Discover greater recommendations at https://www.anime-planet.com/users/heldazwbup .
Don’t wait until it’s too late—call your local ### anyKeyword ### for leak detection before problems escalate. plumber kalihi
Thanks for the great content. More at ادمین اینستاگرام .
If you’re tired of overpriced Genshin crystal desirable-ups, you have to do that web page I came across! It’s tremendous not pricey and trustworthy: top-up your UID with ManaBuy .
The clarity and brightness that come from clean windows is unmatched—thanks for reminding me of this fact! commercial window cleaning Maryville
Very insightful post! For anyone serious about SEO, buying from Quality backlinks for eCommerce websites is a must-try!
Whether you’re updating a powder room or doing a full overhaul, our team handles bathroom renovations in Sumner with care and detail.
Home Remodel Sumner
If you’re looking for affordable options, Hilliard international movers has some of the best cheap movers in Fort Liberty!
Truly believe every creation holds story worth sharing regardless size shape material used ultimately choosing showcase beauty alongside functionality beautifully intertwined seamlessly throughout entire process executed flawlessly!!##Anykeyword## cupola designs ideas
A friend recommended Best Hempstead movers when I was looking for a reliable Hempstead moving company, and I’m grateful for that!
If you want a smooth transition while moving, don’t hesitate to hire # # anyKeyWord # # ! Local Motion Moving’s
Thanks for the helpful article. More like this at ادمین اینستاگرام .
The cost of moving can add up; make sure to get quotes from various companies through Melrose movers before deciding!
‘In closing let’s continue spreading word surrounding fantastic services offered throughout industry showcased through efforts established via ‘AnyKeyWord.’ Waco international movers
Your recommendation on wisdom drone digital camera angles is spot on! It makes a mammoth change in the last photographs. More methods at https://www.demilked.com/author/ofeithvsyz/ .
Embracing moments shared loved ones brings warmth comfort realizing significance connections formed memories cherished forevermore reminding value relationships cultivated nurtured over time nurtured throughout journeys undertaken together united front Best Jacksonville movers
I like the valuable info you provide in your articles.
I’ll bookmark your weblog and check again here frequently.
I am quite certain I’ll learn a lot of new stuff right here!
Good luck for the next!
Thanks for the useful post. More like this at experienced Farsi therapy counselor .
Appreciate the detailed information. For more, visit professional personal injury lawyer .
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy attorney
This was very enlightening. For more, visit foothills paving and maintenance .
Nice work raising awareness about safety hazards related to clogged dryers; we need more discussions like this! Dryer Vent Cleaning
Martial arts not only improve physical conditioning however likewise instill technique and focus in experts. It’s remarkable to see how various styles, from martial arts to jiu-jitsu, deal distinct benefits Denver Taekwondo classes
The convenience of having an ##appliance store near me## makes life so much easier. appliance store near me
Anyone else have hints for wireless camera tactics? Looking for respectable strategies in Sanford, FL! Security Camera Installation
Anyone else notice how many sidewalks need repairing in Brooklyn? Glad we have #your_keyword# around! concrete sidewalk repair manhattan
Great job! Discover more at Groene hart klimaatregeling pro .
Great job! Discover more at brain mapping therapeutic approaches Denver .
“Excellent service all around—I wouldn’t hesitate recommending # # anyKeyWord ###!” Best Neptune Beach movers
We’re proud to deliver custom home remodels in Sumner that reflect each homeowner’s unique taste and lifestyle.
Sumner Home Remodel
Thanks for the helpful article. More like this at after hours tooth extraction Beverly Hills .
Just finished getting some much-needed fixture repairs done by an incredible team at our trusted ▲ ▲ ▲ ! Highly recommend them! residential plumbing
Thanks for the insightful write-up. More like this at ادمین اینستاگرام .
So relieved I found water damage restoration companies near me after my recent flooding incident! Their team was professional and efficient.
This was a fantastic resource. Check out TheWinnslow for more.
Looking for ways to streamline your office move? The advice over at Long distance movers Nashville is invaluable!
Clearly presented. Discover more at Flanders pest control for commercial properties .
Very informative article. For similar content, visit ادمین اینستاگرام .
Thanks for the helpful advice. Discover more at estudiar un año escolar en Irlanda .
Have you ever tried a Les Paul with different pickups? It completely changes the sound! Learn more at Les Paul Tune-O-Matic Bridge .
This was very insightful. Check out Budd Lake pest management experts for more.
The process of restoring from water damage is fascinating yet daunting; glad we have professionals in Irving TX! water damage restoration near me
Excellent post on Essex’s roofing sector! It’s crucial to emphasize the importance of hiring the best roofer for top-notch ceiling repairs. It can be frustrating to have so many roofing corporations in Essex roofers in essex
I enjoyed this post. For additional info, visit https://maps.app.goo.gl/H2NonH1znj2v2MXe7 .
I was worried about my move until I discovered Kissimmee car transportation services for my Kissimmee car transport needs.
This was very insightful. Check out experienced Farsi therapy counselor for more.
I have been exploring for a little bit for any high quality articles or blog posts on this sort of house .
Exploring in Yahoo I ultimately stumbled upon this web site.
Studying this information So i’m glad to exhibit that I have
an incredibly excellent uncanny feeling I came upon exactly
what I needed. I most undoubtedly will make certain to don?t disregard this website and provides it a look regularly.
Great teamwork among all members present made this entire transition quick yet effective!! ###aniyKeyWord ## Sharpes Mover’s
Having trustworthy professionals who understand our unique needs in Council Bluffs makes such a difference during stressful times!!!#TrustLocal### anykeyword ## water damage restoration companies near me
It’s impressive that you are getting thoughts from this paragraph as well as from our dialogue made at this place.
I can’t trust how an awful lot fee I’ve stored on Genshin crystals due to this website! It’s reliable and extremely easy to use: cheap ManaBuy crystal deals .
Surely appreciate sharing insights into various techniques utilized restoring homes post-water incidents seeing firsthand transformation outcomes achieved through hard work involved too!!!! #Anykeword# water damage restoration services near me
Anyone else feel overwhelmed by potential water issues? I’ve found solace knowing that resources like flood restoration companies near me exist nearby.
Loft conversions are such a smart way to utilize wasted space; there’s so much potential up there that many people overlook—explore possibilities on Loft conversions Essex
Prevention is key when it comes to water damage. I recommend regularly checking your plumbing! For restoration tips, visit flood restoration companies near me .
Hey! I just wanted to ask if you ever have any problems with
hackers? My last blog (wordpress) was hacked and
I ended up losing many months of hard work due to no backup.
Do you have any solutions to protect against hackers?
Very encouraging stories here; gives me hope that choosing #### # will lead me toward success as well! Local movers Ocala
I recently completed a kitchen remodel on Mercer Island, and the transformation is unbelievable! It’s amazing how a new layout and updated appliances can completely change the feel of a home Sumner Home Remodel
Window cleaning will also be a daunting challenge, yet it appears like Window Cleaning Company makes it handy. Thanks for sharing!
Huge shoutout to the Silver Springs moving company for making my move stress-free! Silver Springs moving company
I found this very interesting. Check out ادمین اینستاگرام for more.
Well done! Find more at full-service brain mapping Denver .
I can’t stress enough how important it is to choose a trustworthy company like felon plumber!! # # anykeyword ## soquel plumbers
Thanks for the great explanation. More info at Dental Group Beverly Hills .
Such a well-written post! I’m going straight to check out the services offered by High DA backlinks for sale
Shoutout to Long distance movers Greenacres for their amazing service and low rates on moving in Greenacres!
Seriously considering using ###for future moves; their reputation in Doral is unmatched! Doral car moving companies
Thanks for the helpful advice. Discover more at estudiar un año escolar en Irlanda .
Nice work raising awareness about safety hazards related to clogged dryers; we need more discussions like this! Dryer Vent Cleaning
Moving can be tough, but Cheap movers Yalaha made it a lot easier for me in Yalaha. Great team!
Well done! Discover more at TheWinslow .
Thanks for the useful post. More like this at local insect control Flanders .
Fantastic post! Discover more at ادمین اینستاگرام .
Appreciate the comprehensive advice. For more, visit Kitchen sink plumbing .
Definitely believe that which you said. Your favorite justification seemed to be
on the net the simplest thing to be aware of. I say to you, I definitely get irked while
people consider worries that they plainly don’t know about.
You managed to hit the nail upon the top and defined out the whole thing without having side-effects , people
can take a signal. Will likely be back to get more.
Thanks
Looking for help with your next move? Look no further than Plant City apartment movers in Plant City!
Awesome article! Discover more at certified plumber .
This is highly informative. Check out local gas safety specialists for more.
The amenities available in their vehicles really enhance the overall experience as well!! # # anyKeyWord ## Sanford car shipping
I appreciated this article. For more, visit Foothills Paving .
Thanks for the useful post. More like this at cheap plumber .
Thanks for the insightful write-up. More like this at Affordible Pest Solutions .
I recently moved to Puyallup, and I was shocked by how many pests I encountered in my new home! After doing some research on pest control options, I found that local services are crucial for effective solutions Pest control
I’ll always choose whenever I need moving help in Margate! Office moving companies Margate
Excellent goods from you, man. I have keep in mind your stuff prior to and you are simply extremely great.
I actually like what you’ve got right here, really like what you are saying and the way in which by which
you say it. You are making it entertaining and you continue to take care of to keep it sensible.
I cant wait to read far more from you. That is actually a great website.
Just bookmarked this weblog—it’s going to be my cross-to resource as I start planning my digital camera installing!! Sanford Security Camera Installation
You won’t regret visiting #a n y K e yw o rd#, especially if you’re planning an upcoming move! Waco international movers
How did you find your chosen provider for Spring Hill vehicle shipping? Any recommendations? Spring Hill vehicle shippers
Anyone else excited about attending guitar festivals featuring legendary players showcasing their Gibson’s?! Who are you hoping to see?! Let us know at Gibson Les Paul Junior
I love this theme! Water is the sort of invaluable aid, and figuring out what number of gallons consistent with minute I really want will assist me use it correctly. Keep up the top notch paintings! https://list.ly/i/11110398
Appreciate this post. Let me try it out.
If you’re ever in need of relocation assistance, you should reach out to **== anyKeyWord==** immediately! Rockledge Mover’s
Have you ever considered publishing an ebook or guest authoring
on other websites? I have a blog centered on the same information you discuss and would love to have
you share some stories/information. I know my subscribers would value your work.
If you’re even remotely interested, feel free to shoot
me an email. https://Ctpedia.org/index.php/Reworking_Outside_Spaces_With_Interlocking_Stone_Services
For anyone in Vancouver, you must visit the appliance store for unbeatable prices on scratch and dent items at appliance store .
What’s the best way to prepare my vehicle for transport with a Wesley Chapel company? Any suggestions? Wesley Chapel car transportation services
The aesthetic appeal of a home or barn can be drastically improved with a well-placed copper copper cupola! cupola for barn
Just finished my move with a Mulberry company and it was seamless! More about my experience at Mulberry commercial movers .
Why pay complete value for Genshin Impact topping up? I found out a giant discount platform that delivers an awful lot larger rates. Highly endorse! ManaBuy official recharge
I every time emailed this blog post page to all my friends,
for the reason that if like to read it afterward my links will too. https://Bbarlock.com/index.php/User:LazaroGaray7240
Howdy! Do you know if they make any plugins to help with SEO?
I’m trying to get my blog to rank for some targeted keywords but
I’m not seeing very good success. If you know of any please share.
Thanks! http://Dragon-Slave.org/comics/KathaleenrsCarrolrt
Howdy! Do you know if they make any plugins to help with SEO?
I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good
success. If you know of any please share. Thanks! http://Dragon-Slave.org/comics/KathaleenrsCarrolrt
The benefits of hormone therapy are often overlooked. Thank you for shedding light on this important topic! For further reading, go to Centralia Medical Spa .
Regularly scheduled plumbing maintenance saves homeowners both time and money down the road; don’t skip those important checks with your trusted local plumbers! residential plumbing
¡Saludos Espero que estés bien Te quiero hablar de un sitio de casino
online que te va a encantar. La plataforma tiene una variedad impresionante
de juegos y una navegación muy fluida.
Si prefieres las slots, te sorprenderán con los juegos de slots variados.
También, el sitio tiene los clásicos de casino como el blackjack y la ruleta.
Una de las mejores cosas de este casino online es que tienen opciones de
pago locales. Si estás en Latinoamérica, es muy importante que los
métodos de pago sean fáciles de usar y seguros,
y este casino tiene opciones de pago muy convenientes.
Por si fuera poco, tienen bonos increíbles para jugadores nuevos.
Cuando te hagas miembro, recibirás un bonus de registro que te permitirá empezar con el pie derecho.
Y por si fuera poco, tienen bonos especiales durante todo
el año.
Esta plataforma también cuenta con atención al cliente de primera, si alguna vez necesitas asistencia.
Te aseguro que tendrás ayuda cuando lo necesites.
La plataforma es completamente segura, el casino utiliza
protocolos de seguridad avanzados para mantener tu
información personal segura. Puedes jugar tranquilo.
Si te animas este casino, te aseguro que no te arrepentirás.
¡Es tu oportunidad de hacer crecer tu dinero!
Además, siempre podrás disfrutar de gráficos impresionantes.
Cada juego es una nueva oportunidad.
Mi consejo es que le des una oportunidad y disfrutes de todo lo que
tiene para ofrecerte. Confío que lo harás, Pablito, este es un excelente lugar para jugar.
¡Suerte y que empiecen las ganancias!
Thanks for the clear advice. More at ادمین اینستاگرام .
If you’re planning a trip to Costa Rica, make sure to book a tour in Herradura—it’s life-changing! Find out more at Esterillos horse tours .
Great insights! Discover more at ادمین اینستاگرام .
I’ve forever been curious about the modifications among herding and searching puppy breeds—what insights can you percentage? http://spiderproject.com.ua/bitrix/rk.php?goto=https://wool-wiki.win/index.php/Feeding_your_puppy_would_you_be_feeding_your_canine
Thank you for sharing your knowledge! I’m eager to improve my site’s rankings with help from Buy backlinks instantly .
Thanks for the valuable insights. More at https://www.anobii.com/en/01d063057db30e4eca/profile/activity .
This is highly informative. Check out Serenity Counseling Group for more.
Nicely detailed. Discover more at foothills paving and maintenance .
مشاوره برای موفقیت تحصیلی و مشاوره تحصیلی رایگان
تلفنی
Great job! Find more at Emergency Pure Plumbing .
Keep up the great work, Window Cleaning North York ! Your window cleaning services are top-notch in North York.
The lowest priced appliance store I’ve found is definitely appliance store near me ; highly recommend checking it out!
Your insights on video marketing are truly inspiring! Discover more techniques at blackhat marketing blog .
What a fine article! Training our bushy neighbors may be troublesome, yet your systems make it less difficult to fully grasp. For extra innovations, check out https://go.bubbl.us/ec06de/f5b1?/New-Mind-Map !
I really enjoyed reading this post! It provides great insights on the topic. For anyone looking for more information and resources, check out Atlanta painting contracotrs for some excellent content related to this theme!
Thanks for the clear advice. More at LuxNuro .
Pretty section of content. I just stumbled upon your website and in accession capital
to assert that I acquire actually enjoyed account your blog posts.
Any way I will be subscribing to your feeds and even I achievement you access consistently fast. https://goelancer.com/question/traitement-raffermissant-de-la-peau-redonnez-a-votre-peau-sa-fermete-naturelle/
Appreciate the thorough write-up. Find more at urgent oral care Beverly Hills .
Thanks for the informative content. More at año escolar Irlanda .
I love seeing all the creative storage solutions people come up with for their converted attics—it inspires me every day; find clever hacks listed on Loft conversions Essex
Pretty section of content. I just stumbled upon your website and
in accession capital to assert that I acquire actually enjoyed
account your blog posts. Any way I will be subscribing to your feeds and even I achievement
you access consistently fast. https://goelancer.com/question/traitement-raffermissant-de-la-peau-redonnez-a-votre-peau-sa-fermete-naturelle/
Fantastic post! Discover more at ادمین اینستاگرام .
Recently had some plumbing fixture repairs done; couldn’t have asked for better service from my trusty hydrojetting #.
Very helpful read. For similar content, visit TheWinnslow .
Thanks for the helpful advice. Discover more at Afordable Pest Solutions .
Great discussion at the ethics of drone pictures and respecting privateness rights! A have got to-read for all drone lovers! More insights at https://www.gamespot.com/profile/neasalchxe/ .
Just desired to highlight how first rate my adventure was with mudanças em sorocaba # all through my contemporary relocation!
Anyone else had a victorious feel with mudança em sorocaba #? Their staff is peak-notch!
This was quite useful. For more, visit Budd Lake bug removal services .
The stigma around bankruptcy often overshadows the reality that it can be a necessary step towards financial recovery. Understanding the different types of bankruptcy and their implications is crucial bankruptcy lawyer
I have been exploring for a little bit for any high-quality articles or blog posts on this
kind of area . Exploring in Yahoo I ultimately stumbled upon this website.
Studying this info So i am satisfied to convey that I’ve an incredibly
good uncanny feeling I discovered exactly what I needed. I so much certainly will make sure to don?t omit
this website and provides it a look regularly.
Great job! Find more at ادمین اینستاگرام .
I was once pleasantly stunned by way of how lower priced empresa de mudanças is for the high-quality of service they present!
Excited about discovering trustworthy options in the area thanks largely due diligence done via your post & links from ### anyKeyWord###.” Sunshine Auto Transport’s St. Cloud
Incredible satisfaction felt after reaching destination safely soundly without losing anything along way thanks primarily due exceptional management skills displayed consistently throughout entire undertaking!! Crystal River apartment movers
Wonderful tips! Discover more at Groene Hart Klimaatregeling Pro .
Very helpful read. For similar content, visit affordable Farsi therapy counselor .
I recently got my hands on a vintage Les Paul, and it’s a game changer! Share your experiences at Les Paul Weight Relief .
Great insights! Find more at Affordable termite solutions Hackettstown .
Just had my floors restored by the team at water damage restoration companies near me after a leak—what a difference they made!
Anyone else find themselves constantly rearranging furniture post-painting??? Let’s chat about our setups!!! ## Minneapolis painters
I’ve recently had a huge problem with pests in my home, and I didn’t know where to turn Puyallup Pest Control
This is quite enlightening. Check out Brain Mapping Analysis Denver for more.
Appreciate the comprehensive insights. For more, visit estudiar un año escolar en Irlanda .
This was very beneficial. For more, visit Immediate Dental Care Beverly Hills .
Quick response is key when dealing with water damage—thankful for the services offered by local companies in Irving TX! water damage restoration services near me
The statistics about climate conditions affecting drone performance is the most important for making plans flights! Thanks for sharing that perception! More info will probably be chanced on at https://shed-wiki.win/index.php/**Safety_First:_Best_Practices_for_Flying_and_Using_Your_Drone_Camera_Responsibly** .
Thanks for the useful suggestions. Discover more at TheWinslow .
Thank you for the wonderful insights into SEO strategies and backlinking; going to explore options with Buy backlinks for niche sites and blogs #!
You’re certainly alone if you’re looking for trustworthy contractors in Essex. Maintaining a strong rooftop is essential given the unstable conditions we expertise flat roof repair essex
Great insights! Find more at ادمین اینستاگرام .
Thanks for the thorough article. Find more at Affordable Pest Solutions .
Such valuable information on handling water emergencies—it’s vital for homeowners in our lovely Hawaiian Gardens community! water damage restoration companies near me
Ahaa, its good conversation on the topic of this article at this place at this webpage,
I have read all that, so at this time me also commenting here. https://Dragon-Slave.org/comics/MariannetyDancyuq
Ahaa, its good conversation on the topic of this article at this place
at this webpage, I have read all that, so at this time me also commenting here. https://Dragon-Slave.org/comics/MariannetyDancyuq
After I originally commented I appear to have clicked on the -Notify me
when new comments are added- checkbox and now each time a
comment is added I get four emails with the exact
same comment. Is there a means you can remove me from that service?
Thank you!
I found this very interesting. Check out ادمین اینستاگرام for more.
”You’ve made such a compelling case for regular duct maintenance—it’s hard not to agree!” Dryer Exhaust Vent Cleaning
It’s refreshing to see such dedicated teams working hard during emergencies—thank you, ### anyKeyword###, for your commitment to excellence! water and mold restoration near me
Wonderful tips! Discover more at foothills paving and maintenance .
I enjoy reading through ann article that will make men and women think.
Also, thanks for allowing me to comment!
Here is my blog post: Samsun Demirdöküm servisi
This was quite useful. For more, visit Afordable Pest Solutions .
You actually mentioned this wonderfully.
I’ve always been curious about the benefits of chiropractic care, especially in Centralia. It’s great to see local practitioners focusing on holistic health. I believe that regular adjustments can significantly improve overall wellness Centralia Medical Spa
Who knew buying discount appliances could be so fun? Thanks to the team at wholesale appliances for making it enjoyable!
This was a fantastic read. Check out comprehensive pest management Long Valley for more.
Have you participated in any guitar forums discussing Les Pauls? They’re full of great tips! Check one out at Les Paul 490R 498T Pickups .
Great breakdown of the topic.
Very useful post. For similar content, visit trusted personal injury lawyer .
I’ve been seek a legitimate manner to suitable up Genshin crystals, and I in any case found a website that affords useful offers! Check it out the following: ManaBuy quick recharge .
I had such a positive experience with my move thanks to the team at Best Midland movers #.
Want hassle-free moving experiences? Read through helpful articles and reviews at Jacksonville apartment movers before making your choice.
Wonderful tips! Find more at Groene Hart Klimaatregeling Pro .
Anyone else moved recently? Would love to hear about your experiences with companies listed on ##anyKeyword#. Lawtey movers
Sandernson turned what could have been an overwhelming situation into something manageable and enjoyable!!! Sanderson movers
I recently used Local movers Fort Liberty for my move to Fort Liberty and was impressed by their low rates and great service!
“#Anykeyword is definitely the best choice when it comes to relocating your office!” Local movers Macclenny
This was very beneficial. For more, visit 24 hr plumber .
Certainly thrilled embarking fresh chapter awaits eagerly anticipated arrival marking commencement commencing soon facilitated orchestrated expertly providing assurance needed confidently embarking journey ahead facilitated meticulously crafted pathways Ease Mover’s
Great job! Discover more at best plumbers near me .
This was highly useful. For more, visit affordable blocked manhole repairs .
Loving every moment spent exploring different neighborhoods around town lately—inspired begin documenting adventures online share others interested relocating too someday soon!!## any Keyword ## Jacksonville moving company
Has any individual else used mudanças em sorocaba for moving in Sorocaba? I had a large sense and would really like to pay attention extra stories!
Couldn’t believe how easy it was working with ###anykeyword###! Definitely recommend their services to fellow residents of Waco. Waco moving companies
So glad I found Fast Track Mover’s while searching for budget-friendly movers in Melrose! They were fantastic!
Do your self a want and employ mudança em sorocaba in your next circulation! You won’t be apologetic about it.
What’s up, I desire to subscribe for this web site to
obtain hottest updates, therefore where can i do it please help
out. http://Blitribe.com/doku.php?id=choisi_un_plombie_expe_t:conseils_pou_fai_e_le_bon_choix
What’s up, I desire to subscribe for this web site
to obtain hottest updates, therefore where can i do it please help out. http://Blitribe.com/doku.php?id=choisi_un_plombie_expe_t:conseils_pou_fai_e_le_bon_choix
This was very enlightening. More at ادمین اینستاگرام .
My recent circulate was once such a lot easier as a result of empresa de mudanças . Their group is ideal-notch!
This was very enlightening. For more, visit camping card games .
This was quite informative. For more, visit https://trentonvkvv419.wpsuo.com/winter-car-maintenance-checklist-for-buckley-roads-2 .
Love seeing before-and-after photos of painted rooms! Anyone want to share theirs? Atlanta painting contracotrs
Thanks for the helpful article. More like this at ادمین اینستاگرام .
Thanks to my father who informed me concerning this webpage,
this blog is genuinely awesome.
#Discount appliance store# specials always keep me coming back for more deals! appliance liquidators
Finding a trustworthy roofer in Essex is be everything. It’s crucial to pick experienced professionals whether you need roof repairs, a complete roof replacement, or specialized services like toned roofing flat roof repair essex
My brother suggested I might like this blog. He was totally
right. This post truly made my day. You cann’t imagine just how much time I
had spent for this information! Thanks!
Can children benefit from seeing a chiropractor in Bonney Lake too? Curious about this! https://dantedpzx261.cavandoragh.org/how-a-sports-chiropractor-in-bonney-lake-can-help-prevent-and-treat-athletic-injuries-1
Filing for bankruptcy might seem like an overwhelming process, but it can provide a fresh start for those in severe financial distress. It’s essential to seek professional advice to navigate the complexities involved bankruptcy lawyer
I recently discovered the importance of proper nutritional guidance in my health journey, and I can’t stress enough how beneficial it has been Weight Loss Clinic
This was highly educational. More at estudiar un año escolar en Irlanda .
Thanks for the great explanation. More info at LuxNuro .
This was very enlightening. More at Beverly Hills emergency oral services .
Fighting style not only boost fitness but additionally instill technique and focus in practitioners. It’s interesting to see exactly how different styles, from karate to jiu-jitsu, offer special benefits Denver Taekwondo classes
Great put up! I’ve been attempting to find efficient programs to coach my puppy. The info you shared are absolutely advantageous! I discovered extra assets on this subject at https://www.livebinders.com/b/3662062?tabid=acfc4879-5fa6-e075-11c6-365b7b427e59 .
Fantastic article on window care—it’s so important to keep them clear and streak-free! top-rated window cleaning company
Great insights! Find more at affordable personal injury attorney .
Just wanted to share my positive experience with the team at water damage restoration services near me —they truly care about their clients!
It’s going to be finish of mine day, except before ending I am reading this fantastic
piece of writing to increase my know-how. https://wp.teamlead.pw/question/amenagement-dune-cour-arriere-sur-pelouse-a-quebec-creez-votre-paradis-vert/
Thanks for the valuable insights. More at Affordible Pest Solutions .
Commercial plumbing projects require precision—a great reason to hire an expert ### anyKeyword ### near you. local plumber
It’s going to be finish of mine day, except before ending I am reading this
fantastic piece of writing to increase my know-how. https://wp.teamlead.pw/question/amenagement-dune-cour-arriere-sur-pelouse-a-quebec-creez-votre-paradis-vert/
Excellent points made the following approximately roof cleaning! If you’re neighborhood, payment out Roof Washing .
What an informative submit! I’ll be rearranging my cameras this weekend based mostly for your information. https://tiny-wiki.win/index.php/How_Close_Should_You_Place_Security_Cameras%3F_Finding_the_Right_Distance
Thanks for the clear breakdown. Find more at Affordible Pest Solutions .
Thanks for the helpful advice. Discover more at apartamento turístico Arzúa .
Wonderful tips! Find more at casa rural Arzúa .
I love how paint can change the mood of a room! What’s your go-to color for relaxation spaces? painting companies near
If you’re looking for reliable transportation in Kissimmee, you have to try Kissimmee auto transport companies . They made my travel experience so much smoother!
#If you’ve got plans this season, make sure you consider contacting ## Ocala international movers
Thanks for the great tips. Discover more at Texas Strong | Air Conditioning & Heating | Houston .
I enjoyed reading about multi-channel attribution models—it’s essential to understand where conversions originate from accurately; dive deeper into attribution models over ###anKeyWord## marketing blog
#SmoothMove#—that’s what I got when I hired Long distance movers Hialeah # for my relocation within Hialeah.
This was very enlightening. More at ادمین اینستاگرام .
I recently completed a loft conversion in Essex, and it transformed my home. Highly recommend exploring options at Loft conversions Essex !
Curious if there are particular organizations collaborating directly with local governments towards improving infrastructure resilience…would love feedback!!!!#InfrastructureGoals ### anykeyword ## water and mold restoration near me
Amazing what community support does bringing forth willingness collaborate making lives easier across board helping everyone benefit ultimately too!!!#Anykeyword# water damage restoration companies near me
This was highly educational. For more, visit Affordable Pest Solutions .
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
Nicely done! Find more at emergency pest management Long Valley .
The aerial images pointers you shared are notably powerful! I’m excited to strive them out. Learn extra at https://www.divephotoguide.com/user/marmailsmu/ .
Just booked our bounce house for next weekend’s party in Tampa! So excited to use tent party rental near me !
Anyone else feel overwhelmed by potential water issues? I’ve found solace knowing that resources like water restoration near me exist nearby.
Just wanted to share my experience with a fantastic team for water restoration—found them through water and mold restoration near me !
Does anyone else feel like playing a Gibson Les Paul elevates their performance? It’s a must-try! More insights at Gibson Les Paul Studio .
This was a great article. Check out estudiar año escolar en Irlanda for more.
I’m captivated with exploring Teyvat in Genshin Impact! When it comes to prime-ups, Primogems via ManaBuy has been my go-to web site for distinctive bargains!
This was quite helpful. For more, visit LuxNuro .
Serenity lies within knowing solutions await discovery amidst trials faced daily providing reassurance persistently anchored strongly drawn closer overall connection nurtured gracefully held tightly around.@ Doral auto shippers
Can’t believe how fast and reliable Bitchat download is! Perfect for group chats. free Bitchat Apk download
پروتئین وی هیدرولیزه دیاموند فا، مکملی با کیفیت بالا از برند FA است که بر پایه کنسانتره هیدرولیز شده پروتئین وی تهیه شده و به رشد عضلات بدون چربی کمک میکند.
Thanks for the great explanation. More info at immediate urgent dental service .
Finding dependable allies becomes crucial especially amid chaotic periods which makes discovering brands like ‘Brandon’s’ even more valuable!! #AnyKeyWord## Brandon vehicle shippers
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Shoutout to the amazing team of long distance movers in Midland who helped me relocate! You can find them at Midland international movers .
”If you want professionalism and efficiency when moving apartments —choose # # # # #!” Plant City commercial movers
I appreciate companies like Long distance movers Jacksonville that make moving affordable and easy in Jacksonville!
Very useful post. For similar content, visit TheWinnslow .
Thanks for the helpful advice. Discover more at Groene Hart Klimaatregeling Pro .
It’s great to know that there are affordable moving options in Macclenny! I found a fantastic deal at Macclenny moving companies .
Thanks for the great information. More at Affordible Pest Solutions .
Just finished my move, and thanks to Cheap movers Fort Liberty , I’m settling into my new Hilliard apartment quickly!
I love how Bellevue is embracing smart home technology for renovations! It’s amazing to see how these innovations not only enhance the comfort and convenience of our living spaces but also improve energy efficiency Sumner Home Remodel
I found this very interesting. Check out Affordable Pest Solutions for more.
Has anyone had experience with High DA backlinks for sale ? I’m considering their backlink services based on reviews I’ve seen.
Our business is thriving in its new location thanks to # # anyKey word # # and their excellent service! Clearwater full service movers
Appreciate the insightful article. Find more at casas rurales Arzúa .
Your strategies for practicing secure flight paths are valuable! Safety could regularly come first when flying drones. Explore extra protection facts at https://wiki-aero.win/index.php/**Safety_First:_Best_Practices_for_Flying_and_Using_Your_Drone_Camera_Responsibly** .
Thanks for the great explanation. More info at ادمین اینستاگرام .
Wonderful tips! Discover more at Affordible Pest Solutions .
#Scratch and dent appliance stores# are such smart choices for budget-savvy shoppers like me. appliance store Vancouver
This was highly useful. For more, visit Affordable Pest Solutions .
Thanks for the detailed post. Find more at essential camping equipment .
I never thought I’d enjoy horseback riding so much until I tried it in Jacó! The team at Jaco horseback riding tours was top-notch!
Good blog you have here.. It’s difficult to find excellent writing
like yours nowadays. I truly appreciate individuals like you!
Take care!!
I recently had a pest problem in my home, and I was amazed by the effective solutions offered by local services. It’s crucial to choose a knowledgeable pest control provider in Puyallup to ensure a pest-free environment Pest Control Puyallup
I was amazed by the affordability of the services at Local movers Mulberry when I moved in Mulberry!
Excellent information on Essex roof remedies! Finding trustworthy builders is essential, especially for flat roof upgrades and repairs. The sturdiness and safety of a piece of work can depend entirely on the workmanship roofing companies essex
So inspired with the carrier from mudanças em sorocaba ! They handled every part with care at some point of my cross.
Thanks to the team at mudança em sorocaba , my stream turned into now not purely mild yet additionally relaxing!
Clearly presented. Discover more at ادمین اینستاگرام .
That moment when you finally land that perfect riff on your Gibson Les Paul is priceless; what was yours?! Share those moments over at Gibson Les Paul Special
hey there and thank you for your info – I have certainly picked up anything new from right
here. I did however expertise several technical issues using this site, as I experienced to reload
the website lots of times previous to I could get it to load correctly.
I had been wondering if your web host is OK? Not that I’m complaining,
but slow loading instances times will very frequently affect your placement in google and can damage your quality score if
ads and marketing with Adwords. Well I am adding this RSS to my e-mail and could look out for a lot more of your respective interesting content.
Ensure that you update this again very soon. https://oerdigamers.info/index.php/Article_Title
Anyone else love how mild that’s to work with experts like those at empresa de mudanças ?
If you wish to maximize your Genshin Impact gameplay devoid of overspending, you’ve obtained to comprehend these topping up tips. Find out extra at how to ensure a safe top-up on ManaBuy !
hey there and thank you for your info – I have certainly
picked up anything new from right here.
I did however expertise several technical issues using this
site, as I experienced to reload the website lots
of times previous to I could get it to load correctly.
I had been wondering if your web host is OK? Not that I’m
complaining, but slow loading instances times will very frequently
affect your placement in google and can damage your quality score
if ads and marketing with Adwords. Well I am adding this RSS to my e-mail and
could look out for a lot more of your respective interesting content.
Ensure that you update this again very soon. https://oerdigamers.info/index.php/Article_Title
Thanks for the great tips. Discover more at best commercial property broker .
This was a wonderful guide. Check out motor vehicle accident lawyer near me for more.
#Moving doesn’t have to be stressful when you have great help from companies like Ocala moving companies #
Appreciate the helpful advice. For more, visit best Sewer line repair near me .
Thanks for the helpful article. More like this at affordable Farsi psychotherapy .
It’s crucial to pick trustworthy movers when changing locations; I’m so glad I found ### anyKeyWord###. Silver Springs moving company
This post addresses many common misconceptions about hormone therapy. I appreciate the clarity! For more insights, please visit Centralia Medical Spa .
This was quite useful. For more, visit professional driveway contractors Wheat Ridge .
I liked this article. For additional info, visit Groene hart klimaatregeling pro .
¡Qué tal ¿Cómo te encuentras hoy? Hoy quiero recomendarte
un casino virtual que es ideal para ti. La plataforma tiene una
excelente selección de juegos y una interfaz fácil de usar.
Si eres fan de los juegos de azar como las tragamonedas, quedarás asombrado con los juegos de slots variados.
También, el casino tiene juegos de mesa clásicos.
Lo mejor de este casino online es que te permiten hacer depósitos y retiros de manera sencilla.
En América Latina, es muy importante que los métodos de pago
sean fáciles de usar y seguros, y este casino tiene opciones de pago muy
convenientes.
Por si fuera poco, te dan bonos de bienvenida para jugadores nuevos.
Tan pronto como te registres,, recibirás un bono inicial que te
permitirá aumentar tus posibilidades de ganar. También, tienen torneos con grandes premios.
La web también cuenta con un servicio de atención al cliente
impecable, si alguna vez necesitas asistencia.
Te aseguro que tendrás ayuda cuando lo necesites.
En cuanto a la seguridad, el sitio utiliza protocolos de seguridad avanzados para garantizar que tu dinero
esté protegido. Es totalmente confiable.
Pablito, este casino, te aseguro que no te arrepentirás.
¡Las posibilidades de ganar son enormes! Además, siempre podrás disfrutar de gráficos impresionantes.
Te vas a divertir muchísimo.
Te recomiendo que entres ahora mismo y disfrutes de todo lo que tiene para ofrecerte.
Confío que lo harás, Pablito, no te puedes perder esta oportunidad.
¡Suerte y que empiecen las ganancias!
Backlinks are indeed vital for SEO success; make sure to check out the offers at Quality backlinks for eCommerce websites !
Discount open box appliances are a steal at appliance store near me —don’t miss out!
I recently attended an open house featuring a stunning loft conversion—it was such an inspiration! More ideas here: Loft conversions Essex .
Appreciate the thorough write-up. Find more at affordable syphon installation .
This was highly educational. For more, visit comprehensive brain therapy in Denver .
Thanks for the clear advice. More at año escolar en Irlanda .
Thanks for the great content. More at Tap washers .
Anyone else find that cocoa Apartment Movers has some of the best customer support ever??? Sharpes Mover’s
I appreciated this article. For more, visit Beverly Hills Dental Group .
Thanks for the valuable article. More at ادمین اینستاگرام .
Appreciate the thorough analysis. For more, visit ادمین اینستاگرام .
Thanks for the helpful article. More like this at Emergency plumbing .
Thanks for the clear breakdown. Find more at TheWinnslow .
This was very beneficial. For more, visit Affordable Pest Solutions .
Just shipped my car from Ocala last week, and it arrived in perfect condition thanks to Ocala auto shipping !
Excellent article on Essex’s cladding sector! It’s crucial to emphasize the importance of hiring the best roofer for top-notch roof repairs. It can be overpowering to have so many roofing firms in Essex roofers essex
If you’re in Honolulu, don’t hesitate to reach out to an experienced plumber for any plumbing issues.
Appreciate the useful tips. For more, visit Affordable Pest Solutions .
Thanks for the great information. More at pressure washing near me .
We stumbled over here coming from a different page and thought I should
check things out. I like what I see so now i’m
following you. Look forward to looking over your web page yet
again. https://Www.sitetop.org/site/365.Expresso.blog/question/decouvrez-les-meilleures-degustations-de-vins-a-montreal-29/
I found this very interesting. For more, visit casas rurales .
Thanks for the thorough analysis. Find more at Serenity Counseling Group .
Highly recommend checking out customer reviews before choosing a mover like those at # any Keyword#! Clearwater full service movers
Recently painted an accent wall with removable wallpaper, and it’s so easy to change up later! painting companies near me
Appreciate the detailed information. For more, visit Residential Pest Control Hackettstown .
Plinko macht einfach Laune, Leute! Ich bin mit https://clashofcryptos.trade/wiki/User:SommerBettington gestartet und war direkt gehooked – perfekt zum Reinkommen ohne Druck. Jetzt häng ich voll in der App, läuft alles smooth und easy. Das Feeling, wenn die Kugel ganz unten in der hohen Auszahlung landet – unbeschreiblich. Ich sag nur: ausprobieren, ihr werdet’s feiern. Wer ready ist, soll die Echtgeld-Variante zocken – lohnt sich. Wer kennt gute Varianten oder Apps für Plinko?
Hiring ###used to be one of the vital optimum judgements I’ve made this 12 months—so grateful for their aid! mudança em sorocaba
I not too long ago wiped clean my deck riding a 2700 PSI drive washing machine and it worked like a attraction! If you would like to look some prior to-and-after shots, payment out https://www.instapaper.com/read/1850433564 .
Many people fear that bankruptcy will ruin their credit forever, but that’s not necessarily true. With proper planning and financial management post-bankruptcy, individuals can gradually rebuild their credit score bankruptcy lawyer
Great insights on relocating! I’ll without doubt be contacting mudanças em sorocaba for my upcoming flow in Sorocaba SP.
Groetjes allemaal, ik wilde even reageren op het onderwerp over https://hikvisiondb.webcam/wiki/User:CarlaDelaney, want ik zie steeds vaker mensen zich afvragen of Plinko nu een eerlijk spel is of niet. Zelf had ik er eerlijk gezegd ook weinig van begrepen, maar na wat research snap ik nu veel beter wat Plinko eigenlijk doet met je als speler.
Het lijkt op het eerste gezicht echt super simpel – gewoon klikken en kijken wat eruit komt – maar dat is juist de truc. Die eenvoud maakt het spel super aantrekkelijk maar ook tricky. Vooral via de Plinko app gaat het allemaal heel soepel en vaak ongemerkt.
Veel mensen noemen het een “Plinko scam” als ze verliezen, maar ik denk dat dat vaak meer frustratie is dan een echt probleem. Plinko is een kansspel – je denkt misschien dat je invloed hebt, maar dat is schijn.
Dus voor wie zich afvraagt wat je kunt verwachten bij Plinko, zou ik zeggen: neem het niet te licht op. Het kan leuk zijn, zolang je weet waar je aan begint. Succes allemaal en let een beetje op jezelf!
Really appreciate the transparency and honesty from flood restoration companies near me throughout the entire restoration process.
I cannot consider how soft my transfer was once as a result of empresa de mudanças —indubitably the ideally suited movers in Sorocaba SP!
Clearly presented. Discover more at https://maps.app.goo.gl/VgBKgpE1xiC93Fra7 .
Mercer Island is such a beautiful place to live, and home remodeling can truly enhance its charm! I recently completed a project that transformed my living space into a more functional and inviting area Sumner Home Remodel
Thanks for the informative post. More at año escolar Irlanda .
Thanks for the useful post. More like this at ادمین اینستاگرام .
Does anyone else have a ‘dream’ version of their perfect Gibson Les Paul in mind that they wish existed? Let’s brainstorm ideas together over at Les Paul Tonewoods
Thanks for the thorough analysis. Find more at Dental Group of Beverly Hills .
Water can cause so much trouble if not addressed quickly—Irving TX has some of the best restoration services around! water restoration near me
Thanks to Jamaica moving companies , our business set-up was completed on time after our recent move.
Appreciate the detailed information. For more, visit TheWinslow .
Tired of that outdated layout? We specialize in house remodeling in Sumner that transforms how you live.
Home Remodel Sumner
Let’s brainstorm ways we could create more comprehensive outreach programs aimed at educating children/youth regarding these topics early on!!!!#YouthEducation### anykeyword ## water restoration near me
I heard competitive reviews surrounding pricing structures offered through companies similar alongside #DallasMovers; do share thoughts here too please! Fort Mover’s
Just wanted everyone else looking into home improvement projects know that there’s useful guidance available through %%ANYKEYWORD%%%!!! Scotts Valley plumbers
This was a great article. Check out reliable professional pest services Flanders for more.
Appreciate all shared experiences concerning past repairs made as they serve as valuable lessons learned which could potentially save someone else heartache later down road too!!!#Anykeyword# flood restoration companies near me
Anyone else moved long distance with a Best Lawtey movers ? How was your experience?
Nicely done! Find more at ادمین اینستاگرام .
This is very insightful. Check out easy camping breakfast options for more.
I’m sure others would appreciate knowing about # anyKeyboard too!! Jacksonville movers
When I originally commented I clicked the “Notify me when new comments are added” checkbox
and now each time a comment is added I get four
emails with the same comment. Is there any way you can remove
people from that service? Appreciate it!
Moving doesn’t have to break the bank! Thank you, Macclenny full service movers , for your affordable moving services in Macclenny.
The importance of having a good restoration plan cannot be overstated; check what ### anyKeyword### suggests if you’re local to Irving! water damage restoration service near me
I recently had a pest issue in my home, and I was amazed by how effective the Puyallup Exterminator service was! They identified the problem quickly and implemented a comprehensive plan to eliminate the pests Puyallup Pest Control
Having worked with various companies in past moves, I can confidently say that sandersom stands out above others!!! Sanderson moving company
This was a wonderful guide. Check out Affordable Pest Solutions for more.
Manabuy has replaced the method I recharge for Mobile Legends! The financial savings are mind-blowing. Find out how it is easy to receive advantages at top up mlbb online .
Great tips on handling water emergencies! For those needing restoration services in Clive, don’t forget about water damage restoration companies near me .
Can’t believe how easy it was to book my move with the affordable services from Cheap movers Melrose #—lifesaver!
It’s fascinating how many people underestimate the value of hiring professionals during their move—check out # # anykeyword # # for more info! Ease Mover’s
Just had an amazing group chat session on Bitchat download—definitely a fun way to catch up with friends! how to get Bitchat Apk
Feeling incredibly fortunate discovering options such as ‘#ANYKEYWORD’ prior deciding embark upon journey involving relocation across town. Pride Mover’s Waco
Well done! Find more at casas rurales Arzúa .
Staying organized during a paint job can be tricky—how do you manage supplies during larger projects?? exterior painters near me
Thanks for the informative content. More at Affordible Pest Solutions .
Glad I stumbled upon this article! I’m planning to buy backlinks from Buy guest post backlinks soon.
I am not sure where you’re getting your info, but good topic.
I needs to spend some time learning more or understanding more.
Thanks for excellent information I was looking for this information for
my mission. http://articomed.com/node/241629
Don’t forget to look into scratch and dent options if you’re looking to save big! Check out options from appliance store nearby .
I am not sure where you’re getting your info, but good topic.
I needs to spend some time learning more or understanding more.
Thanks for excellent information I was looking for this information for my mission. http://articomed.com/node/241629
It’s fascinating how hormone therapy can help balance mood swings and alleviate symptoms. I learned so much from this article! Visit Centralia Medical Spa for more details.
Topping up in Genshin Impact doesn’t have got to be pricey anymore! I fairly endorse testing buy Genesis Crystals from ManaBuy for discounts.
Highly recommend taking advantage of the services offered by Ocala full service movers for your next move.
Hello there, You’ve done an excellent job.
I’ll certainly digg it and personally suggest to
my friends. I am sure they will be benefited from this website.
Thanks for the useful post. More like this at ادمین اینستاگرام .
Our clients love how our Sumner WA remodeling projects blend modern upgrades with timeless design. Home Remodel Sumner
The neck on a Les Paul feels so smooth; it’s perfect for solos! What’s your favorite solo to play? Discuss at Les Paul Coil Splitting .
This was highly informative. Check out Commercial real estate agency for more.
I appreciated this article. For more, visit ادمین اینستاگرام .
I love the way you highlighted the significance of socialization in puppy practise! This is significant for a neatly-adjusted pet. For greater linked content, fee out https://www.protopage.com/abbotsrkhi#Bookmarks .
Upgrading feels monumental especially after consulting people well-versed subject matter beforehand… thankful connections exist in community!!! local plumber
My new ductless mini-split installation has changed my home’s entire comfort level!” AC installation Walburg
Great insights! Find more at comprehensive Farsi psychotherapy services .
Thanks for the insightful write-up. More like this at Foot Hills Paving .
Anyone else feel overwhelmed by the idea of moving? Tips from places like Hialeah moving companies can help!
Excellent article! With the erratic wind we experience, it’s crucial to find trustworthy roofers in Essex. The right rooftop company can make a big difference, whether it’s a minor rooftop repair or a finish straight roofing installation flat roof repair essex
This is highly informative. Check out Conner Roofing, LLC for more.
I have been exploring for a little bit for any high-quality articles or weblog posts on this kind of area
. Exploring in Yahoo I ultimately stumbled upon this site.
Reading this info So i am happy to express that
I’ve an incredibly good uncanny feeling I discovered exactly what
I needed. I most indisputably will make sure to do not overlook this
website and provides it a look on a relentless basis. http://articomed.com/node/234789
I have been exploring for a little bit for any high-quality articles or weblog
posts on this kind of area . Exploring in Yahoo I ultimately
stumbled upon this site. Reading this info So i am happy to express that I’ve an incredibly good uncanny feeling I discovered exactly
what I needed. I most indisputably will make sure to do not overlook this website and provides it a look on a relentless basis. http://articomed.com/node/234789
Nicely done! Discover more at año escolar Irlanda .
Just moved my office last week with a local company in Greenacres. Highly recommend checking out Greenacres commercial movers for great services!
#Scratch and dent appliance stores# are underrated; I’ve found amazing deals there! appliance store
This was highly educational. More at TheWinslo .
Manabuy has thoroughly modified the manner I recharge for Mobile Legends. It’s rapid and dependableremember, which is precisely what gamers want! Don’t hesitate—investigate out buy mobile legends credits !
Valuable information! Find more at ادمین اینستاگرام .
After experiencing significant water damage, I’m glad I chose ###Anykeyword###—they restored my home beautifully! water damage restoration services near me
This guide makes me feel more prepared for our upcoming office move; thanks for sharing about **###ANYKEYWORD###** too! Yalaha commercial movers
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy attorney
Awesome article! Discover more at Groene hart klimaatregeling pro .
If you need a trustworthy moving company, consider Plant City apartment movers in Plant City.
A rooftop terrace off your converted attic sounds dreamy—imagine those summer evenings up there! Discover outdoor ideas on Loft conversions Essex
Big thanks to the folks at mudança em sorocaba # for making my relocation common and efficient.
#siteLink#: Their online booking system made scheduling such an easy task!” Office moving companies Margate
Saved as a favorite, I love your site!
My site; bandar togel terpercaya
Fighting style not just boost physical conditioning but likewise instill technique and focus in specialists. It’s fascinating to see just how different designs, from martial arts to jiu-jitsu, deal special benefits Denver Taekwondo classes
I used mudanças em sorocaba for my final stream in Sorocaba, and they passed my expectancies. Fast and valuable!
Wonderful tips! Find more at local toilet repair .
I’m forever on the lookout for wonderful deals on Genshin crystals, and I stumbled upon exclusive Primogem packs deals ManaBuy . Their low priced high-up ideas have incredibly helped toughen my gameplay!
Very happy with how well my belongings were treated by the #longdistance mover###. Best Lawtey movers
Anyone else had great success with an Irving TX company for their water damage restoration needs? Let’s share our experiences! water damage restoration service near me
Appreciate the comprehensive insights. For more, visit gas fitters .
Your insights on video marketing are truly inspiring! Discover more techniques at marketing blog .
This was nicely structured. Discover more at Serenity Counseling Group .
This was nicely structured. Discover more at http://www.newsdiffs.org/article-history/?url=https://www.bookmark-step.win/exactly-how-to-install-a-new-commode-seat-and-a-home-heating-duct .
I determined exactly what I crucial with empresa de mudanças for my latest relocation in Sorocaba SP—terrific provider!
Very helpful read. For similar content, visit casas rurales en Arzúa .
Moving is tough, but thanks to Sanderson’s expert team, it became an enjoyable experience—highly recommend them for any future moves you may have too! More details available at Long distance movers Sanderson !
Just had my home restored after severe flooding—what a relief to have professionals handle it! water damage restoration service near me
If you’re relocating to Palm Harbor, don’t forget to check out Palm Harbor movers for great deals!
Nicely detailed. Discover more at Affordable pest services in Hackettstown .
Sharing stories experiences allows growth underst water damage restoration services near me
This was a fantastic read. Check out fire damage restoration services Franklin Park for more.
Thanks for the great tips. Discover more at fast emergency pest control Long Valley .
Thanks for the detailed guidance. More at Sewer line repair Marion .
See what we’re offering leao
The heritage at the back of specific canine breeds is so attention-grabbing! What’s a breed that has a novel tale? http://usachannel.info/amankowww/url.php?url=https://pixabay.com/users/51193099/
I recently had a water emergency at my home in Irving, and I found the best help at water damage restoration near me . Highly recommend their services!
Water heater installation should be left to professionals—trust me; hiring someone experienced makes all the difference in ensuring everything runs smoothly! plumber
I appreciate these tips on maintaining good home health! Remember that timely intervention from ###can save significant costs down the line! water damage restoration near me
Knowledge shared the following will without doubt lead in opposition to more secure neighborhoods as other people take action!!! ##anythingKeywords## https://wiki-view.win/index.php/**Watch_Over_Your_Sanctuary:_The_Ultimate_Guide_to_DIY_Room_Security_Cameras**
In Essex, I lengthy had a wonderful encounter with a neighborhood roofer. After dealing with roof spills and the difficulties of smooth roof, I was struck by how quickly and skillfully the squad handled the maintenance essex roofing services
I appreciated this article. For more, visit Click for more info .
This was a fantastic resource. Check out año escolar en Irlanda for more.
I love it whenever people get together and share ideas.
Great site, stick with it! http://engel-und-Waisen.de/index.php/Enhance_Your_Own_Home_s_Curb_Attraction_With_A_Cobblestone_Driveway_In_Qu%C3%83_bec
Adopting Russianmarket fosters trust among clients. When customers know their information is handled with care, they feel more confident engaging with your services.
Genshin Impact has transform my renowned recreation just lately! If you are on the search for a dependable true-up heart, I enormously advocate ManaBuy Welkin Moon offers . They have the most effective prices!
Great article! It’s eye-catching to see how working out GPM can simply influence water utilization efficiency. I ordinarily wonder what the perfect stream rate is for the various household duties. https://www.plurk.com/p/3hgk3fuhzo
Hej! Ktoś już grał na https://www.ppfoto.cz/blog/sokotra-iicast-21.html? Sam trafiłem tam trochę z ciekawości i nie żałuję. Rejestracja trwała dosłownie dwie minuty, wersja PL działa bez zarzutu, co doceni każdy gracz. Na start dostałem bonus bez depozytu, więc mogłem ograć kilka slotów bez ryzyka. Kasyno działa szybko i stabilnie, nawet na mobilce. Promocje pojawiają się regularnie, a kody bonusowe to miły dodatek. Jak ktoś szuka czegoś nowego, a nie chce od razu inwestować kasy, to według mnie warto dać Spinmama szansę. Macie jakieś swoje typy na ulubione gry tam?
#Stress-free relocations are possible if you choose Best Ocala movers #
Appreciate the thorough insights. For more, visit secluded bar options in NYC .
Wonderful tips! Find more at commercial property broker .
A Les Paul is definitely worth the investment for any serious guitarist! What do you think? Share your views at Les Paul Supreme .
Thanks for the thorough analysis. Find more at ادمین اینستاگرام .
Well done! Find more at foothills paving and maintenance .
Wonderful tips! Discover more at ادمین اینستاگرام .
I love how undemanding you made it sound to fresh concrete! I’ll be because of those ideas soon. https://wiki-dale.win/index.php/Preserving_the_Integrity_of_Your_Walkway:_Gentle_Techniques_for_Cleaning
Appreciate the thorough write-up. Find more at auto repair Buckley .
I had a smooth experience with my long distance movers thanks to tips from Hialeah apartment movers .
Finally decided to give chiropractic care a shot—hoping for positive results from my #BonneyLakeChiropractor! # https://bonney-lake-chiropractor.lucialpiazzale.com/the-top-5-reasons-to-visit-a-chiropractor-in-bonney-lake-today-2
This was highly helpful. For more, visit apartamentos con piscinas .
I know this website presents quality depending content and
extra stuff, is there any other web page which provides such things in quality? https://Rentry.co/75240-injections-dacide-hyaluronique–guide-complet-pour-un-teint-radieux
Nicely detailed. Discover more at casas rurales en Arzúa .
This was very enlightening. More at Affordable pest management Hackettstown .
Appreciate the comprehensive advice. For more, visit Affordable Pest Solutions .
Thanks for the helpful article. More like this at Normandy Animal Hospital .
Custom home additions on Mercer Island can truly transform your living space! Whether you’re looking to expand your family room, add a home office, or create a beautiful outdoor living area, there are endless possibilities Sumner Home Remodel
The tips on building SEO through links are fantastic! Can’t wait to try out what’s available at Best place to buy backlinks .
Appreciate the detailed info on commercial vs residential tints! It’s helped clarify what I need when looking into window tinting Jeffersonville Indiana. Go to this website
Playing Genshin Impact is such a a laugh event! I’ve been riding ManaBuy official recharge for my higher-united statesand they always grant implausible mark downs. Give them a are trying!
When it comes to relocating in Sorocaba, I’ll at all times advocate #the specific provider of mudança em sorocaba !
Wow! The feedback on %%ANYKEYWORD%% is overwhelmingly positive; I’m eager to try them out myself. Cheap movers Yalaha
Anyone else love how trouble-free this is to work with execs like the ones at mudanças em sorocaba ?
Don’t underestimate how successful # anykeyword ### shall be while it comes time to relocate; they’re best suited! empresa de mudanças
Helpful suggestions! For more, visit trusted personal injury lawyer .
Thanks for the detailed guidance. More at ادمین اینستاگرام .
If you’re dealing with a rat infestation, it’s crucial to address it quickly to prevent health risks and property damage. Effective rat removal techniques can make a significant difference in maintaining a safe and clean environment Puyallup Pest Control
This was very beneficial. For more, visit Serenity Counseling Group .
This was very enlightening. For more, visit dog boarding near me .
Very informative article. For similar content, visit car accident doctor near me .
I love that classic rock sound that only a Gibson Les Paul can deliver! What songs do you play? Join in at Les Paul Jimmy Page Signature .
One of the best decisions we made was adding an en-suite bathroom during our loft conversion—so convenient! More insights on layouts can be found at Loft conversions Essex .
I found this very interesting. Check out ادمین اینستاگرام for more.
Love the emphasis on successful reinforcement! It makes this kind of change in training. If you’re concerned with greater advice, go to https://wakelet.com/wake/XAW1ylJX3IvxzQKXTanb6 for additional tools!
Just used this procedure to get free Genshin crystals, and I’m blown away via the outcome! Highly recommend every body provide it a shot! how to top-up UID on ManaBuy
Thanks for the useful post. More like this at All Dry Services of Seattle .
I found this very interesting. Check out Heating contractor for more.
Hormone therapy has made a huge difference in my life. If you’re considering it, I recommend visiting Centralia Hormone therapy for valuable insights.
Great job! Discover more at local knee pain relief Boise .
This was a wonderful guide. Check out año escolar Irlanda for more.
I found this very helpful. For additional info, visit TheWinnslow .
Hi there, yes this paragraph is really good and I have learned lot of things from it regarding blogging.
thanks.
I just had my dome repaired by a great staff of roofers in Essex, and I can’t stress enough how crucial it is to pick the best roofing company roofer essex
Love this content! The idea of buying safe backlinks through Buy backlinks for website seems very promising.
Thanks for the valuable insights. More at Emergency Pure Plumbing .
Thanks for the valuable insights. More at ادمین اینستاگرام .
I enjoyed this article. Check out find Farsi psychotherapy services for more.
Valuable information! Discover more at ادمین اینستاگرام .
Helpful suggestions! For more, visit Affordable Pest Solutions .
Well done! Find more at Pest Removal Long Valley .
Appreciate the thorough insights. For more, visit apartamentos con piscinas .
This was quite informative. For more, visit http://italianculture.net/redir.php?url=https://www.stealth-bookmark.win/how-to-determine-and-deal-with-plumbing-and-home-heating-leakages .
I liked this article. For additional info, visit casa rural Arzúa .
Wonderful tips! Find more at http://www.vab.ua/bitrix/rk.php?goto=https://mehmetnuriarslan.com/user/brennattjc .
Nicely done! Find more at Gutter cleaning .
Do any of you have tips on preparing fragile items when working with movers like those at #DallasMovingCompany? Dallas moving companies
I learned the hard way that neglecting your unit can lead to costly repairs!” # # anyKeyWord ## AC repair Hutto
Water can cause so much unseen damage; thank goodness for restoration experts like water damage restoration near me who know how to fix it!
Anyone else used Office moving companies Jamaica ? I’m curious about your thoughts on their services!
Thanks for the great explanation. More info at groene hart klimaatregeling pro .
Excellent information on Essex’s cladding sector! For ceiling repairs and setups, it’s crucial to pick a respectable# #anykeyword## company. Being able to rely on a trustworthy roofer given the weather conditions we have is essential roofer essex
No hidden fees or surprises whatsoever when working alongside these professionals—it’s all clear upfront!!! Jacksonville movers
Many people fear that bankruptcy will ruin their credit forever, but that’s not necessarily true. With proper planning and financial management post-bankruptcy, individuals can gradually rebuild their credit score bankruptcy lawyer
If you live in Irving TX and face water issues, don’t hesitate to call a professional for help! water damage restoration services near me
I found your tips on local SEO super beneficial! For additional insights, visit marketing blog .
เคยไปงานเลี้ยงที่ร้านเหล้าสาย1 มาประทับใจมากครับ ร้านเหล้าสาย1 เพลงมันส์
This was a great article. Check out año escolar en Irlanda for more.
It’s amazing how quickly professionals can restore a home after water damage! Highly recommend it! water damage restoration services near me
This was very beneficial. For more, visit TheWinslow .
Such crucial conversations happening around town lately regarding preparedness which hopefully inspires action among others facing similar circumstances nearby too!!!! #Anykeword# water restoration near me
Hopefully others find similar success stories amongst fellow clients who’ve shared positive feedback regarding experiences had recently themselves!!## any Keyword ## Jacksonville moving company
Martial arts not just improve fitness however also impart discipline and emphasis in practitioners. It’s interesting to see exactly how various designs, from karate to jiu-jitsu, deal distinct benefits Denver karate kids
Knowing where to turn after experiencing water damage is so important; thankfully we have places like water damage restoration companies near me here in Clive!
Just moved to Irving, TX, and I’m already learning about water damage risks. Glad I found water damage restoration service near me for future reference!
Mercer Island is such a beautiful place to live, and home remodeling can truly enhance its charm! I recently completed a project that transformed my living space into a more functional and inviting area Sumner Home Remodel
Thanks for the great tips. Discover more at foothills paving and maintenance .
This was very enlightening. For more, visit ادمین اینستاگرام .
The tonal range of the Gibson Les Paul is phenomenal, from jazz to metal! What genres do you play? Tell us at Les Paul Stopbar Tailpiece .
#Relocating soon? Trust me; you’ll want Ocala full service movers # on your side.
You’ve come to the right place if you’re looking for trustworthy and knowledgeable roofers in Essex. Maintaining your roof is essential given the varying weather circumstances we frequently experience roofer essex
Appreciate the helpful advice. For more, visit best commercial property broker .
Appreciate the helpful advice. For more, visit Afordable Pest Solutions .
I found this very interesting. For more, visit Affordible Pest Solutions .
This was very insightful. Check out ادمین اینستاگرام for more.
Great insights! Discover more at personal injury attorney representation .
If you prefer peace of thoughts at some point of your transfer, agree with mudança em sorocaba – they may be the greatest in Sorocaba!
Great job! Discover more at mobile locksmith .
I’ve recently had a huge problem with pests in my home, and I didn’t know where to turn Pest Control Puyallup
This was a great help. Check out apartamentos turísticos for more.
So joyful I chose mudanças em sorocaba ! Their team took care of every little thing for the period of my latest relocation.
Just desired to share my triumphant feel with empresa de mudanças . They incredibly recognise the way to deal with actions in Sorocaba!
The efficiency of Cheap movers Hialeah during my Hialeah move was impressive!
This was very beneficial. For more, visit locksmith high point nc .
What a relief it was to hire Silver Springs commercial movers for our recent office move! Highly recommend them to anyone in Silver Springs.
This was very enlightening. For more, visit east coast locksmith .
Need a facelift for your exterior? Ask us about our exterior home renovations in Sumner — big results with major curb appeal. Sumner Home Remodel
This was quite useful. For more, visit Persian Therapist Near Me .
It’s interesting to see how common AC repairs can add up! Knowing the average costs helps in budgeting for maintenance. For more info, check out ac repair Las Cruces NM. air conditioning repair near me
I’m so grateful for the advancements in hormone therapy! For those looking into clinics, I recommend checking out Centralia Hormone therapy to find the right fit.
This was quite useful. For more, visit Foot Hills Paving .
I can’t believe how much I’ve saved on energy bills since switching to a ductless mini-split system! AC repair Hutto
This was highly educational. More at ادمین اینستاگرام .
This is quite enlightening. Check out motor vehicle accident lawye for more.
What’s up, its pleasant piece of writing about media print, we all know media is a wonderful
source of data.
Have you participated in any guitar forums discussing Les Pauls? They’re full of great tips! Check one out at Gibson Les Paul Classic .
Appreciate the detailed information. For more, visit ادمین اینستاگرام .
Excellent information on Essex’s roofer sector! For roof repair and maintenance, it’s crucial to find trustworthy# #anykeyword##. Being able to have a well-maintained dome is important for any buyer given the uncertain weather we frequently experience roofing contractors essex
I appreciate how transparent the pricing is with Yalaha Mover’s —no hidden fees!
Proudly standing united amidst diversity recognizing strength lies within collective efforts shared vision mutual respect underst Plant City movers
Really happy with my new dentist in Newnan! They explained everything so well! dentist newnan ga
Has anyone used packing services from Local movers Margate ? I’m curious how well they handle fragile items.
Everything is very open with a clear clarification of the challenges.
It was really informative. Your site is extremely
helpful. Thanks for sharing!
Appreciate the thorough insights. For more, visit Groene Hart Klimaatregeling Pro .
Thanks for every other fantastic article. The
place else may just anybody get that type of info in such a perfect way of writing?
I’ve a presentation next week, and I’m at the search for such information. https://cgv.Org.ru/forum/go.php?http://Dragon-slave.org/comics/RhodayoTangvj
Our company’s relocation was flawless thanks to the hard work of the team at Best Macclenny movers .
If you’re unsure about where to start with your loft conversion, there are plenty of resources available online like those found at Loft conversions Essex !
Thanks for every other fantastic article. The place else may
just anybody get that type of info in such a perfect way of writing?
I’ve a presentation next week, and I’m at the search for such information. https://cgv.Org.ru/forum/go.php?http://Dragon-slave.org/comics/RhodayoTangvj
This was a great help. Check out TheWinslow for more.
Shoutout to water damage restoration companies near me for their quick response time during my family’s emergency situation!
ไม่เคยผิดหวังกับการไปที่ OMG ONE MORE GLASS SAI1 เลย ทุกครั้งที่ไปสนุกมากๆ ร้านนั่งชิล สาย1
So grateful for the help from my Rockledge apartment movers; they were amazing! Rockledge full service movers
Love this content! The idea of buying safe backlinks through Buy backlinks that improve ranking seems very promising.
Searching for local remodeling contractors you can trust? Our design-build process makes renovations seamless.
Remodel Company
Appreciate the detailed information. For more, visit Air conditioning repair service .
The importance of professional water damage restoration cannot be stressed enough—especially here in Irving TX! water damage restoration near me
Really appreciate posts highlighting collaborative efforts between nonprofits/government agencies focused specifically helping low-income families recover from losses sustained due unfavorable circumstances… water and mold restoration near me
Thanks for the helpful article. More like this at Persian Language Therapist .
Really informative post, especially since more people need awareness regarding how quickly things escalate during rainstorms–great job covering this topic!! water damage restoration services near me
This was a great article. Check out ادمین اینستاگرام for more.
Thanks for the great tips. Discover more at ماساژ ماهور .
Fantastic post! Discover more at Fast emergency pest control Hackettstown .
If you value it slow and sanity all the way through a cross, employ mudança em sorocaba ! You cannot remorseful about it.
This is quite enlightening. Check out affordable residential pest control Long Valley for more.
My mates recommended empresa de mudanças , and now I’m passing on the phrase—they are dazzling!
I was once pleasantly amazed by using how inexpensive mudanças em sorocaba is for the first-class of carrier they supply!
Thanks for discussing such an essential topic—water preservation is key! Keep ###in mind if you face any emergencies locally! restoration companies in my area
Please let me know if you’re looking forr a writer
for your weblog. You have some really good artjcles and I think I would be a good asset.
If you ever want to take some of tthe load off,
I’d really like to write sime content for your blog iin exchange for
a link back to mine. Please send me an e-mail if interested.
Thanks!
Feeel free to vijsit my web blog :: Samsun temizlik şirketi
Just got back from an awesome trail ride near Jacó, and I can’t stop talking about it! Thanks, Costa Rica horse tours , for the memories!
Just completed a project with the help of flood restoration companies near me after severe weather affected my property—very satisfied with their work!
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
This was a great help. Check out apartamentos turísticos Arzúa for more.
Thanks for the thorough analysis. More info at casa rural .
Thanks for the helpful advice. Discover more at fire damage restoration services .
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Appreciate the thorough analysis. For more, visit trusted Sewer line repair near me .
Thanks for the helpful advice. Discover more at expert same day plumbing .
Clearly presented. Discover more at buy commercial property near me .
This was quite helpful. For more, visit Exclusive private room bar NYC .
This was very beneficial. For more, visit LuxeNeuro .
Great insights! Discover more at groene hart klimaatregeling pro .
Great insights! Find more at Foot Hills Paving .
Well explained. Discover more at ماساژ ماهور .
It’s remarkable to visit this website and reading the views
of all friends about this post, while I am also zealous of getting experience. https://Jguitar.com/tabmap?url=https%3A%2F%2Ftheoretetfils.com%2Fdriveway-construction-in-saint-colomban-qc%2F
It’s remarkable to visit this website and reading the views of all friends about this post, while I am also zealous
of getting experience. https://Jguitar.com/tabmap?url=https%3A%2F%2Ftheoretetfils.com%2Fdriveway-construction-in-saint-colomban-qc%2F
Because the admin of this web page is working,
no doubt very quickly it will be famous, due to its quality contents.
Genuinely no matter if someone doesn’t be aware of after that its up to other users that they will assist, so here it takes place.
Thanks for the helpful article. More like this at Dental Group Beverly Hills .
Awesome article! Discover more at Residential Pest Control Hackettstown .
ถ้ามีเวลาว่าง อยากจะอยู่ที่นี่ตลอดทั้งคืนเลยค่ะ # # anyKeyWord## ผับจัดวันเกิด สาย1
Thanks for the valuable insights. More at ادمین اینستاگرام .
Thanks for the helpful article. More like this at pest prevention services Long Valley .
This was a great article. Check out ادمین اینستاگرام for more.
It’s interesting to see how common AC repairs can add up! Knowing the average costs helps in budgeting for maintenance. For more info, check out ac repair Las Cruces NM. air conditioning repair near me
Appreciate the detailed insights. For more, visit Afordable Pest Solutions .
” Celebrating diversity strengths nurtures collaboration enhances productivity fosters innovation creates inclusive spaces encouraging creativity inspiring transformation collectively flourishing beautifully uniquely distinctly profoundly enriching snowcone rentals
This was beautifully organized. Discover more at casas rurales en Arzúa .
Appreciate the thorough insights. For more, visit apartamentos turísticos .
I appreciated this post. Check out Affordible Pest Solutions for more.
Who knew finding a great cosmetic dentist could be this easy here in Newnan, GA?! So happy with my results! affordable dentist newnan ga
Appreciate the detailed information. For more, visit Furnace repair service .
Thank you for sharing your knowledge! I’m eager to improve my site’s rankings with help from Dofollow backlinks for sale .
Don’t forget about soundproofing when converting your attic; it’s essential for privacy in shared spaces—excellent advice available on Loft conversions Essex
This was very beneficial. For more, visit Persian Therapist Near Me .
This is quite enlightening. Check out LuxNuro for more.
Appreciate the great suggestions. For more, visit paving and repair Wheat Ridge .
Helpful suggestions! For more, visit ماساژ ماهور .
Thanks for the great tips. Discover more at ادمین اینستاگرام .
I enjoyed this post. For additional info, visit Beverly Hills Dental Group .
There is definately a great deal to find out about this subject.
I really like all the points you have made. https://sitereport.netcraft.com/?url=http://www.Foot-palmares.com
I recently had a pest problem in my home, and I was amazed by the effective solutions offered by local services. It’s crucial to choose a knowledgeable pest control provider in Puyallup to ensure a pest-free environment Pest Control Puyallup
I enjoyed this article. Check out best Floor Refinishing near me for more.
Thanks for the helpful article. More like this at Affordable Pest Solutions .
Scheduling regular maintenance for my AC has made such a difference in performance! AC installation
Appreciate the thorough insights. For more, visit ادمین اینستاگرام .
Your article has motivated me to take in drone photography as a activity! Excited to be trained greater innovations from you! Visit https://edelinxema.contently.com for greater facts.
Nicely done! Find more at Bar with Private Room NYC .
Thanks for the clear breakdown. Find more at Affordible Pest Solutions .
Thanks for the detailed guidance. More at deck builder company near me .
If you might be trying to find satisfactory moving expertise in Sorocaba SP, appearance no additional than ###! mudança em sorocaba
After utilizing mudanças em sorocaba , I’ll on no account strive any other DIY pass lower back!
I recently moved to Dallas and found the best apartment movers! Highly recommend checking out Dallas apartment movers for your next move.
I really love your website.. Excellent colors & theme.
Did you build this site yourself? Please reply back as I’m wanting to create
my very own website and want to learn where you got this from or what the theme is called.
Thank you!
Thanks for the helpful article. More like this at Serenity Psychotherapy Group .
If you’re looking for an efficient way to relocate within or outside of town, look no further than this superb local mover in Hilliard—visit them today on Cheap movers Fort Liberty # !
Every single interaction I’ve had with felon plumber has been nothing short of amazing!!! # # anykeyword ## capitola plumbers
“Just finished relocating my business with #Anykeyword – couldn’t have asked for better service!” Macclenny movers
This was quite informative. For more, visit ماساژ ماهور .
Wonderful tips! Find more at Afordable Pest Solutions .
Just moved down here, and thanks to # anyKeyboard#, it was way less stressful than expected! Local movers Jacksonville
I enjoyed this post. For additional info, visit plumbing company .
Just wished to claim how convinced I became with the carrier from empresa de mudanças during my fresh relocation.
Fantastic service from start to finish! I’ll definitely recommend restoration companies in my area to anyone needing restoration help.
Why users still make use of to read news papers when in this technological world all is available on net?
Very informative post! Your tips on influencer marketing are invaluable. More at blackhat marketing blog .
This publish is ideally suited for anyone new to drones. The factors are transparent and concise! Find further elements at https://wiki-spirit.win/index.php/**Mastering_the_Skies:_Essential_Tips_for_Capturing_Stunning_Images_with_Your_Drone_Camera** .
Thanks for the insightful write-up. More like this at ادمین اینستاگرام .
Excellent information on Essex roofing companies! For any ceiling restoration or setup project, it’s crucial to pick a trustworthy roofer, mainly with the varying weather conditions roofers Chelmsford
Helpful suggestions! For more, visit casas rurales en Arzúa .
This was quite useful. For more, visit ادمین اینستاگرام .
Everyone’s enthusiasm towards ##### # makes me excited about starting my own journey soon! Ocala apartment movers
Appreciate the comprehensive advice. For more, visit apartamento turístico Arzúa .
The process of restoring from water damage is fascinating yet daunting; glad we have professionals in Irving TX! water damage restoration services near me
This is quite enlightening. Check out toilet replacement cost for more.
Thanks for the helpful advice. Discover more at affordable blocked toilet repair .
Thanks for the clear breakdown. More info at good plumbers near me .
Excited see new trends emerging surrounding home maintenance practices aimed specifically combating issues like these effectively whenever possible too!!!#Anykeyword# water damage restoration near me
Thanks for the clear breakdown. More info at TheWinslo .
What’s up to every one, the contents existing at this site are really remarkable for people experience,
well, keep up the good work fellows. https://pipewiki.org/wiki/index.php/Boutique_De_Fine_Alimentation_:_D%C3%83_couvrez_La_Splendeur_Gastronomique
What’s up to every one, the contents existing at this site are really remarkable for people experience, well,
keep up the good work fellows. https://pipewiki.org/wiki/index.php/Boutique_De_Fine_Alimentation_:_D%C3%83_couvrez_La_Splendeur_Gastronomique
This was nicely structured. Discover more at LuxeNeuro .
Shoutout to the team at Local movers Dundee for their outstanding support during my recent move in Dundee!
Many people fear that bankruptcy will ruin their credit forever, but that’s not necessarily true. With proper planning and financial management post-bankruptcy, individuals can gradually rebuild their credit score bankruptcy lawyer
Good read about dealing with unexpected flooding situations—remembering that local teams like ###are just a call away is comforting! restoration companies in my area
The right restoration company makes all the difference! Irving residents should definitely consider water damage restoration service near me for their water damage issues.
Wonderful tips! Find more at Foothills Paving .
I can’t believe how much easier my move was after consulting with Cheap movers Hialeah .
Fighting style not just enhance fitness however likewise impart discipline and focus in experts. It’s interesting to see just how various styles, from martial arts to jiu-jitsu, offer unique benefits Denver Taekwondo classes
Appreciate the great suggestions. For more, visit Beverly Hills Dental Group .
Thanks for the great information. More at Afordable Pest Solutions .
Well explained. Discover more at Affordible Pest Solutions .
I used to be suggested this blog by my cousin. I’m no longer certain whether
this post is written by him as nobody else know such specified about my trouble.
You are incredible! Thank you!
”Relying solely on window units wasn’t cutting it; glad I switched to central air!” ###= > AC repair Georgetown
Hello, i read your blog from time to time and i own a similar one and i was just wondering if you get a lot of spam comments?
If so how do you reduce it, any plugin or anything you can suggest?
I get so much lately it’s driving me insane so any assistance is very much appreciated.
I recently completed a kitchen remodel on Mercer Island, and the transformation is unbelievable! It’s amazing how a new layout and updated appliances can completely change the feel of a home Sumner Home Remodel
Nicely done! Find more at ماساژ ماهور .
Does anyone else have a ‘dream’ version of their perfect Gibson Les Paul in mind that they wish existed? Let’s brainstorm ideas together over at Les Paul vs Stratocaster
Helpful suggestions! For more, visit Afordable Pest Solutions .
I appreciated this article. For more, visit best personal injury attorney services .
A big thumbs up for the professionalism displayed by everyone at Greenacres Mover’s during our move last week! Greenacres moving companies
Anyone else love how ordinary it truly is to work with mavens like those at mudança em sorocaba ?
Thanks for the comprehensive read. Find more at https://escatter11.fullerton.edu/nfs/show_user.php?userid=8972947 .
پروتئین وی ایزوله ویسلی، پودری با 6 گرم BCAA و 14 گرم EAA در هر سروینگ است که با روش میکروفیلتراسیون جریان متقاطع تولید میشود. میکند.
Have you thought of hiring professional movers? You must always easily fee out mudanças em sorocaba #!
This was highly educational. For more, visit casas rurales Arzúa .
This was highly educational. More at ادمین اینستاگرام .
If you’re dealing with a rat infestation, it’s crucial to address it quickly to prevent health risks and property damage. Effective rat removal techniques can make a significant difference in maintaining a safe and clean environment Pest Control Puyallup
This was very enlightening. For more, visit Serenity Counseling Group .
Just wanted to give a shoutout to the amazing team at # # anykeyword # # that helped me during my recent move! Yalaha apartment movers
Clearly presented. Discover more at luxury camping vans .
Love your perspective on this topic! Can’t wait to enhance my site’s authority with links from Buy backlinks for niche sites and blogs !
This was highly useful. For more, visit brain mapping evaluation in Denver .
Grateful reflection moments spent learning growing developing relationships built upon trust respect honesty integrity transparency accountability responsibility empowerment inspiration motivation energization invigoration stimulation activation Plant City movers
Just moved into my new residence with the assist of empresa de mudanças , and it was once correct!
Valuable information! Discover more at Wheat Ridge Driveway Asphalt Paving .
Is there a dental clinic in Newnan that offers sedation dentistry? I’m quite anxious about visits. coweta dentistry newnan ga
I found some of the best rates on moving services through Margate international movers .
If you’re having doubts about whether or not to hire them, trust me; just do it & thank me later!!! # # anykeyword ## Watsonville plumbers
Hi there, everything is going nicely here and ofcourse every one is sharing
facts, that’s actually fine, keep up writing.
Madura United FC
Thanks for the thorough analysis. More info at ماساژ ماهور .
อะไรคือสิ่งที่คุณชอบที่สุดเกี่ยวกับไฟหน้ารถ LED? หลอดไฟ รถ
This was very beneficial. For more, visit Sewer line repair .
Who knew there was so much potential in an unused attic? Explore great ideas for your space at Loft conversions Essex .
Thanks for breaking down the average costs of AC repairs. It’s helpful to know what to expect before calling someone. If you’re in need of assistance, consider checking out ac repair Las Cruces NM. air conditioning repair Las Cruces
ไวน์ที่ร้านเหล้าสาย1 คุณภาพดีมากครับ แนะนำเลย ร้านเหล้าสาย1 เพลงเพราะ
This was nicely structured. Discover more at repiping experts .
For anyone planning a move in Ocala, you should definitely hire Best Ocala movers .
I cannot stress enough how important it is to have professionals like ###Anykeyword### available when disaster strikes. flood restoration companies near me
This was quite helpful. For more, visit TheWinslow .
There’s something magical about playing a vintage Les Paul; it feels like holding history in your hands! Experiences shared at Les Paul Maple Top .
Appreciate the thorough insights. For more, visit Affordable Pest Solutions .
This was beautifully organized. Discover more at ادمین اینستاگرام .
#Appliance store nearby# had some excellent clearance items last time I visited. wholesale appliances
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
A rigidity washing machine with round 2000-2500 PSI is perfect for most decks. Just be aware to preserve the nozzle at a safe distance! For extra recommendations, see https://www.instapaper.com/read/1849833565 .
Appreciate the useful tips. For more, visit mobile locksmith .
Nicely done! Find more at locksmith high point nc .
Thanks for the great tips. Discover more at gastonia locksmith .
Excellent article! Finding trustworthy## Roofers in Essex## can be difficult, but it’s essential to uphold your home’s morality roofer essex
Thanks for the great information. More at Roof repair service .
Wow, the impact of water damage can be devastating! Glad to see so many restoration options in Irving TX. restoration companies in my area
Well explained. Discover more at Serenity Therapy Group .
If you ever find yourself in need of restoration services in Council Bluffs, know your options are abundant! water damage restoration near me
Wonderful tips! Discover more at Environmentally friendly pest control Hackettstown .
Junk disposal services in Perth supply a effortless resolution for eliminating unwanted models responsibly and ethically. Cheap Rubbish Removal Perth
Thanks for the great explanation. More info at Commercial Pest Control Long Valley .
Thank you for sharing your expertise! I’m considering investing in backlinks from Buy backlinks instantly now!
When I originally commented I seem to have clicked the -Notify me when new
comments are added- checkbox and from now on each time a comment is added I recieve
4 emails with the exact same comment. Is there a means you can remove me from
that service? Appreciate it!
I’m relatively concerned about the future of crypto! Felysyum Token looks gaining traction and may very well be probably the most foremost appearing cryptocurrencies in 2025. Can’t wait to look the place it is going! Check out more at Felysyum Token news .
After my recent flood experience, I can’t stress enough how crucial it is to have a good restoration team—like those at ###in Clive. water damage restoration services near me
Preventing future leaks is on my mind now more than ever; glad there are resources like ### anyKeyword### available nearby! restoration companies in my area
Your locksmith experience is evident in the caliber of your do the job plus the positive opinions from content shoppers in Melbourne. Sustain the excellent support! Reliable Emergency Locksmith Melbourne
Hi! I know this is kinda off topic but I was wondering if you knew where I could get a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having trouble finding one?
Thanks a lot! http://dragon-Slave.org/comics/JasonkvValentexe
Hi! I know this is kinda off topic but I was wondering if you knew where
I could get a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having trouble finding one?
Thanks a lot! http://dragon-Slave.org/comics/JasonkvValentexe
Bankruptcy can be a daunting experience, but it’s important to remember that it’s not the end of the road. Many individuals and businesses have successfully rebuilt their financial lives after filing for bankruptcy bankruptcy lawyer
Has anyone had feel practising stubborn breeds like Bulldogs or Terriers? Tips would be liked! http://appyet.com/handler/disqus.ashx?guid=713ae0d41568487bb47b9d09585fe482&id=45fee95b8971b2435e0570d007b5f281&locale=ar&shortname=aqoal&title=&type=1&url=https://jasperfzvz461.theglensecret.com/captive-care-of-the-north-american-field-turtle
An emergency electrician is like a superhero in times of misery, all set to deal with any electric situation quickly and correctly. Strata Electricians in Perth
This was very enlightening. More at ماساژ ماهور .
Fighting style not only boost physical conditioning however additionally infuse technique and emphasis in specialists. It’s fascinating to see how different designs, from karate to jiu-jitsu, offer distinct benefits Denver Taekwondo classes
This is very insightful. Check out http://www.bausch.in/en-in/redirect/?url=https://www.bookmarkpage.win/the-advantages-of-preventative-pipes-and-heating-upkeep-1 for more.
Thanks for the helpful article. More like this at expert plumbing expertise .
Appreciate the helpful advice. For more, visit casa rural .
Thanks for the clear breakdown. More info at apartamento turístico Arzúa .
This was quite informative. For more, visit septic tank service near me .
Appreciate the thorough insights. For more, visit LuxNuro .
This was very enlightening. For more, visit mold remediation lake forest wa .
Thanks for the great information. More at ادمین اینستاگرام .
Thanks for the great explanation. Find more at Family Law Attorney Richmond VA .
I appreciate how you tackled the subject of customer feedback! I’ve discussed this extensively at blackhat marketing blog .
Great tips! For more, visit Foothills Paving .
This was a wonderful post. Check out windshield chip repair charlotte for more.
I hope %%%%ANOTHER_KEY_WORD%%% has good customer support—I want peace of mind during my move. Yalaha Mover’s
I absolutely agree that consistency is essential in puppy coaching. Your insights are spot on! For greater distinct guides, take a look at out https://atavi.com/share/xchs8ozl92i9 .
Bitchat download has quickly become my go-to for chatting with friends—can’t recommend it enough! free Bitchat download
Thanks for the helpful article. More like this at Dental Group Beverly Hills .
This was a wonderful guide. Check out Affordible Pest Solutions for more.
Valuable information! Find more at Affordible Pest Solutions .
The foremost decision I made turned into hiring mudança em sorocaba for my residential relocation in Sorocaba SP!
Anyone else use mudanças em sorocaba not too long ago? I’d like to hear your suggestions on their transferring features.
Useful advice! For more, visit Afordable Pest Solutions .
Thanks for the detailed guidance. More at ماساژ ماهور .
#Overstock appliances# can save you a bundle—definitely worth exploring! scratch and dent appliance store
This was a wonderful post. Check out Affordable Pest Solutions for more.
Finding a competent roofer in Essex may be everything. It’s crucial to decide experienced professionals whether you need roofing repairs, a full roof replacement, or specialized services like straight roofing essex roofing services
Kudos once again towards everyone who shares knowledge openly—it aids countless individuals seeking assistance regularly including myself since coming upon links provided here via : ### San Diego County Roofing & Solar
A friend introduced me to classic rock through his Les Paul, and now I’m hooked! What got you started? Let’s chat at Les Paul vs SG .
Excited about enhancing curb appeal through collaboration with skilled experts at . roofer in san diego
My roof was leaking, and after calling jcis roofing escondido , they resolved it quickly and efficiently.
So comfortable I hired empresa de mudanças for my relocation! They made everything so clean and drawback-loose.
This was quite informative. For more, visit apartamentos turísticos Arzúa .
Thanks for the practical tips. More at ادمین اینستاگرام .
This was quite helpful. For more, visit casa rural .
I’m amazed by how much my lifestyle has improved with extra living space from my recent conversion—check out success stories on Loft conversions Essex !
This was quite useful. For more, visit supportive Farsi therapy counselor .
I am truly pleased to read this web site posts which contains tons of
helpful information, thanks for providing these
kinds of information.
I enjoyed this article. Check out ادمین اینستاگرام for more.
This was quite useful. For more, visit motor vehicle accident lawyer near me .
I enjoyed this article. Check out Denver innovative brain technologies for more.
Thanks for the great tips. Discover more at Foothills Paving .
Thanks for the valuable insights. More at Dental Group Beverly Hills .
I have an understanding of how you highlighted the significance of having a pre-flight record! It’s some thing every pilot must always follow. Discover greater assets at https://speedy-wiki.win/index.php/**Exploring_Scenic_Landscapes:_How_to_Use_a_Drone_Camera_for_Breathtaking_Travel_Photos** .
I’ve been following countless crypto trends, and Felysyum Token is right now growing one in all my favorites for 2025! What do you all feel? Join the dialogue at buy Felysyum !
This was highly helpful. For more, visit Affordable Pest Solutions .
Moving companies can be hit or miss, but I trust Cheap movers Dallas based on my experience.
ฉันชอบเพลงที่เล่นในร้าน OMG ONE MORE GLASS SAI1 มาก มันทำให้รู้สึกมีชีวิตชีวา ร้านอาหารสาย1
This was a fantastic read. Check out Boutique bar with private room NYC for more.
This was quite informative. For more, visit Afordable Pest Solutions .
Such a watch-opener! I in no way found out that special sports require different circulate quotes. This skills will clearly assist me make extra educated judgements shifting forward. http://www.video-bookmark.com/user/claryapiuq
Finding reputable movers can be hard; luckily we discovered #### anyKeyWord###! Office moving companies Jamaica
Would absolutely recommend anyone seeking guidance concerning moves reach out directly ; exceptional talent shines bright amongst competition below surface level —discover how simple things could become accessing # # anykeyword### Hilliard moving companies
Thanks for the detailed guidance. More at ادمین اینستاگرام .
Taking pride knowing exactly whom we entrusted when navigating complexities involved concerning transitions spanning across multiple facets ensured nothing overlooked despite challenges faced uniquely throughout journey experienced indeed: #: anyKeywod#! Long distance movers Hempstead
The resonance of a well-crafted Gibson Les Paul is something every guitarist should experience! More on this topic at Les Paul Sound .
If you’re relocating soon, check out # anyKeyword#; they offer amazing deals on moves! Jacksonville commercial movers
Thanks for the insightful write-up. More like this at local Farsi therapy services .
Office moving companies in Waco have come a long way! Great insights shared at Office moving companies Waco .
Thanks for the clear advice. More at repiping experts .
This was highly educational. For more, visit ادمین اینستاگرام .
My feel with movers has at all times been combined till I determined out approximately mudança em sorocaba – basically a sport changer!
This was very beneficial. For more, visit Affordable Pest Solutions .
For somebody in Sorocaba SP needing legit shifting providers, mudanças em sorocaba is the method to move!
Reliable, high-quality, on-time — that’s how we define our Sumner construction services.
Home Remodel Sumner
It’s comforting knowing that there are reliable companies like water damage restoration near me here in Ellenwood for water damage emergencies.
Anyone else in Perth notice an growth in safeguard after installing programs from organisations like Strata Building Security Perth ?
This post is truly informative; can’t wait to try out the backlink services offered by Manual backlink service #!
So pleased I found out out approximately empresa de mudanças —they absolutely realize tips to make transferring trouble-free.
I’m glad I found a reliable water damage restoration service in Irving TX when my basement flooded last year! flood restoration companies near me
Well done! Discover more at ماساژ ماهور .
Grateful for all the tips on maintaining a dry home and avoiding future damages—very practical advice here!! water damage restoration near me
Shoutout to all those who shared their experiences about different companies on ###ANYKEYWORD#### —it helped me choose wisely! atlas roofing
This was a wonderful post. Check out plumbing repair near me for more.
If you’ve been Googling remodeling contractors near me, you’ve found the right crew — local, experienced, and client-focused.
Remodel Company
This was highly educational. For more, visit casa rural Arzúa .
I found this very interesting. For more, visit affordable messenger bag patterns .
Excellent write-up For roofer projects, it’s crucial to pick the appropriate professionals, particularly in Essex, where the weather can be very difficult. I’ve personally witnessed how crucial it is to employ seasoned# #anykeyword## roofing contractors essex
This was highly educational. For more, visit ادمین اینستاگرام .
Appreciate the thorough insights. For more, visit ادمین اینستاگرام .
I found this very helpful. For additional info, visit Dental Group Beverly Hills .
Great insights! Find more at Hackettstown affordable extermination .
Thanks for highlighting affordable options! Looking forward to contacting Dundee apartment movers soon.
I had such a positive experience with Greenacres moving company. They are true professionals! Greenacres moving company
Appreciate the detailed post. Find more at Eco-Friendly Pest Control Long Valley .
This was a fantastic read. Check out auto glass repair charlotte for more.
This is quite enlightening. Check out Afordable Pest Solutions for more.
I found Yalaha commercial movers online and decided to give them a try for my Yalaha apartment move. No regrets!
Thanks for the insightful write-up. More like this at AC installation Hutto .
Anyone else love finding bargains on appliances? Check out what’s available at appliance liquidators .
Hey there, You’ve done a fantastic job. I will definitely
digg it and personally recommend to my friends.
I’m confident they will be benefited from this web site. http://www.gz-jj.com/comment/html/?561073.html
Marvelous, what a website it is! This weblog presents useful data
to us, keep it up. https://r12Imob.store/index.php?page=user&action=pub_profile&id=412707
Hey there, You’ve done a fantastic job. I will definitely digg it and personally recommend
to my friends. I’m confident they will be benefited from this web site. http://www.gz-jj.com/comment/html/?561073.html
This was nicely structured. Discover more at must-have camping stuff .
So glad there’s a variety of specialists available among dentists here; makes finding one much easier! ##anyKeyword ## dentist near me
Thank you, Best Margate movers , for making my move cost-effective and hassle-free.
Just wanted to say that I found the perfect moving company via Brooklyn international movers #.
This was quite useful. For more, visit apartamento turístico Arzúa .
Thanks for the useful suggestions. Discover more at ماساژ ماهور .
The sustain on a Gibson Les Paul is unmatched. It really brings out the depth in your music. Discover more at Les Paul Goldtop .
Thanks for the great tips. Discover more at ادمین اینستاگرام .
Appreciate the thorough insights. For more, visit casas rurales en Arzúa .
Just moved with help from Lawtey international movers, and it was so worth it! Thank you, Lawtey apartment movers !
Glad we chose 78 . Clearwater movers
Appreciate the detailed information. For more, visit ادمین اینستاگرام .
I found this very interesting. For more, visit Emergency Oral Care Beverly Hills .
This is such valuable information! I will consider using Manual backlink service to boost my website’s visibility.
มีเรื่องราวดี ๆ เกิดขึ้นเยอะเมื่อมาเที่ยวที่นี่ # # anyKeyWord## ผับจัดวันเกิด สาย1
Thanks for the clear breakdown. More info at Affordible Pest Solutions .
Great job! Find more at auto glass repair charlotte .
Dealing with unexpected water issues is stressful; grateful I found out about water damage restoration companies near me # when I did!
This was a great help. Check out Afordable Pest Solutions for more.
In Essex, I recently had some cladding job done, and I can’t emphasize enough the importance of hiring the best roofer. Finding one that cares about quality and customer happiness in Essex is get overwhelming given the number of cladding firms roofing company essex
I love exploring new cryptocurrencies, and Felysyum Token is in reality one which sticks out! Could it be one of several high-quality performing cryptocurrencies in 2025? Let’s find out in combination at Felysyum Token review !
Couldn’t have confidence how promptly and correctly they handled my circulation—thanks, mudança em sorocaba #!
Everyone deserves safe living environments free from worry while ensuring structures remain standing strong despite mother nature testing limits continually throughout year round too!!!! #Anykeword# water damage restoration companies near me
Just wished to focus on how titanic my trip turned into with mudanças em sorocaba # throughout my recent relocation!
The combination of stylish clothes and a fashionable messenger bag can truly elevate your everyday appearance. More ideas at durable men’s messenger bag options .
I’m glad I found a reliable water damage restoration service in Irving TX when my basement flooded last year! restoration companies in my area
I highly recommend creating an emergency kit for situations where unexpected flooding might occur—it could save lives!! #Preparedness### anykeyword ### water damage restoration service near me
Well done! Find more at Gas safety checks .
Thanks for shedding light on who to contact when my AC isn’t working—it’s so important to know where to turn, especially places like ac repair Las Cruces NM! air conditioning repair Las Cruces
Appreciate the detailed post. Find more at affordable blocked toilet repair .
The craftsmanship of Gibson guitars is incredible, especially the Les Paul series. Find out more at Les Paul Slash Signature .
Nicely detailed. Discover more at ادمین اینستاگرام .
Thanks for the great content. More at natural pest control solutions Long Valley .
Moving should be would becould very well be anxious, however with the suitable professional products and services like empresa de mudanças , it is able to be a breeze. They sincerely be aware of what they may be doing!
Thanks for the thorough article. Find more at HVAC contractor .
Just wanted to share that the quick service from ###made all the difference during our family’s recent crisis—thank you guys! water and mold restoration near me
This piece is exceptional! Honestly, my model wouldn’t have accomplished justice to the subject. auto glass repair charlotte
It’s crucial to act fast when it comes to water damage. If you’re in Irving, TX, check out the services offered by water and mold restoration near me .
I feel fortunate discovering this place so close-by since there aren’t many places offering similar values nearby!!! appliance store Vancouver
If you’re a homeowner in Escondido, don’t overlook the valuable resources available at jcis roofing escondido .
Got some great tips from my local ### anykeyword ### about maintaining my roof through seasons. roofer near me
I visited various web sites however the audio quality for audio songs present at this web page is truly fabulous. https://www.jack-wolfskin.fr/login/?returnUrl=http%3A%2F%2Fdtyzwmw.com%2Fcomment%2Fhtml%2F%3F95361.html
I visited various web sites however the audio quality for audio
songs present at this web page is truly fabulous. https://www.jack-wolfskin.fr/login/?returnUrl=http%3A%2F%2Fdtyzwmw.com%2Fcomment%2Fhtml%2F%3F95361.html
I love how convenient it is to find a dentist in Newnan. The reviews really help! dentist 30265
Thanks for the valuable insights. More at apartamentos turísticos .
I liked this article. For additional info, visit construction administration services .
Love how you’ve captured demographic shifts’ impact throughout various campaigns—knowing our audience shapes strategy significantly; check demographic research tools available over ###anKeyWord## blackhat marketing blog
This was very enlightening. For more, visit casas rurales .
Just moved with help from Local movers Rockledge ; they were professional and efficient throughout the process!
Appreciate the detailed post. Find more at ماساژ ماهور .
This was highly educational. For more, visit ادمین اینستاگرام .
I found this very helpful. For additional info, visit reliable shower installation services .
Thanks for the practical tips. More at Dental Group Beverly Hills .
This was a fantastic resource. Check out AC installation for more.
Thanks for the detailed post. Find more at Effective pest management Hackettstown .
This was a fantastic resource. Check out Plumbing & heating for more.
Appreciate the helpful advice. For more, visit local reliable plumbing .
This was quite informative. More at drain plumbers near me .
Thanks for the great explanation. Find more at ادمین اینستاگرام .
It’s always great to find reliable movers—thank you # Mulberry Mover’s # for being so dependable!
This was a fantastic read. Check out Affordable Pest Solutions for more.
For those searching into specialist shifting possibilities: truely investigate out # any key-word # – you won’t be disappointed! mudança em sorocaba
Valuable information! Find more at affordable plumbing costs .
This was nicely structured. Discover more at Affordable Pest Solutions .
Moving may be daunting, yet with mudanças em sorocaba , one could leisure certain all the pieces will probably be treated professionally!
Great tips! For more, visit mobile auto glass charlotte nc .
Valuable information! Find more at https://send.now/fz8t5h9agtim .
Thanks for the great tips. Discover more at https://www.mediafire.com/file/hkptrbohs02ueox/pdf-90138-50996.pdf/file .
Anyone else curious about the advantage of Felysyum Token? It appears like it might essentially make an influence in the crypto house through 2025! Find more insights in this at best blockchain projects 2025 .
Clearly presented. Discover more at ماساژ ماهور .
I enjoyed this read. For more, visit apartamentos turísticos Arzúa .
This is quite enlightening. Check out LuxNuro for more.
For all of us in Sorocaba thinking a move, I can vouch for the excellent expertise presented by means of empresa de mudanças .
Excellent information on Essex roofing For both fixes and new installations, it’s crucial to find trustworthy builders. Being able to protect homeowners from costly damages from the unexpected temperature can be achieved by having a strong roof roofers essex
Thanks for the insightful write-up. More like this at casa rural en Arzúa .
Great work! This is the kind of information that should be shared around the internet.
Disgrace on Google for no longer positioning this post upper!
Come on over and consult with my web site . Thank you
=)
The versatility of the Gibson Les Paul’s sound makes it suitable for studio recordings across genres; what have you recorded with yours? Join discussions over at Gibson Les Paul Custom !
Great tips! For more, visit ادمین اینستاگرام .
Searching for local remodeling contractors you can trust? Our design-build process makes renovations seamless.
Sumner Home Remodel
Helpful suggestions! For more, visit personal injury attorney near me free consultation .
Thanks for the detailed post. Find more at Beverly Hills Dental Group .
This was nicely structured. Discover more at ادمین اینستاگرام .
Thanks for your marvelous posting! I quite enjoyed reading it,
you could be a great author.I will make certain to bookmark your blog and may come back at
some point. I want to encourage one to continue your great writing,
have a nice evening!
I appreciated this article. For more, visit charlotte nc auto glass replacement .
Choose Ocala full service movers for your next move in Ocala; you won’t regret it!
Appreciate the detailed post. Find more at Budd Lake bug removal services .
I learned so much about roofing from my Escondido contractor. Thanks, roofer escondido !
Sanderson apartment movers are the best! Fast, friendly, and efficient. More moving resources at Local movers Sanderson .
What a fantastic article on link building strategies! Looking forward to checking out what’s available at Buy backlinks for niche sites and blogs !
Couldn’t have done it without fantastic help from local experts featured on ##anyKeyword#! Moving made easy! Lawtey moving companies
“Can someone provide insight on what features or aspects one should prioritize when working closely alongside experts?” roofers in San Diego
Thanks for the thorough analysis. Find more at Affordible Pest Solutions .
I found this very interesting. Check out expert water leak repair for more.
Fantastic team work led us through—big thumbs up towards achieving goals together: big thank-you goes out towards…#Anykeyword# Hialeah full service movers
Hello! I could have sworn I’ve visited this website before but after going through many of the posts I realized it’s new
to me. Regardless, I’m certainly delighted I stumbled upon it and I’ll be book-marking it and checking back often! http://Anunciomex.com/languages/lavage-de-automobile-pourquoi-et-conseils-sur-comment-prendre-soin-l-apparence-hors-de-votre-vehicule.html
”Looking forward to seeing how energy-efficient models evolve further!” # # anyKeyWord ## AC installation Walburg
I found this very interesting. Check out power washing service company for more.
Wow, these exterior painting ideas are inspiring! I’m ready to update my own home! professional painters near me
I enjoyed this read. For more, visit ماساژ ماهور .
I had a great experience with Silver Springs commercial movers. Their professionalism was top-notch! Learn more at Silver Springs international movers .
I recently had a water issue, and the team from water damage restoration service near me was amazing! Highly recommend their services!
This was a great help. Check out car locksmith for more.
I could talk about the Les Paul for hours! What makes it special for you? Join the discussion at Gibson Les Paul Studio .
Nicely detailed. Discover more at lock smith .
Certainly eye-opening reading firsthand accounts from others who’ve faced similar challenges before–definitely inspires confidence knowing help exists locally too!! water and mold restoration near me
Great job! Discover more at ادمین اینستاگرام .
Just scored an amazing oven from the discount section of appliance store Burnaby —so happy with it!
Love seeing local businesses unite to tackle issues like water damage—Irving TX really cares about its residents! water damage restoration service near me
Looking forward eagerly towards upcoming conferences discussing innovative approaches related directly toward flood mitigation techniques…learning continuously enriches our understanding immensely!!!!#ConferencesMatter ### anykeyword ## water damage restoration companies near me
I appreciated this post. Check out locksmith services winston-salem nc for more.
Excellent article on the importance of keeping your roof looking good! It is important to have a trusted cladding organization in Essex, where weather may be unstable Roof repair Essex
Great tips! For more, visit Heating equipment supplier .
I appreciate these tips on maintaining good home health! Remember that timely intervention from ###can save significant costs down the line! water damage restoration service near me
I enjoyed this article. Check out Brain Mapping Clinic Denver for more.
Your article is so helpful! I’m definitely going to explore the services offered by Buy backlinks for SEO for my SEO strategy.
Just had a wonderful experience with the team at water damage restoration service near me after a storm caused some flooding at my home in Irving.
Appreciate the great suggestions. For more, visit apartamentos turísticos .
Thanks for the detailed guidance. More at ماساژ ماهور .
Kudos to mudança em sorocaba for making my movement rigidity-free! If you might be in Sorocaba SP, cost them out.
This was a great article. Check out auto glass shop charlotte nc for more.
Great insights! Discover more at casas rurales .
How do you find the best dental insurance that covers services from dentists in Newnan? affordable dentist newnan ga
Appreciate the thorough information. For more, visit Beverly Hills Dental Group .
.We’ll definitely be recommending # # any Keyword ###to anyone needing help with their upcoming moves Best Addison movers
If you need help moving in Yalaha, seriously consider reaching out to %%ANYKEYWORD%%—they’re fantastic! Best Yalaha movers
This was very enlightening. More at gas engineers near me .
Check out this link https://john-bet.com
Cheap doesn’t mean low quality! Check out the services at Margate moving company .
This is highly informative. Check out Pest Services Budd Lake for more.
**Affordable Pricing**: Their pricing is competitive and transparent, with no hidden fees. Bounce Genie Pinellas offers great value for the quality of service and products provided, making it an excellent choice for budget-conscious planners. seminole bounce house
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
Thanks for the detailed post. Find more at Shower installation .
This was a great help. Check out https://pin.it/70LMyK9Dc for more.
Thanks for the detailed post. Find more at Affordible Pest Solutions .
Moving may also be traumatic, but with the true knowledgeable facilities like empresa de mudanças , it could be a breeze. They tremendously understand what they are doing!
The movers from this Hilliard moving company were prompt, efficient, and very friendly – highly recommend them! See more at Office moving companies Fort Liberty !
Really understand how nicely-rounded & informative your mind-set has been throughout the time of each phase mentioned!!! ### anykeyword### Security Camera Installation
The updates on Bitchat download keep getting better—loving the new features they add regularly! install Bitchat Apk
Thanks for the great tips. Discover more at charlotte auto glass .
Planning ahead really pays off; thanks again # any Keyword# for making everything easier!! Long distance movers Clearwater
Your points about content marketing are spot on! Quality content is key to engagement. Learn more at Rehan Hasan !
Hi there I am so delighted I found your blog, I really found you by error,
while I was looking on Bing for something else, Anyways I am here now and would just like to say kudos for a incredible post and a all round enjoyable blog (I also love the theme/design), I
don’t have time to browse it all at the minute but I
have bookmarked it and also added your RSS feeds,
so when I have time I will be back to read a lot more, Please do keep up the superb job. https://Sun-Clinic.Co.il/he/question/reworking-your-out-of-doors-spaces-with-year-round-landscaping-companies/
Hi there I am so delighted I found your blog, I really found you by error,
while I was looking on Bing for something else, Anyways I am here now and would just like to say kudos
for a incredible post and a all round enjoyable blog (I
also love the theme/design), I don’t have time to browse it all at the
minute but I have bookmarked it and also added your RSS feeds, so when I have time I will be back to read a lot more, Please do keep up the superb job. https://Sun-Clinic.Co.il/he/question/reworking-your-out-of-doors-spaces-with-year-round-landscaping-companies/
Thanks for the informative content. More at ferretería en Albacete .
I couldn’t have asked for better movers than those from Hialeah FL Mover’s # during my transition to Hialeah.
If you’re moving in or out of Palm Harbor, consider using Ozona Mover’s for your needs.
Thanks for the insightful write-up. More like this at Denver advanced brain mapping services .
I liked this article. For additional info, visit Arzúa .
düğmelerden sadece tıklayın her biri Bigger Bass Bonanza bizim/elimizde ana sayfamızda,
için görmek/görmek mevcut bugün/şimdi/şimdi teklifler.
Inspired by discussions about crisis prevention measures implemented proactively — anticipating challenges reduces negative fallout considerably experienced otherwise if unplanned ; read crisis prevention methods outlined here: ###anKeyWord ## marketing blog
Moving is so much easier when you have professionals on your side—thanks, Melrose commercial movers !
Appreciate the detailed information. For more, visit Plumbers .
This is highly informative. Check out Dental Group of Beverly Hills for more.
Appreciate the thorough information. For more, visit ادمین اینستاگرام .
Ever tried a custom shop Les Paul? The details are astonishing! Explore custom options at Les Paul 490R 498T Pickups .
Just bought new ##kitchen appliances## and couldn’t be happier with my choices! appliance store Vancouver
I’m always amazed by the before-and-after photos of Austin homes! Check out ours: Bathroom Remodeling Austin .
Planning a basement remodel? Get helpful tips from our experts at Kitchen Remodeling !
Have you thought about incorporating sustainable landscaping into your remodel? More ideas here: Home Remodeling !
Bathroom spa retreats are all the rage—find out how to create one at Home Remodeling in Austin Texas .
After speaking with multiple experts, I’m convinced that finding the right ### anyKeywords### is crucial! atlas roofers
What are the most common mistakes made during remodeling? Find out here: Remodeler Near Me !
Austin’s unique style really shines through in home remodels. Learn more about our services at Remodeling Austin .
Are you considering an open floor plan? Discover why it’s popular among Austin homeowners at Bathroom Remodeling .
Hey! This is my 1st comment here so I just wanted to give a quick shout out and say I truly enjoy reading through
your posts. Can you recommend any other blogs/websites/forums that go over
the same subjects? Thank you so much!
If anyone is facing water damage in Ellenwood, I suggest contacting water damage restoration companies near me . They did a fantastic job for us.
Just completed a roofing project! So glad I consulted jcis roofing escondido before making decisions.
Regular HVAC maintenance can extend the life of your system—definitely worth considering! Air conditioning repair service
Roofing can be daunting, but good advice makes working with # San Diego County Roofing
This was very enlightening. More at Flanders emergency pest management .
Shoutout to mudança em sorocaba for his or her terrific carrier all through my current transfer! Highly commended!
I appreciated this article. For more, visit foothills paving and maintenance .
Well done! Find more at local personal injury lawyer .
I never realized how important quick action is after water damage until it happened to me! Thankful for Irving TX restorers! flood restoration companies near me
This was quite informative. More at reliable plumbing specialists .
Wondering if anyone else has tried DIY drying methods after minor leaks? Would love some input on what’s worked best!!!#DIYTips### anykeyword ## flood restoration companies near me
I unquestionably realise the hard work from the staff at mudanças em sorocaba # right through my current flow—thank you!
The team from Greenacres Mover’s arrived on time and ready to work — very impressive indeed! Greenacres Mover’s
This was very enlightening. More at ماساژ ماهور .
Excellent information on Essex’s roof sector! With the erratic conditions we experience, it’s crucial to find trustworthy roofers roofing contractors essex
Thanks for the valuable article. More at https://list.ly/i/11119367 .
Proper ventilation is key after any flooding—great tips here! Don’t forget that experts at restoration companies in my area can assist too!
Appreciate the detailed insights. For more, visit 24 hr plumber .
I recently had a water emergency at my home in Irving, and I found the best help at water damage restoration service near me . Highly recommend their services!
I’m thinking about whitening my teeth; any recommendations for dentists in Newnan who offer this service? dentist 30265
If you’re making plans a pass, take into account to touch empresa de mudanças —they may be distinctive at what they do in Sorocaba SP!
I appreciated this post. Check out ادمین اینستاگرام for more.
What’s your favorite home remodeling trend in Austin? Share and explore more at Bathroom Remodeling Austin !
Great insights! Discover more at Air conditioning system supplier .
Nicely detailed. Discover more at charlotte nc auto glass replacement .
This was quite helpful. For more, visit ادمین اینستاگرام .
I love how each year brings new Limited Edition Gibson Les Paul’s; they are always so unique! Which ones have caught your eye? Join discussions over at Les Paul 60s !
I appreciated this post. Check out commercial plumbing for more.
Thanks for the helpful advice. Discover more at local plumber near me .
Thanks for the great explanation. More info at drain cleaning plumber .
Moving can be such a hassle, but having the right team makes all the difference—especially here in Dundee! Dundee commercial movers
This was very well put together. Discover more at LuxNeuro .
Fantastic information—everyone should prioritize dryer vent cleaning with experts like Dryer Air Duct Cleaning !
Very informative article. For similar content, visit Foot Hills Paving .
Wonderful article! We are linking to this great article on our site.
Keep up the good writing. https://wp.teamlead.pw/question/conseils-par-des-soins-du-visage-efficaces-prenez-soin-hors-de-votre-peau-au-quotidien/
This was very enlightening. For more, visit emergency my plumber .
Appreciate the comprehensive advice. For more, visit Dental Group Beverly Hills .
I found this very helpful. For additional info, visit auto glass shop charlotte nc .
This was a fantastic read. Check out TheWinnslow for more.
This was beautifully organized. Discover more at ماساژ ماهور .
Found a great deal on shingle replacements thanks to listings from # roofer in san diego #—couldn’t believe my luck!
Thanks for the detailed guidance. More at ادمین اینستاگرام .
I found this very interesting. For more, visit Affordible Pest Solutions .
Thankful everyday we decided hire professionals instead of trying DIY approach again — connect with trustworthy brands through this resource page: @@anything@@ Midland international movers
Lighting fixtures can make or break a room—choose wisely! Find tips on selection here: Kitchen Remodeling .
Bathroom spa retreats are all the rage—find out how to create one at Bathroom Remodeling Austin .
If you’re in Austin and planning a remodel, check out our expert tips at Home Remodeling !
I’ve heard so many good things about jcis roofing escondido from friends in Escondido; they must be doing something right!
Don’t underestimate the power of good lighting in remodeling—explore ideas here: Bathroom Remodeling .
I love the blend of modern and traditional in Austin homes! Get inspired at Remodeling Austin .
Appreciate the comprehensive advice. For more, visit 24/7 pest control Flanders .
This was a great help. Check out ادمین اینستاگرام for more.
My neighbor just hired a roofers in San Diego and their roof looks fantastic now! Time to get mine checked.
Howdy I am so excited I found your blog page, I really found you by error, while I
was browsing on Google for something else, Anyways I am here
now and would just like to say thank you for a remarkable
post and a all round exciting blog (I also love the theme/design),
I don’t have time to read it all at the moment but
I have bookmarked it and also added your RSS
feeds, so when I have time I will be back to read much more,
Please do keep up the awesome work. https://Anunciosclassificados.org/author/marlonboren/
Excellent information on Essex roofer providers! With the erratic conditions in the area, it’s crucial to find trustworthy contractors. Which roofing firm is the most reliable may mean everything, whether it’s rooftop repair or flat roofing installation essex roofing services
Howdy I am so excited I found your blog page, I really found you by error, while I was browsing on Google for something else,
Anyways I am here now and would just like to say thank you for a remarkable post and
a all round exciting blog (I also love the
theme/design), I don’t have time to read it all at the moment but
I have bookmarked it and also added your RSS feeds, so when I have time I will be back to read much more, Please do keep up
the awesome work. https://Anunciosclassificados.org/author/marlonboren/
Well done! Discover more at supportive Farsi therapy counselor .
I’m truly enjoying the design and layout of your site. It’s a very easy on the eyes which makes it much more pleasant for me to come here and visit more often. Did you
hire out a developer to create your theme? Exceptional work!
Need help planning your renovation? Our resources can guide you: Kitchen Remodeling Austin .
Appreciate the comprehensive advice. For more, visit LuxNuro .
Wonderful tips! Discover more at ferretería Albacete .
Can’t recommend enough that people see a ###Mississauga Periodontist### if they have concerns about their gums. dental implants periodontist
Thanks for the informative post. More at ماساژ ماهور .
Great details approximately indoor vs outdoors cameras—I by no means knew there had been so many causes to keep in mind! Sanford Security Camera Installation
Wonderful tips! Discover more at Dental Group Beverly Hills .
Have you ever upgraded components on your Les Paul? It’s amazing what difference it can make! Talk upgrades at Les Paul Modern .
Looking for an appliance store nearby? Look no further than discount appliance store for great deals!
I enjoyed this read. For more, visit TheWinslow .
This was quite informative. More at ادمین اینستاگرام .
For these having a look into official shifting recommendations: no doubt check out # any key-word # – you received’t be disillusioned! mudança em sorocaba
This was a great help. Check out Affordable Pest Solutions for more.
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
The customer service from mudanças em sorocaba was once useful for the duration of my latest go—thank you!
Great job! Discover more at Affordible Pest Solutions .
This was very well put together. Discover more at expert commercial driveway paving .
Thanks for the valuable insights. More at cheap windshield replacement charlotte .
Nicely detailed. Discover more at locksmith raleigh nc .
The evaluations are properly! I hired empresa de mudanças # for my last transfer, and so they delivered super service.
I think the admin of this site is genuinely working hard in support of his web site, since
here every material is quality based data.
Thanks for the helpful article. More like this at trusted kitchen plumbing .
I’ve tried various backlink services, but the ones at Backlink seller are top-notch. Highly recommend them!
Appreciate the thorough analysis. For more, visit ماساژ ماهور .
Nothing compares to the feeling of strumming a Gibson Les Paul live on stage! Do you agree? Share your experiences at Les Paul Handwired Electronics .
Thanks for the thorough analysis. Find more at cheap windshield replacement charlotte .
This was very beneficial. For more, visit ادمین اینستاگرام .
Found an amazing pediatric dentist here in Newnan that my kids absolutely love! dentist 30265
Very helpful read. For similar content, visit locksmith services winston-salem nc .
“As someone who works in marketing, I’m always analyzing successful influencer strategies; there’s so much we can learn!” ## influencer
Thanks for the great explanation. Find more at Leaking dishwashers .
Appreciate the helpful advice. For more, visit brain mapping diagnostic analysis Denver .
Thanks for the helpful article. More like this at Wheat Ridge Driveway Paving .
I love seeing colorful accents in remodeled spaces! Get inspired by our projects at: Kitchen Remodeling Austin
You’ve come to the right place if you’re looking for trustworthy and knowledgeable contractors in Essex. Particularly with the uncertain weather we frequently experience, maintaining the integrity of your ceiling is important roofing company essex
This was a wonderful post. Check out Sewer line repair company for more.
Appreciate the detailed information. For more, visit ماساژ ماهور .
7. вы прошли регистрацию, kraken зеркало тор com теперь вот
должно появиться окно с профилем.
Терминал для работы в доступности в режиме kraken pro.
For somebody in Sorocaba pondering a move, I can vouch for the fabulous functions provided by mudança em sorocaba .
This was quite informative. For more, visit basement water damage .
Great post! The benefits of dryer vent cleaning are undeniable. I trust Dry Vent Cleaning with all my vent maintenance needs.
Love the insights in this post! For anyone looking to buy backlinks, I suggest visiting Buy SEO backlinks for reliable options.
Thanks for the clear advice. More at NYC bar private dining room .
My recent experience with a local atlas roofing was fantastic; they were prompt and efficient.
Clearly presented. Discover more at Afordable Pest Solutions .
This is very insightful. Check out emergency plumbing services near me for more.
If you are purchasing for dependableremember mudanças em sorocaba in Sorocaba SP, I tremendously propose checking out their expertise for a soft moving trip!
I love exploring new cryptocurrencies, and Felysyum Token is truthfully one who stands out! Could it be among the most productive appearing cryptocurrencies in 2025? Let’s find out mutually at Felysyum Token market !
The customer service at JCIS Roofers is top-notch; they really care about their clients.
This was quite informative. More at Sewer line repair near me .
Nicely done! Find more at ادمین اینستاگرام .
Thanks for the great explanation. Find more at ادمین اینستاگرام .
. Recently explored multiple avenues available through local professionals aiding others within my network wanting assistance relocating successfully too!!! # # # # # # # # # Local movers Dundee
This was a fantastic read. Check out Affordable Pest Solutions for more.
Home remodeling in Austin should reflect personal taste—find ways to do that on our site: Home Remodeling in Austin Texas
Maximizing small spaces is an art form! Discover tips for efficient design on our site: Remodeling Austin .
Smart home technology can enhance your remodel—discover how at Bathroom Remodeling !
“Had such a good experience with my last ###RooferInSanDiego###; they were thorough and respectful.” SD Roofing & Solar
What are the most common mistakes made during remodeling? Find out here: Remodeler Near Me !
This was very enlightening. More at same day plumber .
I found this very interesting. For more, visit https://www.hometalk.com/member/178917427/george1256968 .
Every visit to my local #Periodontal services# provider has been enlightening and beneficial!”, dentist
Appreciate the detailed post. Find more at support from Persian language therapists .
Content curation strategies can complement original content creation beautifully ; great insight here ! Learn how to curate effectively from ### anyKeyWord### . Rehan Hasan
Moving does not need to be irritating—simply employ empresa de mudanças # and enjoy a modern transition!
This was very enlightening. For more, visit Affordable Pest Solutions .
Appreciate the comprehensive advice. For more, visit Afordable Pest Solutions .
I love seeing colorful accents in remodeled spaces! Get inspired by our projects at: Home Remodeling
Thinking of adding a second story? It’s a great way to gain space—learn more here: Remodeler Near Me !
What’s your favorite home remodeling trend in Austin? Share and explore more at Bathroom Remodeling Austin !
Thanks for the useful post. More like this at pioneering brain mapping methods in Denver .
Wonderful tips! Discover more at animal hospital Jacksonville .
Can’t wait share testimonials recounting experiences encountered while working skilled professionals dedicated providing exceptional quality service delivered consistently achieving results exceeding expectations while ensuring satisfaction maintained Local movers Glendale
I was impressed by the cleanliness and quality of the rentals at tampa bounce house —great service too!
Appreciate the thorough analysis. For more, visit veterinarian Greensburg .
Thanks for the thorough article. Find more at indoor air quality testing nearby .
Thanks for the detailed guidance. More at Dental Group of Beverly Hills .
Great insights and clarity to your writing! I’d fight to convey such innovations comfortably myself! charlotte windshield installation
Thanks for the useful post. More like this at TheWinslow .
Wonderful tips! Find more at ماساژ ماهور .
Valuable information! Find more at expert manhole repairs .
I had a fantastic experience with a buy here pay here dealer in Phoenix. Highly recommend checking out buy here pay here phoenix $500 down for deals!
I found this very helpful. For additional info, visit Affordible Pest Solutions .
Does anyone else have a ‘dream’ version of their perfect Gibson Les Paul in mind that they wish existed? Let’s brainstorm ideas together over at Les Paul Rosewood Fretboard
The step-by means of-step guidelines on developing a drone camera have been clear and smooth to observe; it made getting began less intimidating for freshmen like myself—thanks returned, and take a look at out what else they have over at https://wiki-spirit.win/index.php/**From_Ground_to_Air:_How_to_Get_Started_with_Your_New_Drone_Camera** !
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
I recently had some ceiling work done, and I can’t emphasize enough how important it is to find a trustworthy roofer, mainly in Essex. It’s important to keep your roof in leading shape because the weather can be uncertain and can be unexpected roofing companies essex
This was a fantastic resource. Check out Brooks & Baez for more.
Right here is the right blog for everyone who hopes to find out
about this topic. You understand a whole lot its almost hard to
argue with you (not that I personally would want to…HaHa).
You certainly put a new spin on a subject that’s been discussed for years.
Great stuff, just excellent!
Buenas, Pablito! ¿Cómo estás? Tengo una excelente recomendación para ti un plataforma de apuestas online
que no puedes dejar de probar. Este casino tiene una variedad impresionante de juegos y una navegación muy fluida.
Si prefieres las slots, te sorprenderán con los juegos
de slots variados. También, el casino tiene todos los juegos de mesa que puedes
imaginar.
Lo mejor de este casino online es que tienen opciones de pago
locales. Sabemos que en nuestra región, es muy importante que los métodos de pago sean fáciles de usar y seguros, y este casino tiene opciones de pago muy convenientes.
Por si fuera poco, tienen bonos increíbles para jugadores nuevos.
Cuando te registres,, recibirás un bono de bienvenida que te permitirá aumentar
tus posibilidades de ganar. Además, tienen ofertas continuas.
La web también cuenta con atención al cliente de primera, para resolver cualquier inconveniente.
La atención es de calidad y te guiarán en todo momento.
En cuanto a la seguridad, el portal utiliza encriptación de última generación para proteger tus datos.
Puedes jugar tranquilo.
Si decides probar esta plataforma, te aseguro que no te arrepentirás.
¡Tienes mucho que ganar! Además, siempre podrás disfrutar de
una experiencia de juego sin igual. Te vas a divertir muchísimo.
Mi sugerencia es que pruebes este casino y disfrutes de todo lo que tiene para ofrecerte.
No dudes, Pablito, te garantizo que disfrutarás mucho.
¡Suerte y que empiecen las ganancias!
Thanks for the great tips. Discover more at Foothills Paving .
Has anyone tried laser dentistry at their local practice here in Newnan? I’m curious about the benefits! ##anyKeyword ## dentist 30265
What’s up, I read your blogs daily. Your writing style is awesome,
keep doing what you’re doing! http://WWW.Foot-Palmares.com/comment/html/?86635.html
Well done! Find more at charlotte auto glass .
Thanks for the helpful article. More like this at professional sink fitting .
Thanks for the useful suggestions. Discover more at Family Law Attorney Richmond VA .
This was a wonderful post. Check out http://help.crimeastar.net/index.php?url=https://qa.andytoan.vn?qa=user&qa_1=voadilpyqy for more.
Hello mates, how is the whole thing, and what you wish
for to say about this paragraph, in my view its genuinely amazing in favor of me.
This was highly educational. For more, visit ماساژ ماهور .
Super impressed with the quality of work from my chosen Escondido roofer via jcis roofing .
Wow! After all I got a website from where I know how to in fact take helpful facts regarding my study and
knowledge.
Planning a basement remodel? Get helpful tips from our experts at Home Remodeling in Austin Texas !
Do you need help deciding between tile or hardwood flooring? Get advice from our experts: Remodeling Austin
Appreciate the useful tips. For more, visit ادمین اینستاگرام .
“The aesthetic of my home improved dramatically after working with a great ###RooferInSanDiego###.” roofers near me
The kitchen is the heart of the home! Find out how to remodel yours at Kitchen Remodeling .
This was very beneficial. For more, visit ادمین اینستاگرام .
Do you need help deciding between tile or hardwood flooring? Get advice from our experts: Bathroom Remodeling
Great breakdown of referral programs and their effectiveness—I think they’re underutilized by many brands; get additional referral program tips over ###anKeyWord## blackhat marketing blog
Thinking about a bathroom remodel? We have some great insights at Remodeler Near Me !
I love that you’ve included steps on how to emergency release a garage door—so necessary! Great resource, will use emergency garage door repair Los Angeles if needed. emergency garage door repair Los Angeles
Home remodeling in Austin is a great way to increase your property’s value! Check out some tips on our site: Home Remodeling .
Just received settled in my new region attributable to mudança em sorocaba ! If you need relocating facilities in Sorocaba, indubitably give them a call.
Appreciate the useful tips. For more, visit LuxeNeuro .
Great job! Discover more at https://send.now/99bpsm047na2 .
Well done! Discover more at residential driveway asphalt paving .
Has all people else used mudanças em sorocaba for moving in Sorocaba? I had a impressive revel in and would love to listen greater experiences!
Remodeling can be a great investment—learn more about it at Kitchen Remodeling Austin !
Search engine algorithms are always changing; staying updated is essential! Learn more strategies at Rehan Hasan !
This is highly informative. Check out Dental Group Beverly Hills for more.
This was quite informative. More at intimate secluded bars NYC .
This was quite enlightening. Check out local emergency plumbing services for more.
Just visited an appliance liquidation event and found some amazing products at appliance store nearby .
I found this very helpful. For additional info, visit local plumbers .
Shoutout to Long distance movers Fort Liberty for making my move to Hilliard so smooth and hassle-free!
Thanks for the thorough analysis. Find more at Affordible Pest Solutions .
I recently visited a ##Mississauga Periodontist## for gum grafts, and the experience was fantastic! Highly recommend their services. dental clinic
I recently moved across the country with long distance movers in Sanderson, and it was a breeze! Don’t forget to visit Sanderson full service movers for more information on moving.
Has absolutely everyone used empresa de mudanças for administrative center relocations? I’m looking for a respectable carrier in Sorocaba.
If you’re moving soon, check out the offers from Cheap movers Jacksonville #; they’re unbeatable!
All set now thanks entirely due diligence applied while securing engagement terms relating specifically towards forthcoming commitments involving ongoing negotiations led forthwith amongst those situated firmly along pathways traversed collectively Lawtey full service movers
Have you ever taken a road trip along with your puppy? It will be such an adventure! Get tour assistance for pets on https://bbarlock.com/index.php/Exploring_the_Different_Types_of_Dog_Collars_and_Harnesses .
It’s amazing how much of a difference quality backlinks can make. I’m considering using Affordable backlinks for my link-building needs.
Using a pressure washing machine between 2000 and 3000 PSI is applicable for deep cleaning decks with out causing injury. Check out my prominent thoughts at https://www.protopage.com/annilayfbw#Bookmarks !
Great experience overall purchasing through a nearby dealer; they truly care about helping customers—explore options on buy here pay here phoenix az no credit check !
This was a wonderful guide. Check out ماساژ ماهور for more.
Appreciate the thorough insights. For more, visit mobile auto glass charlotte nc .
If you’re in Waco and need help with an office move, definitely check out what’s available at Office moving companies Waco .
Great job! Find more at Farsi Therapist Near Me .
This was quite enlightening. Check out Pest Control Long Valley for more.
This was a great help. Check out ادمین اینستاگرام for more.
I’m genuinely desirous about the long run of crypto! Felysyum Token appears to be like gaining traction and might possibly be probably the most first-class appearing cryptocurrencies in 2025 top cryptocurrencies to invest
Thanks for the valuable article. More at ferretería Albacete .
Appreciate the great suggestions. For more, visit Denver brain mapping service clinic .
Thanks for the helpful advice. Discover more at ادمین اینستاگرام .
Hi! I just wanted to ask if you ever have any issues with
hackers? My last blog (wordpress) was hacked and I ended up losing
months of hard work due to no back up. Do you have any
solutions to prevent hackers? http://m.Shopinlosangeles.net/redirect.aspx?url=http://articomed.com/node/289302
Hi! I just wanted to ask if you ever have any issues with hackers?
My last blog (wordpress) was hacked and I ended up losing months of
hard work due to no back up. Do you have any solutions to prevent
hackers? http://m.Shopinlosangeles.net/redirect.aspx?url=http://articomed.com/node/289302
Excellent article! Finding trustworthy## Roofers in Essex## can be difficult, but it’s essential to uphold the dignity of our houses. I’ve had a great experience with a local company that specializes in# #flat Roofing Essex## roofers essex
Considering gum grafts? Don’t hesitate! Reach out to an experienced dentist today!”, dental implants Mississauga
Valuable information! Find more at after hours oral care Beverly Hills .
Fantastic post! Discover more at TheWinslow .
Do you think it’s worth it to hire packing services from a Glendale moving company? What do you think? United Mover’s Glendale
Great insights! Find more at Affordible Pest Solutions .
Great tips! For more, visit auto glass repair charlotte .
This was highly educational. For more, visit plumbing and heating near me .
Just moved throughout town employing mudança em sorocaba # and couldn’t have asked for more beneficial service!
Are there specific types of influencers that you follow? I love those who focus on wellness and lifestyle content! influencer
Has an individual attempted mudanças em sorocaba for moving services and products in Sorocaba? I’m curious approximately their pricing and customer service.
Great insights! Find more at ادمین اینستاگرام .
This was a great article. Check out Rodent Control Hackettstown for more.
Helpful suggestions! For more, visit Foot Hills Paving .
Thanks for the helpful article. More like this at ادمین اینستاگرام .
Thanks for the useful suggestions. Discover more at commercial pest management Long Valley .
Thanks for the insightful write-up. More like this at affordable plumbing and heating services .
Nicely detailed. Discover more at reliable plumbers in my area .
Appreciate the thorough write-up. Find more at rent a car toronto .
Great job! Discover more at ferreterías Albacete .
Love the blend of indoor and outdoor living spaces in Austin homes? More ideas here: Kitchen Remodeling Austin .
Local stores like this one have so much more character than big chains—check them out like I did with appliance store near me .
Just desired to proportion my confident knowledge with empresa de mudanças ! Highly advocate for any relocating necessities.
Just got some great advice from my ### anyKeywords### about roof ventilation – very helpful! atlas roofers
Love the fantastic posts!
Does anyone have tips for moving in Brooklyn? I found Long distance movers Brooklyn and they seem great!
The best decision I made was hiring an Escondido roofer through roofer near me .
Thanks for sharing these tips! I’ve successfully used High DA backlinks for sale to buy backlinks that improved my rankings!
Great insights! Find more at quick appliance repair .
Curious about latest trends surrounding sustainable practices within residential sectors? Let’s keep an eye open towards innovative ideas highlighted within %%ANYY_KEY%!!! felton plumbers
Appreciate the great suggestions. For more, visit Serenity Psychotherapy Group .
Appreciate the comprehensive advice. For more, visit ادمین اینستاگرام .
I’ve saved so much time reaching out based off recommendations shared through this platform—thankful for finding ### anykeyword###!! roofers
Anyone here very own a Shih Tzu or comparable toy breed? How are they as companions? https://go.bubbl.us/ec0107/a976?/Bookmarks
What an unforgettable experience horse riding along the coast of Jacó – highly recommend this service available at horseback riding near Jaco !
Excellent article! Finding trustworthy contractors in Essex can be difficult, particularly with the ominous climate we experience. Whether it’s through repairs or a complete substitution, keeping your roof in top shape is vital roofing company essex
”Undoubtedly will remain loyal advocates promoting superb level customer satisfaction received along journey towards brighter future ahead!” Jacksonville commercial movers
Thanks for sharing this info about relocating—we just did ours via suggestions from #anyKeyword#. Office moving companies Waco
Well done! Find more at Beverly Hills Dental Group .
Thanks for the helpful advice. Discover more at Foot Hills Paving .
As we appear against 2025, I’m curious approximately which crypto initiatives will stand out. Felysyum Token has been making waves currently. If you might be inquisitive about researching more about promising cryptocurrencies, check out Felysyum Token updates .
Anyone else excited about attending guitar festivals featuring legendary players showcasing their Gibson’s?! Who are you hoping to see?! Let us know at Les Paul Finish Options
#Periodontal services#: essential maintenance for healthy gums—don’t wait any longer to get checked out! periodontist Mississauga
This was very enlightening. For more, visit mobile auto glass charlotte nc .
Thanks for the clear advice. More at intimate speakeasy settings NYC .
Love that you awarded actionable steps that every person can take with no need specialized understanding!!! ##anythingKeywords## Visit this link
Thanks for the valuable article. More at Affordible Pest Solutions .
Appreciate the insightful article. Find more at Affordable Pest Solutions .
The role of customer feedback loops in improving strategy was well articulated; thanks for sharing this valuable insight! Visit Rehan Hasan for similar discussions.
I love how hassle-free you made it sound to clean concrete! I’ll be due to these hints soon. https://shed-wiki.win/index.php/How_Winter_Affects_Your_Sidewalk_and_Tips_for_Spring_Cleaning_Without_a_Pressure_Washer
Thanks for the useful post. More like this at Hackettstown pest management services .
Thanks for the helpful advice. Discover more at Serenity Therapy Group .
Thanks for the thorough article. Find more at Affordable Pest Solutions .
Great job! Discover more at ادمین اینستاگرام .
Excellent read—backlinks are so important! I highly recommend looking into what’s available at Order backlinks .
Thanks for the valuable article. More at ادمین اینستاگرام .
If you need support with periodontal issues, look no further than a specialized ##Periodontist##. periodontist
Thanks for the detailed guidance. More at charlotte auto glass .
Anyone considering an office relocation should look up what Bronx movers offers.
This was nicely structured. Discover more at brain mapping with neurofeedback techniques Denver .
This was quite informative. More at Beverly Hills Dental Group .
Navigating credit issues is easier with buy here pay here dealers in Phoenix; check them out at buy here pay here phoenix az !
Appreciate the thorough analysis. For more, visit cost of toilet installation .
Just moved to San Diego and need a trustworthy atlas roofing sd for routine maintenance.
Thanks for the clear breakdown. More info at TheWinslo .
This was a wonderful post. Check out Affordible Pest Solutions for more.
Thanks for the thorough analysis. More info at shower drain cleaning services .
Kudos to the dedicated professionals at my local roofing company—they really know their stuff thanks to ##anyKeyword#! roofer escondido
Thanks for the useful suggestions. Discover more at https://atavi.com/share/xcphs2z7ke60 .
I found your tips on local SEO super beneficial! For additional insights, visit blackhat marketing blog .
This was a fantastic read. Check out ماساژ ماهور for more.
I found this very interesting. Check out Affordible Pest Solutions for more.
I recently learned about energy-efficient roofing thanks to my roofers . What a game changer!
This was quite useful. For more, visit ادمین اینستاگرام .
This was a fantastic read. Check out locksmith raleigh nc for more.
Love the emphasis on triumphant reinforcement! It makes this sort of difference in education. If you’re all for more recommendations, go to Learn more for additional supplies!
This was very enlightening. For more, visit local 24 hour plumber .
This was a fantastic read. Check out emergency blocked manholes for more.
I every time spent my half an hour to read this website’s articles daily
along with a mug of coffee.
¡Qué tal Espero que todo vaya excelente Quiero contarte sobre un casino virtual que te va
a encantar. La plataforma tiene una variedad
impresionante de juegos y una navegación muy fluida.
Si prefieres las slots, te fascinarán con la gran cantidad de slots.
Incluso, el casino tiene todos los juegos de mesa que puedes
imaginar.
Lo que más me gusta de este casino online es que tienen opciones
de pago locales. En América Latina, es muy importante que los métodos de pago
sean fáciles de usar y seguros, y este casino tiene un sistema de pagos rápido y seguro.
Y lo mejor de todo es que ofrecen promociones geniales para
jugadores nuevos. Cuando te registres,, recibirás un regalo para nuevos jugadores que te permitirá darle un buen comienzo a tu experiencia.
Y por si fuera poco, tienen promociones regulares.
Este casino también cuenta con atención al cliente
de primera, por si necesitas ayuda. Siempre podrás hablar
con un agente.
Otro punto fuerte del casino es la seguridad, el sitio
utiliza protocolos de seguridad avanzados para garantizar que tu dinero esté protegido.
No tendrás que preocuparte por nada.
Te invito a que te registres en este casino, te aseguro que no te
arrepentirás. ¡Es el momento perfecto para empezar a jugar!
Además, siempre podrás disfrutar de gráficos impresionantes.
Cada juego es una nueva oportunidad.
Mi sugerencia es que le des una oportunidad y disfrutes de
todo lo que tiene para ofrecerte. No dudes, Pablito, no te puedes
perder esta oportunidad. ¡Suerte y que empiecen las ganancias!
Wonderful tips! Find more at Affordable Pest Solutions .
Great tips! For more, visit pest exterminator Long Valley .
Well done! Find more at ادمین اینستاگرام .
Fantastic post! Discover more at ferretería cerca de mí .
From packing to unloading, my Midwest movers were incredible every step of the way—more info available at Midland international movers .
The Gibson Les Paul is truly iconic! I love how it combines classic design with modern tone. Check out more at Les Paul vs SG .
Appreciate the insightful article. Find more at locksmith gastonia nc .
Excellent information on Essex-based roofer organizations! It’s important for homeowners to comprehend the value of normal rooftop maintenance. If never addressed right away, dilemmas like spills or damaged bricks can result in expensive repairs flat roofing essex
Thanks for the valuable insights. More at fall heating repairs .
Thanks for the practical tips. More at ماساژ ماهور .
Each tip you shared makes me think extra sure about making advised selections referring to dwelling house safety!! Security Camera Installation Sanford
Well done! Find more at Serenity Therapy Group .
An outstanding share! I’ve just forwarded this onto a
colleague who has been doing a little research on this. And he actually ordered me lunch
because I found it for him… lol. So allow me to reword this….
Thanks for the meal!! But yeah, thanx for spending some time
to discuss this subject here on your web site.
The benefits of dental implants are incredible! They really do enhance your quality of life. Thank you, ##Periodontist##! periodontist near me
This was a great article. Check out plumbing and heating for more.
This is highly informative. Check out ادمین اینستاگرام for more.
I loved your point about authentic storytelling in branding—so important today! More inspiration at Rehan Hasan !
Great discussion on the ethics of drone pictures and respecting privateness rights! A must-examine for all drone lovers! More insights at http://timoore.eu/skins/timoore/redirect.php?url=https://rentry.co/z5sfkffu .
Thanks for the thorough analysis. Find more at affordable quality driveway paving .
Anyone else think that moving is easier with professionals like Cocoa apartment movers? Cocoa international movers
This was nicely structured. Discover more at Auto City Locksmith .
This was quite useful. For more, visit emergency shower drain repair .
Nicely done! Discover more at payday loans new orleans .
Great job! Discover more at plumbing contractors near me .
The history behind Gibson Les Paul guitars is fascinating! What’s your favorite fact about them? Discuss at Les Paul Zakk Wylde Signature .
So happy I chose a buy here pay here option in Phoenix! Explore your choices at buy here pay here phoenix az .
Moving offices can be daunting, but my Hempstead international movers in Hempstead made it such a smooth experience!
Appreciate the insightful article. Find more at NYC boutique bars with private rooms .
The testimonials available at #=#anything# helped me choose reliable #=apartmemt#movers# in #=MacClennyy# Local movers Macclenny
#Mississauga Periodontist#: providing top-notch treatments that make patients smile brighter every day! dental surgery
Has anyone used an office moving company in Melrose that they would recommend? I’m looking! Long distance movers Melrose
Well done! Find more at ماساژ ماهور .
Excellent content covering everything from hourly rates to specifics within each service type—I’m looking forward to exploring more about what’s offered at cleaning services Blairsville, PA! local cleaning services near me
Thanks for the comprehensive read. Find more at Serenity Psychotherapy Group .
Thanks for the great explanation. More info at Afordable Pest Solutions .
Thanks for the great information. More at effective pest management Long Valley .
This was very beneficial. For more, visit best plumbing .
I just had my roof repaired, and I can’t stress enough how crucial it is to locate trustworthy## Builders in Essex## roofers Chelmsford
Well explained. Discover more at ferreterías Albacete .
Quality posts is the main to interest the users to visit the
website, that’s what this website is providing. https://WWW.Geokniga.org/ext_link?url=http://dragon-slave.org/comics/MicheletoChampye
If you’re feeling stressed about your upcoming relocation, just remember there are plenty of qualified #anyKeyword# ready to assist you! Office moving companies Bellevue
Quality posts is the main to interest the users to
visit the website, that’s what this website is providing. https://WWW.Geokniga.org/ext_link?url=http://dragon-slave.org/comics/MicheletoChampye
This was highly educational. More at ادمین اینستاگرام .
This was a fantastic resource. Check out TheWinslow for more.
This was nicely structured. Discover more at rent a car .
I found this very interesting. Check out building design for more.
The roofing industry can be tricky, but jcis roofing makes it simple and reliable.
This was a fantastic read. Check out ماساژ ماهور for more.
Dogs have a unique means of creating day by day really feel brighter! How does your puppy deliver pleasure into your life? Tell us on https://wiki.gta-zona.ru/index.php/How_to_Create_a_Daily_Routine_that_Works_for_You_and_Your_Dog !
If you’re looking for a reliable plumber kalihi , I highly recommend checking out local options in Honolulu. They really know their stuff!
This was nicely structured. Discover more at basement water damage repair .
Very informative! It’s surprising what number worker’s fail to notice the magnitude of GPM in their daily lives. I’ll virtually be checking my fixtures and home equipment now! https://www.plurk.com/p/3hgnx9iyql
San Diego’s unique climate requires specialist knowledge from our local # roofers in San Diego
Everything is very open with a precise clarification of the
issues. It was truly informative. Your site is useful.
Thanks for sharing!
PSS Sleman
Great insights! Find more at ادمین اینستاگرام .
Fantastic post! Discover more at ادمین اینستاگرام .
I found this very interesting. Check out Afordable Pest Solutions for more.
This was a wonderful post. Check out ferreterías Albacete for more.
What do you believe you studied makes mixed-breed puppies one-of-a-kind in contrast to purebreds? Share your feelings less than! https://e58dp.mssg.me/
#Dental Clinic#: where your path toward better oral health begins—book that appointment today! dentist near me
The neck on a Les Paul feels so smooth; it’s perfect for solos! What’s your favorite solo to play? Discuss at Les Paul Historic Reissue .
Can’t wait for summer riding camps—I found some awesome options on horseback riding near Jaco !
Great insights! Find more at https://unsplash.com/@marielekke .
I truly appreciate your technique of writing a blog. I added it to my bookmark site list and will
This was very beneficial. For more, visit animal hospital .
Appreciate the detailed post. Find more at Aldridge Roofing & Restoration .
This was quite informative. More at Farsi speaking counseling .
Nicely done! Discover more at ادمین اینستاگرام .
I enjoyed this article. Check out indoor air quality testing nearby for more.
Thanks for the valuable insights. More at K. Vet Animal Care .
This was nicely structured. Discover more at ماساژ ماهور .
Appreciate the thorough write-up. Find more at Plumbing and heating .
Informative post—thank you! I’m getting quotes from several places, including the highly recommended Brandon vehicle shipping .
Thanks for the valuable insights. More at plumbing line .
Shoutout to all the incredible office moving companies in Melrose making relocations easier for businesses like ours! Best Melrose movers
Great article highlighting the importance of dryer vent care—let’s keep our homes safe by reaching out to experts like Dryer Vent Cleaning #.
Definitely going to proportion this with my pals; we all need refreshing sidewalks in our neighborhood! https://wiki-square.win/index.php/Understanding_the_Science_Behind_Cleaning_Products_for_Concrete_Surfaces
This is such an informative article! I’m continually looking for new methods to improve my canine’s behavior. I found a few super suggestions at https://www.social-bookmarkings.win/the-expense-of-canine-tuition-camp-can-vary-commonly-depending-on-components-like-region-period that enhances your options.
Love your perspective on this topic! Can’t wait to enhance my site’s authority with links from Is it safe to buy backlinks in 2025? !
Valuable information! Discover more at foothills paving and maintenance .
#Gum grafts#: it’s incredible how they can restore both function and aesthetics—talk to your trusted #Dentist#! dentist near me
Roof maintenance is essential! Thanks to my local ### anyKeywords### for keeping it in shape! roofer near me
Fantastic suggestions for finding the top roofing contractors in Essex! With the erratic temperature we experience, the importance of superior rooftop never be overstated roofers in essex
The creativity displayed by social media influencers in content creation is always impressive and inspiring! influencers
Thanks for the informative post. More at TheWinslo .
This is quite enlightening. Check out toilet installation services for more.
Has anyone tried playing classical music on a Gibson Les Paul? It sounds surprisingly good! Let’s discuss genre blending over at Les Paul Sunburst !
Tankless water heaters provide endless hot water without taking up space—a perfect option for small homes or apartments looking for efficiency! local plumber
Just got a quote from roofer escondido , and their pricing is very competitive for Escondido roofers.
Appreciate the insightful article. Find more at ماساژ ماهور .
Just got my first car through a buy here pay here program in Phoenix! Visit buy here pay here car lots phoenix az to see what’s available.
This was quite useful. For more, visit knee pain relief Boise ID .
Learning opportunities abound when researching contractors online—grateful for what’s available through ### anykeyword###!! San Diego County Roofing
This was a wonderful post. Check out Afordable Pest Solutions for more.
Thanks for the thorough analysis. More info at ادمین اینستاگرام .
Very useful post. For similar content, visit ادمین اینستاگرام .
ความแตกต่างระหว่างไฟหน้าธรรมดาและไฟหน้าโปรเจคเตอร์คืออะไร? อ่านที่นี่เลย หลอดไฟรถ
Thank you for sharing your data about aerial mapping with drones; that is something I’ve been curious about for some time now! Check out more at https://dongxi.douban.com/link2/?url=https://wiki-spirit.win/index.php/**Elevate_Your_Photography_Game:_Creative_Techniques_for_Using_a_Drone_Camera** .
Everyone involved showed such dedication towards making sure every detail was taken care of at #OfficeMoversTangerine! Tangerine apartment movers
The merits of getting a defense camera technique are simple! I need to get this accomplished quickly. Sanford Security Camera Installation
The importance of quality backlinks can’t be stressed enough; check out Is it safe to buy backlinks in 2025? for reliable services!
Have you ever participated in a puppy convey or match? It sounds so unique! Learn extra about nearby activities at https://front-wiki.win/index.php/Why_Consistency_is_Key_in_Training_Your_Dog_Effectively .
When it comes to cleaning a deck, I came across that a strain washer with as a minimum 2500 PSI works wonders. It honestly will get rid of grime and dust! Check out greater pointers at https://www.plurk.com/p/3hgnx9iyql .
Appreciate the helpful advice. For more, visit emergency plumbing repair .
Appreciate the thorough insights. For more, visit car locksmith .
This was a wonderful guide. Check out TheWinnslow for more.
This was highly helpful. For more, visit ادمین اینستاگرام .
Excellent article on Essex roof providers! Finding trustworthy roofers who can handle anything from upgrades to new deployments is always important. Being able to have a strong ceiling is more crucial than ever in the face of unstable conditions roofer essex
Loving how natural and comfortable my new dental implants feel; such an improvement thanks to an expert hand at work from my trusted ###Periodontists### office! dentist
I found this very interesting. Check out lock smith for more.
I enjoyed this post. For additional info, visit Professional local pest control Hackettstown .
Thanks for the comprehensive read. Find more at trusted pest control services Long Valley .
Hello friends, nice article and nice urging commented
here, I am in fact enjoying by these.
Is anyone else fascinated by the rich history behind each model of the Gibson Les Paul’s lineage? What’s your favorite historical fact? Engage with us over at Les Paul Ace Frehley Signature !
This publish is a really good source for new puppy householders! I surely relish the useful guidance you’ve offered. For further reading, go to https://www.paste-bookmarks.win/the-cost-of-dog-schooling-camp-can-range-generally-based-on-factors-like-location-length .
Thanks for the comprehensive read. Find more at loan agency new orleans .
Great job! Find more at ماساژ ماهور .
작은 피로도 놓치지 않는 섬세한 관리, 토닥이에서 차원이 다른
케어를 만나보세요. 지금 이용해보세요.
Love seeing such thorough exploration related to this obligatory matter—it if truth be told encourages informed choice-making!!! # #anythingKeywords ## https://stalinarch.ru/wiki/index.php/How_to_Secure_Every_Angle:_Effective_Camera_Positioning_Tips
Thanks for the helpful advice. Discover more at Serenity Therapy Group .
For anyone with credit issues, buy here pay here is a lifesaver in Phoenix. Visit buy here pay here phoenix az for more information.
I’ve finally tackled my fear of dental surgery thanks to an understanding and skilled ##Dentist##. periodontist
Very informative article. For similar content, visit ادمین اینستاگرام .
This was very enlightening. For more, visit ادمین اینستاگرام .
Hello, i think that i saw you visited my blog thus
i came to “return the favor”.I’m trying to find things to enhance my web site!I
suppose its ok to use a few of your ideas!!
The connection between lint buildup and fire risk is alarming! Thanks for bringing attention to this topic—check out Dryer Vent Cleaning Seattle !
Thanks for the insightful write-up. More like this at locksmith high point nc .
” Our neighborhood block party wouldn’t have been half as fun without that huge waterslide we rented last month—it really brought everyone together!” # # anyKeword#” renting tents near me
San Diego’s weather can be tough on roofs. Make sure to consult with professionals from atlas roofing sd for a thorough inspection.
Appreciate the detailed information. For more, visit foothills paving and maintenance .
The team from Tangerine Commercial Movers exceeded our expectations in every way during our recent move! Fantastic service! Visit Tangerine commercial movers for details.
Wonderful advice shared here regarding SEO best practices; highly considering using links from Buy SEO backlinks #
I’m so glad I chose Homestead car transportation services for my recent homestead vehicle shipment—everything went smoothly!
Thanks for the comprehensive read. Find more at TheWinslow .
Appreciate the comprehensive advice. For more, visit https://maps.app.goo.gl/ozEA9FpDvYZWJRa6A .
A Les Paul is definitely worth the investment for any serious guitarist! What do you think? Share your views at Les Paul Fretboard Radius .
From start to finish, %made my recent move seamless and enjoyable. Plantation apartment movers
After my storm damage, I called JCIS Roofers , and they quickly helped me out with repairs.
When tackling commercial plumbing needs, go with someone experienced—like our fantastic local ### anyKeywords### team! trenchless sewer line
I appreciated this post. Check out ادمین اینستاگرام for more.
I on no account proposal approximately the value of battery lifestyles administration at the same time flying drones! Great reminder! For additional insights, test out http://www.bausch.pk/en/redirect/?url=https://hubpages.com/@merrinktxl .
When I originally commented I clicked the “Notify me when new comments are added”
checkbox and now eac time a comment is added I get three emails with the same comment.
Is there any way you caan remove people fom that
service? Bless you!
Allso visit my site Hijyenik Klozet Poşeti
“Can anyone share tips on how to maintain roofs between visits from your ###RooferInSanDiego###?” San Diego County Roofing
With skilled hands, the massage at 토닥이 completely relieved
my fatigue from the day. I’m genuinely satisfied with the experience.
If you’re considering moving, make sure you check out what’s available at Best Ocoee movers
Appreciate the detailed insights. For more, visit ادمین اینستاگرام .
Wonderful tips! Discover more at ferreterías Albacete .
Love this content! The idea of buying safe backlinks through Link building service seems very promising.
Just finished dental surgery, and I’m feeling great! Big thanks to my amazing ##Dentist## for the support. periodontist near me
This was highly educational. For more, visit TheWinslow .
Great job! Discover more at ماساژ ماهور .
I liked this article. For additional info, visit LuxNuro .
Appreciate the thorough information. For more, visit ادمین اینستاگرام .
Helpful suggestions! For more, visit ادمین اینستاگرام .
I enjoyed this post. For additional info, visit Foothills Paving .
Thanks for the great information. More at Afordable Pest Solutions .
Thanks for the useful post. More like this at Dental Group Beverly Hills .
Appreciate the thorough insights. For more, visit Affordable Pest Solutions .
Genshin Impact can drain my wallet, so I’m excited to hear any money-saving strategies! Primogems via ManaBuy
Great job! Find more at ferretería Albacete .
An intriguing discussion is worth comment. I think
that you should publish more on this subject matter, it might not be a taboo subject but
typically folks don’t speak about such topics. To the next!
Cheers!!
So grateful for all that I’ve learned from consultations regarding dental health and procedures.”, dental implants Mississauga
Tankless water heaters are fantastic! My Honolulu plumber explained everything during the installation process.
This was very enlightening. For more, visit Affordable Pest Solutions .
The binding on a Gibson Les Paul adds such elegance to its design! Do you have a favorite finish color? Share thoughts at Les Paul Traditional .
A huge shoutout to everyone who helped us find our amazing local Escodnido Roofer through ##anyKeyword#! JCIS Roofers
This was quite useful. For more, visit ادمین اینستاگرام .
Thanks for the useful suggestions. Discover more at ماساژ ماهور .
The guidelines theory is golden; it allows keep every little thing well prepared and reduces anxiousness in the time of actions! mudança em sorocaba
Using strong bins can shop lots quandary all through shipping! Great recommendation the following! mudanças em sorocaba
Thanks in support of sharing such a pleasant opinion, paragraph is nice,
thats why i have read it fully
Thanks for the detailed guidance. More at Serenity Therapy Group .
This paragraph will assist the internet visitors for creating new webpage or even a blog from start to end.
I invariably suggestion extra GPM was once more beneficial, however now I observe that it relies upon on the process at hand. This submit has opened my eyes to the value of matching pass charges with needs. https://padlet.com/devpage7pbziy/bookmarks-makh7r0bn5x4ciw4/wish/L8KjW9Pb39XYZJbv
This was quite informative. More at LuxNeuro .
This was very enlightening. For more, visit Boiler breakdowns .
Appreciate the comprehensive insights. For more, visit ادمین اینستاگرام .
This was beautifully organized. Discover more at emergency plumbing prices .
I appreciated this post. Check out checkatrade plumbers for more.
This was nicely structured. Discover more at Foothills Paving .
Planning an office move soon? Definitely consider looking into options at Long distance movers Plantation —they’ve got great reviews on local companies in Pompano Beach!
I enjoyed this read. For more, visit Beverly Hills Dental Group .
For those living in Phoenix, the buy here pay here options are plentiful! Visit buy here pay here phoenix az to learn more.
Hey there! I’m at work surfing around your blog from
my new iphone 3gs! Just wanted to say I love reading through your blog
and look forward to all your posts! Carry on the great work!
Thanks for the insightful write-up. More like this at https://maps.app.goo.gl/ZjUR3iGdEyYpM5Wd6 .
Thank you for sharing your knowledge! I’m eager to improve my site’s rankings with help from White hat link building .
Wonderful tips! Find more at TheWinslo .
I enjoyed this read. For more, visit ماساژ ماهور .
I’ve heard mammoth things approximately ManaBuy discount recharge for topping up Genshin crystals! Can’t wait to check out it out myself.
This was very enlightening. For more, visit Affordible Pest Solutions .
Thanks for the insightful write-up. More like this at reliable drain cleaning services .
Hello there! I simply would like to offer you a big thumbs up for your great
information you have right here on this post.
I am returning to your site for more soon.
สุดท้ายแล้วก็ต้องกลับมาที่ร้านเหล้าสาย1 เพราะบรรยากาศดีมาก! ร้านชิลเหมาะกับจัดวันเกิด สาย1
Nicely done! Discover more at Serenity Therapy Group .
The feeling when you hit that first chord on a fresh set-up Gibson Les Paul is unbeatable! How often do you set up yours? Let’s talk setups over at Best Les Paul for Blues !
Just finished my search for office movers and settled on Winter Haven commercial movers ! Excited for our move in Winter Haven.
Relocating to Bellevue? Make sure you read up on local movers first! Great insights await you at Local movers Bellevue .
”Feeling thankful after stumbling upon this insightful post addressing core challenges often encountered while navigating procedures related towards safely transferring personal vehicles throughout densely populated environments primarily influenced by Houston car transportation services
This was highly informative. Check out Affordible Pest Solutions for more.
This was beautifully organized. Discover more at ادمین اینستاگرام .
Moving across state lines? Make sure you consult with a qualified agent from Sinton via Flexible Vehicles Shippings
The crew at # # anyKeyWord# # helped me move quickly and efficiently into my new apartment in Melrose—highly recommend them! Melrose moving companies
This post is a brilliant source for brand spanking new puppy householders! I definitely understand the lifelike suggestions you’ve supplied. For in addition interpreting, consult with https://www.booknose.win/the-rate-of-canine-guidance-camp-can-differ-largely-relying-on-explanations-like-region-length .
Every visit to my local #Periodontal services# provider has been enlightening and beneficial!”, gum grafts
I found this very interesting. Check out rent a car for more.
This was a great article. Check out intimate bar experiences NYC for more.
ไฟหน้าแบบไหนที่เหมาะกับสภาพถนนในเมืองไทยที่สุดครับ?? ร้าน เปลี่ยน โคม ไฟ หน้า รถยนต์ ใกล้ ฉัน
Organizing resources prior to a pass is so valuable! Check out mudança em sorocaba for additional counsel and hints.
Thanks for the recommendation on maintaining a first-evening container handy; it makes settling in a lot more easy! empresa de mudanças
Thank you for addressing time-honored error other folks make while shifting—recognition enormously allows hinder them subsequent time around mudanças em sorocaba
This is quite enlightening. Check out ادمین اینستاگرام for more.
Does everyone right here have journey with big puppy breeds? How do they evaluate to smaller ones? https://www.symbaloo.com/mix/bookmarks-1gj3
This post is truly informative; can’t wait to try out the backlink services offered by Best link building service 2025 #!
This was very enlightening. For more, visit LuxNuro .
Appreciate the comprehensive insights. For more, visit Affordable Pest Solutions .
¡Qué tal Espero que estés bien Tengo una excelente recomendación para ti un casino virtual que es perfecto para jugadores como tú.
Este casino tiene una oferta increíble de juegos y una interfaz fácil de usar.
Si eres un fanático de las tragamonedas, te sorprenderán con la amplia oferta de juegos.
Incluso, el casino tiene los clásicos de casino como el blackjack y la ruleta.
Lo que más me gusta de este casino online es que ofrecen métodos de pago muy accesibles.
Sabemos que en nuestra región, es muy importante que los métodos de pago sean fáciles de usar y seguros, y este casino tiene opciones de pago
muy convenientes.
Además, te dan bonos de bienvenida para jugadores nuevos.
Tan pronto como te registres,, recibirás un regalo para nuevos jugadores que te permitirá comenzar a jugar con ventaja.
También, tienen bonos especiales durante todo
el año.
La web también cuenta con soporte al cliente
24/7, si tienes dudas o problemas. Siempre tendrás un agente disponible.
La plataforma es completamente segura, el portal
utiliza tecnología de encriptación para que tu privacidad esté a salvo.
Jugar aquí es completamente seguro.
Si decides probar esta web, te aseguro que no te arrepentirás.
¡Las posibilidades de ganar son enormes! Además, siempre podrás disfrutar de una interfaz fluida y agradable.
Te vas a divertir muchísimo.
Mi sugerencia es que entres ahora mismo y disfrutes de todo lo que tiene para ofrecerte.
Ya sabes, Pablito, te garantizo que disfrutarás mucho.
¡Suerte y que empiecen las ganancias!
Appreciate the comprehensive advice. For more, visit Pest Removal Long Valley .
แนะนำให้ทุกคนมาลองเล่นเกมตอนกลางคืนที่นี่กันเถอะ # # anyKeyWord## ผับจัดวันเกิด สาย1
Useful advice! For more, visit Foot Hills Paving .
This was very beneficial. For more, visit Dental Group of Beverly Hills .
For those living in San Diego, don’t forget to check out roofer in san diego for reliable roofing professionals.
#Dental Clinic# staff were so supportive during my journey with #dental implants#—I couldn’t have done it without them! periodontist near me
This is very insightful. Check out Affordable Pest Solutions for more.
This was a wonderful post. Check out https://unsplash.com/@idrosevfor for more.
Thanks for dropping gentle at the so much standard error employees make with digicam placements—positive data! Extra resources
Thanks for the great explanation. More info at ماساژ ماهور .
Recently purchased my car through a local buy here pay here dealer and couldn’t be happier! More details at buy here pay here phoenix az .
Thanks for the helpful article. More like this at Eco-Friendly Pest Control Flanders .
This was quite enlightening. Check out how to repair a dishwasher for more.
Water heaters may seem complicated but rest assured knowing experts are here willing/able assist whenever needed most!! drain cleaning
Great guidance on employing drone cameras! I under no circumstances knew approximately the magnitude of balancing the gimbal. Check out greater at http://www.bookmerken.de/?url=https://www.magcloud.com/user/lefwensmpr .
Great job! Discover more at local tap specialists .
ไฟหน้ารถ LED กับไฟฮาโลเจน อันไหนดีกว่ากัน? ร้านซ่อมไฟหน้ารถยนต์ ใกล้ฉัน
Greetings I am so excited I found your website, I really found you by error, while I was browsing
on Aol for something else, Nonetheless I am here
now and would just like to say thanks a lot for a marvelous post and a all round entertaining blog (I also
love the theme/design), I don’t have time to go through it all at the
minute but I have saved it and also included your RSS feeds, so when I have time
I will be back to read more, Please do keep up the great job.
This was a great help. Check out ادمین اینستاگرام for more.
ฉันรักค็อกเทลที่ OMG ONE MORE GLASS SAI1 มาก อร่อยและสดชื่นสุดๆ ร้านชิลเหมาะกับจัดวันเกิด สาย1
I’m considering adding another Les Paul to my collection; any recommendations? Let’s help each other out at Gibson Les Paul Custom .
Interested if there are tools available simplifying organization efforts throughout entire coordination stages leading up through engagement alongside # # anyKeyWord#. Cheap movers Winter Haven
Well done! Find more at LuxeNeuro .
This is so worthy, exceedingly for first-timers like me! Thanks for breaking it down so in reality! Find more information
This was highly educational. For more, visit Roof repair near me .
Well done! Discover more at ferreterías Albacete .
”Loved learning more about sustainable practices within our local roofing community of # SD Roofing & Solar
Wow, awesome blog layout! How long have you ever been blogging for?
you make running a blog glance easy. The total glance of
your web site is excellent, as smartly as the content! http://www.foot-palmares.com/comment/html/?63220.html
Wow, awesome blog layout! How long have you ever been blogging for?
you make running a blog glance easy. The total glance of your
web site is excellent, as smartly as the content! http://www.foot-palmares.com/comment/html/?63220.html
I liked this article. For additional info, visit Walk-In Emergency Dentist Beverly Hills .
This was quite helpful. For more, visit Foot Hills Paving .
รู้สึกว่าร้าน OMG OneMoreGlass มีเอกลักษณ์เฉพาะตัวจริงๆ นะครับ ร้านเหล้าบางแค
Well explained. Discover more at Plumbing & heating .
Well explained. Discover more at Affordable Pest Solutions .
Thanks for the thorough analysis. More info at TheWinslow .
Anyone else used #(#) anyKeyWord# for their office moves? Would love some feedback! Bronx international movers
This was highly educational. For more, visit ماساژ ماهور .
I’ve been using backlinks from Backlink packages for a while now and have seen significant improvements in my traffic!
I appreciated this post. Check out ادمین اینستاگرام for more.
This was quite helpful. For more, visit Affordable Pest Solutions .
I’ve heard gigantic issues approximately ManaBuy Genshin recharge for topping up Genshin crystals! Can’t wait to are attempting it out myself.
I absolutely love your blog and find many of your post’s to be just what
I’m looking for. Do you offer guest writers to
write content for you? I wouldn’t mind creating a post or elaborating on many of
the subjects you write regarding here. Again, awesome weblog!
Thanks for the informative post. More at Serenity Therapy Group .
Thanks for the great tips. Discover more at Pest Control Services Long Valley .
This was highly educational. For more, visit Affordible Pest Solutions .
Feeling grateful for the care I received from my awesome ##Mississauga Periodontist## during my last visit. periodontist near me
I’ve heard great things about chiropractic services in DeSoto. Thinking of visiting Chiropractor for car accident near me soon!
Your thoughts on video marketing trends were enlightening! Video content is definitely the future. Explore more at Rehan Hasan !
Appreciate the insightful article. Find more at car locksmith .
Thanks for sharing those details! For everybody trying to go properly, be sure to stopover at mudança em sorocaba for specialist guidelines.
Hmm is anyone else having problems with the pictures on this blog loading?
I’m trying to determine if its a problem on my
end or if it’s the blog. Any feed-back would
be greatly appreciated.
https://st-johannes-sundern.de/
Your article is a lifesaver for every body planning a circulate! Don’t fail to remember to envision out mudanças em sorocaba for greater notable tips.
Keep sharing tips on vetting potential candidates because it really helps others looking for quality service like this one! atlas roofing sd
So desirable approximately desiring persistence and flexibility for the period of movements, as matters not often cross as deliberate—it’s exceptional to get ready mentally too! empresa de mudanças
Thanks for the helpful advice. Discover more at Thermostats Gas valves .
Thanks for the clear advice. More at need a plumber .
Thanks for the informative post. More at ماساژ ماهور .
Having access to reliable emergency plumbers makes all the difference when urgent problems arise—you never know when you’ll need them next! Honolulu plumber
What a exclusive article! Training our hairy chums shall be hard, but your systems make it simpler to realize. For greater standards, cost out https://www.bookmarkmaster.win/the-check-of-puppy-training-camp-can-range-broadly-depending-on-reasons-like-location-length !
I read this post completely on the topic of the comparison of latest and preceding technologies,
it’s amazing article.
This was very well put together. Discover more at TheWinslo .
Thanks a lot for sharing this with all of us you actually realize what you’re
talking about! Bookmarked. Please also seek advice from my site =).
We may have a link alternate arrangement among us
Thanks for finally writing about > Certain Scores
May Predict Which Trauma Patients Face High Risk of Multiple
Infections – Healthcare Hygiene magazine < Liked it!
I’ve heard so many good things about roofer escondido from friends in Escondido; they must be doing something right!
A great experience overall thanks to my local Glendale movers – made everything stress-free! Glendale commercial movers
This is quite enlightening. Check out ادمین اینستاگرام for more.
Our community is lucky to have such dedicated care providers specializing in periodontal services!”, dental surgery
This was highly educational. For more, visit LuxNuro .
Thanks for the informative post. More at Slab leak repair .
Helpful suggestions! For more, visit Affordible Pest Solutions .
I appreciated this article. For more, visit Hackettstown dependable pest solutions .
Appreciate the thorough analysis. For more, visit ferretería en Albacete .
Thanks for the useful post. More like this at affordable emergency oral care .
I found an excellent San Diego County Roofing in San Diego who specializes in tile roofing – so impressed with their work!
Thanks for the valuable article. More at Foothills Paving .
Thanks for the clear breakdown. More info at Affordable Pest Solutions .
This was a wonderful post. Check out payday loans new orleans la for more.
Loved sharing experiences with others about our favorite reliable options among those wonderful services available locally!!!# anyKeywords # Bronx moving companies
Thanks for the thorough analysis. More info at ماساژ ماهور .
This is quite enlightening. Check out Flanders rodent extermination for more.
Thanks for the valuable article. More at ادمین اینستاگرام .
Great post on the significance of user experience in web design! Essential for conversions! More ideas at Rehan Hasan !
Thanks for the insightful write-up. More like this at Serenity Therapy Group .
Great article stuffed with major moving hints and methods! Don’t pass over journeying empresa de mudanças for additional insights!
Organization is fundamental whilst relocating. Thanks for sharing those successful insights! mudanças em sorocaba
Your emphasis on maintaining fragile items whereas packing is so incredible; I’ve made that mistake ahead of! mudança em sorocaba
Cheap ways to top up? Count me in! I need to enhance my characters without spending too much. ManaBuy UID top-up
I didn’t appreciate how marvelous it’s to examine local policies previously flying a drone. Thanks for the understanding! Explore more at http://www.badmoon-racing.jp/frame/?url=https://direct-wiki.win/index.php/**Exploring_Scenic_Landscapes:_How_to_Use_a_Drone_Camera_for_Breathtaking_Travel_Photos** .
This was nicely structured. Discover more at ادمین اینستاگرام .
Just sealed the deal on my new-to-me car with a buy here pay here option—so excited! More info at buy here pay here phoenix $500 down .
Thanks for the helpful advice. Discover more at LuxeNeuro .
This is quite enlightening. Check out sink installation services for more.
Is anyone else fascinated by the rich history behind each model of the Gibson Les Paul’s lineage? What’s your favorite historical fact? Engage with us over at Vintage Les Paul Guitars !
Thanks for the informative content. More at automotive locksmith winston-salem nc .
Appreciate the comprehensive advice. For more, visit http://noreferer.net/?url=https://store.magic-tricks.ru//user/hyarisnixh .
This was a fantastic read. Check out toilet plumber for more.
Valuable information! Find more at ferretería Albacete .
I’ve seen many good reviews about # Winter Haven movers #; I’m excited about using their services next month!
This was a wonderful post. Check out Dental Group Beverly Hills for more.
Thanks for the informative content. More at Commercial Driveway Paving Wheat Ridge .
Moving is such an important life event—make sure you choose wisely who helps make it happen; trust those experienced professionals like those found via searching “movers st augustines” online today! St. Augustine moving companies
This was highly educational. For more, visit ماساژ ماهور .
This was highly educational. For more, visit local insect control Budd Lake .
Great article on auto shipping! I’ll definitely be using the recommendations from Houston car transportation services .
My experience with Sinton has been nothing short of excellent; they care about their clients! Sinton car transportation services
Helpful suggestions! For more, visit TheWinslo .
Wonderful tips shared; looking forward to improving my website’s performance with help from __ anyKeyWord__! High DA backlinks for sale
This was quite enlightening. Check out underfloor heating troubleshooting for more.
Great job! Find more at ادمین اینستاگرام .
This was very beneficial. For more, visit Afordable Pest Solutions .
My experience with restoration companies in my area was excellent! They turned a nightmare into a manageable situation quickly.
Great job! Discover more at ادمین اینستاگرام .
This was very beneficial. For more, visit Serenity Therapy Group .
I recently faced water damage in my home, and I wish I had known about the services available in Hawaiian Gardens earlier! flood restoration companies near me
Great job! Find more at Affordible Pest Solutions .
Seriously considering another move just because of how easy things were with # anyKeyWord#! Hawthorne apartment movers
Genshin Impact can be expensive, but I’m intrigued by your approach. Let’s hear it! buy Genshin recharge at ManaBuy
This was a great help. Check out Hackettstown pest management solutions for more.
This was highly educational. More at certified plumber .
Quick response is key when dealing with water damage—thankful for the services offered by local companies in Irving TX! water damage restoration companies near me
Saving money while ensuring quality craftsmanship seems possible thanks largely due diligence conducted via platforms like ###ANYKEYWORD#### ! roofer near me
Remember—the sooner you act, the better your chances of minimizing damages!! Don’t wait!! #TakeAction water damage restoration companies near me
Thanks for the great information. More at car rental toronto .
The diversity of perspectives showcased in your articles makes for an enriching experience when visiting Stallion Guns .
Does anyone else have a ‘dream’ version of their perfect Gibson Les Paul in mind that they wish existed? Let’s brainstorm ideas together over at Les Paul Ace Frehley Signature
I’m impressed by how you connect historical events with current issues in your posts at worlds largest online paintball store .
Great insights! Find more at ماساژ ماهور .
Nicely detailed. Discover more at ادمین اینستاگرام .
After moving into an older house, we faced some unexpected plumbing issues; thankfully we found great support through ###in our area! water damage restoration companies near me
This was a great article. Check out Sewer line repair for more.
This was very beneficial. For more, visit building design Norfolk VA .
Appreciate the helpful advice. For more, visit cozy bars with secluded spaces NYC .
Had an excellent experience with a local emergency plumber who handled my situation quickly and professionally—so grateful for their expertise! local plumber
I’ve heard combined evaluations approximately a range of crystal recharge providers, however your experience with Manabuy offers me self assurance to try it! cheap top-up ManaBuy
Every breed has its own one of a kind characteristics and wants. Which breed do you believe is the superb suit for a kinfolk? Share stories at https://wiki-room.win/index.php/The_Importance_of_Hydration_in_Maintaining_Canine_Health !
What are a few lesser-known canine breeds that americans should concentrate on adopting? https://atavi.com/share/xcewktz1qcekn
Got inspired by this blog post—can’t wait to explore # # anY KeyWord # more JCIS Roofers
I found this very helpful. For additional info, visit ادمین اینستاگرام .
I appreciate the insights here! I’ve been hesitant about buying backlinks, but with services like Where to buy backlinks that actually work , it sounds safe and effective.
It’s pleasing how GPM can impression no longer merely efficiency but also the ecosystem. I’m excited to implement some of these recommendations in my dwelling! https://579na.mssg.me/
Hola Espero que todo vaya excelente Hoy quiero recomendarte un casino virtual que es ideal para
ti. Este casino tiene juegos emocionantes para todos los gustos y una experiencia de usuario increíble.
Si prefieres las slots, te fascinarán con la amplia oferta de juegos.
Además, el casino tiene los clásicos de casino como el blackjack y la ruleta.
Una de las mejores cosas de este casino online es
que tienen opciones de pago locales. Sabemos que en nuestra región,
es muy importante que los métodos de pago sean fáciles de usar y seguros, y este casino tiene un sistema de pagos rápido y seguro.
Por si fuera poco, ofrecen promociones geniales para jugadores nuevos.
Tan pronto como te registres,, recibirás un regalo para nuevos jugadores que te permitirá comenzar a jugar con ventaja.
También, tienen torneos con grandes premios.
La web también cuenta con soporte al cliente 24/7,
por si necesitas ayuda. Siempre podrás hablar con un agente.
La seguridad es otro aspecto importante, el portal
utiliza encriptación de última generación para mantener tu información personal
segura. Jugar aquí es completamente seguro.
Si decides probar esta web, te aseguro que no te arrepentirás.
¡Tienes mucho que ganar! Además, siempre podrás disfrutar de
una experiencia de juego sin igual. Te vas a divertir muchísimo.
Mi consejo es que te registres cuanto antes y disfrutes de todo lo
que tiene para ofrecerte. Confío que lo
harás, Pablito, este es un excelente lugar para jugar.
¡Suerte y que empiecen las ganancias!
Well done! Find more at LuxeNeuro .
If you’re looking for a reliable Glendale moving company, I highly recommend checking out their services! Office moving companies Glendale
This was very well put together. Discover more at basement water damage Edina .
This was very enlightening. More at residential pest control services Long Valley .
Did anyone else enjoy their experience with a local mover in Winter Haven? Share your stories or check out recommendations at Cheap movers Winter Haven !
Thanks for the valuable insights. More at Afordable Pest Solutions .
I enjoyed this article. Check out Beverly Hills Dental Group for more.
“My neighbor just got their roof done by an amazing ###RooferInSanDiego###; it’s stunning!” roofers
I had a fantastic experience with a buy here pay here dealer in Phoenix. Highly recommend checking out buy here pay here car lots phoenix az for deals!
Love your real looking mind-set closer to more secure transferring practices—so powerful! Visit empresa de mudanças for even greater important content!
Great job! Find more at ماساژ ماهور .
The impact of augmented reality experiences on engagement levels is interesting — thanks for covering it ! Explore AR implementations via ### anyKeyWord### . Rehan Hasan
This was a wonderful post. Check out Affordable Pest Solutions for more.
Appreciate your insights on determining among DIY actions versus hiring professionals—it enables clarify judgements! mudança em sorocaba
Safety first in terms of relocating! I especially advocate traveling mudanças em sorocaba for seasoned suggestions on safe transportation.
Fantastic post! Discover more at emergency plumbing services near me .
Appreciate the comprehensive advice. For more, visit indoor air quality testing services .
I liked this article. For additional info, visit ادمین اینستاگرام .
รีวิวจากผู้ใช้งานจริงเกี่ยวกับสินค้าเหล่านี้น่าสนใจมาก ซ่อมไฟรถยนต์ ใกล้ฉัน
Appreciate the comprehensive advice. For more, visit Water heater repair .
I appreciated this article. For more, visit https://www.hometalk.com/member/178939267/mollie1878831 .
I’ve heard great things about office movers in the Bronx! Look into Bronx international movers for your move.
I’ve been as a result of Manabuy for my Genshin Impact most sensible-america well, and I must agree—it can be definitely more cost effective than the in-sport choices! Highly endorse it! top-up your UID with ManaBuy
This was very enlightening. More at veterinarian Greensburg .
Great tips! For more, visit physical therapy Boise .
Training may well be a hassle, yet your doorstep-by means of-step technique makes it seem doable! I’ll absolutely be trying out https://www.bookmark-belt.win/the-expense-of-puppy-guidance-camp-can-range-broadly-depending-on-points-like-area-length for greater preparation tricks.
This info is priceless. How can I find out more?
Feel free to suref to my web page – temp mail for Netflix trial
Thanks for the great information. More at septic tank service nearby .
Just had my roof replaced by a San Diego roofer I found through atlas roofers . Couldn’t be happier with the results!
I found your comparisons between different weapon types very eye-opening, particularly those featured at Buy Suppressors & Gun Silencers Online .
Great tips on preventing water damage! Also, keep water damage restoration services near me in mind for when emergencies happen.
There’s definately a great deal to know about this issue.
I really like all the points you have made.
This was a fantastic read. Check out mold remediation Seattle WA for more.
Thanks for the great information. More at Immediate Dental Care Beverly Hills .
Finding reliable information surrounding best practices implementing preventative measures protecting properties regularly goes long way ensuring peace mind among families residing nearby helping others underst water damage restoration service near me
Appreciate the helpful advice. For more, visit ادمین اینستاگرام .
This was highly educational. More at emergency plumber near me .
This was quite informative. For more, visit ماساژ ماهور .
Great job! Find more at Afordable Pest Solutions .
I find myself constantly experimenting with my tone settings on my Gibson Les Paul’s pickups; it’s an endless journey! How about you? Share insights over at Les Paul Ace Frehley Signature !
Appreciate the thorough insights. For more, visit knee pain relief near me .
Water heater installations can be tricky; make sure you hire someone who knows what they’re doing! I found an excellent service via ##local plumber## resources. emergency plumber
Anyone looking for reliable water damage restoration should check out the options available in Irving TX! restoration companies in my area
Awesome article! Discover more at Somers Plumbers – Phoenix Plumbing Company .
Just found out out about find UID top-up at ManaBuy for Genshin crystal prime-ups! Looking ahead to wanting it founded on my mates’ suggestions.
Water damage can be devastating, but with the right restoration service, your home can be saved! water restoration near me
Thanks for the useful suggestions. Discover more at Afordable Pest Solutions .
I like the valuable information you provide in your articles.
I will bookmark your weblog and check again here regularly.
I’m quite sure I will learn many new stuff right here! Good luck
for the next!
Has anyone had experience with Link building service ? I’m considering their backlink services based on reviews I’ve seen.
The importance of data analytics in digital marketing cannot be overstated. Discover more at Rehan Hasan !
This was nicely structured. Discover more at roofing contractor near me .
Anyone else think that community resources like ### anyKeyword### are essential for keeping our homes safe from water issues? water damage restoration service near me
I found this very interesting. Check out best termite control Long Valley for more.
I have fun with the reminder to avert priceless archives on hand throughout the time of a go. So pretty much omitted! empresa de mudanças
I liked this article. For additional info, visit Hackettstown best pest management .
Thanks for the great explanation. Find more at Vedder Roofing & Construction .
Great conversations happening around home improvement projects—let’s keep sharing what we’ve learned from sites like this one: ### anykeyword###!! roofers in San Diego
Appreciate the comprehensive insights. For more, visit ماساژ ماهور .
Your tricks are spot-on concerning retaining things organized in the course of a cross—thank you most! Explore extra at mudança em sorocaba !
Your blog is helping alleviate my nervousness about my upcoming stream—thank you tremendously! Visit mudanças em sorocaba for even extra assist!
Thanks for the useful suggestions. Discover more at car key locksmith .
Impressive overview of submit-processing drone photos! Editing can substitute all the pieces. Discover extra procedures at http://set.ua/bitrix/rk.php?goto=https://www.giantbomb.com/profile/stubbadavu/ .
I enjoyed this article. Check out Somers Plumbers – Phoenix Plumbing Company for more.
Very useful post. For similar content, visit ادمین اینستاگرام .
I’m impressed with the community engagement you encourage at Buy Suppressors & Gun Silencers Online . It’s important to foster responsible discussions.
This was a fantastic read. Check out ادمین اینستاگرام for more.
The FAQs section at Arms & Ammunition Dealers is a great resource for anyone looking to learn more about gun laws.
How do you take care of your Gibson Les Paul? Any maintenance tips would be appreciated! Share ideas at Les Paul Custom Shop .
I’ve visible techniques for 1500 to 2000 PSI for softer woods, yet I’ve had terrific luck with 2500 PSI. You can be informed greater approximately it at https://wakelet.com/wake/RP9E3Lgb4h1y0U6UNff9x .
Thanks for the great information. More at loan agency new orleans .
Cheap ways to top up? Count me in! I need to enhance my characters without spending too much. find discount recharge at ManaBuy
Love how informative this submit is—it simplifies every thing about settling on and setting up safeguard cameras! Security Camera Installation Sanford
Thanks for the valuable article. More at LuxNuro .
Great tips! For more, visit professional water leak services .
This post really opened my eyes to the importance of backlinks! I found a great source at Affordable backlinks .
Thanks for the clear breakdown. Find more at Afordable Pest Solutions .
Thanks for the great tips. Discover more at Emergency pest management Hackettstown .
Helpful suggestions! For more, visit Beverly Hills Dental Group .
This was quite helpful. For more, visit ادمین اینستاگرام .
Thanks for the great explanation. More info at Afordable Pest Solutions .
This was highly educational. For more, visit local my plumber services .
Very useful post. For similar content, visit https://www.plurk.com/p/3hh28a3e0w .
Had such a smooth transaction buying my car through a local dealer; check out their offerings at buy here pay here phoenix $500 down !
Manabuy has made my Genshin Impact leading-ups lots more cost-effective—heavily, why failed to I switch faster? Great provider! secure pay with ManaBuy
Nicely done! Find more at Affordable Pest Solutions .
I enjoyed this read. For more, visit expert plumbing costs .
It’s encouraging to see platforms like Pistol wholesalers & distributors that address both sides of the gun debate thoughtfully.
I had a smooth moving experience thanks to the affordable services listed on Office moving companies Plantation in Pompano Beach.
I like the efforts you have put in this, regards for all the great content.
This was a fantastic read. Check out plumbing companies near me for more.
Well done! Find more at local gas plumbers .
Thanks for the clear breakdown. More info at LuxNeuro .
My experience finding a roofer using atlas roofers was seamless! Highly recommended for anyone needing help.
This is very insightful. Check out ادمین اینستاگرام for more.
I found this very interesting. For more, visit urgent oral care Beverly Hills .
Thank you for sharing those worthy insights! It’s fresh to work out a focal point on awareness puppy conduct. I put forward vacationing https://www.yankee-bookmarkings.win/the-payment-of-puppy-coaching-camp-can-differ-commonly-relying-on-factors-like-place-period for even extra extensive recommendation!
Great discussion regarding chatbot implementation within websites — they enhance user navigation and assistance significantly ! Discover chatbot platforms through ### anyKeyWord### . Rehan Hasan
Helpful suggestions! For more, visit ادمین اینستاگرام .
This is very insightful. Check out Afordable Pest Solutions for more.
The resources for understanding different types of firearms at Authorized and Licensed firearms and Air Guns Dealers are invaluable for enthusiasts.
This was quite informative. For more, visit locksmith winston salem nc .
I enjoyed this post. For additional info, visit urgent plumber .
This was quite informative. More at Brooks & Baez .
Tankless water heaters are fantastic! My plumber explained everything during the installation process.
Great article jam-packed with elementary shifting hints and hints! Don’t pass over vacationing empresa de mudanças for extra insights!
The reviews on this site helped me choose my mover in Hawthorne! Highly recommend checking it out: Hawthorne apartment movers .
If you desire a quickly manner to peak up Genshin crystals, I’ve heard that ManaBuy discount recharge is valued at testing!
The neck on a Les Paul feels so smooth; it’s perfect for solos! What’s your favorite solo to play? Discuss at Vintage Les Paul Guitars .
Hello, yup this article is really good and I have learned lot
of things from it regarding blogging. thanks.
Thanks for the valuable article. More at Afordable Pest Solutions .
Organizing offers earlier a pass is so considerable! Check out mudança em sorocaba for extra information and methods.
Appreciate your insights on choosing between DIY actions versus hiring experts—it supports make clear judgements! mudanças em sorocaba
Thanks for the practical tips. More at toilet clog fix .
Hi there everyone, it’s my first go to see at this web
page, and piece of writing is truly fruitful in favor of me, keep
up posting these articles or reviews. http://www.gz-jj.com/comment/html/?566314.html
Hi there everyone, it’s my first go to see at this web page,
and piece of writing is truly fruitful in favor of me, keep up
posting these articles or reviews. http://www.gz-jj.com/comment/html/?566314.html
Thanks , I’ve recently been looking for information about
this topic for a while and yours is the
best I’ve found out so far. However, what in regards to
the bottom line? Are you positive concerning the supply? http://dragon-slave.org/comics/ErnestinehfCovertqx
Appreciate the great suggestions. For more, visit ادمین اینستاگرام .
Anyone considering a new roof should definitely reach out to an Escondido roofer from roofer near me .
Thanks , I’ve recently been looking for information about this
topic for a while and yours is the best I’ve found out so far.
However, what in regards to the bottom line? Are you positive concerning the
supply? http://dragon-slave.org/comics/ErnestinehfCovertqx
“Thanks, everyone, for sharing your recommendations! Can’t wait to contact some local ###RooferInSanDiego### next week.” roofers near me
I appreciated this post. Check out https://pointy-staircase-1b3.notion.site/The-Importance-of-Expert-Drainpipe-Cleansing-and-Heating-Solutions-22e60295952f8093a04fd80f9956d9fe?source=copy_link for more.
I’ve been in search of low in cost tactics to recharge Genshin crystals, and your recommendation for Manabuy sounds promising! I’ll deliver it a shot. ManaBuy UID top-up
Fantastic article! I love the way you emphasised security whilst flying drones. For more insights, consult with http://neurostar.com/en/redirect.php?url=https://rapid-wiki.win/index.php/**Drone_Photography_one_hundred_and_one:_Common_Mistakes_to_Avoid_for_Clearer,_Sharper_Images** .
I’m grateful for the contributions made by various authors featured on your site; they bring unique insights to discussions about guns. Stallion Guns
If you need a reliable vehicle fast, consider buy here pay here options in Phoenix! More info at buy here pay here phoenix $500 down .
Your commitment to firearm safety education at guns for sale is commendable! Keep spreading awareness.
Your post about integrating online and offline marketing strategies was very informative—thanks for sharing! More info available at Rehan Hasan !
I could talk about the Les Paul for hours! What makes it special for you? Join the discussion at Les Paul Weight Relief .
This was very enlightening. More at Brain Mapping Treatment Denver .
This post is invaluable. When can I find out more?
Anyone here ever had any doubts about their roofs? Definitely look into consultations booked through ###ANYKEYWORD#### —they set everything straight! atlas roofing
پروتئین وی اتمیک ناکلیر نوتریشن، یک مکمل پودری است که به راحتی در مایعات حل میشود و به شما کمک میکند تا پروتئین باکیفیت به رژیم غذاییتان اضافه کنید.
Thanks for the great tips. Discover more at Beverly Hills immediate urgent dental services .
Appreciate the comprehensive advice. For more, visit ادمین اینستاگرام .
Thanks for the valuable insights. More at Budd Lake pest management experts .
Love the way you spotlight company before a move! For greater insights, confirm to review out empresa de mudanças .
Water heater installations can be daunting, but with an expert ### anyKeyword ### by your side, it’s stress-free. drain cleaning
Who wouldn’t want a smart and cheap way to top up? I’m definitely interested in your approach! ManaBuy Welkin Moon
Helpful suggestions! For more, visit pest management solutions Flanders .
I love the conception of because of colour-coded labels for varied rooms. It simplifies unpacking! mudança em sorocaba
I under no circumstances notion about the importance of labeling containers until eventually my ultimate go! Very appropriate assistance. mudanças em sorocaba
This was very beneficial. For more, visit LuxNuro .
Great insights! Find more at ادمین اینستاگرام .
I will right away snatch your rss as I can not to find your e-mail subscription link or e-newsletter service. Do you have any? Kindly allow me recognise in order that I could subscribe. Thanks.
Knowing about the $5000 AC Rule has changed my perspective on home repairs! Definitely looking into local options like ac repair Las Cruces NM now. affordable air conditioner repair near me
This is very insightful. Check out Broken pipe for more.
I love how Sports Air Guns, Airgun manufacturers, suppliers & exporters promotes a balanced view on gun rights and responsibilities. Well done!
Appreciate the thorough write-up. Find more at ادمین اینستاگرام .
Well done! Discover more at urgent tooth extraction Beverly Hills .
I appreciate how friendly and knowledgeable the staff at jcis roofing are!
Appreciation goes far beyond words alone—it’s wonderful seeing communities grow stronger alongside each other thanks largely due diligence put forth over time through networks formed surrounding resources like : ### roofers
I appreciate any insights on saving money while playing Genshin Impact. Let’s hear it! ManaBuy Welkin Moon
Appreciate the comprehensive advice. For more, visit https://www.mediafire.com/file/qxgj6juzm8rfaoo/pdf-35714-82807.pdf/file .
This was quite helpful. For more, visit Affordable Pest Solutions .
I found this very helpful. For additional info, visit quick plumber response .
Thanks for the comprehensive read. Find more at ماساژ ماهور .
Appreciate the thorough insights. For more, visit Sewer line repair near me .
The tips for maintaining firearms shared at firearms accessories for any gun or rifle are practical and easy to follow.
This was a fantastic read. Check out Afordable Pest Solutions for more.
If you’re considering a move, don’t hesitate to reach out to Wilmer moving company for quotes! Wilmer Mover’s
For anyone unsure about which Santa Ana auto transport company to choose, head over to Santa Ana car shipping for insights.
This was highly useful. For more, visit https://www.mediafire.com/file/818qbzcuirvld3m/pdf-75550-69049.pdf/file .
Thanks for the detailed guidance. More at ادمین اینستاگرام .
This was very well put together. Discover more at ادمین اینستاگرام .
Can we take a moment to appreciate how beautiful these guitars look under stage lights?! What’s your stage setup like? Show us over at Les Paul Fretboard Radius !
I love this theme! Water is the sort of beneficial aid, and realizing what number gallons in line with minute I really want will lend a hand me use it accurately. Keep up the nice paintings! https://www.symbaloo.com/mix/bookmarks-olb0
Thanks for the great explanation. More info at indoor air quality testing .
I liked this article. For additional info, visit local animal hospital .
Useful advice! For more, visit expert septic tank service near me .
Nicely done! Discover more at local physical therapy .
Great points! If you’re looking to buy backlinks online, definitely check out Buy backlinks for niche sites and blogs !
This was a great article. Check out car rental toronto for more.
I love the emphasis on social media marketing in your post. It’s essential for brand visibility. Visit Rehan Hasan for more strategies!
Genshin Impact can be expensive, but I’m intrigued by your approach. Let’s hear it! best prices for Welkin Moon ManaBuy
This was highly useful. For more, visit Leak detection .
This was highly educational. For more, visit mold remediation lake forest wa .
I enjoyed this article. Check out car accident doctor Boise ID for more.
Thanks for the thorough analysis. Find more at ادمین اینستاگرام .
Envision Low Voltage appears like a secure business enterprise; I’ll be achieving out rapidly for charges! CCTV Installation
Valuable information! Find more at knee pain relief service .
Thanks for the detailed guidance. More at brain mapping treatment specialists in Denver .
Your focus on youth education about guns and safety is so necessary, especially through platforms like Shooting, Hunting, & Outdoor Products .
This is highly informative. Check out expert plumbing and heating for more.
Thanks for the comprehensive read. Find more at local affordable plumbing and heating .
This was very enlightening. For more, visit immediate dental care 24 hours .
I continuously put out of your mind approximately utilities when transferring; your info helped me understand all the pieces I need to do! empresa de mudanças
I found your article on self-defense laws at Imported Pistols to be very informative and timely!
The tonewoods used in Gibson Les Pauls really contribute to their unique sound profile! Which woods do you prefer? Discuss at Vintage Les Paul Guitars .
I appreciate any insights on saving money while playing Genshin Impact. Let’s hear it! safe and secure top-up on ManaBuy
Helpful suggestions! For more, visit ماساژ ماهور .
Thanks for the informative post. More at Affordible Pest Solutions .
پروتئین وی پرو کور فا، یک مکمل خوشطعم و باکیفیت است که حاوی ۱۰۰٪ پروتئین وی کنسانتره (Whey Concentrate) میباشد.
The principle of building an stock list is genius—I wish I had finished that during my closing cross! mudança em sorocaba
Found my perfect vehicle thanks to a nearby buy here pay here dealership—check them out at buy here pay here phoenix $500 down !
Appreciate the comprehensive advice. For more, visit https://maps.app.goo.gl/K441zzMQVqukfBgV6 .
This publish is a super resource for brand spanking new puppy owners! I actual understand the sensible assistance you’ve equipped. For similarly reading, go to https://www.bright-bookmarks.win/the-rate-of-canine-education-camp-can-vary-largely-based-on-explanations-like-region-duration .
Loved your insights on minimizing moving expenses although putting forward security—very lifelike recommendation! mudanças em sorocaba
การบริการลูกค้าของร้านเหล้าสาย1 ทำให้รู้สึกพิเศษจริงๆ ครับ ร้านอาหารสาย1 อร่อย
How important is it to research a breed’s characteristics earlier adopting or buying a dog? Let’s chat approximately this topic! https://papaly.com/4/wc1m
Very useful post. For similar content, visit emergency plumbing services .
This was very enlightening. For more, visit plumbing services .
Thanks for the insightful write-up. More like this at Thermostats Gas valves .
This was a fantastic read. Check out Afordable Pest Solutions for more.
Your article is so helpful! I’m definitely going to explore the services offered by Buy backlinks with high domain authority for my SEO strategy.
Thanks for the detailed guidance. More at ادمین اینستاگرام .
This was highly educational. For more, visit auto repair Buckley .
Well done! Discover more at LuxNeuro .
Love seeing such thorough exploration concerning this elementary subject matter—it in actuality encourages knowledgeable determination-making!!! # #anythingKeywords ## https://romeo-wiki.win/index.php/**How_to_Safely_and_Securely_Mount_Your_Security_Camera_in_High_Places**
The importance of community engagement in online branding can’t be overstated—thanks for this info! Discover more at Rehan Hasan !
This was a fantastic read. Check out Dental Group of Beverly Hills for more.
Appreciate the detailed post. Find more at ماساژ ماهور .
What are your options on by using exhausting water versus gentle water whilst operating energy washers?? Any guidelines?? # # anyK eyword ## https://www.plurk.com/p/3hh7yjs7h0
This was quite helpful. For more, visit Budd Lake Bug Control .
Its like you learn my mind! You appear to know a lot about this, like you
wrote the e book in it or something. I believe that you just
can do with a few % to power the message home a little bit, however other than that, that is great blog.
A great read. I’ll definitely be back.
I’m tired of overspending on in-game currency. I’d love to know your method! how to quick recharge at ManaBuy
Your breakdown of state-by-state regulations at Imported Pistols is a much-needed guide for gun owners.
Thanks for the informative content. More at ادمین اینستاگرام .
Thanks for the practical tips. More at Afordable Pest Solutions .
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
Your blog is packed with priceless files that each and every aspiring drone photographer should study—thank you for sharing all these pointers and hints, can’t wait to explore in addition assets awarded by way of traveling http://tudositok.hu/redirect.php?ad_id=10000033&ad_url=https://mike-wiki.win/index.php/**Exploring_Scenic_Landscapes:_How_to_Use_a_Drone_Camera_for_Breathtaking_Travel_Photos** !
Such an gentle-to-stick with advisor, I’m certain I’ll see fabulous effects after following your innovations!! https://wiki-legion.win/index.php/From_Grimy_to_Gleaming:_Cleaning_Your_Sidewalk_Without_Pressure_Washing
Your packing hacks are useful—I can’t wait to strive them out subsequent time I relocate! empresa de mudanças
Useful advice! For more, visit ماساژ ماهور .
Love how you spotlight group prior to a circulate! For greater insights, be sure to test out mudança em sorocaba .
I’ve had my share of HVAC issues in Springfield, MO, and finding a trustworthy repair service made all the difference. It’s crucial to choose a company that knows the local climate and can provide prompt service. hvac companies
The quest for affordable in-game currency is real! Share your wisdom with us please! cheap Primogem packs at ManaBuy
I appreciate how accessible mental health care is in New York City, especially around Grand Central station! Explore your options at psychiatrists Brooklyn .
Thanks for the useful post. More like this at Immersion Heaters Cylinders .
Your weblog has been splendid advantageous as I arrange to transport! For even more recommendations, consult with mudanças em sorocaba right now!
Does anyone else feel inspired just by looking at a Gibson Les Paul? It’s truly an art piece! Share what inspires you over at Les Paul Joe Perry Signature !
This article is a should-learn for all of us seeking to retailer on their water invoice. Understanding what number of gallons consistent with minute you actually need can lead to extraordinary mark downs! https://www.livebinders.com/b/3662228?tabid=1e4577db-b9a0-deed-c9d6-92a36038990a
Great job! Find more at ادمین اینستاگرام .
Thanks for the clear advice. More at https://pastelink.net/y8pusf6l .
Great job! Find more at Divorce Lawyer services Richmond VA .
This is quite enlightening. Check out https://andersonamox092.lowescouponn.com/finding-trustworthy-citizen-plumbers-in-your-area for more.
This was a wonderful guide. Check out instant payday loans new orleans for more.
Dogs have a particular means of creating day-after-day believe brighter! How does your doggy deliver pleasure into your lifestyles? Tell us on https://wiki-burner.win/index.php/Famous_Dogs_in_History_and_Pop_Culture_You_Should_Know_About !
I don’t even understand how I stopped up right here, but I believed this put up was once good.
I don’t know who you are however certainly you are
going to a famous blogger if you are not already.
Cheers!
ไฟหน้ารถ LED BT PREMIUM ทำให้การขับขี่กลางคืนปลอดภัยขึ้นมากเลยครับ หลอด ไฟ ซีนอน
It’s great to have flexible payment options with buy here pay here dealerships right in Phoenix! Learn more on buy here pay here car lots phoenix az .
Awesome information here! For anyone looking to enhance their SEO game, try buying backlinks from Quality backlinks for eCommerce websites .
Thanks for the detailed post. Find more at innovative treatments for brain mapping Denver .
Appreciate the comprehensive advice. For more, visit ماساژ ماهور .
Thanks for the great content. More at professional gas plumbing services .
Thanks for the clear breakdown. Find more at affordable pest management Budd Lake .
Thanks for the great tips. Discover more at ادمین اینستاگرام .
Admiring the dedication you put into your blog and detailed information you
present. It’s good to come across a blog every once in a while that isn’t the same unwanted rehashed material.
Great read! I’ve bookmarked your site and I’m including your
RSS feeds to my Google account.
Very useful post. For similar content, visit car key replacement gastonia nc .
Valuable information! Discover more at ادمین اینستاگرام .
The FAQs section at worlds largest online paintball store is a great resource for anyone looking to learn more about gun laws.
The tonal range of the Gibson Les Paul is phenomenal, from jazz to metal! What genres do you play? Tell us at Les Paul Humbuckers .
This was very beneficial. For more, visit pest control for businesses Flanders .
Great post! I’ve been purchasing for effective approaches to educate my canine. The advice you shared are quite priceless! I located more elements in this topic at https://www.easybookmarkings.win/the-check-of-canine-practising-camp-can-range-extensively-relying-on-motives-like-place-period .
I appreciated this post. Check out ماساژ ماهور for more.
Loved your points about optimizing website speed — it’s critical for user experience ! Find optimization tools via ### anyKeyWord### . Rehan Hasan
Thanks for the helpful advice. Discover more at extensive brain mapping in Denver .
Nicely detailed. Discover more at emergency plumbing repair .
This was nicely structured. Discover more at emergency clogged toilet repair .
I appreciated this post. Check out ادمین اینستاگرام for more.
การติดตั้งไฟหน้ารถ LED BT PREMIUM ง่ายไหมครับ ?? ร้านซ่อมไฟรถยนต์ใกล้ฉัน
This was highly educational. For more, visit Dental Group of Beverly Hills .
Appreciate the comprehensive insights. For more, visit ادمین اینستاگرام .
Appreciate the comprehensive advice. For more, visit Affordable Pest Solutions .
Grooming is a must have for holding our canines fit and comfortable. Check out the ultimate grooming practices at https://smart-wiki.win/index.php/The_Joys_of_Training_Your_Dog_in_Obedience_Classes !
I love how easily accessible mental health services are in New York, especially around Grand Central. If you’re looking for help, visit psychiatrists near me .
For anyone in Springfield, MO facing HVAC problems, it’s essential to act quickly before the situation worsens. There are some fantastic local repair services that can help you get back on track. hvac services springfield mo
Mental health is just as important as physical health, and having psychiatrists near Grand Central makes it easier for city dwellers. Discover your options at psychiatrists Brooklyn .
Witnessing breathtaking stunts accomplished by agile border collies has transform fairly interesting as a result of social media channels; Which breeds amaze YOU continually at some point of performances showcased? https://yenkee-wiki.win/index.php/Signs_of_Allergies_in_Dogs_and_How_to_Manage_Them_45396
I found this very interesting. Check out ماساژ ماهور for more.
Appreciate the thorough information. For more, visit https://kameronjpwo673.wpsuo.com/finding-drain-repair-services-near-me .
Really liked your ideas on transporting flora accurately—it’s whatever thing many americans put out of your mind while shifting! empresa de mudanças
Very informative article. For similar content, visit https://raymondodbq703.cavandoragh.org/schedule-your-wheel-alignment-in-bonney-lake-today-6 .
This is very insightful. Check out locksmith services winston-salem nc for more.
Organizing prior to a movement is key! I determined a few exact materials at mudança em sorocaba that helped me streamline my process.
The importance of mental health awareness in relation to firearm ownership highlighted on Guns: Pistols, Rifles, Shotguns & More is vital!
Great pointers on through drone cameras! I never knew approximately the magnitude of balancing the gimbal. Check out greater at http://gamesjp.com/jump.php?url=https://wiki-square.win/index.php/**Drone_Photography_a_hundred_and_one:_Common_Mistakes_to_Avoid_for_Clearer,_Sharper_Images** .
Thank you for highlighting the value of making a moving timeline—I’ll undoubtedly use that next time! mudanças em sorocaba
Buenas, Pablito! ¿Cómo te encuentras hoy? Te quiero
hablar de un casino virtual que es perfecto para jugadores como tú.
Este casino tiene una oferta increíble de juegos y una navegación muy fluida.
Si prefieres las slots, quedarás asombrado con los juegos de
slots variados. Además, el casino tiene juegos de mesa populares.
Lo que más me gusta de este casino online es que tienen opciones de pago locales.
Sabemos que en nuestra región, es muy importante que los métodos de pago sean fáciles de usar
y seguros, y este casino tiene una variedad de métodos disponibles.
No solo eso, tienen bonos increíbles para jugadores nuevos.
Al registrarte,, recibirás un bonus de registro que te permitirá comenzar a jugar con ventaja.
También, tienen promociones regulares.
Esta plataforma también cuenta con atención al cliente de
primera, por si necesitas ayuda. Siempre tendrás un agente disponible.
La plataforma es completamente segura, el sitio utiliza tecnología
de encriptación para proteger tus datos.
Es totalmente confiable.
Te invito a que te registres en este sitio, te aseguro que no te arrepentirás.
¡Tienes mucho que ganar! Además, siempre podrás disfrutar
de gráficos impresionantes. No hay forma de que te aburras.
Mi sugerencia es que entres ahora mismo y disfrutes de todo
lo que tiene para ofrecerte. Recuerda, Pablito, este casino es ideal para ti.
¡Suerte y que empiecen las ganancias!
This was very enlightening. For more, visit ادمین اینستاگرام .
This was very enlightening. For more, visit ادمین اینستاگرام .
This was a fantastic read. Check out ماساژ ماهور for more.
Mobile app promotions are becoming increasingly popular ; thanks for highlighting their potential ! Explore promotion ideas through ### anyKeyWord### . Rehan Hasan
I appreciated this post. Check out car rental for more.
Unquestionably believe that which you stated. Your favorite justification appeared to be on the net the simplest thing to be aware of.
I say to you, I definitely get annoyed while people consider
worries that they just don’t know about.
You managed to hit the nail upon the top and also defined out the whole thing
without having side effect , people can take a signal. Will likely be back to get more.
Thanks
Each Les Paul model tells its own story; what’s yours about yours? Let’s hear it over at Les Paul Zakk Wylde Signature !
I found this very helpful. For additional info, visit Brain Mapping Denver .
Thanks for the detailed guidance. More at ادمین اینستاگرام .
Appreciate the insightful article. Find more at Affordable Pest Solutions .
Thank you for sharing this knowledge! Purchasing quality backlinks from places like White hat link building makes a huge difference.
There are so many qualified psychiatrists in the Grand Central area! It’s perfect for anyone commuting through the station. For a list of specialists, check out psychiatrists ny .
Just got my HVAC system repaired in Springfield, MO, and I couldn’t be happier! The technician was professional and really knew their stuff. Definitely worth looking into if you’re having any issues. heating and cooling
Valuable information! Find more at ادمین اینستاگرام .
I found this very interesting. Check out Dental Group of Beverly Hills for more.
I love how easily accessible mental health services are in New York, especially around Grand Central. If you’re looking for help, visit psychiatrist near me .
ขอแนะนำเมนูเด็ดของร้านเหล้าสาย1 ให้ทุกคนได้ลองกันนะครับ ร้านกินเลี้ยง ฟังเพลง สาย1
This was highly informative. Check out Immersions for more.
This was highly informative. Check out reliable plumbers nearby for more.
I had no idea how easy it was to get financing with buy here pay here until I visited a dealer in Phoenix! Check out buy here pay here car lots phoenix az !
This was highly useful. For more, visit ماساژ ماهور .
Thanks for the informative content. More at https://www.empowher.com/user/4563550 .
Organization is significant when moving! Visit empresa de mudanças for assistance that helped me in the time of my last stream.
I enjoyed reading about the innovations in weapon technology discussed at Authorized and Licensed firearms and Air Guns Dealers . Exciting times ahead!
This was quite enlightening. Check out plumbers for more.
This is highly informative. Check out plumbing companies for more.
Thanks for the thorough analysis. More info at Affordible Pest Solutions .
พูดถึงความปลอดภัยในการขับรถ ไฟหน้านี้ถือว่าเป็นสิ่งสำคัญที่สุด ### ไฟหน้า led
This was a great article. Check out LuxeNeuro for more.
Your blog has been exceptional invaluable as I practice to head! For even more tips, go to mudança em sorocaba at this time!
Clearly presented. Discover more at ادمین اینستاگرام .
Does anyone else feel inspired just by looking at a Gibson Les Paul? It’s truly an art piece! Share what inspires you over at Les Paul Quilt Maple !
The emphasis on cautious making plans enormously resonates with me as I practice to relocate—enormous process right here! Be definite to discover what’s at mudanças em sorocaba #!
Great insights on the challenges faced by Bulk Ammunition, Gun Parts, & More! ! It’s crucial to understand the regulations involved in the industry.
I liked this article. For additional info, visit Afordable Pest Solutions .
Thanks for the thorough analysis. Find more at ماساژ ماهور .
The mental health resources available in the Grand Central area are impressive! If you need guidance, check out psychiatrist near me for some great psychiatrist listings.
I’ve heard that psychiatrists near Grand Central offer flexible hours for busy professionals. It’s great to have mental health support right in the heart of the city! Visit psychiatrist NYC to learn more.
Such an informative post! Quality links are a game-changer, and I’ll be exploring Best place to buy backlinks for my needs.
This was very beneficial. For more, visit Dental Group Beverly Hills .
Valuable information! Discover more at kitchen and bathroom taps .
This post makes me want to try out on-site auto repair right now! Sounds amazing! Modesto mobile mechanic services
A force washer with around 2000-2500 PSI is good for so much decks. Just take note to hinder the nozzle at a protected distance! For more guidelines, see https://www.foxtrot-bookmarks.win/to-effectually-sparkling-a-deck-a-rigidity-washing-machine-with-a-psi-quantity-of-2500-to-3000-is-perfect .
Have any funny pet fails or mishaps came about in the course of training periods along with your furry good friend? Let’s share stories over ### anykeyword ### Discover more
Taking side in charity runs/pursuits helping corporations assisting neglected animals conjures up involvement really with no query–Which reasons resonate strongest in my view motivating traders looking for chances combined FUN & WORK concurrently https://aged-wiki.win/index.php/Dogs_as_Family_Members:_The_Benefits_They_Bring_to_Our_Lives
This was very enlightening. More at ادمین اینستاگرام .
Excited about sharing what I’ve learned here with company—they’ll indubitably profit from figuring out more about pressures used with ease!!!! # https://www.plurk.com/p/3hh7yjs7h0
Appreciate the insightful article. Find more at seguros de viajes .
Do any of your buddies or family members have puppies too, growing just a little % whilst getting collectively? Share community adventures over on https://research-wiki.win/index.php/Preparing_Your_Pet_for_Emergencies:_A_Safety_Checklist
Valuable information! Discover more at Pest Control Flanders .
Appreciate the comprehensive advice. For more, visit ادمین اینستاگرام .
I appreciate your breakdown of various digital marketing channels! So informative! Discover more at Rehan Hasan !
Thanks for the great explanation. More info at ماساژ ماهور .
Very helpful read. For similar content, visit local plumber near me .
Moreno Valley has some amazing on-site auto repair options! Check them out at brake repair mobile service Moreno Valley .
Thanks for the great explanation. More info at Kitchen plumbing .
Heya i am for the first time here. I found this board and I find It truly
helpful & it helped me out much. I’m hoping to offer one thing back and aid others like you aided me.
Thank you for providing a platform that encourages responsible discussions about firearms and their use, such as seen on Bulk Ammunition, Gun Parts, & More! .
Thanks for the great explanation. More info at Emergency plumbing .
Really appreciate how helpful they were throughout all steps @ anykeyword! https://www.gamespot.com/profile/cyrinappks/
The market trends discussed at Authorized and Licensed firearms and Air Guns Dealers are fascinating! It’s interesting to see how consumer preferences evolve.
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
Love the emphasis on successful reinforcement! It makes this sort of big difference in exercise. If you are eager about extra info, talk over with https://www.stall-bookmarks.win/the-settlement-of-canine-education-camp-can-differ-extensively-depending-on-elements-like-position-period for additional materials!
Well explained. Discover more at loan agency new orleans .
I highly recommend exploring buy here pay here dealerships in Phoenix for great deals! Find out more at buy here pay here phoenix az .
I enjoyed this read. For more, visit LuxeNeuro .
I enjoyed this post. For additional info, visit ادمین اینستاگرام .
Very helpful read. For similar content, visit professional clogged shower drain .
This was a wonderful guide. Check out seguros de viajes for more.
Appreciate the thorough insights. For more, visit Afordable Pest Solutions .
This was a wonderful post. Check out ماساژ ماهور for more.
Today, I went to the beach with my children. I found a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and
screamed. There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is completely off topic but I
had to tell someone!
This was very enlightening. More at professional immediate dental services .
This post makes me want to try out on-site auto repair right now! Sounds amazing! Modesto mobile mechanic services
The value of retaining remarkable contacts useful for the duration of a cross is not going to be overstated—excellent reminder! empresa de mudanças
Thanks for sharing these tips on buying backlinks; I’m definitely checking out Best link building service 2025 !
Clearly presented. Discover more at ادمین اینستاگرام .
The magnitude of preserving relevant contacts accessible throughout the time of a circulation should not be overstated—nice reminder! mudança em sorocaba
Remarkable! Its truly remarkable article, I
have got much clear idea about from this paragraph.
Content repurposing is a smart strategy for maximizing reach—thanks for highlighting that! Learn more at Rehan Hasan !
The conception of creating an inventory listing is genius—I desire I had performed that in my closing stream! mudanças em sorocaba
Thanks for the great tips. Discover more at Afordable Pest Solutions .
This guide become fairly insightful and has already extended my drone flying potential noticeably; shopping ahead to making use of what I’ve learned the following and from other resources like the ones to be had at http://www.memememo.com/link.php?url=https://www.honkaistarrail.wiki/index.php?title=**Drone_Photography_one_hundred_and_one:_Common_Mistakes_to_Avoid_for_Clearer,_Sharper_Images** !
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at Shooting, Hunting, & Outdoor Products !
Thanks for the clear advice. More at top pest control Budd Lake .
This was very beneficial. For more, visit ماساژ ماهور .
I will right away take hold of your rss as I can’t find your e-mail subscription link or e-newsletter service. Do you’ve any? Kindly let me recognize in order that I may just subscribe. Thanks.
Has anyone tried on-site auto repair in Moreno Valley? I found some great options at mobile auto repair Moreno Valley CA !
This was a wonderful guide. Check out Beverly Hills Dental Group for more.
I invariably idea extra GPM changed into higher, yet now I have an understanding of that it relies on the venture to hand. This post has opened my eyes to the magnitude of matching move rates with demands. https://www.third-bookmarks.win/to-adequately-refreshing-a-deck-a-strain-washing-machine-with-a-psi-range-of-2500-to-3000-is-perfect
Grooming is important for preserving our canine suit and comfortable. Check out the choicest grooming practices at https://extra-wiki.win/index.php/Seasonal_Care_for_Dogs:_Keeping_Your_Pup_Safe_Year-Round !
I’ve been that means to improve my protection approach, and your blog became simply what I needed to get began!! https://mighty-wiki.win/index.php/**Mounting_Indoor_vs._Outdoor_Security_Cameras:_What_You_Need_to_Know**
Appreciate this thorough analysis on buying links; I’m eager to see what’s available at Dofollow backlinks for sale now!
Well done! Find more at ادمین اینستاگرام .
I enjoyed this post. For additional info, visit quick shower drain unclogging .
Appreciate the thorough write-up. Find more at same day plumbing repairs .
Appreciate the detailed post. Find more at ادمین اینستاگرام .
Buenas, Pablito! ¿Cómo te encuentras hoy? Tengo una excelente recomendación para
ti un casino en línea que no puedes dejar de probar.
La plataforma tiene una oferta increíble de juegos y una navegación muy
fluida.
Si eres fan de los juegos de azar como las tragamonedas, te sorprenderán con los
juegos de slots variados. Incluso, el sitio tiene todos los juegos de
mesa que puedes imaginar.
Una de las mejores cosas de este casino online es que tienen opciones
de pago locales. En nuestra parte del mundo, es muy importante que
los métodos de pago sean fáciles de usar y seguros, y este casino tiene un sistema de
pagos rápido y seguro.
Por si fuera poco, tienen ofertas que no puedes dejar pasar para jugadores
nuevos. Al registrarte,, recibirás un regalo para nuevos jugadores que te permitirá comenzar a
jugar con ventaja. Y por si fuera poco, tienen torneos con grandes premios.
La web también cuenta con un equipo de soporte disponible todo
el tiempo, por si necesitas ayuda. La atención es de calidad
y te guiarán en todo momento.
La plataforma es completamente segura, el sitio utiliza encriptación de última generación para proteger tus datos.
No tendrás que preocuparte por nada.
Si decides probar este sitio, te aseguro que no te arrepentirás.
¡Es tu oportunidad de hacer crecer tu dinero!
Además, siempre podrás disfrutar de una experiencia de juego sin igual.
Cada juego es una nueva oportunidad.
Mi sugerencia es que entres ahora mismo y disfrutes de todo lo que tiene para ofrecerte.
Ya sabes, Pablito, te garantizo que disfrutarás mucho.
¡Suerte y que empiecen las ganancias!
Great job! Discover more at ماساژ ماهور .
Appreciate the comprehensive insights. For more, visit seguros viajes .
Great data on residential actions! I forever uncover that making plans beforehand makes a good sized difference. empresa de mudanças
This was very enlightening. For more, visit https://griffincbyy556.trexgame.net/top-7-signs-your-car-needs-brake-repair-in-bonney-lake-10 .
Thanks for the clear breakdown. Find more at tap servicing .
Great article crammed with critical relocating tricks and tips! Don’t pass over visiting mudança em sorocaba for added insights!
I love how you emphasized defense while lifting heavy furniture—splendid reminder for absolutely everyone! mudanças em sorocaba
Training may be a obstacle, yet your doorstep-with the aid of-step method makes it look plausible! I’ll completely be trying out Visit this link for greater lessons hints.
Appreciate the comprehensive advice. For more, visit nc .
Appreciate the thorough analysis. For more, visit http://www.siteglimpse.com/external/ext.aspx?url=https://hurqalya.org/member.php?action=profile&uid=162138 .
This was very beneficial. For more, visit Central heating installations .
Recently got my windshield tinted by #AnyKeyWord#, and it looks fantastic! Great service too. https://www.cheaperseeker.com/u/galairidce
This was quite useful. For more, visit ادمین اینستاگرام .
Thanks for the insightful write-up. More like this at ماساژ ماهور .
Highly recommend checking out the inventory at local buy here pay here dealerships in Phoenix! Visit buy here pay here phoenix az .
Great insights! Find more at plumber around me .
Have determined individual eco-friendly brands featuring sustainable merchandise geared in opposition to pampering doggies lately?! Let’s examine environmentally mindful possibilities a possibility this day mutually! https://romeo-wiki.win/index.php/The_Science_Behind_Why_Dogs_Love_Us_So_Much
Great job! Find more at plumber cost .
I appreciated this post. Check out seguros de viaje baratos for more.
Excellent points made regarding the importance of engaging headlines in blogs ! They truly drive clicks . Check out headline formulas from ### anyKeyWord### . Rehan Hasan
This was very enlightening. For more, visit Heating engineers .
Finally, an answer to my long waits at traditional garages—with onsite repairs, I’ll save so much time! Modesto mobile mechanic services
This was a wonderful post. Check out ادمین اینستاگرام for more.
Dogs have an incredible capability to feel our emotions. It’s gorgeous how they could alleviation us whilst we need it maximum! Learn greater at https://speedy-wiki.win/index.php/The_Best_Apps_Every_Dog_Owner_Should_Have .
Great article! Buying backlinks can really boost your site’s visibility. I recommend checking out Backlink seller for some excellent options.
I didn’t realise how outstanding it is to review neighborhood rules in the past flying a drone. Thanks for the recordsdata! Explore greater at http://m.shopinanchorage.com/redirect.aspx?url=https://wiki-cable.win/index.php/**Unlocking_Aerial_Photography:_A_Beginner%27s_Guide_to_Using_Your_Drone_Camera** .
This was highly educational. For more, visit ادمین اینستاگرام .
This was quite informative. For more, visit ماساژ ماهور .
What’s up to all, how is the whole thing, I think every one is getting more from this
website, and your views are nice in favor of new users. https://asp-edo.ru/bitrix/redirect/
Clearly presented. Discover more at https://padlet.com/krawczykcalcote296ukvik/bookmarks-cc0qd5a9n4pyqe4l/wish/kxodWG1kbPyjQgP7 .
What’s up to all, how is the whole thing, I think every one
is getting more from this website, and your views are nice in favor of new users. https://asp-edo.ru/bitrix/redirect/
Excellent goods from you, man. I have understand your stuff previous to and you are just extremely
magnificent. I really like what you’ve acquired here, certainly like what you’re stating and the way in which you
say it. You make it entertaining and you still take care of to keep it smart.
I can’t wait to read far more from you. This is actually a great website.
The discussion around hunting rights and regulations at Buy Suppressors & Gun Silencers Online is informative and well-articulated.
Simply want to say your article is as astonishing.
The clearness in your put up is just spectacular and that i could suppose you
are a professional on this subject. Well with your permission allow me
to clutch your feed to keep up to date with
drawing close post. Thank you a million and please keep up the rewarding
work.
Hi! I realize this is somewhat off-topic however I needed to ask.
Does building a well-established blog like yours take a massive amount work?
I am completely new to writing a blog however I do write
in my journal daily. I’d like to start a blog so I will be able
to share my own experience and feelings online. Please let me
know if you have any kind of ideas or tips for brand new
aspiring bloggers. Thankyou! https://R12Imob.store/index.php?page=user&action=pub_profile&id=415381
I found this very helpful. For additional info, visit ادمین اینستاگرام .
I can’t believe how much time I saved by opting for on-site auto repair! Thanks to Moreno Valley mobile mechanic services !
I enjoyed reading about the innovations in weapon technology discussed at Sports Air Guns, Airgun manufacturers, suppliers & exporters . Exciting times ahead!
Vehicle shipping can be daunting, but with San Antonio auto shipping in San Antonio, it was a breeze! Definitely check them out.
Thanks for reminding us to update our deal with all over the place—it’s one of those things which may quite simply slip our minds! empresa de mudanças
The wholesale appliance options at local appliance store are perfect for anyone remodeling their home!
Such great advice shared here about backlinking safely online! Definitely considering services from Best backlink services for small businesses !
Thanks for the detailed guidance. More at ادمین اینستاگرام .
Email segmentation plays a key role in improving open rates ; such an important topic discussed here ! Dive deeper into segmentation tactics through ### anyKeyWord### . Rehan Hasan
I appreciated this post. Check out ماساژ ماهور for more.
Your emphasis on covering fragile items whilst packing is so appropriate; I’ve made that mistake formerly! mudança em sorocaba
Do you could have any concepts for eco-friendly force washing machine detergents? I want to be more sustainable! https://pixabay.com/users/51304978/
This was very enlightening. More at seguros de viaje baratos .
Your article makes me feel greater arranged for my upcoming circulation—thank you for your complete successful guide! mudanças em sorocaba
Finding an affordable yet reliable Glendale moving company is key to a successful move! Office moving companies Glendale
The best part about buying from a buy here pay here dealership? It’s all local! Check out buy here pay here near me for more info.
Having mechanics come directly to us is such an innovative idea; onsite repairs are the future! emergency mobile mechanic Modesto
Nicely done! Find more at ادمین اینستاگرام .
This was a great article. Check out cheap car hire for more.
This was very enlightening. For more, visit Clogged toilet .
Thanks for the helpful advice. Discover more at reliable checkatrade plumbers .
Can anyone share their experiences with overnight moves for offices in Alachua? Need tips on this! Long distance movers Alachua
Thanks for the clear breakdown. More info at ادمین اینستاگرام .
It’s refreshing to see a site like Authorized and Licensed firearms and Air Guns Dealers that values education over sensationalism in the firearms debate.
It’s appropriate time to make some plans for the future and it is time to be happy. I have read this post and if I could I wish to suggest you few interesting things or suggestions. Perhaps you can write next articles referring to this article. I want to read more things about it!
Appreciate the detailed information. For more, visit ماساژ ماهور .
I found this very helpful. For additional info, visit Water heater repair .
So impressed with how user-friendly the site is! Check out everything about Sunnyvale movers at Sunnyvale movers #.
This is exactly what I’ve been looking for! The Lost Generator sounds like a smart and
affordable way to take control of energy costs. I love that it doesn’t require fancy tools or a tech background—definitely giving
this a try.
It’s perfect time to make some plans for the future
and it is time to be happy. I’ve read this post and if I could I desire to suggest you some interesting things or advice.
Perhaps you can write next articles referring to this article.
I wish to read more things about it!
It’s refreshing to see a site like Shooting, Hunting, & Outdoor Products that values education over sensationalism in the firearms debate.
Very informative! It’s sudden what number of human beings put out of your mind the magnitude of GPM in their day to day lives. I’ll simply be checking my fixtures and appliances now! https://www.social-bookmarkings.win/to-adequately-sparkling-a-deck-a-power-washer-with-a-psi-latitude-of-2500-to-3000-is-right
This was quite useful. For more, visit seguros de viaje baratos .
Moreno Valley has some amazing on-site auto repair options! Check them out at on-site auto repair Moreno Valley .
Every puppy has its own unique persona. What’s your canine’s quirks? Share your memories at https://lima-wiki.win/index.php/How_to_Choose_the_Right_Name_for_Your_New_Puppy !
Training periods would be so profitable, mainly after they examine new hints! What methods has your dog mastered? Share experiences at https://wiki-nest.win/index.php/Building_a_Strong_Bond_with_Your_Rescue_Dog !
This was a wonderful guide. Check out Burst pipes for more.
I appreciated this post. Check out https://privatebin.net/?c2a284fd38d50a07#9QQBuv4NmEF5kHPhdXqNbh8U97gSAR2qGuvvJnRx5a88 for more.
Great put up about the value of company when moving! Check out empresa de mudanças for more very good content!
What a relief it was to hire professionals like those at #(#) anyKeyWord# for our move! Bronx commercial movers
Have discovered myself bonding over playdates prepared among fellow puppy house owners inside group communities —What occasions would be hosted in the community within YOUR area ? https://wiki-burner.win/index.php/Why_Consistency_is_Key_in_Training_Your_Dog_Effectively
Your blog is a goldmine of information! I’ll definitely reach out to Backlinks for sale for backlink services soon!
การเปลี่ยนมาใช้ไฟหน้ารถ LED BT PREMIUM ทำให้รถดูทันสมัยขึ้นครับ ซ่อมไฟหน้ารถยนต์
Wonderful tips! Discover more at ادمین اینستاگرام .
Great insights! Discover more at ماساژ ماهور .
Can everyone percentage their experiences with therapy or carrier canines from distinctive breeds—they’re virtually inspiring! https://wakelet.com/wake/jDHKSI_eXjHlkMpo7cgh9
The significance of conserving fundamental contacts to hand during a cross will not be overstated—incredible reminder! mudanças em sorocaba
This was very enlightening. More at trust a trader plumber .
Thanks for the helpful advice. Discover more at quick cistern syphon solutions .
ร้านเหล้าสาย1 มีบาร์เทนเดอร์ที่เก่งมากเลยนะครับ ร้านเหล้าฟังเพลงสาย1
The key takeaway for successful relocations is planning ahead; find helpful checklists over ###anything### Bellevue full service movers
Clearly presented. Discover more at ادمین اینستاگرام .
I recently used Sinton car shippers for my vehicle transport and was very impressed with their service! Sinton vehicle transport
With so many options available, I’m glad I picked San Antonio car transport # for my last vehicle shipment.
Your thoughts on adapting to mobile-first indexing are highly relevant today—good read! Explore further details at Rehan Hasan !
If you’re looking for a reliable Houston auto shippers in Houston, TX, I highly recommend checking them out for all your vehicle shipping needs!
Very timely guidance as many other people are investing in abode safeguard as of late; thank you for sharing!! check here
There is certainly a great deal to know about this subject.
I like all of the points you made.
Bed bug issues? You’re not alone! Check out what worked for me through Junk hauling .
This put up is a positive resource for new dog householders! I rather appreciate the real looking advice you’ve offered. For additional interpreting, visit https://www.bookmark-fuel.win/the-charge-of-dog-training-camp-can-vary-generally-depending-on-aspects-like-region-length .
Thanks for the comprehensive read. Find more at ماساژ ماهور .
Kudos on overlaying equally technical information and realistic recommendation—it honestly caters good to all audiences!!! ## anykeyword### Home Security Camera Installation
Super easy process with #AnyKeyWord#—from scheduling an appointment to getting the work done on time! https://giphy.com/channel/onovenbbcn
Just accomplished by using my new fuel-powered model, and wow, what continual—it made immediate paintings of my soiled patio!! http://slhair.ru/user/elmarafzdu
This was a wonderful guide. Check out ادمین اینستاگرام for more.
Thanks for shedding light on this topic! I’ve used Backlinks provider to buy backlinks and was very satisfied.
Thanks for the helpful article. More like this at local fall heating installation .
Appreciate the insightful article. Find more at affordable plumbing .
Thanks for the great explanation. More info at payday loans new orleans la .
Thanks for the clear advice. More at phim sex hàn quốc .
“For safe and efficient boiler removal services, trust only professionals like # demolition company near me #.”
Desire exists universally amongst people everywhere wishing always find someone trustworthy capable assisting them journeying through life adventures often unpredictable uncertain challenging daunting yet ultimately rewarding satisfying fulfilling Cheap movers Dundee
The costs seem pretty reasonable for window tinting in Jeffersonville, IN. Can’t wait to get started! Window tinting Jeffersonville Indiana here I come! custom tinting Jeffersonville Indiana
Just sealed the deal on my new-to-me car with a buy here pay here option—so excited! More info at buy here pay here phoenix az no credit check .
Fantastic insights into on-site auto repair services in Modesto—definitely considering it now! auto repair near me Modesto
Thanks for the clear breakdown. More info at ماساژ ماهور .
Wonderful tips! Discover more at ادمین اینستاگرام .
Fantastic breakdown of settings for other video resolutions and body fees on drones – very informative! For extra small print, visit http://seclub.org/main/goto/?url=https://quebeck-wiki.win/index.php/**From_Ground_to_Air:_How_to_Get_Started_with_Your_New_Drone_Camera** .
Appreciate the helpful advice. For more, visit ادمین اینستاگرام .
Knowledge won due to reports shared sparks pleasure—a reminder we’re by no means on my own in our struggles or tasks!!!! ## https://wiki-quicky.win/index.php/Your_Comprehensive_Guide_to_Non-Pressure_Washing_Sidewalk_Maintenance
This blog has some great tips on finding the best Glendale moving company for your needs! Long distance movers Glendale
I love the emphasis on social media marketing in your post. It’s essential for brand visibility. Visit Rehan Hasan for more strategies!
Using robust bins can save a lot hindrance all through transport! Great guidance the following! empresa de mudanças
I’ve heard great things about Winter Haven apartment movers when it comes to commercial moves in Winter Haven. Definitely worth considering!
Trustworthy garage door solutions are hard to find, but garage door repair expert company in San Antonio delivers every time!
If you’re eager about a rigidity washer to your deck, I propose some thing above 2000 PSI. It makes the process such a lot simpler! For distinctive guidelines, head over to https://www.nav-bookmarks.win/to-safely-clean-a-deck-a-pressure-washer-with-a-psi-vary-of-2500-to-3000-is-ideal .
Loved my recent experience with an onsite mechanic; they were super professional—details here: ###: any keyword###! mobile mechanic near me Moreno Valley
Great tips! For more, visit seguros de viaje baratos .
A big thank you to the talented team at our chosen Bellevue Local movers Bellevue – they exceeded all expectations during our move.
Looking for movers you can trust in St. Augustine? I highly recommend St. Augustine moving companies !
วัสดุของไฟหน้ารถ LED BT PREMIUM แข็งแรงจริงไหม ?? ซ่อมไฟรถยนต์ ใกล้ ฉัน
Great information on residential actions! I consistently uncover that planning forward makes a extensive change. mudança em sorocaba
Dogs have a exotic means of constructing each day experience brighter! How does your domestic dog deliver pleasure into your lifestyles? Tell us on https://romeo-wiki.win/index.php/Barking_Mad!_Why_Do_Some_Breeds_Bark_More_Than_Others%3F !
Thanks for the clear advice. More at plumbers near me .
Each interaction experienced while utilizing resources found via “(mel rose)” resulted positively impacting journey overall-happy exploring possibilities ahead!-visit link ! Melrose apartment movers
This was nicely structured. Discover more at Pumps .
Loved your insights on minimizing transferring charges at the same time as conserving safeguard—very life like counsel! mudanças em sorocaba
Great tips! For more, visit quick 24 hour plumber response .
Thank you for sharing your knowledge! I’m eager to improve my site’s rankings with help from Best backlink services for small businesses .
I have learn several good stuff here. Definitely price bookmarking for revisiting.
I wonder how a lot effort you put to create such a excellent informative site.
Just finished a big ##commercial demolition## project. It was intense but the team made it look easy with their expertise! demolition company near me
This was quite helpful. For more, visit https://keegansxlb076.iamarrows.com/using-pipe-connectors-properly .
What’s up to every , for the reason that I am genuinely keen of reading this
blog’s post to be updated regularly. It consists of pleasant
material. http://Imatranperhokalastajat.net/index.php/component/kide/history/-/index.php?option=com_kide
What’s up to every , for the reason that I am genuinely keen of reading
this blog’s post to be updated regularly. It consists of pleasant material. http://Imatranperhokalastajat.net/index.php/component/kide/history/-/index.php?option=com_kide
Deep-cleaning carpets and fabric could make this kind of big difference in how recent your property feels! Your pointers had been large, and I’ll check out in addition techniques from house cleaning services woodbury, ca .
I appreciate the information about on-site auto repair in Modesto—it sounds perfect for families! on-site auto repair Modesto
So happy I chose a buy here pay here option in Phoenix! Explore your choices at buy here pay here near me .
I enjoyed this read. For more, visit ماساژ ماهور .
Using music or podcasts while cleaning makes the process a lot less tiresome!” Find more enjoyable ways to tidy over at house cleaning service near me .
Great job! Discover more at ادمین اینستاگرام .
Thanks for the clear advice. More at phim sex hay .
Thank you for sharing these beneficial insights! It’s clean to determine a spotlight on working out dog behavior. I advocate touring https://www.bookmarking-planet.win/the-cost-of-canine-workout-camp-can-vary-extensively-relying-on-elements-like-vicinity-length for even more first-rate information!
Your insights into coping with emotional stress for the period of a transfer were very comforting, thank you for sharing that point of view! empresa de mudanças
Thanks for the thorough article. Find more at LuxeNeuro .
When some one searches for his necessary thing, so he/she desires
to be available that in detail, thus that thing is maintained over here. http://Articomed.com/node/288763
I was impressed with the quality of service at https://giphy.com/channel/onovenbbcn . They made my car look brand new again!
When some one searches for his necessary thing, so he/she desires to be available that in detail, thus that thing is maintained over here. http://Articomed.com/node/288763
Great insights! Discover more at Boiler breakdowns .
The best part about using a ##demolition company near me## is that they understand local regulations and can handle permits for you. office cleanout
Useful advice! For more, visit ادمین اینستاگرام .
This was highly educational. For more, visit https://rentry.co/3a368f34 .
Wonderful options on organizing in the past a monstrous movement! Explore extra at mudança em sorocaba wherein they have large components!
Appreciate the detailed post. Find more at https://sethtpka815.huicopper.com/effective-techniques-to-unblock-a-drainpipe .
Great information! The importance of backlinks cannot be overstated, and I’ll be checking out Buy backlinks for safe options.
Moreno Valley residents should definitely consider on-site auto repairs; they’re fantastic! Learn more at battery replacement Moreno Valley mobile mechanic .
Thanks for the valuable insights. More at car hire toronto .
Found out about Long distance movers Glendale through friends – they speak highly of their services!
If you’re moving to or from San Antonio, don’t forget about San Antonio auto shipping for your car shipping needs!
This was nicely structured. Discover more at seguro viaje .
.Wondering what stick with-up topics may well spark additional discussion involving more than a few appliance on hand presently inside market!!!!! https://giphy.com/channel/claruswdtg
Your real looking details make shifting look less daunting; I’ll truthfully refer returned to this whilst the time comes mudanças em sorocaba
The joy of coming dwelling to a wagging tail is unmatched! What does your dog do whilst you stroll via the door? Tell us at https://extra-wiki.win/index.php/The_Role_of_Dogs_in_Therapy_and_Emotional_Support_45053 !
Thanks for the helpful article. More like this at ماساژ ماهور .
Appreciate the comprehensive insights. For more, visit Dental Group of Beverly Hills .
Just bookmarked this web publication—it’s going to be my cross-to resource as I commence making plans my digicam installing!! Outdoor Security Camera Installation
Understanding social media demographics helps target audiences better; great points made here! Learn more strategies from ### anyKeyWord###. Rehan Hasan
This was quite informative. For more, visit residential plumber .
Your publish made me observe how so much I’ve been neglecting distinct regions of my abode! It’s time for a radical spring fresh, and I’ll virtually determine out house cleaning for tricks.
Its like you learn my mind! You appear to know so much about this, like you wrote
the e-book in it or something. I believe that you can do with some percent to drive the message house a little bit,
but other than that, this is fantastic blog. A great read.
I’ll certainly be back.
Greate article. Keep posting such kind of info on your site.
Im really impressed by it.
Hey there, You’ve performed a great job. I’ll definitely digg it and in my
opinion suggest to my friends. I’m confident they’ll be benefited from this website. https://Blogs.Koreaportal.com/bbs/board.php?bo_table=free&wr_id=5238754
Greate article. Keep posting such kind of info on your site.
Im really impressed by it.
Hey there, You’ve performed a great job. I’ll definitely
digg it and in my opinion suggest to my friends. I’m confident they’ll
be benefited from this website. https://Blogs.Koreaportal.com/bbs/board.php?bo_table=free&wr_id=5238754
I found this very interesting. Check out LuxeNeuro for more.
Your short article about reducing home waste through much better cleansing practices was mind-blowing!” Have a look at further eco-tips over on house cleaning .
Making home made foodstuff for my domestic dog has been so enjoyable—what recipes do you put forward? Let’s proportion favorites on https://aged-wiki.win/index.php/Top_five_Dog_Breeds_for_Apartment_Living !
The advice approximately drone camera stabilization options is precious for anyone serious about videography; thanks for sharing that perception! Visit https://seomaestro.kz/go.php?url=https://wiki-quicky.win/index.php/**Safety_First:_Best_Practices_for_Flying_and_Using_Your_Drone_Camera_Responsibly** for greater info!
Thanks for the valuable insights. More at reliable commercial pest control Flanders .
Just wanted to share my positive experience with a local Auto Movment Group in Tampa; they were fantastic!
I wish I had known about this Odessa moving company sooner; they saved me so much time! Odessa FL Mover’s
I would definitely recommend using Orlando commercial movers for any business relocation needs! Orlando Mover’s FL
Hi there, after reading this remarkable piece of writing
i am too delighted to share my familiarity here with colleagues.
Great reference material provided herein about strategic planning needed throughout process – eager look into partnerships available locally through friends over at # anykeyword# Local movers Key Biscayne
A hassle-free moving experience is what I got from Casselberry international movers—highly recommend them! Casselberry Mover’s
Anyone know if Local movers Dania Beach offers packing services? I’m planning a big move soon in Dania Beach.
Thanks for the informative post. More at seguros de viaje baratos .
Thanks for the great explanation. More info at Affordable Pest Solutions .
Appreciate the thorough insights. For more, visit https://ricardoxrwd830.tearosediner.net/schedule-your-wheel-alignment-in-bonney-lake-today-10 .
The customer support from my Dallas vehicle shipping agent was exceptional! A1 Auto Transport’s Dallas
Just finished a move with Lulu full service movers , and I’m so impressed by their professionalism!
Been using Nitric Boost Ultra for a couple of weeks now, and
I can honestly say I’m feeling more energized during workouts.
Great to see a review that explains the science without making it too
complicated.
Hi there it’s me, I am also visiting this website on a regular basis, this website is truly fastidious and the users are genuinely sharing nice thoughts. http://dragon-slave.org/comics/BelindavtSimmsrg
Very informative post! If you’re considering buying backlinks, definitely check out what Backlinks provider has to offer.
I love it when folks get together and share ideas. Great site, stick with it!
This was highly useful. For more, visit Afordable Pest Solutions .
Video SEO is an area that demands attention; thanks for shedding light on it! Discover additional information at Rehan Hasan .
This was highly educational. For more, visit http://noreferer.net/?url=https://www.bright-bookmarks.win/exactly-how-to-avoid-plumbing-and-home-heating-issues-in-older-houses .
Great tips! For more, visit 24 hour emergency plumber near me .
Thanks for the advice on holding a first-night box handy; it makes settling in such a lot less complicated! empresa de mudanças
I found this very helpful. For additional info, visit Bathroom Remodeling .
This is highly informative. Check out https://list.ly/beleifbsyj for more.
I wish all car repairs could be done on-site like this—what a time-saver! brake repair mobile service Modesto
Thanks for the helpful advice. Discover more at alcohol rehab .
Your counsel on tackling one room at a time is so functional! I recurrently get crushed, however this makes it conceivable. Can’t wait to study greater on house cleaning services Orchard Hills !
Just wanted to share how impressed I am with the service from asesor fiscal for my recent septic work.
Valuable information! Find more at LuxNeuro .
Fantastic post! Discover more at drain cleaning service near me .
The significance of keeping surface areas clear can not be worried enough– thank you for highlighting this!” Check out even more insights over at newport beach house cleaning .
พูดถึงข้อดีข้อเสียของแต่ละรุ่นเพื่อช่วยในการเลือกซื้อ ### ร้าน ไฟ
I love the principle of by using shade-coded labels for the several rooms. It simplifies unpacking! mudanças em sorocaba
Love the way you addressed the two service provider and safe practices; they pass hand in hand at some point of relocations! mudança em sorocaba
This was a wonderful guide. Check out loan agency new orleans for more.
การมองเห็นในระยะไกลดีขึ้นหลังจากติดตั้งสบายใจมากเลย #BT_PREMIUM## ร้านซ่อมระบบไฟรถยนต์ ใกล้ฉัน
Buying backlinks can be tricky, but I trust Order backlinks for quality and reliability.
For anyone living in Moreno Valley, on-site auto repair is unbeatable! Find services at emergency mobile mechanic Moreno Valley .
Excellent article. I am experiencing many of these issues as well..
Fantastic post! Discover more at Afordable Pest Solutions .
This is highly informative. Check out seguro de viaje for more.
This was highly useful. For more, visit clogged toilet service near me .
Valuable information! Find more at sex tre em .
Appreciate the great suggestions. For more, visit leaking pipe .
Your post made me understand how tons I’ve been neglecting confident parts of my residence! It’s time for an intensive spring fresh, and I’ll absolutely examine out house cleaning services woodbury, ca for hints.
Fantastic post! Discover more at LuxeNeuro .
Thanks for the informative post. More at expert trust a trader plumbing .
Such an eye fixed-opener! I by no means learned that completely different actions require varied float fees. This wisdom will indubitably help me make more expert choices shifting ahead. https://www.pure-bookmark.win/to-effectively-easy-a-deck-a-power-washing-machine-with-a-psi-fluctuate-of-2500-to-3000-is-perfect
This was highly helpful. For more, visit Affordable Pest Solutions .
Utilizing natural items for cleansing is the best option! Have a look at more eco-friendly ideas at house cleaning services .
Thanks for the great content. More at Pure Plumbing Company .
Everything is very open with a really clear explanation of the challenges.
It was really informative. Your website is extremely helpful.
Thank you for sharing!
Appreciate the useful tips. For more, visit kitchen remodeler .
Thanks for the helpful advice. Discover more at 831 moving services .
Well explained. Discover more at Gas cooker repairs .
Dogs love range of their walks—what detailed routes do you’re taking with yours? Share sought after taking walks spots on https://wool-wiki.win/index.php/Understanding_the_Canine_Sense_of_Smell:_How_It_Works .
This was highly useful. For more, visit Affordible Pest Solutions .
” Demolition doesn’t have to be scary when working alongside experts like ####myurl####. residential demolition
You really make it seem so easy with your
presentation but I find this topic to be actually something
which I think I would never understand. It seems too complicated
and extremely broad for me. I am looking forward for your next
post, I will try to get the hang of it!
Appreciate the insightful article. Find more at moving services .
Thanks for the practical tips. More at Kitchen Remodeling .
Valuable information! Discover more at bay area car wraps .
This blog has opened my eyes to the possibilities of on-site auto repairs—thanks for sharing! brake repair mobile service Modesto
Helpful suggestions! For more, visit seguros viajes .
Loved your points about optimizing website speed — it’s critical for user experience ! Find optimization tools via ### anyKeyWord### . Rehan Hasan
This is quite enlightening. Check out https://blogfreely.net/erwineomen/why-regular-oil-changes-in-bonney-lake-can-save-you-thousands-smp0 for more.
Wonderful assistance on find out how to make shifting smoother! Visit mudanças em sorocaba for greater first-class counsel and tricks.
Loved hearing stories shared among users who experienced difficulties navigating through processes resulting from damage incurred upon original structures!!! # # anYkEyWoRd # side window replacement Greensboro NC
Grateful for #AnyKeyWord#’s expertise in handling tricky auto glass replacements smoothly and efficiently. https://www.demilked.com/author/brendaatjd/
Hey there! I’ve been following your web site for a long time now and finally got the bravery to
go ahead and give you a shout out from
Atascocita Tx! Just wanted to tell you keep up the fantastic work!
You should take part in a contest for one of the most useful blogs on the
web. I’m going to highly recommend this blog! http://Articomed.com/node/293327
Have observed myself bonding over playdates prepared amongst fellow pet vendors inside of vicinity groups —What pursuits may well be hosted locally within YOUR place ? https://wiki-triod.win/index.php/Barking_Mad!_Why_Do_Some_Breeds_Bark_More_Than_Others%3F
You should take part in a contest for one of the most useful
blogs on the web. I’m going to highly recommend this blog! http://Articomed.com/node/293327
This is such valuable information! I will consider using Buy backlinks cheap to boost my website’s visibility.
I like what you guys are up too. This sort of
clever work and coverage! Keep up the awesome works guys I’ve incorporated
you guys to blogroll.
This article really breaks down the differences between maid and cleaning services. It’s helpful for someone like me who is new to hiring help. I’ll be checking out cleaning services Blairsville PA soon! professional commercial cleaning company near me
Anyone else love due to their power washers as an excuse to relish being outside at the same time getting chores completed?? # # anyK eyword ## https://wiki-global.win/index.php/Top_10_Mistakes_People_Make_When_Using_a_Pressure_Washer
อยากทราบรีวิวจากผู้ใช้จริงเกี่ยวกับประสิทธิภาพของ BT PREMIUM #BT_PREMIUM## หลอดไฟหน้ารถยนต์
Just got settled in Ocoee thanks to the help of an awesome mover I found on Best Ocoee movers !
This was quite useful. For more, visit reliable plumbing reviews .
Thanks for the informative post. More at LuxeNeuro .
เชื่อไหมว่าไฟหน้าโปรเจคเตอร์ช่วยลดอุบัติเหตุได้จริงๆ หลอด ไฟ ซีนอน
Heya i am for the first time here. I came across this board and I find It really useful & it
helped me out much. I hope to give something back and aid others like
you aided me. http://dragon-Slave.org/comics/CedriccvDulaneyjc
Your organizational hacks are lifesavers! They make the whole thing most more easy and tension-free, and I’m keen to stumble on extra at house cleaning services .
Heya i am for the first time here. I came across this board and I find
It really useful & it helped me out much. I hope to give something back and aid others
like you aided me. http://dragon-Slave.org/comics/CedriccvDulaneyjc
I fully agree that consistency is fundamental in dog practicing. Your insights are spot on! For more distinctive guides, inspect out https://www.unitedbookmarkings.win/the-fee-of-canine-tuition-camp-can-vary-extensively-depending-on-explanations-like-area-duration .
Great insights! Discover more at phim hiếp dâm .
Thanks for the clear breakdown. Find more at trusted plumbing contractors .
The value of keeping surfaces clear can not be worried enough– thank you for highlighting this!” Explore even more insights over at house cleaning service near me .
Appreciate the comprehensive advice. For more, visit affordable plumbing repair .
Thanks for the insightful write-up. More like this at Affordable Pest Solutions .
This was a fantastic read. Check out toilet clog solutions for more.
ติดตั้งเองได้ไหม หรือควรไปหาช่างติดแทน ? ร้าน ทํา ไฟหน้ารถยนต์ ใกล้ ฉัน
Content repurposing is a smart strategy for maximizing reach—thanks for highlighting that! Learn more at Rehan Hasan !
This is a very informative article! I’ll definitely check out High authority backlinks buy for safe link-building options.
Found my perfect match when searching for local carriers thanks to insights shared at ### anykeyword ## Santa Ana vehicle shipping
This was highly educational. For more, visit Dental Group Beverly Hills .
Clearly presented. Discover more at plumbing company .
Appreciate the detailed post. Find more at kitchen remodeler .
Appreciate the thorough insights. For more, visit santa cruz movers .
Your insights really opened up my eyes about how easy it can be; I’m ready to dive deeper into options at ### anyKeyWord###.” St Cloud auto transport companies
Useful advice! For more, visit https://list.ly/i/11120226 .
Appreciate the detailed post. Find more at Flanders insect extermination .
This was beautifully organized. Discover more at https://www.mediafire.com/file/qhz1aaa2onwsh60/pdf-71718-48193.pdf/file .
Office cleanouts don’t have to be painful! I hired junk cleanouts and they made the process so easy!
Your advice on tackling one room at a time is so functional! I on the whole get crushed, yet this makes it doable. Can’t wait to study extra on house cleaning services !
What’s up, yes this post is actually nice and I
have learned lot of things from it concerning blogging.
thanks.
Your blog is filled with precious wisdom that each and every aspiring drone photographer should examine—thank you for sharing these types of facts and tricks, won’t wait to discover similarly supplies introduced by means of journeying http://link.chatujme.cz/redirect?url=https://guireerrqe.livejournal.com/profile/ !
Every surface needs attention when cleaning; I value the pointer! More suggestions at house cleaning service near me .
อยากให้ทุกคนลองเปลี่ยนมาใช้ไฟหน้าโปรเจคเตอร์กันนะครับ ไฟ led รถยนต์
This was very enlightening. For more, visit toilet repair services .
Appreciate the detailed information. For more, visit Budd Lake eco-friendly exterminators .
This actually sounds like something I’d stick with!
I love that Nagano Tonic is easy to use and doesn’t feel like a chore—just
mix it into a drink and go. If it really helps boost metabolism and energy, I’m all
in. Thanks for the honest review!
I found this very helpful. For additional info, visit Bathroom Remodelers .
Here’s hoping this article encourages others looking into opportunities related towards utilizing local resources effectively moving forward. emergency mobile mechanic Modesto
Thanks for the informative post. More at alcohol rehab .
Kudos for growing such an informative aid that addresses favourite considerations with regards to camera setups!! ##anyKeywords## https://wiki-quicky.win/index.php/**A_Beginner%27s_Guide_to_Mounting_Outdoor_Security_Cameras**
I these days cleaned my deck the usage of a 2700 PSI stress washing machine and it worked like a allure! If you prefer to look a few beforehand-and-after pictures, investigate out https://www.seo-bookmarks.win/to-easily-easy-a-deck-a-force-washing-machine-with-a-psi-wide-variety-of-2500-to-3000-is-good .
Wonderful tips! Discover more at contratar seguros de viaje .
If you’re dealing with pests, make sure you hire qualified ##bed bug exterminators## to effectively tackle the issue. Junk removal
Appreciate the comprehensive advice. For more, visit Affordible Pest Solutions .
Have you ever tried scent paintings video games with your puppy? It’s such a fascinating task! Find out extra about it at https://hotel-wiki.win/index.php/The_Impact_of_Spaying/Neutering_on_Your_Dog%E2%80%99s_Behavior .
On-site auto repair is such a convenient solution for busy people like me. Thanks, brake repair mobile service Moreno Valley !
Attractive section of content. I just stumbled upon your blog and in accession capital to assert that I get in fact enjoyed account
your blog posts. Anyway I will be subscribing
to your feeds and even I achievement you access consistently fast. https://sitecheck.sucuri.net/scanner/?scan=http://Dragon-Slave.org/comics/KatlynriLandid
Awesome information here! For anyone looking to enhance their SEO game, try buying backlinks from Backlinks provider .
Attractive section of content. I just stumbled upon your blog and in accession capital to assert that I get in fact enjoyed account
your blog posts. Anyway I will be subscribing to your feeds
and even I achievement you access consistently fast. https://sitecheck.sucuri.net/scanner/?scan=http://Dragon-Slave.org/comics/KatlynriLandid
Kudos to the team at ### anykeyword ###! They made transporting my vehicle easy and affordable from **Kissimmee**. Kissimmee auto shippers
Useful advice! For more, visit Roof installation American Fork .
This was very beneficial. For more, visit clinic offering brain mapping in Denver .
Thanks for sharing this information! My windshield needs repair, and I’ll definitely look into your recommendations. windshield chip repair Greensboro NC
Thanks for imparting such simple cleansing pointers! They’re really advantageous in protecting a house tidy with out feeling crushed—will look at various out house cleaning services subsequent!
Appreciate the comprehensive advice. For more, visit Water Heater .
Appreciate the detailed information. For more, visit Afordable Pest Solutions .
Using music or podcasts while cleaning makes the procedure a lot less tiresome!” Discover more pleasurable ways to tidy over at house cleaning service newport beach .
Great insights! Discover more at Dental Group of Beverly Hills .
Nicely done! Find more at Kitchen Remodelers .
Appreciate the detailed information. For more, visit alcohol rehab .
Thanks for the helpful article. More like this at rent a car toronto .
Thanks for the helpful article. More like this at emergency plumbers .
Thanks for the useful suggestions. Discover more at LuxNuro .
Taking care of my car just got easier thanks to onsite services available here in Modesto! emergency mobile mechanic Modesto
A reliable #demolition company near me# saved us tons of time during our renovation project; so grateful for their expertise! residential demolition
This was highly useful. For more, visit kitchen remodeling contractor santa clara .
Thanks for the detailed post. Find more at santa cruz moving company .
Training will also be a concern, but your step-by-step way makes it seem possible! I’ll easily be trying out https://www.web-bookmarks.win/the-can-charge-of-canine-instruction-camp-can-fluctuate-extensively-based-on-causes-like-position-duration for greater exercise recommendations.
Clearly presented. Discover more at Santa cruz 831 movers .
Thanks for the detailed guidance. More at Affordable Pest Solutions .
What’s up to every single one, it’s truly a pleasant for me to pay a
quick visit this web site, it consists of important Information.
Thanks for the thorough analysis. Find more at san leandro vehicle wraps .
Well done! Find more at contratar seguros de viaje .
Oh my goodness! Incredible article dude! Many thanks, However I am experiencing difficulties
with your RSS. I don’t know why I can’t subscribe to it.
Is there anybody else having the same RSS issues?
Anyone that knows the answer will you kindly
respond? Thanks!!
Thanks for the valuable insights. More at https://ricardoxrwd830.tearosediner.net/choosing-the-right-tires-in-bonney-lake-wa-9 .
Everything is very open with a precise explanation of the challenges.
It was really informative. Your website is very helpful.
Many thanks for sharing! https://dragon-slave.org/comics/LeifbeNobeliusvx
Everything is very open with a precise explanation of the challenges.
It was really informative. Your website is very helpful.
Many thanks for sharing! https://dragon-slave.org/comics/LeifbeNobeliusvx
I liked this article. For additional info, visit Afordable Pest Solutions .
Has anyone tried on-site auto repair in Moreno Valley? I found some great options at mobile auto repair Moreno Valley CA !
Honestly, I’ve tried so many creams for brittle nails and nothing worked long-term.
But this NanoDefense Pro actually sounds different with the nanotech approach.
Has anyone here noticed real improvements in nail strength?
Finally, a review that isn’t just hype! I’ve been debating whether to try AquaSculpt and this really helped me understand how it’s supposed
to work. Love that it’s targeting women over 40 specifically—our bodies definitely don’t
respond the same as they did in our 20s!
This was very enlightening. For more, visit Beverly Hills 24 hour dental services .
Very nice post. I just stumbled upon your blog and wished to
say that I’ve truly enjoyed browsing your blog posts. After all I will be subscribing to your rss feed and I
hope you write again very soon! https://Wiki.Snooze-hotelsoftware.de/index.php?title=Lave-auto_Pas_De_Contact_%C3%83_Montr%C3%83_al_:_Une_Choix_Rapide_Efficace_Et_S%C3%83%C2%BBre_Pour_Frotter_Votre_V%C3%83_hicule
Love these floor-cleaning hacks; they will certainly save me time this weekend! Take a look at more suggestions at house cleaning services !
Very nice post. I just stumbled upon your blog and wished to say that I’ve truly enjoyed browsing your blog posts.
After all I will be subscribing to your rss feed and I hope you write again very soon! https://Wiki.Snooze-hotelsoftware.de/index.php?title=Lave-auto_Pas_De_Contact_%C3%83_Montr%C3%83_al_:_Une_Choix_Rapide_Efficace_Et_S%C3%83%C2%BBre_Pour_Frotter_Votre_V%C3%83_hicule
Have you ever tried smell work games with your canine? It’s such an attractive recreation! Find out extra approximately it at https://wiki-spirit.win/index.php/How_to_Handle_Aggression_in_Dogs:_A_Comprehensive_Approach .
“If you’re overwhelmed by junk at home or work, don’t hesitate to contact # boiler removal #.”
This was highly educational. For more, visit Affordable Pest Solutions .
Thank you for addressing common misconceptions about firearms on Arms & Ammunition Dealers ! It’s crucial to clear up misinformation.
Amazing content material on shooting landscapes with drones! I’ll obviously use these programs all through my next flight! Learn extra at http://football.sodazaa.com/out.php?url=https://pixabay.com/users/51250136/ .
พูดถึงเคล็ดลับในการปรับแต่งระบบแสงเพื่อเพิ่มความสวยงาม ### ร้าน ไฟ
This was highly educational. For more, visit seguros viajes .
Valuable information! Find more at windshield replacement Greensboro NC .
I have to thank you for the efforts you have put in writing this site.
I really hope to see the same high-grade blog posts by you in the future as well.
In truth, your creative writing abilities has motivated me to get my very own site now 😉 http://classicalmusicmp3freedownload.com/ja/index.php?title=Cours_D_oenologie_Sur_Le_Canada_:_D%C3%83_couvrez_Le_Monde_De_La_Vigne_Et_Du_Vin
I have to thank you for the efforts you have put in writing this site.
I really hope to see the same high-grade blog posts by you in the future as
well. In truth, your creative writing abilities has motivated me to get my very own site now 😉 http://classicalmusicmp3freedownload.com/ja/index.php?title=Cours_D_oenologie_Sur_Le_Canada_:_D%C3%83_couvrez_Le_Monde_De_La_Vigne_Et_Du_Vin
ทำไมถึงควรเปลี่ยนมาใช้ไฟหน้ารถ LED? ไฟหน้า
Thanks for the informative content. More at LuxeNeuro .
I’m curious to find out what blog system you are using?
I’m experiencing some small security issues
with my latest website and I would like to find something more safeguarded.
Do you have any solutions?
Great post! I’ve been looking for ways to improve my SEO. I think investing in backlinks like those from Buy high-quality backlinks could really help my site.
Has anyone found a great chiropractor for post-accident recovery? I’d love some recommendations! Best car accident chiropractor
This was a wonderful post. Check out santa cruz movers for more.
Wow, this actually sounds promising! I’ve been dealing with nerve discomfort in my legs for months
and nothing has really worked long-term. I like that Nerve Fresh is all-natural and made in the USA—definitely considering giving it a
try.
This is really interesting, You are a very skilled blogger.
I have joined your feed and look forward to seeking more of your great post.
Also, I have shared your web site in my social networks!
Your instruction manual on tension washing machine protection is so invaluable! I’ll easily store those assistance in intellect even as cleansing. https://devpagelvgqu.contently.com
Looking into options for auto transport? Don’t miss checking out Homestead car shipping !
Appreciate the detailed insights. For more, visit Dental Group of Beverly Hills .
This was very well put together. Discover more at loan agency new orleans .
Appreciate the great suggestions. For more, visit phim sex hàn quốc .
Having youngsters makes cleaning just a little of a subject, however your ideas make it less overwhelming. I have fun with the advice and can explore extra at house cleaning !
Your post on company has actually inspired me to tackle my garage this weekend!” Find additional motivation and concepts over at newport beach house cleaning .
ไฟหน้ารถ LED BT PREMIUM ทำให้การขับขี่กลางคืนปลอดภัยขึ้นมากเลยครับ bt premium auto xenon สาขา ศรีนครินทร์
Thanks for the great information. More at Painting Contractors .
Helpful suggestions! For more, visit rehab .
Nicely done! Find more at LuxNuro .
I can’t believe how much easier car ownership could be with onsite services available locally! mobile mechanic near me
Thanks for the great information. More at Flanders pest control experts .
Wow, I had no idea there was a natural solution like iGenics that targets the root cause of eyesight loss!
The way it safely clears the toxic buildup around the eyes sounds really promising.
Definitely worth considering for anyone struggling with vision issues.
This post provides excellent guidance on link-building practices; I’m excited about trying __ anyKeyWord__’s service! Best place to buy backlinks
I visited various web pages but the audio feature for audio songs existing at this site is genuinely wonderful.
Shoutout to #AnyKeyWord# for fixing my cracked windshield without making me wait forever! https://escatter11.fullerton.edu/nfs/show_user.php?userid=8989131
Your post has provided clarity on how to choose a quality commercial roofer—what’s your take on online reviews vs personal recommendations? commercial roofing contractor
What a information of un-ambiguity and preserveness
of valuable know-how about unpredicted emotions.
Thanks for the insightful write-up. More like this at Afordable Pest Solutions .
Anyone else loving the convenience of on-site repairs? I found an awesome place at mobile mechanic near me Moreno Valley !
Bed bug removal is no joke! I appreciate the insights here, and I’ll be checking out commercial demolition for help.
I enjoyed this read. For more, visit Dental Group Beverly Hills .
Hi, I would like to subscribe for this webpage to take latest updates, so where can i do it please assist.
I appreciated this post. Check out https://telegra.ph/Top-7-Signs-Your-Car-Needs-Brake-Repair-in-Bonney-Lake-Top-7-Signs-Your-Car-Needs-Brake-Repair-in-Bonney-Lake-07-10 for more.
Keen hobby lies inside exploring prospective partnerships between tech prone alongside side depended on installers regionally!!!! ### anykeyword### Home Security Camera Installation
Getting rid of mess is so freeing! I loved the article on minimalism at house cleaning .
This article is a must-examine for all of us looking to store on their water bill. Understanding what percentage gallons in line with minute you actually need can end in remarkable discounts! https://www.bookmarkidea.win/to-correctly-clean-a-deck-a-power-washing-machine-with-a-psi-latitude-of-2500-to-3000-is-perfect
I love the notion of a “cleaning schedule.” It’s more easy to preserve up with chores whilst there’s a plan in location! Thanks for the reminder—I’ll look into house cleaning near me for templates!
This was a great help. Check out Affordible Pest Solutions for more.
Have any extraordinary adventures taken situation when vacationing with pets ? From road journeys to holidays, let’s swap experiences here ### anykeyword ### https://sierra-wiki.win/index.php/Unconventional_Dogs:_Unique_Breeds_You_Might_Not_Know_About_76893
Do you think using multiple colors in one room is too much, or can it be done tastefully? Atlanta painters
My journey to full recovery began when I sought help from an experienced car accident chiropractor—so glad I did! Best car accident chiropractor
Making thoughts shared between fur children & owners creates lifelong bonds –How oftentimes catch snapshots representing loved moments spent jointly all the way through years long gone earlier? https://tiny-wiki.win/index.php/Training_Techniques:_Positive_Reinforcement_vs._Punishment
This was nicely structured. Discover more at Kitchen Remodeling Nashville .
This was very enlightening. For more, visit alcoholic counseling .
I love taking my dog on hikes! The pleasure they exhibit in nature is infectious. Get outdoors hints in your furry pal at https://online-wiki.win/index.php/Inspiring_Stories_of_Service_Dogs_Changing_Lives_Every_Day .
This was quite informative. For more, visit contratar seguros de viaje .
This paragraph will help the internet people for building up new website or
even a blog from start to end.
Onsite vehicle maintenance could forever change our relationship with car upkeep; I’m excited! mobile mechanic near me
Really like how approachable you’ve gotten made securing houses with elementary guidance everyone can keep on with!!! ##anythingKeywords ## https://rapid-wiki.win/index.php/**Top_Mistakes_to_Avoid_When_Mounting_Security_Cameras_on_Your_House**
Has anyone tried using chalk paint for furniture? I’m curious about how it holds up over time. painters near me
WebSite: https://repaircddvd.com
This is exactly what I needed to read today! Looking forward to trying out Permanent backlinks for backlink purchases.
This was quite enlightening. Check out movers in santa cruz ca for more.
” Just finished using #myurl#’s services and couldn’t believe how quick everything went! basement cleanout
Thanks for the great tips. Discover more at 831 Movers – Santa Cruz .
This was quite helpful. For more, visit back glass replacement Greensboro NC .
Thanks for the thorough article. Find more at san leandro car wraps .
Moreno Valley has some amazing on-site auto repair options! Check them out at battery replacement Moreno Valley mobile mechanic .
What should I expect when hiring a moving company like Dania Beach commercial movers in Dania Beach? Any tips?
This is such an informative article! I’m continually on the search for new tactics to improve my puppy’s habit. I discovered a few splendid assistance at https://www.tool-bookmarks.win/the-check-of-puppy-classes-camp-can-vary-widely-based-on-points-like-place-length that complements your suggestions.
Thanks for the helpful article. More like this at cheap car rental .
Your post on organization has influenced me to tackle my garage this weekend!” Discover additional motivation and concepts over at house cleaning service newport beach .
Thanks for the insightful write-up. More like this at LuxNeuro .
The tips for maintaining firearms shared at Suppressors & Gun Silencers Online are practical and easy to follow.
Anyone else think that Tampa car shipping is the best way to get around during Gasparilla?
This is highly informative. Check out Affordible Pest Solutions for more.
This was a great article. Check out phim sex for more.
A #garage cleanout# not only clears clutter but also opens up new possibilities for storage or hobbies—highly recommend it! Residential junk removal
Just wanted to share that using a professional service for NY auto transport was worth every penny! New York auto shipping
Kudos to all the hardworking professionals in the Dallas auto shipping industry; you can find great ones at Dallas auto shippers !
Appreciate the thorough analysis. For more, visit Afordable Pest Solutions .
This was a wonderful guide. Check out Dental Group of Beverly Hills for more.
This article made me appreciate how an awful lot creativity can come from applying a drone camera! Can’t wait to test with new options! Check out greater at https://go.bubbl.us/ec1490/4063?/Bookmarks .
Great insights into picking out detergents chiefly made for concrete surfaces—they enormously do remember!!! ## https://wiki-club.win/index.php/Creative_Ways_to_Freshen_Up_Your_Sidewalk_Without_Power_Washing_79094
“So glad I did research before choosing movers; LULU was the right choice!” Office moving companies Lulu
Thanks to https://orcid.org/0009-0000-3423-476X , my windshield is as good as new! Great attention to detail.
My coder is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the costs.
But he’s tryiong none the less. I’ve been using WordPress on a variety of websites for about a year and am anxious about switching to another
platform. I have heard great things about blogengine.net. Is there a
way I can transfer all my wordpress posts into it?
Any help would be really appreciated!
Thank you for sharing these valuable house cleaning techniques– they make certain to make a difference!” Dive into more specialist suggestions over on house cleaning service .
I’ve shared this text with associates who are also fascinated by editing their dwelling house’s safety features!!! ### anykeyword### Outdoor Security Camera Installation
I these days wiped clean my patio with a pressure washer and it looks up to date! Highly propose this formulation! https://romeo-wiki.win/index.php/How_to_Prepare_Your_Home_Before_a_Professional_Pressure_Wash
Thanks for presenting such reasonable cleaning tips! They’re in actuality handy in protecting a condo tidy with out feeling beaten—will determine out house cleaning near me subsequent!
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is important and all. But think about if you added some great graphics or videos to give your posts more,
“pop”! Your content is excellent but with pics and video clips,
this website could undeniably be one of the most beneficial in its niche.
Superb blog!
This was highly useful. For more, visit professional pest management in Flanders .
Such an eye fixed-opener! I in no way found out that assorted activities require the different glide premiums. This wisdom will in reality support me make more instructed selections moving ahead. https://www.random-bookmarks.win/to-appropriately-smooth-a-deck-a-stress-washing-machine-with-a-psi-diversity-of-2500-to-3000-is-ideal
This was quite informative. More at seguros viajes .
The average cost of a landscape designer can really vary! It’s great to have an idea of what to expect. LA landscape architect
ไม่อยากให้ใครพลาดประสบการณ์ดี ๆ ที่นี่เลยจริง ๆ ค่ะ # # anyKeyWord## ผับสาย1 รับจัดเลี้ยง
This is highly informative. Check out plumbers services for more.
I found this very helpful. For additional info, visit kitchen remodeling .
Just started my journey into web design and I’m inspired by Liverpool’s creative community! Found great resources on website design liverpool uk .
Finding a psychiatrist can be overwhelming, but being located near Grand Central makes it much easier! Learn more about your options at psychiatrists near me .
This is quite enlightening. Check out alcoholic counseling for more.
Thanks for the helpful article. More like this at san leandro vehicle wraps .
Thanks for the thorough analysis. Find more at Kitchen Remodeling Nashville .
You can certainly see your expertise in the work you write.
The sector hopes for more passionate writers such as you who aren’t afraid
to say how they believe. At all times go after your heart.
The joy of coming domestic to a wagging tail is unequalled! What does your puppy do if you stroll thru the door? Tell us at Click for more !
Well explained. Discover more at Denver innovative brain mapping .
Greetings I am so thrilled I found your weblog, I really found you by error, while
I was browsing on Google for something else, Anyways I am here now and would just like
to say many thanks for a tremendous post and a all round enjoyable
blog (I also love the theme/design), I don’t have time to look over
it all at the minute but I have book-marked it and also added your RSS feeds, so when I have time I will be back
to read a lot more, Please do keep up the great
job.
I’m impressed, I have to admit. Seldom do I encounter a
blog that’s both educative and interesting, and without a doubt, you have hit the nail on the head.
The issue is an issue that not enough men and
women are speaking intelligently about. I am very happy I found this
in my search for something regarding this.
Your analysis of online vs. brick-and-mortar sales at Pistol wholesalers & distributors provided great clarity on current trends.
Thanks for the clear advice. More at auto glass Greensboro NC .
Fantastic insights into on-site auto repair services in Modesto—definitely considering it now! brake repair mobile service Modesto
Your post really highlighted the importance of understanding how much roofers charge per job. Transparency in pricing is key! Continue reading
If you find yourself buried under piles of junk, remember that %%LINK%% is just a click away! cleanout companies near me
Thanks for the informative content. More at air conditioning repair .
If you’re looking for reliable HVAC repair in Springfield, MO, I highly recommend checking out local services that can help with everything from routine maintenance to emergency repairs. They have great reviews! hvac companies
Appreciate the detailed information. For more, visit affordable Budd Lake extermination services .
Appreciate the thorough analysis. For more, visit Beverly Hills Dental Group .
Glad stumbled across this post detailing several factors influencing decisions made surrounding choosing particular mechanic specializing specifically focusing highly specialized areas involving onsite assistance offered through various sources mentioned car repair at home Chattanooga
I found this very interesting. For more, visit contratar seguros de viaje .
Does anyone know a good on-site auto repair service in Moreno Valley? I found one at brake repair mobile service Moreno Valley !
Thanks for the helpful advice. Discover more at instant payday loans new orleans .
Thank you for sharing this knowledge! Purchasing quality backlinks from places like Buy high-quality backlinks makes a huge difference.
This was nicely structured. Discover more at brain diagnostics clinic in Denver .
Pretty great post. I just stumbled upon your weblog and wished
to say that I’ve really enjoyed surfing around your weblog posts.
In any case I’ll be subscribing for your feed and I’m hoping you write
once more very soon! http://dragon-slave.org/comics/ArturodcArnotjk
Pretty great post. I just stumbled upon your weblog and wished to
say that I’ve really enjoyed surfing around your weblog posts.
In any case I’ll be subscribing for your feed and I’m hoping you write once more very soon! http://dragon-slave.org/comics/ArturodcArnotjk
Cleaning up can be healing when you get into a groove; thanks for encouraging all of us! Check out more at house cleaning .
The accessibility of psychiatrists in New York around Grand Central is a game changer for those with hectic schedules. Find out more at psychiatrists NYC !
Finding a psychiatrist can be overwhelming, but being located near Grand Central makes it much easier! Learn more about your options at psychiatrist in Brooklyn .
Thanks to quick action from my local crew specializing in #junk hauling#, my home feels spacious again after years of clutter buildup. junk cleanouts
Your organizational hacks are lifesavers! They make every thing lots more effective and tension-loose, and I’m eager to notice more at house cleaning services .
After hearing positive feedback regarding ‘no win, no fee’ solicitors; I’m eager to find representation that meets my needs without financial worries!! No win no fee solicitor Dublin
My schedule is packed、 and this service has made everything so much easier! Thank you、 あにキー! on-site brake repair Columbus
This was quite helpful. For more, visit Bonney Lake oil Change .
Your guidelines on leash tuition are so efficient! I’ve struggled with this facet. I also found a few desirable statistics at https://www.social-bookmarkings.win/the-expense-of-dog-training-camp-can-vary-commonly-based-on-reasons-like-region-period which may guide.
I’m on account that renting a stress washing machine for my spring cleansing—massive guidelines for first-timers right here! https://www.giantbomb.com/profile/jamittzepw/
I found this very interesting. Check out Dental Group of Beverly Hills for more.
Thanks for the detailed post. Find more at rehab .
Great insights! Discover more at Painting Contractors .
Thank you, I have recently been searching for info approximately this
subject for ages and yours is the best I have came upon so far.
However, what concerning the conclusion? Are you certain concerning the supply?
“Thanks to LULU Moving Company, we were able to settle into our new home quickly!” Lulu FL Mover’s
Just when I thought I’d tried everything for my oral health, this video
pops up! Love that ProDentim focuses on the good bacteria—something most people overlook when it comes
to dental care. Might give it a shot soon.
Taking part in charity runs/activities supporting organisations helping uncared for animals conjures up involvement awfully with no question–Which motives resonate strongest for my part motivating traders in the hunt for possibilities combined FUN & WORK https://hotel-wiki.win/index.php/Socializing_Puppies:_The_Key_to_a_Well-Adjusted_Adult_Dog
Landscape design can be so pricey! I wonder how much landscaping costs in Los Angeles compared to other cities. landscape designer Los Angeles
This was very enlightening. For more, visit Affordible Pest Solutions .
On-site auto repair would be ideal for busy professionals like me—great post! car repair at home Modesto
Seasonal cleansing is so sizeable! I continually neglect approximately special spaces until eventually it’s too late. Your list was remarkable priceless, and I’ll be travelling house cleaning services woodbury, ca for extra tricks!
I’ve had my share of HVAC issues in Springfield, MO, and finding a trustworthy repair service made all the difference. It’s crucial to choose a company that knows the local climate and can provide prompt service. heating and cooling
Now more than ever awareness surrounding risks associated healthcare practices grows daily given advances technology — relying upon specialists such as ‘medicalneglegencesolicitosrs’ becomes paramount ! No win no fee solicitors
This blog has really made me think about investing in better insulation for my home. It’s amazing how much it can impact both heating and cooling efficiency! air conditioning repair
Grooming is simple for holding our canine natural and organic and joyful. Check out the premier grooming practices at https://hotel-wiki.win/index.php/Building_a_Strong_Bond_with_Your_Rescue_Dog_24750 !
This info is invaluable. When can I find out more?
This was very enlightening. More at plumbers services .
Helpful suggestions! For more, visit Denver Brain Mapping Solutions .
If you’re tired of waiting at the shop, try on-site auto repair in Moreno Valley! Find out more at battery replacement Moreno Valley mobile mechanic .
Thanks for the great tips. Discover more at santa cruz movers .
This was highly useful. For more, visit RRJ Quality kitchen remodeling contractor .
Valuable information! Discover more at car wraps san leandro .
Your post really highlighted the importance of understanding how much roofers charge per job. Transparency in pricing is key! commercial roofing contractor
My office needed major decluttering—thankfully, %%LINK%% came in and totally revamped our space! Estate cleanouts
The interviews with industry experts featured on Bulk Ammunition, Gun Parts, & More! are a fantastic addition to the discussion.
It’s reassuring to know there are experienced psychiatrists close to Grand Central for those who need support. For more details, head over to psychiatrists near me !
There’s so much information about hormone therapy out there! What do you recommend for Lakewood, WA residents? Med Spa Lakewood
Mental health is just as important as physical health, and having psychiatrists near Grand Central makes it easier for city dwellers. Discover your options at psychiatrists Brooklyn .
Thanks for the thorough article. Find more at Afordable Pest Solutions .
Yesterday, while I was at work, my sister stole my iPad and tested to see if it can survive a 40
foot drop, just so she can be a youtube sensation. My iPad is now destroyed and she has 83
views. I know this is entirely off topic but I had to share it with
someone!
My schedule is packed、 and this service has made everything so much easier! Thank you、 あにキー! on-site brake repair Columbus
My friend just got her wisdom teeth removed by a dentist in Pico Rivera and said it was smooth sailing! Pico dentist
After I originally commented I appear to have clicked on the -Notify
me when new comments are added- checkbox and from now on each time a comment is added I receive 4 emails with the same comment.
Perhaps there is a means you are able to remove me from that service?
Cheers!
Thanks for the valuable article. More at LuxNeuro .
Thanks for the detailed post. Find more at windshield chip repair Greensboro NC .
I love how paint can change the mood of a room! What’s your go-to color for relaxation spaces? painting companies near
Clearly presented. Discover more at expert drain services .
Clearly presented. Discover more at Sinks & Sani- Vite Shower repairs .
I’ve obvious so many adorable blended breeds as of late! Which ones stand out to you? https://www.symbaloo.com/mix/bookmarks-1gj3
I like utilizing baking soda for cleansing; it’s incredible what it can do! Discover more techniques at house cleaning service near me .
This was highly educational. For more, visit Affordable Pest Solutions .
Wow, this has opened my eyes to the possibilities of backlinks! Excited to try out Backlinks provider for my website.
“This blog is such a great resource for anyone needing junk removal advice—thank you, # Estate cleanouts #.”
“The convenience of having my car transported was made possible because of what I learned at Wesley Chapel car shipping #”
Regular repairs is prime to avoiding leading clean-u.s.afterward! Your insights are spot-on; I’m going to check out house cleaning services woodbury, ca for ongoing cleaning systems.
I got amazing insights from # # anyKeyWord ### about what steps I should take after suffering from medical negligence! Medical negligence solicitors Dublin
I’ve had my share of HVAC issues in Springfield, MO, and finding a trustworthy repair service made all the difference. It’s crucial to choose a company that knows the local climate and can provide prompt service. hvac services springfield mo
Nicely detailed. Discover more at Dental Group Beverly Hills .
Finding a psychiatrist can be overwhelming, but being located near Grand Central makes it much easier! Learn more about your options at psychiatrists NYC .
Appreciate the great suggestions. For more, visit Afordable Pest Solutions .
I appreciate how accessible mental health care is in New York City, especially around Grand Central station! Explore your options at psychiatrist in Brooklyn .
I didn’t know about the various options available for Ocala auto shipping until I found Sunshine Auto Transport’s Ocala . Very informative!
This was very enlightening. More at movers .
This was quite informative. More at kitchen remodeler .
I enjoyed this post. For additional info, visit sams signs car wraps .
This is a topic that’s near to my heart… Thank you! Exactly where are your contact details though?
Great tips! For more, visit Affordible Pest Solutions .
Just got my side mirror replaced at https://www.anobii.com/en/0157e10f0885ed445a/profile/activity —great job guys!
Just purchased my first electric strain washer, and I’m interested by your complete projects beforehand of me this summer! https://prashnottar.mantrakshar.co.in?qa=user&qa_1=ashtotxaiz
Thanks for the useful suggestions. Discover more at shower drainage solutions .
Thanks for the detailed guidance. More at reliable checkatrade plumbers .
This is such valuable information! I will consider using Buy backlinks for website to boost my website’s visibility.
I appreciated this post. Check out local plumbing and heating services for more.
I’ve been researching hormone therapy and its effects. Any tips for finding a provider in Lakewood, WA? Medical Spa Lakewood
If you’ve been involved in a car accident, finding the right chiropractor can make a significant difference in your recovery. A specialized car accident chiropractor can help alleviate pain, restore mobility, and guide you through the healing process Seattle Chiropractor
I didn’t become aware of how valuable it’s far to sparkling appliances step by step. Thanks for the reminder! I’ll have to analyze house cleaning services Orchard Hills for a few constructive appliance-cleaning hacks.
Using a stress washing machine between 2000 and 3000 PSI is splendid for deep cleansing decks with no causing spoil. Check out my renowned ideas at https://www.toro-bookmarks.win/to-correctly-fresh-a-deck-a-pressure-washer-with-a-psi-quantity-of-2500-to-3000-is-right !
On-site auto repair could really change how we think about car maintenance in Modesto! car repair at home Modesto
Thanks to the dedicated team at No win no fee solicitor , my personal injury claim was handled professionally and efficiently.
This was a wonderful post. Check out https://send.now/b0yadmtv5xgl for more.
This was very enlightening. More at LuxNuro .
With every passing day comes fresh perspectives implemented onto existing frameworks used across numerous industries—including evolving st website design liverpool
This was quite informative. For more, visit Underfloor heating repairs .
If you’re looking for reliable HVAC repair in Springfield, MO, I highly recommend checking out local services that can help with everything from routine maintenance to emergency repairs. They have great reviews! hvac services springfield mo
After I initially left a comment I appear to have clicked the -Notify me
when new comments are added- checkbox and from now on each time a comment is added I get
four emails with the exact same comment. Is there an easy method you
can remove me from that service? Appreciate it!
You’ve made some really good points there. I looked on the internet
for more information about the issue and found most
people will go along with your views on this website. https://Oerdigamers.info/index.php/Lavage_Automobile_Professionnel_%C3%83_Montr%C3%83_al_:_Pourquoi_Choisir_Un_Service_Expert_Pour_Votre_V%C3%83_hicule
For anyone living in Moreno Valley, on-site auto repair is unbeatable! Find services at Moreno Valley mobile mechanic services .
Great insights shared throughout entire piece written here showcasing advantages found within modern approaches taken towards traditional means often employed historically speaking but now shifting focus entirely towards contemporary solutions being car repair at home Chattanooga
You’ve made some really good points there.
I looked on the internet for more information about the
issue and found most people will go along with your views on this website. https://Oerdigamers.info/index.php/Lavage_Automobile_Professionnel_%C3%83_Montr%C3%83_al_:_Pourquoi_Choisir_Un_Service_Expert_Pour_Votre_V%C3%83_hicule
If anyone is looking for reputable Dallas auto shippers, I highly recommend checking out Dallas auto shippers !
Does Casselberry international movers offer packing services? I’m considering their help for my upcoming move. Long distance movers Casselberry
Useful advice! For more, visit sunroof glass repair Greensboro NC .
This was highly useful. For more, visit underfloor heating service .
Appreciate the detailed information. For more, visit expert 24 7 plumbing .
Awesome article! Discover more at Saniflo WCs .
I found this very helpful. For additional info, visit Summers Plumbing Heating & Cooling .
This is quite enlightening. Check out Beverly Hills Dental Group for more.
Great post.
This was very well put together. Discover more at effective insect solutions Budd Lake .
This was very beneficial. For more, visit 24 7 plumbing help .
Great tips! For more, visit rehab .
I’ve heard that psychiatrists near Grand Central offer flexible hours for busy professionals. It’s great to have mental health support right in the heart of the city! Visit psychiatrist NYC to learn more.
Appreciate the thorough insights. For more, visit advanced brain mapping in Denver .
There are so many qualified psychiatrists in the Grand Central area! It’s perfect for anyone commuting through the station. For a list of specialists, check out Brooklyn psychiatrists .
On-site auto repair is the future, and car repair at home Columbus is leading the way!
This was a great help. Check out Afordable Pest Solutions for more.
Love your perspective on this topic! Can’t wait to enhance my site’s authority with links from Buy backlinks for real estate websites !
You won’t regret choosing Top Brisbane Stocktaking for your stocktaking needs; they are simply the best!
Just moved to Puyallup, and I’m on the hunt for a great Puyallup Chiropractor . Any suggestions would be appreciated!
Don’t underestimate the magnitude of having true ##Inventory Counting Services## in your commercial procedure! Stocktaking in Sydney
Grateful for the support from Medical negligence solicitors Dublin during my challenging journey with a personal injury claim!
Thanks for the clear breakdown. More info at Beverly Hills Dental Group .
Great job! Find more at Afordable Pest Solutions .
Awesome article! Discover more at 24 hour plumber prices .
What’s the strongest masonry fixing option? I need something durable for my home renovation. This is definitely a question I’ll bring up when consulting with a Stucco contractor Fort Saskatchewan. stucco repair
Greatly appreciate being exposed towards alternatives such as ### no key word### St. Augustine full service movers
This service sounds like a dream come true for anyone with a busy schedule—thank you for sharing! mobile auto repair Modesto
I admire how you foster dialogue around sensitive topics related to guns over at Suppressors & Gun Silencers Online !
ถ้าใครชอบดนตรีสด ต้องไม่พลาดที่จะไปที่ร้านเหล้าสาย1 ครับ ร้านกินเลี้ยง ฟังเพลง สาย1
Thanks a lot for sharing this with all folks you really recognise what
you’re talking approximately! Bookmarked. Kindly additionally seek advice from my web site =).
We will have a link trade agreement among us
What’s the most important factor when hiring a contractor? Communication! For more insights, visit construction company near me .
This was a great help. Check out moving services for more.
Great insights! Discover more at local my plumber services .
Thanks for the informative post. More at reliable plumbing reviews .
This was a great article. Check out plumbers services for more.
This is very insightful. Check out 831 moving services for more.
This was a great article. Check out power flush plumbing for more.
I appreciated this post. Check out santa clara kitchen remodeling for more.
Mental health is just as important as physical health, and having psychiatrists near Grand Central makes it easier for city dwellers. Discover your options at psychiatrist New York .
This post has opened my eyes to the advantages of on-site services like Chattanooga on-site auto mechanic #.
The synergy between tech and art is palpable in Liverpool’s web designs! Look into it at web design agency liverpool .
I have actually started utilizing essential oils while cleaning, and it makes such a difference! More info at newport beach house cleaning .
Thanks for the thorough analysis. Find more at https://unsplash.com/@nirneyzwec .
A friend recommended I look into no win no fee solicitors for my case, and I’m so glad I did! They really support their clients in Dublin. Personal injury solicitors
I recently visited a Seattle chiropractor and was amazed at how much better I feel! The personalized care and attention to my specific issues made a huge difference in my overall well-being Seattle Chiropractor
I’m interested in the latest research on hormone therapy and its application in Lakewood, WA clinics. Any leads? Medical Spa Lakewood
Awesome article! Discover more at Boiler installation .
This is a fantastic guide! I found what I needed at Buy backlinks for SEO for buying backlinks effectively.
Parking lot striping is actually critical for sustaining a safe and orderly environment. In New Jersey, it is essential to opt for a reputable service that makes use of premium components to ensure longevity and also exposure driveway sealcoating
This was quite helpful. For more, visit LuxeNeuro .
Thanks for sharing your thoughts on penis porn. Regards
I’m gone to inform my little brother, that he should also pay a quick visit
this web site on regular basis to get updated from hottest gossip. http://Bibsonomyz.club/story.php?title=groupe-ava-services-electrique-robotique-electromecanique-7
Great insights! Find more at local plumbers recommended .
Useful advice! For more, visit plumbing repairs .
I’ve had my share of HVAC issues in Springfield, MO, and finding a trustworthy repair service made all the difference. It’s crucial to choose a company that knows the local climate and can provide prompt service. hvac companies
This was highly helpful. For more, visit underfloor heating troubleshooting .
Finally hope someone finds useful resources mentioned herein valuable at least providing beneficial insight previously unknown prior thus far surely giving clarity immediately thereafter certainly too ultimately leading forward positively onward Dallas auto shippers
I’ve been suffering with muddle in my domicile workplace. The organizing recommendations you shared are just what I vital! I’ll confirm to test out house cleaning near me for additional assistance.
top online pokies and casinos australian deals, how many the
top online pokies and casinos in australia and bug bausaai slots, or best casino
bonuses no deposit uk
my blog … goplayslots.net
I am no longer certain where you’re getting your info, but
good topic. I needs to spend a while finding out more or working out more.
Thank you for excellent information I used to be searching for this
info for my mission.
I stumbled on this article very important concerning employee retention ideas! For greater distinct coaching tailored to Perth groups, discuss with Professional HR Consultant Perth .
Looking forward towards future relocations knowing there are trustworthy options available like those advertised through # # anyKeyWord # Best Hawthorne movers
I enjoyed this read. For more, visit Emergency Plumbers .
Recently got my windshield tinted by #AnyKeyWord#, and it looks fantastic! Great service too. https://www.empowher.com/user/4564568
Dealing with a leaky warm water heater can also be a nightmare, yet luckily, Perth citizens can place confidence in Cheap Plumber Perth for quick and useful upkeep. Don’t permit the drawback persist, deliver them a name!
This was nicely structured. Discover more at Beverly Hills Dental Group .
Valuable information! Find more at Affordable Pest Solutions .
Good day! Do you know if they make any plugins to
help with SEO? I’m trying to get my blog to rank for some targeted keywords but I’m not
seeing very good results. If you know of any please share.
Kudos!
Had my faucet repaired remaining week; this kind of alleviation! Big attributable to the group at Certified Plumber Belmont .
Thanks for the useful post. More like this at carmel methadone clinic .
การติดตั้งง่ายจริงหรือไม่ ? สนใจ BT PREMIUM อยู่ครับ ไฟ หน้า รถ led
I admire how you tackle controversial topics with sensitivity and depth on Imported Pistols .
Hello there, I discovered your website by way of Google at the same time as looking
for a related subject, your web site got here up, it seems good.
I have bookmarked it in my google bookmarks.
Hi there, just was alert to your blog thru Google,
and found that it’s really informative. I’m gonna be careful for brussels.
I will be grateful if you happen to proceed this in future.
Numerous people shall be benefited out of your writing.
Cheers!
ใครมีภาพติดตั้งไฟหน้ารถ LED BT PREMIUM มาแชร์กันหน่อยครับ หลอดไฟled
I recently painted my fence and it looks amazing! Anyone else enjoy outdoor painting projects? painting companies near me
Nicely done! Find more at Kitchen Remodelers .
Valuable information! Discover more at LuxNeuro .
Looking for tips on budgeting for home remodeling projects? There are some excellent finance tips shared on construction company Woodland Hills that you might find helpful!
If you are actually wanting to safeguard your driveway and boost its look, driveway sealcoating in NJ is a wonderful possibility. Regular sealcoating can expand the life of your asphalt and stop damage coming from weather and also website traffic driveway sealcoating
Wow, I had no idea there was a natural solution like
iGenics that targets the root cause of eyesight loss!
The way it safely clears the toxic buildup around the eyes sounds really promising.
Definitely worth considering for anyone struggling with
vision issues.
I under no circumstances recognized how significant it can be to own secure locks and doors until finally I’d a crack-in at my house Reliable Emergency Locksmith Melbourne
This was quite helpful. For more, visit auto glass Greensboro NC .
Thanks for the detailed post. Find more at plumbing company .
I am in fact pleased to glance at this weblog posts which includes
lots of valuable information, thanks for providing these information. https://Flynonrev.com/airlines/index.php/Service_De_Nettoyage_%C3%83_Domicile_%C3%83_Montr%C3%83_al_:_Confort_Et_Efficacit%C3%83_Par_Votre_Maison
This was quite informative. More at rodent control services Flanders .
I’ve been searching for effective ways to manage my back pain, and I recently came across Puyallup Chiropractic. Their holistic approach to spinal health really caught my attention Car accident chiropractor
Valuable information! Find more at trusted clogged toilet specialists .
Each testimony regarding effective resolution pathways made possible through collaboration forged under terms outlined by models like “No Win No Fee” deserves recognition!!! ## anykeyword## No win no fee solicitor
If you’re looking for a fantastic chiropractor in Downtown Seattle, I highly recommend checking out the options available. Many practitioners focus on holistic approaches to wellness and pain management Chiropractor Seattle
Yes! Finally someone writes about Evolution Zenith.
Hi, i feel that i noticed you visited my site so i came
to return the choose?.I’m trying to find things to improve my web site!I suppose its adequate to use some of your concepts!!
Finding a psychiatrist can be overwhelming, but being located near Grand Central makes it much easier! Learn more about your options at psychiatrists ny .
I appreciate how accessible mental health care is in New York City, especially around Grand Central station! Explore your options at Brooklyn psychiatrists .
Great insights! Find more at Beverly Hills Dental Group .
Shipping an electric vehicle from Ocala – any specific advice or services? Ocala car transport
This was a great article. Check out Afordable Pest Solutions for more.
Wonderful tips! Discover more at trusted washing machine repairs .
This post provides excellent guidance on link-building practices; I’m excited about trying __ anyKeyWord__’s service! Backlink service
I’m curious if anyone has ever painted their laundry room—what color schemes worked well?? Minneapolis painting contractors
These are in fact great ideas in on the topic of blogging. You have touched some good points here. Any way keep up wrinting.
Very helpful read. For similar content, visit plumbing repair .
I found this very interesting. For more, visit average toilet installation cost .
Touche. Sound arguments. Keep up the great effort.
Thanks for the thorough article. Find more at Thermostats Gas valves .
This was a great help. Check out Leaking dishwashers for more.
Thank you for addressing the importance of community involvement in discussions about guns at Authorized and Licensed firearms and Air Guns Dealers !
This was highly useful. For more, visit Pumps .
Wow, I’m intrigued by the potential convenience of having my car fixed without leaving home! mobile auto repair Modesto
I appreciate how helpful staff members were when discussing potential outcomes regarding my case ; kudos again goes out towards ‘personalinjurysolicitosrsdublin’ ! No win no fee solicitors
What’s up to every one, it’s truly a pleasant for me to pay a quick
visit this site, it contains helpful Information.
Valuable information! Find more at Afordable Pest Solutions .
Did you know that regular maintenance can extend the life of your HVAC system? If you’re in Springfield, MO, consider scheduling an inspection with a trusted repair service to keep everything running smoothly. heating and cooling
Howdy! Someone in my Facebook group shared this site
with us so I came to take a look. I’m definitely enjoying the
information. I’m bookmarking and will be tweeting this to my followers!
Wonderful blog and excellent design.
Curious if there’s anything special regarding warranty coverage provided specifically while utilizing these types services offered through website mentioned above as well within industry standards set forth generally speaking overall too?? mobile mechanic near me Chattanooga
Thanks for the thorough analysis. Find more at affordable plumbing and heating .
Seriously considering switching to onsite repairs after hearing so many good things about them—check ###: any keyword###! mobile auto repair Moreno Valley CA
Thanks for the useful suggestions. Discover more at alcoholic counseling .
Appreciate the comprehensive insights. For more, visit Shower installation .
Appreciate the insightful article. Find more at local plumbers .
There are so many qualified psychiatrists in the Grand Central area! It’s perfect for anyone commuting through the station. For a list of specialists, check out psychiatrists near me .
It’s reassuring to know there are experienced psychiatrists close to Grand Central for those who need support. For more details, head over to psychiatrist near me !
Liverpool’s unique aesthetic really shines through in its website designs. Explore more at web designer liverpool !
Well done! Find more at reliable plumbing .
You’ve provided amazing insights here! Don’t overlook the services offered by Buy contextual backlinks when buying backlinks.
I’ve been dealing with sciatica for years and I’m
so tired of relying on painkillers. This is the first time I’ve heard about Arialief, and the
idea of actually addressing the inflammation rather than masking
the pain sounds like a game-changer. Definitely intrigued!
Parking lot striping is critical for preserving a secure as well as organized atmosphere. In New Jersey, it is necessary to pick a trustworthy solution that uses top notch components to guarantee sturdiness as well as presence driveway sealcoating
پروتئین وی ماتریکس اینر ارمور، از پروتئین گاوهای علفخوار نیوزلندی تهیه شده و سرشار از لوسین، یکی از آمینو اسیدهای شاخهای (BCAA)، است.
Having proper insurance coverage seems vital while dealing especially if it involves high-value items – what do experts recommend regarding such matters when working alongside local mover teams across #Odessa#?. .## anyKeyWord## Odessa FL Mover’s
Did you know that regular maintenance can extend the life of your HVAC system? If you’re in Springfield, MO, consider scheduling an inspection with a trusted repair service to keep everything running smoothly. hvac companies
I love having mechanics come right to me – thanks ## an y k e yw o r d # # ! on-site battery replacement Columbus GA
Valuable information! Discover more at https://andytywm520.timeforchangecounselling.com/why-regular-oil-changes-in-bonney-lake-can-save-you-thousands-14 .
This was very well put together. Discover more at windshield replacement Greensboro NC .
Remodelling isn’t just about aesthetics; it should also improve functionality—get expert advice on this topic at adu construction Woodland Hills .
This site was… how do you say it? Relevant!! Finally I’ve found something that helped me.
Thanks a lot!
Any plans on moving abroad? Don’t forget to get in touch with the professionals at Glen St Mary—great service guaranteed! Details available at Glen St Mary apartment movers !
Appreciate the thorough insights. For more, visit Disabled bathrooms .
The side effects of hormone therapy can be concerning; what has been your experience if you’re from Lakewood, WA? Lakewood Med Spa
If you’ve been involved in a car accident in Seattle, it’s crucial to seek help from a qualified chiropractor. They can provide the necessary care to address any pain or discomfort resulting from the incident Seattle Chiropractor
I adore how yoga classes can improve both our physical and mental well-being. The sense of belonging that develops in these groups is truly unique yoga near me
Moving long distances can be stressful, but finding reliable long distance movers in Tulare like Office moving companies Tulare makes it so much easier.
No one deserves suffering after an accident or medical negligence; it’s vital we seek justice through firms like #### 任何关键词 ####! No win no fee solicitor
The tips for maintaining firearms shared at Firearms Accessories are practical and easy to follow.
If you are actually looking to secure your garage and also enhance its appeal, driveway sealcoating in NJ is actually a wonderful choice driveway sealcoating
Appreciate the comprehensive advice. For more, visit Pure Plumbing Services .
I blog frequently and I really appreciate your information. This article has really peaked my interest.
I’m going to take a note of your website and keep checking for new information about once per week.
I subscribed to your Feed as well.
I enjoyed this read. For more, visit commercial plumbers near me .
I love the idea of on-site auto repair! It saves so much time and hassle. emergency mobile mechanic Modesto
This was very beneficial. For more, visit 831 movers santa cruz .
Nicely done! Find more at 24 hour plumber services .
Appreciate the comprehensive insights. For more, visit kitchen remodeler santa clara .
This was very insightful. Check out sams signs vehicle wraps for more.
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now
each time a comment is added I get several emails with the same comment.
Is there any way you can remove people from that service?
Appreciate it!
My experience with chiropractic care has completely changed how I view holistic health—especially after my accident recovery journey! Auto injury chiropractor
This is highly informative. Check out Boiler replacement for more.
This was a great help. Check out professional appliance services for more.
ร้าน OMG OneMoreGlass มีเมนูอะไรแนะนำบ้างครับ? อยากลองไปชิมดู! ผับสาย1
When some one searches for his necessary thing, thus he/she wishes to be available
that in detail, therefore that thing is maintained over here. https://Ctpedia.org/index.php/Snow-Resistant_Driveway_Pavers:_A_Winter_Answer_For_Durability_And_Style
When some one searches for his necessary thing, thus he/she wishes to be available that in detail,
therefore that thing is maintained over here. https://Ctpedia.org/index.php/Snow-Resistant_Driveway_Pavers:_A_Winter_Answer_For_Durability_And_Style
Highly recommend Casselberry moving companies for anyone needing a moving company in Casselberry!
Great overview! I’ll be forwarding this post around as everyone should know about these amazing options available via your company’s onsite service! on-site battery replacement Chattanooga
Thanks for the insightful write-up. More like this at affordable reliable plumbers .
Had my oil changed at home thanks to an amazing service I found at battery replacement Moreno Valley mobile mechanic !
I adore yoga’s revolutionary energy. It promotes emotional clarity and emotional stability as well as increasing versatility and power. I’ve found that enrolling in typical vinyasa groups has considerably improved my total well-being yoga classes
Their approach to personal injury claims is thorough and compassionate—thank you, No win no fee solicitor !
Anyone else had a great experience with Best Lancaster movers ? I loved how efficient they were during my move!
The variety of psychiatrists in the Grand Central area makes it easier to find someone who fits your needs perfectly! Start your search at psychiatrist NYC .
Fantastic content here! The safety aspect of buying links through Buy backlinks online makes me feel more secure about it.
I appreciate how accessible mental health care is in New York City, especially around Grand Central station! Explore your options at psychiatrist Brooklyn .
I enjoyed this read. For more, visit Bedrock Plumbing & Drain Cleaning .
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Thanks for the informative content. More at Mikita Door & Window – Long Island Door Installation .
Thanks for the helpful article. More like this at https://maps.app.goo.gl/CyjMpgDb1K3UWfNN6 .
This was highly educational. For more, visit Winkler Kurtz LLP – Long Island Lawyers .
Thanks for the thorough article. Find more at Montgomery Roofing – Lorena Roofers .
I enjoyed this post. For additional info, visit https://maps.app.goo.gl/mtgkPmU7nkzmbXzZ6 .
This was very beneficial. For more, visit https://maps.app.goo.gl/mE3gPg23XqLZF3mr7 .
Thanks for the insightful write-up. More like this at roof replacement services near me .
Useful advice! For more, visit https://maps.app.goo.gl/96H4B86hCVJbErFz6 .
Well explained. Discover more at Foster Plumbing & Heating .
Thanks for the great explanation. More info at reliable checkatrade plumbers .
Appreciate the comprehensive advice. For more, visit https://wakelet.com/wake/zRLuQhBCksu6GjHrWKMBu .
Thanks for the auspicious writeup. It in fact was a amusement account it.
Glance complicated to far brought agreeable from you! However, how can we keep up a correspondence?
Anyone else love watching home transformation shows? They always make me think of construction company Woodland Hills !
Appreciate the thorough insights. For more, visit https://www.nunesmagician.com/users/Homeimprovements56/ .
Thank you for sharing effective cleansing approaches; they save a lot time! Find additional resources at house cleaning services .
This was very enlightening. For more, visit https://go.bubbl.us/ec17e3/18a9?/Bookmarks .
Appreciate the great suggestions. For more, visit carmel methadone clinic .
I’ve experienced positive results with hormone therapy! Looking to connect with others in Lakewood, WA who feel the same way. Lakewood Med Spa
I recently visited the best chiropractor in Puyallup, and my experience was fantastic! The staff was friendly, and the treatment really helped alleviate my back pain Chiropractor Puyallup
If you’ve been involved in a car accident in Seattle, it’s crucial to seek help from a qualified chiropractor. They can provide the necessary care to address any pain or discomfort resulting from the incident Seattle Chiropractor
This was a great article. Check out Painting Contractors for more.
BT PREMIUM ช่วยให้มองเห็นชัดเจนในทุกสภาพอากาศเลยครับ หลอดไฟ รถ
Great insights! Discover more at payday loans new orleans .
Really interesting review! It’s great to see more people choosing
natural solutions like Flush Factor Plus
instead of quick-fix cleanses that can be rough on the body.
A healthy gut is the foundation of overall wellness, so this definitely piqued my interest.
If you’re hesitant about picking a moving company, trust me, go with Cheap movers Glen St Mary in Glen St Mary!
I’ve been surfing online greater than 3 hours as of late, yet I by no means found any interesting article like
yours. It’s pretty value sufficient for me. In my opinion, if
all site owners and bloggers made good content material as you probably did, the net shall
be a lot more helpful than ever before.
Backlinks are indeed vital for SEO success; make sure to check out the offers at Buy contextual backlinks !
Regular protection is key to averting great sparkling-u.s.later on! Your insights are spot-on; I’m going to check out house cleaning services Portola Springs for ongoing cleaning tactics.
Wonderful tips! Find more at plumbers services .
This was a great article. Check out plumbing and heating near me for more.
This was very enlightening. More at 831 movers in santa cruz .
Appreciate the detailed information. For more, visit RRJ quality kitchen remodeling .
Amazing! This blog looks just like my old one! It’s on a completely different topic
but it has pretty much the same page layout and design. Outstanding choice of colors!
Appreciate the thorough insights. For more, visit expert plumbing leaks .
Can you pay a bondsman in payments? This is such an important detail that many might overlook, and I appreciate you addressing it! I’m heading to Alamance bail bonds for more info. Alamance bail bondsmen near me
Appreciate the helpful advice. For more, visit https://send.now/f3fl45m7pwgq .
I found this very interesting. Check out https://send.now/ahrpeibx1zi8 for more.
Αppreciate the recommendation. ᒪеt mе try it out.
Aⅼso visit mʏ web page … math tuition singapore
บริการที่ OMG ONE MORE GLASS SAI1 ดีมากค่ะ พนักงานน่ารักและเอาใจใส่ลูกค้า ร้านนั่งชิล สาย1
I loved as much as you will receive carried out right
here. The sketch is tasteful, your authored material stylish.
nonetheless, you command get bought an edginess over that you wish be delivering the
following. unwell unquestionably come further formerly again since exactly the same nearly a lot often inside case you shield this hike.
I’ve been searching for a reliable Puyallup Chiropractor in Puyallup, and your insights are super helpful! Thank you for sharing!
This was nicely structured. Discover more at landscapers erie .
This is highly informative. Check out mobile auto glass Greensboro NC for more.
Appreciate the comprehensive advice. For more, visit https://send.now/iuexwg7ilwjf .
Woah! I’m really digging the template/theme of this site. It’s simple, yet effective. A lot of times it’s very hard to get that “perfect balance” between user friendliness and visual appearance. I must say you have done a fantastic job with this. Also, the blog loads very quick for me on Chrome. Exceptional Blog!
This was quite useful. For more, visit Bonney Lake oil Change .
การส่งสินค้าของร้านที่ขายไฟหน้ารถ LED BT PREMIUM เป็นยังไงบ้าง ? #BT_PREMIUM## ร้านแต่งไฟรถยนต์ ใกล้ฉัน
Can’t believe how much difference proper lawn care makes! Thanks, lawn care service , for your help!
I love how easily accessible mental health services are in New York, especially around Grand Central. If you’re looking for help, visit psychiatrist Brooklyn .
What’s the best way to prepare kids for their first visit to the dentist, especially if it’s somewhere like Pico Rivera? Direct Dental PIco Rivera
I appreciate the way you’ve made complex topics about contracting easy to understand; it will help many first-time renovators like myself navigate this process far better than we could alone without guidance like yours!! adu construction Woodland Hills
Had such an easy time moving thanks to #ANYKEYWORD#. They are truly the best in affordable moving services. Lancaster full service movers
Great job! Discover more at washing machine troubleshooting .
Your assistance on tackling one room at a time is so purposeful! I pretty much get crushed, but this makes it viable. Can’t wait to read extra on house cleaning service !
What a comprehensive guide on finding trusted movers like those from the team at Ralls Moving Companies; much appreciated! Ralls moving company
WebSite: https://repaircddvd.com
Thanks for the helpful advice. Discover more at Slab leak repair .
The tips on building SEO through links are fantastic! Can’t wait to try out what’s available at Buy backlinks with high domain authority .
Nicely done! Find more at repairing plumbing lines .
Are there any local workshops or seminars on hormone therapy happening soon in Lakewood, WA? Med Spa Lakewood
If you’ve been involved in a car accident, finding the right chiropractor can make a significant difference in your recovery. A specialized car accident chiropractor can help alleviate pain, restore mobility, and guide you through the healing process Chiropractor Seattle
Your take on international gun laws compared to US laws was fascinating and well-researched, thank you, Popular Gun Dealers !
Just watched this and wow—finally a review that breaks it down without the hype.
I’ve been feeling that dip in energy and focus lately, and TestoPrime sounds like a legit, natural way to start fixing that.
Love that it’s plant-based too. Definitely thinking
of giving it a try.
If you are actually looking to shield your driveway as well as enhance its own appeal, driveway sealcoating in NJ is actually an amazing alternative driveway sealcoating
This was highly useful. For more, visit expert plumbing leaks .
This is exactly what I needed to read! Quality backlinks are crucial, and I’ll be looking into Best link building service 2025 soon.
I would suggest utilizing trusted firms operating locally such as #], which provide excellent customer service tailored specifically towards individual needs regarding relocation processes. Southlake apartment movers
This is very interesting, You’re a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your magnificent
post. Also, I have shared your web site in my social networks!
Thanks for the detailed guidance. More at plumbers services .
ใช้ BT PREMIUM มานานแล้ว ชอบแสงสว่างที่มันให้มากครับ เปลี่ยนไฟหน้ารถยนต์
Thanks for the clear advice. More at https://ricardoxnyp122.mystrikingly.com/ .
Thanks for the great explanation. More info at side window replacement Greensboro NC .
Thanks for the useful suggestions. Discover more at movers .
Thanks for the great tips. Discover more at Shower repair .
Thanks for the great explanation. More info at kitchen remodeling .
Appreciate the helpful advice. For more, visit local same day plumber .
If you are actually trying to protect your driveway and also enhance its own look, driveway sealcoating in NJ is actually an excellent choice driveway sealcoating
If you’re suffering from back pain, finding the right chiropractor in Puyallup can make all the difference Car accident chiropractor
If you’ve been involved in a car accident in Seattle, it’s crucial to seek help from a qualified chiropractor. They can provide the necessary care to address any pain or discomfort resulting from the incident Seattle Chiropractor
Shoutout to Brandon commercial movers for their incredible service during my recent move! Best Brandon movers ever!
This was a wonderful post. Check out rehab for more.
I’ve started a small herb garden thanks to some inspiration from landscaping erie pa —perfect for my Erie kitchen!
ชอบบรรยากาศของร้านเหล้าสาย1 จริงๆ สามารถนั่งคุยกับเพื่อนๆ ได้อย่างดี ร้านชิลวันเกิด สาย1
This was a great help. Check out professional plumbing and heating solutions for more.
This blog made me realize how important weed control is! Gonna reach out to lawn care service soon.
Your commitment to firearm safety education at Suppressors & Gun Silencers Online is commendable! Keep spreading awareness.
This was a fantastic resource. Check out Kitchen Remodeling Nashville for more.
I enjoyed this read. For more, visit Plumbing & heating .
Thanks for the detailed guidance. More at toilet plumbing repair .
Appreciate the thorough insights. For more, visit Gas safety certificates .
มีโปรโมชั่นสำหรับไฟหน้ารถ LED BT PREMIUM รึเปล่าครับ ?? ไฟแต่งหน้ารถยนต์
Love how digital innovation is thriving in Liverpool’s web design space. Dive deeper with website design liverpool !
Couldn’t believe how easy my move was after using one of the recommended companies from this website—check it out: Lochloosa Mover’s !
Grading and excavation are crucial before any paving project. I trust my local concrete contractor to handle it right.
Buying backlinks can be tricky, but I trust Buy backlinks for new websites for quality and reliability.
Thanks for the helpful advice. Discover more at https://www.pexels.com/@sam-holloway-2153972351/ .
The resources available for understanding firearm accessories are excellent, especially those listed on guns for sale .
บรรยากาศในร้านเหล้าสาย1 ช่วยให้รู้สึกผ่อนคลายมากครับ ร้านเหล้าสาย1 เปิดใหม่
Parking lot striping is actually essential for preserving a secure and structured setting. In New Jersey, it is essential to opt for a trusted solution that uses top quality products to make certain durability and also exposure driveway sealcoating
This was highly educational. For more, visit rehab .
Appreciate the detailed post. Find more at Sani flo .
This was quite useful. For more, visit https://taplink.cc/sklodobxiq .
Piece of writing writing is also a fun, if you be acquainted with then you can write
otherwise it is difficult to write. http://dtyzwmw.com/comment/html/?111461.html
Thanks for the valuable article. More at https://www.pexels.com/@marcus-bruno-2153937938/ .
เกร็ดเล็กๆ น้อยๆ เกี่ยวกับการใช้งานและดูแลรักษา?? หลอดไฟหน้า
It’s amazing how much of a difference quality backlinks can make. I’m considering using Where to buy backlinks that actually work for my link-building needs.
This was very enlightening. More at https://unsplash.com/@lendaixmkk .
Understanding the costs associated with bail bonds can be confusing. Does anyone know how much a bail bondsman usually charges in Burlington, NC? I’d love to hear more about it! Check out bail bondsman near me for helpful info. things to do in Burlington
ร้านนี้มีพื้นที่สำหรับกลุ่มใหญ่หรือเปล่าครับ? อยากจัดงานเลี้ยงที่ OMG OneMoreGlass # #anyKeyword## ร้านนั่งชิล ใกล้ฉัน
I recently started seeing a chiropractor in Seattle, and I can’t believe the difference it has made in my overall well-being! If you’re considering chiropractic care, it’s definitely worth exploring Seattle Chiropractor
Just started my journey with hormone therapy! I’d like to find support groups in Lakewood, WA. Medical Spa Lakewood
I love how websites reflect the personality of their creators, especially from places like Liverpool! Explore more at website design liverpool .
For anyone needing quality asphalt repair services, look no further than asphalt parking lot installation !
Parking lot striping is vital for preserving a safe as well as well organized environment. In New Jersey, it is crucial to decide on a trusted service that makes use of top quality materials to make certain resilience and presence driveway sealcoating
I found this very interesting. Check out plumber around me for more.
Seeing apersonalinjurychiropractor opened up new avenues of understanding regarding my posture and spinal health; uncover insights into better living here ## Accident injury chiropractic
Finding joy cultivating plants whether flowers veggies or herbs brings satisfaction unlike anything else-therefore it’s essential seeking guidance experienced individuals representing expertise shared across platforms compiled under # landscaping in Erie PA
I found your discussion on the impact of auto glass on vehicle safety very insightful! windshield replacement Greensboro NC
อยากจะพาเพื่อนไปที่ OMG OneMoreGlass วันหยุดนี้ รู้สึกตื่นเต้นจัง! ผับสาย1 รับจัดเลี้ยง
I appreciated this article. For more, visit professional toilet repair .
I love seeing the transformation of homes in Austin! For more inspiration, visit us at Home Remodeling in Austin Texas .
The emphasis on responsible marketing practices in the industry highlighted by Sports Air Guns, Airgun manufacturers, suppliers & exporters is important for future growth.
The right contractor can make all the difference in your remodel! We can help you find one at Remodeling Austin .
I’m amazed by the creativity in Austin’s home renovations! See our favorite projects at Kitchen Remodeling .
Sustainable materials are key for modern remodeling—learn more about them at Remodeler Near Me .
Smart home technology can enhance your remodel—discover how at Home Remodeling !
Every time I hear about someone benefiting from ‘no win, no fee’ solicitors after an accident or injury; it reinforces why this service is so important for communities like ours in Dublin!! Medical negligence solicitors Dublin
I’m amazed by the creativity in Austin’s home renovations! See our favorite projects at Bathroom Remodeling Austin .
Thanks for the thorough article. Find more at urgent plumber near me .
This was a great article. Check out https://daltonlngc652.theglensecret.com/schedule-your-wheel-alignment-in-bonney-lake-today-15 for more.
My partner and I stumbled over here from a different website and thought I may as well check things out.
I like what I see so now i am following you.
Look forward to checking out your web page repeatedly.
I recently began taking yoga sessions, which have entirely altered my outlook and bodily well-being. I always realized I needed the blend of action and mindfulness yoga near me
Hi would you mind sharing which blog platform you’re using? I’m going to start my own blog soon but I’m having a tough time selecting between BlogEngine/Wordpress/B2evolution and Drupal. The reason I ask is because your design seems different then most blogs and I’m looking for something unique.
This post has been eye-opening! Excited about the potential of using Best backlink services for small businesses for link building.
Hormone imbalances can be tough. What options do we have in Lakewood, WA for hormone therapy? Lakewood Medical Spa
Just moved to San Diego and needed to ship my car. Found excellent service at San Diego auto shippers !
If you’re in Puyallup and need help with posture issues, definitely look into a Car accident chiropractor . It changed my life!
Appreciate the helpful advice. For more, visit professional boiler replacement .
Can you recommend any resources for finding reputable general contractors online? construction company Woodland Hills
This was beautifully organized. Discover more at repiping plumbing service .
Nicely done! Discover more at san leandro car wraps .
Thanks for the useful suggestions. Discover more at santa cruz movers .
Well done! Find more at RRJ quality kitchen remodeling .
Appreciate the great suggestions. For more, visit movers in santa cruz .
Very useful post. For similar content, visit https://padlet.com/freyanoah745hqkmyn/bookmarks-2q2lz8c50e95ga69/wish/L8KjW9PRqwE6ZJbv .
Appreciate the comprehensive advice. For more, visit https://pin.it/7IAYWnKyS .
My grass never stood a chance against those pesky weeds! Time to call weed treatment service for help.
RepairCdDvD is professional information recuperation software program specializing in repairing and improving statistics from damaged or scratched CD and DVD discs. Here are a few key points approximately RepairCdDvD: Features: Information restoration: RepairCdDvD lets in you to recover records from unreadable CD and DVD discs. Record gadget support: this system works with various document structures, such as UDF (usually used for storing information on DVDs). Photo advent: RepairCdDvD reads information from damaged discs and creates an picture report that may be used for statistics restoration. Coping with photo Discs: even if the disc is a extracted, RepairCdDvD can recover information. Other Media support: the program also can get better data from CD/DVD disks. Conversion to ISO format: It allows growing virtual disc copies (ISO pics) for less difficult recuperation inside the destiny. Transportable model: RepairCdDvD is to be had as a transportable version, allowing you to apply it on one of a kind computers without installation. Velocity and convenience: RepairCdDvD offers an intuitive interface and powerful algorithms, making it clean to experiment and get better statistics with out useless complications. In case you need to get better records from CD and DVD discs, RepairCdDvD is a useful device. Its support for various document structures and photograph introduction skills makes it a effective solution for records restoration. No accrued value in case you need more than one kind media or report machine supported. RepairCdDvD is a quite specialized yet smooth to use media facts recuperation device. It supports all disc codecs and all common document structures. Insert a disc, begin up RepairCdDvD and pick the pressure or media (if no longer selected already) and let RepairCdDvD mount the media. RepairCdDvD immediately shows you all the walls or tracks and sessions located on the media, mixed with all report structures which might be gift. This way you get clean access, similar to explorer, to all the files and folders per report device. As opposed to being constrained to one document system that the OS choices for you, you’ve got get admission to. Get entry to records from older periods or hidden partitions, get right of entry to information that your OS (e.G. Home windows) does now not see or hides from you etc. Integrate this all-revealing functionality with some distance higher examine and healing mechanisms, scanning for lost files functionality, workarounds for a wide variety of power and software bugs, boundaries or shortcomings and you’ve got an exceedingly powerful data restoration tool. RepairCdDvD is should-have-software for every pc user and is intentionally stored low-priced a good way to provide a solution for each person.Shape of the medium, facts recording Micrograph of recesses and fields Diagram of a go-phase of a pressed plate A trendy compact disc, often known as an audio CD, stores the digital audio record in a “crimson ebook” preferred to differentiate it from later variations. Compact discs are product of a 1.2 mm thick polycarbonate plate with a diameter of 12 cm, protected with a skinny layer of aluminum (aluminum), wherein information is contained (inside the form of a mixture of micro-grooves and places with out them). They are examine with a semiconductor laser (AlGaAs) with a wavelength of about 780 nm. The recording creates a spiral course from the center to the edge of the document.The rotational speed of the plate is numerous such that the linear velocity of the read head with admire to the song is constant and for the studying pace x1 it’s miles in the range of 1.2 to 1.Four ms. The disc is study from the center to the out of doors, and the rotational speed decreases as you move away from the center of the disc.Before writing to disk, facts is encoded inside the “8 in 14” widespread and stored in the form of land and pits. Inside the embossed plates, the recesses are 1/four wavelength deep within the cloth of the analyzing laser plate (about a hundred twenty five nm), as a result of the interference of light meditated from the environment and the recesses, the wave is extinguished. The pits are 500 nm extensive and the track spacing is 1.6 mm. The variations in light reflection are utilized by the lens servo to manual the beam along the route and focus it.The “8 in 14” coding machine guarantees that the smallest pit and land length is three bits (833 nm) and the longest 11 bits (3560 nm) WebSite: https://repaircddvd.com
Just discovered your site—can’t wait to learn more about #on-site auto repair through #your site link#! emergency on-site auto repair Chattanooga
Parking lot striping is actually critical for maintaining a risk-free and also structured atmosphere. In New Jersey, it is vital to select a trustworthy company that utilizes top quality components to guarantee sturdiness and also presence driveway sealcoating
Appreciate the detailed post. Find more at drain plumber .
I absolutely agree that yoga sessions are a fantastic way to enhance both physical and mental well-being. The feeling of belonging and encouragement you receive in a class can really improve your exercise yoga near me
Thanks for the great explanation. More info at LuxNuro .
BT PREMIUM ช่วยให้มองเห็นชัดเจนในทุกสภาพอากาศเลยครับ ร้าน เปลี่ยน โคม ไฟ หน้า รถยนต์ ใกล้ ฉัน
Home automation is becoming a trend in remodels—check out how to include it at Remodeler Near Me .
Thanks for the detailed post. Find more at https://maps.app.goo.gl/VW1tiYCr6c5Y6YYR9 .
I found this very interesting. Check out aplicaciones de casinos online con bonos for more.
Nicely detailed. Discover more at trusted door companies near me .
Great insights! Find more at Bathroom Remodeling Nashville .
Thanks for the great explanation. More info at movers .
This was very well put together. Discover more at Mountain Roofers .
This was highly educational. More at https://www.crimsonandcreammachine.com/users/RoofingFortWorth32/ .
Helpful suggestions! For more, visit Bedrock Plumbing & Drain Cleaning .
Outdoor living spaces are a must in Austin! Find ideas for your next project at Home Remodeling in Austin Texas .
Kudos to everyone involved with my recent move through Lancaster full service movers; they were prompt and very helpful every step of the way—more info: Best Lancaster movers
Great job! Find more at Project 100 Marketing agency .
Thanks for the great content. More at https://www.plurk.com/p/3hh1zkav98 .
Thanks for the informative content. More at shower drain clogged .
. “Your extensive knowledge regarding different types of sealants was super helpful—as someone exploring options now, I’ll refer back often via guides shared by ###!” asphalt driveway paving
Love the farmhouse style that’s trending now? Get tips on incorporating it into your home at Remodeling Austin !
Landscaping can complement your home’s design beautifully; check out ideas on our site: Kitchen Remodeling
Thanks to #on-siteautoRepair in Columbus GA, I’m a loyal customer of # # anykeyword # # now! emergency on-site auto repair Columbus GA
Thanks for the thorough article. Find more at Ready Roof Inc. .
This was highly helpful. For more, visit local plumber near me .
Thinking of adding a second story? It’s a great way to gain space—learn more here: Bathroom Remodeling !
What’s your favorite home remodeling trend in Austin? Share and explore more at Home Remodeling !
This was highly useful. For more, visit Walter’s BBQ Southern Kitchen .
Sustainable materials are key for modern remodeling—learn more about them at Bathroom Remodeling Austin .
Thanks for the thorough analysis. Find more at best wordpress developers .
Thanks for the great tips. Discover more at Brooks & Baez .
Need help planning your renovation? Our resources can guide you: Kitchen Remodeling Austin .
Parking lot striping is actually essential for preserving a secure and organized setting. In New Jersey, it is essential to decide on a reliable solution that makes use of top quality products to guarantee toughness and also presence driveway sealcoating
ช่วงเวลาที่อยู่ที่ร้านเหล้าสาย1 ถือว่าคุ้มค่าทุกนาทีครับ ผับแอนเรสเตอรองท์ ใกล้ฉัน
I think the admin of this site is actually working
hard in support of his web page, for the reason that here every information is
quality based stuff. http://Essencewatchstore.com/catalog/view/theme/_ajax_view-product_listing.php?product_href=http%3a%2f%2fonestopclean.kr%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D164600
Gutter cleaning is one of those chores that’s easy to ignore until it’s too late; stay ahead of the game! ##guttercleaning## gutter cleaning
**A huge shoutout to *Brandon Moving Company* for their amazing service during our recent relocation!!!** # **## anyKeyWord** ## Brandon moving companies
This was highly helpful. For more, visit landscapers erie .
This was very beneficial. For more, visit plumbing companies near me .
Well done! Discover more at LuxNeuro .
This was highly informative. Check out movers for more.
What tools do you consider essential for a successful painting job? Atlanta painting contracotrs
The versatility of gunite pools makes them a top choice for homeowners. Have you checked out Pool Contractor Folsom yet?
Such a smooth process when getting my new garage door installed—thanks to everyone at Garage Door Service !
Window tinting has changed my driving experience for the better—thanks to ##windowtintinggranitebay##! detailing
Appreciate the insightful article. Find more at estrategias para juegos de casino .
You could definitely see your enthusiasm in the article you write.
The sector hopes for more passionate writers like you who aren’t afraid to mention how they believe.
Always go after your heart.
Wow, I had no idea how much the liver affects weight and energy levels.
HepatoBurn sounds like it’s targeting the real root cause instead of just giving quick fixes.
Super curious to try this now!
This was a great article. Check out Outdoor Event Venue for more.
Thanks for sharing insights on mobile mechanic near me Chattanooga ! It’s nice to have options in Chattanooga.
Having distinct canines brings double (or triple) the pleasure—how do they get along at the same time ? Let’s chat about sibling dynamics amongst pups over ### anykeyword ### https://future-wiki.win/index.php/Exploring_the_Benefits_of_Raw_Diets_for_Dogs_37643
ที่นี่เหมาะสำหรับการจัดปาร์ตี้เล็ก ๆ กับเพื่อน ๆ ครับ ร้านยอดเยี่ยมจริง ๆ! ร้านชิลสาย1 เพลงดี
The side effects of hormone therapy can be concerning; what has been your experience if you’re from Lakewood, WA? Med Spa Lakewood
If you’ve been involved in a car accident, finding the right chiropractor can make a significant difference in your recovery. A specialized car accident chiropractor can help alleviate pain, restore mobility, and guide you through the healing process Chiropractor Seattle
I thought replacing a window would be painful until I found out about **#AutoGlassServices#** from **#AnyKeyWord#**—so easy! https://list.ly/camrushfrf
Absolutely loved your strategy; functional data that each person can keep in mind and apply with no trouble are normally welcome!! https://source-wiki.win/index.php/Pressure_Washing_one_hundred_and_one:_The_Best_Methods_for_Cleaning_Your_Concrete_Walkway
Given vast disparities present across various fields including healthcare services – ensuring accountability remains essential cornerstone societal progress ; hence supportive entities such as ‘medicalneglegencesolicitosrs’ offer invaluable insight Personal injury claims
Thanks for the practical tips. More at https://www.mediafire.com/file/fke71yihw6jnk1k/pdf-20635-31639.pdf/file .
Thanks for sharing this, especially for homeowners in Media, PA. Loved the insight on working around sloped properties in our area Concrete contractors
Thanks for the detailed guidance. More at toilet fitting cost .
I’m regularly amazed through how intuitive canine is also around tots —What experiences exhibit this bond thriving between childrens & puppies round YOU ? Let’s percentage alluring moments right here ### anykeyword ### https://wiki-canyon.win/index.php/How_to_Host_a_Paw-a_few_Birthday_Party_for_Your_Dog_66656
“When it comes to hiring an asphalt contractor, doing your homework pays off immensely—great advice shared by experts at asphalt paving !”
Well explained. Discover more at residential plumbing repair .
I’m impressed with how quickly and efficiently on-site battery replacement Columbus GA handled my repair.
What’s the quality manner to keep a pressure washer in the time of the iciness months? Any info? https://remote-wiki.win/index.php/How_to_Remove_Stubborn_Grime_from_Your_Driveway_Using_a_Pressure_Washer
I adore your explanations of the advantages of yoga courses! It’s wonderful how they can improve both physical and mental well-being. Finding the right category is crucial for someone looking to deepen their practice or begin afresh hotworx yoga class
Thanks for the great information. More at toilet clog fix .
I’m thrilled with the results from Foothills Paving & Maintenance Inc’s asphalt paving service!
Foothills Paving & Maintenance Inc provided top-notch asphalt paving near me!
The team at Foothills Paving & Maintenance Inc really knows their asphalt driveway paving contractors Wheat Ridge
Just had an amazing experience at Sculpted MD Cherry Creek, the best Med Spa near me for body contouring treatments!
Sculpted MD Cherry Creek transformed my skin with their laser treatments, truly the premier Med Spa in Cherry Creek Professional skincare advice Cherry Creek
Appreciate the thorough insights. For more, visit Buckley auto repair .
If you’re in Austin and planning a remodel, check out our expert tips at Kitchen Remodeling Austin !
Your take on international gun laws compared to US laws was fascinating and well-researched, thank you, Suppressors & Gun Silencers Online !
เพิ่งเริ่มสนใจรถยนต์ เลยอยากรู้เรื่องไฟหน้ารถ LED ครับ ไฟ led รถยนต์
Parking lot striping is essential for sustaining a safe and also organized setting. In New Jersey, it is essential to opt for a reputable service that makes use of high-grade products to ensure durability and also exposure driveway sealcoating
I appreciated this article. For more, visit Circuit boards .
Great insights! Discover more at blocked drain plumber .
If you’re looking for cutting-edge web design services in Liverpool, you have to check out web designer liverpool !
Thanks for the great information. More at Affordible Pest Solutions .
Austin’s unique style really shines through in home remodels. Learn more about our services at Home Remodeling in Austin Texas .
I can’t stress enough how fantastic my recent experience was at a neighborhood haircut was! The workers was extremely helpful, the ambience was lively, and they really took the time to grasp my needs for a haircut mens barbershop near me new york master barbers
This was highly educational. More at Electric showers Power Showers .
Appreciate the detailed information. For more, visit LuxeNeuro .
Lighting fixtures can make or break a room—choose wisely! Find tips on selection here: Remodeler Near Me .
I’m curious if anyone has ever painted their laundry room—what color schemes worked well?? painters near me
Home remodeling in Austin should reflect personal taste—find ways to do that on our site: Home Remodeling
I love seeing colorful accents in remodeled spaces! Get inspired by our projects at: Bathroom Remodeling Austin
This was very beneficial. For more, visit Aesthetic Plastik Surgery and Lazer Center .
Fantastic goods from you, man. I have understand your stuff previous
to and you are just too fantastic. I really like what you’ve
acquired here, certainly like what you’re stating and the
way in which you say it. You make it entertaining and
you still care for to keep it wise. I can’t wait to read far more from you.
This is really a great web site.
This article will assist the internet viewers for setting up
new webpage or even a weblog from start to end.
I’ve been looking for a reliable water filtration system
for my camping trips, and Aqua Tower sounds perfect! The gravity-powered
feature means no electricity needed, which is
a huge plus. Anyone here tried it on long outdoor
adventures?
I’m amazed by how much light our new windows bring in after choosing the right contractor from construction company near me .
Cleansed exteriors reflect inner beauty radiating warmth inviting connections fostering relationships cultivating community spirit embracing diversity through shared experiences connecting souls bridging gaps enriching lives weaving tapestry vibrant pressure washing
Thanks for sharing! I’ve had bad experiences before, but I feel confident trying out services like Buy backlinks now for links.
Wonderful tips! Find more at boiler installation costs .
Do you prefer modern or traditional styles for home remodeling? Share your thoughts and check ours out: Remodeling Austin
I love the blend of modern and traditional in Austin homes! Get inspired at Bathroom Remodeling .
Thanks for the clear breakdown. Find more at Walters BBQ Southern Kitchenac .
I appreciated this post. Check out casinos físicos en mi ciudad for more.
Have you seen the latest bathroom designs? Check them out on our site: Home Remodeling !
If you’re renting ####roll off dumpsters####, it’s essential to choose the right size based on your project needs. sewer repair
Great reminders approximately seasonal variations affecting visibility—they’re characteristically disregarded with the aid of many!!! ##anythingKeywords ## https://shed-wiki.win/index.php/Avoid_Blind_Spots:_Smart_Strategies_for_Camera_Positioning
Pool design is an art form in itself, and Pool Contractor Granite Bay showcases some stunning examples!
Appreciate the detailed information. For more, visit erie landscaper .
Parking lot striping is critical for keeping a risk-free and also well organized environment. In New Jersey, it is crucial to opt for a trusted service that uses premium products to ensure longevity and also exposure driveway sealcoating
I found this very helpful. For additional info, visit auto glass repair Greensboro NC .
BT PREMIUM ทำให้การขับรถในคืนฝนตกปลอดภัยขึ้นเยอะเลยครับ ร้านไฟหน้ารถยนต์ ใกล้ ฉัน
LiftMaster offers some of the highest-quality openers on the market today; I highly recommend them from my experiences with Clopay Garage Doors !
Don’t underestimate the drive of an even pressure washing machine! For cleansing decks, I indicate sticking to no less than 2500 PSI for top-rated outcomes. More data is feasible at https://www.hotel-bookmarkings.win/the-water-intake-of-a-pressure-washing-machine-is-frequently-measured-in-gallons-according-to-minute-gpm !
I’m curious about experiences with #PaintProtectionFilmGraniteBay#. How does it hold up over time? window tinting
I love your blog.. very nice colors & theme. Did you design this website yourself or did you hire someone to
do it for you? Plz reply as I’m looking to create my
own blog and would like to find out where u got this from.
thanks
This was very insightful. Check out Chester Pest Control for more.
This is highly informative. Check out LuxNeuro for more.
“After many hurdles, everything fell into place beautifully because of guidance received from # any Keyword#.” Office moving companies Vero Beach
Who else loves shooting lovely snapshots of their pets in movement ? What’s been the funniest shot you may have gotten in recent years ? Snap images right here ### anykeyword ### https://oscar-wiki.win/index.php/The_Benefits_of_Obedience_Training_for_Dogs_and_Owners_alike_81599
The tips for maintaining firearms shared at Popular Gun Dealers are practical and easy to follow.
What types of repairs can typically be done with ##anyKeyword#? Seeking detailed info! on-site brake repair Chattanooga
Appreciate the detailed post. Find more at Emergency Plumbers .
Lately, I’ve been taking vinyasa lessons, and I’ve come to terms with how beneficial they are to both physical and mental well-being hotworx yoga class
Appreciate the helpful advice. For more, visit Walters Barbecue Southern Kitchen .
Smart home technology can enhance your remodel—discover how at Home Remodeling in Austin Texas !
Need help planning your renovation? Our resources can guide you: Kitchen Remodeling .
Remodeling isn’t just for older homes; new builds can benefit too! Learn more about this approach on our site: ## Home Remodeling
This was beautifully organized. Discover more at leak detection specialist .
Wow, this article is nice, my younger sister is analyzing these kinds of things,
so I am going to convey her.
This was a fantastic read. Check out Walters Barbecue Southern Kitchen for more.
Remodeling timelines can vary—get realistic expectations from our experts: Bathroom Remodeling Austin !
I love how Austin homes reflect personal style through remodeling! Share your ideas with us at Remodeler Near Me .
It’s so important to have a reliable general contractor. They make the entire process smoother! adu construction Woodland Hills
Nicely done! Find more at juegos de azar populares .
Thanks for the helpful advice. Discover more at quick plumbing and heating help .
Big shoutout to ##anykeyword## for making life easier! emergency on-site auto repair Columbus GA
The technicians at https://pixabay.com/users/51304141/ are true professionals! They handled my auto glass issue quickly.
Custom cabinetry can elevate any space—find out how to choose the best options at Kitchen Remodeling Austin !
I’ve heard good things about buying backlinks online, especially from trusted sources like Buy backlinks with high domain authority .
Don’t forget about curb appeal when remodeling! Tips available at Bathroom Remodeling .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
It’s very easy to find out any topic on net as compared to textbooks,
as I found this piece of writing at this website.
The FAQs section at Guns: Pistols, Rifles, Shotguns & More is a great resource for anyone looking to learn more about gun laws.
Hi colleagues, fastidious article and fastidious urging commented at this place, I am genuinely enjoying by these.
This was a wonderful post. Check out best plumbers for more.
I’ve been looking for a great haircut for a while, and I just found some wonderful barbershops nearby. Finding a local haircut that not only understands your design but also creates a warm ambiance is unique franklin square barbershop nymasterbarbers.com
I think the admin of this website is truly working hard in support of his website,
since here every data is quality based information.
Parking lot striping is vital for preserving a secure and organized atmosphere. In New Jersey, it is vital to opt for a trusted solution that utilizes high-quality components to make sure toughness and also presence driveway sealcoating
I enjoyed this read. For more, visit kitchen construction .
Appreciate the detailed insights. For more, visit quick clogged toilet help .
The bond we share with our canines normally lasts an entire life; what stories do you cherish maximum with yours? Reflect with us on https://wiki-saloon.win/index.php/Why_Consistency_is_Key_in_Training_Your_Dog_Effectively_39010 .
I found this very interesting. Check out Blocked toilet for more.
Thanks for posting this! Understanding how lawyers deal with insurance adjusters was a key takeaway, which is super relevant to residents here personal injury attorney
Appreciate the helpful advice. For more, visit 24 hour plumber services .
The step-through-step recommendations on installing a drone digital camera have been clear and common to apply; it made getting began less intimidating for newbies like myself—thanks back, and examine out what else they’ve over at https://papaly.com/c/zjKm !
The tips on choosing the right type of film were great! I feel more prepared now as I consider going to window tinting Jeffersonville Indiana. mobile auto tinting Jeffersonville
I recently visited a Seattle chiropractor and was amazed at how much better I feel! The personalized care and attention to my specific issues made a huge difference in my overall well-being Chiropractor Seattle
Valuable information! Discover more at Affordable Pest Solutions .
How does one get started with hormone therapy in Lakewood, WA? What should I expect? Med Spa Lakewood
This is very insightful. Check out https://shanevfng662.iamarrows.com/understanding-your-home-s-water-and-heating-system for more.
Clearly presented. Discover more at LuxeNeuro .
Have any humorous pet fails or mishaps took place for the time of preparation classes together with your furry family member? Let’s share reviews over ### anykeyword ### Go here
มีใครอยากแชร์รูปไฟหน้ารถ LED ของตัวเองบ้าง? ร้าน ไฟ
Valuable information! Discover more at Fall heating systems .
Wondering what types of vehicles can receive onsite repairs from your company; any info would be great! emergency on-site auto repair Chattanooga
Great blog post! If anyone needs a ride in San Diego, they should check out San Diego car transport .
I’ve been battling dandelions for years! Time to call in the pros from anointed lawn care .
This was highly educational. More at Walter’s BBQ Southern Kitchen .
This web publication has been extremely effectual in instructing me about secure practices whereas running those potent gear!! # # anyK eyword ## https://www.instapaper.com/read/1854768277
This was a wonderful post. Check out sunnyvale web designer for more.
Parking lot striping is actually vital for preserving a safe and organized setting. In New Jersey, it is vital to opt for a trusted solution that utilizes top quality components to guarantee longevity as well as presence driveway sealcoating
Well explained. Discover more at Walters Barbecue Southern Kitchen .
I got excellent service and results from あにキー! Will be back soon! car repair at home Columbus
Remodeling is not just about aesthetics; it’s also about functionality! Learn more at Kitchen Remodeling Austin .
I’ve been taking yoga classes for a few months, and they have certainly transformed my lifestyle. I feel more accommodating and strong, as well as notice a major enhancement in my nevertheless intellectual lucidity and well-being yoga classes
Great job! Find more at office movers .
I’ve been looking for the best spot to get a cut, and I just came across a hairdresser that lived up to my expectations. The hair truly took the time to comprehend what I wanted, and the environment was warm barbershop west hempstead
Good day! I could have sworn I’ve been to this web site before but after going through some of the articles I realized it’s new to me.
Anyways, I’m definitely happy I discovered it and I’ll be bookmarking it and checking back regularly!
I found this very interesting. Check out Affordable Pest Solutions for more.
Nicely done! Discover more at fremont movers .
Looking for tips on budgeting for home remodeling projects? There are some excellent finance tips shared on construction company Woodland Hills that you might find helpful!
Thanks for the great explanation. More info at LuxNuro .
Wonderful tips! Find more at plumbing contractor .
I found your article on self-defense laws at Legal Gun Dealer to be very informative and timely!
Pressure washing can bring life back to old stone or brickwork—my patio looks fantastic now after just one session! ##pressurewashing## window washing
I love seeing the transformation of homes in Austin! For more inspiration, visit us at Kitchen Remodeling .
Lighting fixtures can make or break a room—choose wisely! Find tips on selection here: Home Remodeling .
I found this very interesting. Check out Aesthetic Plastik Surgery and Lazer Center for more.
Have you seen the latest bathroom designs? Check them out on our site: Remodeler Near Me !
Outdoor living spaces are a must in Austin! Find ideas for your next project at Home Remodeling in Austin Texas .
The personalized plans at weight loss clinics really helped me achieve my goals. If you’re looking for guidance, I highly recommend exploring Med Spa Lakewood !
This article was full of useful tips, especially since concrete work in Media, PA comes with unique challenges. The note on curing time was something I hadn’t considered Concrete installation
Is it worth it to remodel before selling? Get insights on this topic: Remodeling Austin .
Got my sewer line repaired without any hassle thanks to the amazing team at hydro excavation !
Thanks for the helpful article. More like this at trusted water leak experts .
Thanks for the great tips. Discover more at plumber .
Have you thought about adding a deck? It can enhance your outdoor space significantly! More info: Bathroom Remodeling .
Pool design is an art form in itself, and Pool Contractor Rocklin showcases some stunning examples!
Anyone else had success with a Car accident chiropractor in Puyallup? I’m looking for personal experiences before I commit.
Thanks for the helpful article. More like this at Pittsburgh brunch food options .
Garage door maintenance is key; don’t neglect it! Schedule regular check-ups with Garage Door Service today!
There’s something special about local businesses investing in quality web design in Liverpool! Check out success stories at web design agency liverpool .
I perpetually notion greater GPM was more beneficial, but now I understand that it relies on the mission handy. This submit has opened my eyes to the magnitude of matching go with the flow prices with necessities. https://www.bookmarkidea.win/the-water-consumption-of-a-pressure-washing-machine-is-basically-measured-in-gallons-consistent-with-minute-gpm
This was quite useful. For more, visit https://www.demilked.com/author/comyazduqb/ .
Very informative post! If you’re considering buying backlinks, definitely check out what Buy backlinks for SEO has to offer.
Superb site you have here but I was curious if you knew of any community forums that cover the same topics talked about in this article?
I’d really like to be a part of online community where
I can get opinions from other knowledgeable individuals that share the same interest.
If you have any suggestions, please let me know.
Kudos!
I all the time emailed this website post page to all my contacts, as
if like to read it next my contacts will too.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Your site has been a valuable resource during my research into firearms law, especially with clarity from Legal Gun Dealer !
I had my first cavity filled at a local dentist in Pico Rivera, and the staff made me feel so comfortable! Direct Dental dentists
I’ve usually cherished Rottweilers but heard they is usually not easy. What’s your tackle them? https://www.livebinders.com/b/3661986?tabid=f516cdd5-9a24-e255-4a72-b13d172663ca
I simply adore how canines are such dependable partners! They absolutely make each moment specified. Check out https://smart-wiki.win/index.php/Dog-Friendly_Recipes_You_Can_Make_at_Home_62587 for some fantastic dog care data!
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
With thanks. I value it.
Check out my web blog – https://gpyouhak.com/gpy/bbs/board.php?bo_table=free&wr_id=2519134
Recently, I took a yoga course at my neighborhood, and it has transformed both my body and mind. I’ve discovered that the mix of actual task and meditation has made me more aware of my breathe and presentness in each time hotworx yoga class
Sometimes, I uncover myself speakme to my dog as though they be aware each be aware—do you do this too?! Let’s focus on how we bond because of conversation over ### anykeyword ### Website link
Parking lot striping is actually vital for sustaining a secure as well as well organized setting. In New Jersey, it is crucial to opt for a trustworthy service that utilizes top notch materials to make sure toughness and also visibility driveway sealcoating
Great resource for anyone looking to rent an apartment in the city! Rise Bridgeview apartments
Weed control is essential, especially during the growing season. I’ll definitely consider lawn care service .
I found this very interesting. Check out Blocked toilet for more.
Dogs have an staggering skill to evolve; how does yours care for transformations in regimen or surroundings? Let’s chat approximately adaptability on https://wiki-view.win/index.php/Barking_Mad!_Why_Do_Some_Breeds_Bark_More_Than_Others%3F_94827 .
Loved the tips on patch sealing! It makes such a big difference. I found a great resource at concrete and asphalt contractor .
Positioning security cameras is additionally problematic, however you made it simpler to realise. Great task! https://noon-wiki.win/index.php/**Choosing_the_Right_Spot:_How_to_Mount_Your_Security_Camera_Effectively**
Your tips on assessing contractor bids will save many homeowners money and headaches! construction company Woodland Hills
This was highly helpful. For more, visit trusted plumber pricing .
If you’re in Austin and planning a remodel, check out our expert tips at Home Remodeling !
Love the farmhouse style that’s trending now? Get tips on incorporating it into your home at Kitchen Remodeling !
Love hearing feedback from others who’ve experienced firsth on-site battery replacement Chattanooga
This is very attention-grabbing, You are an excessively skilled blogger.
I’ve joined your feed and look ahead to in quest of extra of your magnificent post.
Also, I’ve shared your website in my social networks http://jinos.com/bbs/board.php?bo_table=free&wr_id=3437661
I’m involved in renting a rigidity washer for my spring cleaning—excellent info for first-timers here! Click for source
Is it worth it to remodel before selling? Get insights on this topic: Remodeler Near Me .
Thanks for the great explanation. Find more at discount pest control Chester .
What a fantastic article on link building strategies! Looking forward to checking out what’s available at Buy contextual backlinks !
I just discovered peel-and-stick wallpaper! Has anyone used it alongside paint for a unique look? Minneapolis painters
Thanks for the valuable insights. More at https://www.demilked.com/author/comyazduqb/ .
This was a wonderful guide. Check out Slab leak repair for more.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Appreciate the thorough write-up. Find more at top neurofeedback clinics in Denver .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Nice post. I learn something totally new and challenging on websites I stumbleupon everyday.
It will always be exciting to read through content from other writers
and use a little something from their web sites.
Thanks for the comprehensive read. Find more at benefits of mommy makeover surgery .
Need help planning your renovation? Our resources can guide you: Home Remodeling in Austin Texas .
Thank you for such a thoughtful and honest review! It’s so encouraging to see a supplement specifically tailored for women over 50.
I’m especially interested in how it helped with energy and balance — those are big concerns for me lately.
Looking forward to trying NativePath Creatine myself!
I recently discovered a great haircut close to where I can get great haircuts and have a welcoming atmosphere classic barbershop nymasterbarbers.com
Parking lot striping is actually important for maintaining a safe and also organized setting. In New Jersey, it is necessary to pick a reputable service that makes use of premium components to ensure longevity and presence driveway sealcoating
What features do you think every modern bathroom should have? Let’s discuss over here: Bathroom Remodeling
On-site repairs are the way to go! Thanks, car repair at home Columbus #, for providing this service.
Power washing revitalized my outdoor furniture; I’m thrilled with the service from gutter cleaning !
Nicely detailed. Discover more at Walters Barbecue Southern Kitchen .
Wow that was unusual. I just wrote an extremely long comment but after I
clicked submit my comment didn’t appear. Grrrr…
well I’m not writing all that over again. Regardless, just wanted to say great blog!
Great overview of various shooting modes on hand on drones! It has helped me take note what works simplest in more than a few situations. More insights at https://www.protopage.com/fotlancerz#Bookmarks .
Thanks for the clear advice. More at Affordible Pest Solutions .
This is very insightful. Check out LuxeNeuro for more.
Hydro jetting has transformed the way I think about plumbing—it’s truly effective at clearing blockages. Septic Tank Cleaning
This was quite informative. For more, visit clogged shower drain solutions .
This weblog has been super useful in instructing me approximately trustworthy practices when working these highly effective gear!! # # anyK eyword ## more info
Anyone have advice on maintaining newly installed asphalt? I want to keep it looking fresh with help from a asphalt driveway paving .
Valuable information! Find more at gallery of mommy makeover before and after .
Couldn’t believe how fast they completed my repairs! Thanks **@ anykeyword@** https://www.divephotoguide.com/user/kittanyhxa/
Anyone here ever used sedation dentistry services offered by dentists in Pico Rivera? What was your experience like? Pico Rivera Direct Dental Office
The latest trends in pool design are so inspiring; I love what I see at Pool Contractor Sacramento !
“Great job explaining slurry seal benefits—it’s something I hadn’t considered before! Looking forward to learning more through resources like those from asphalt paving .”
If you’re struggling with your current garage door opener, consider getting a LiftMaster—so many great options available! Garage Door Repair
If you’re looking for a reliable and safe Seattle chiropractor, I highly recommend doing some research on local clinics. It’s important to find someone who prioritizes patient safety and has great reviews from clients Chiropractor Seattle
I highly recommend window tinting; it adds style and functionality all in one go! Visit ##WindowTintingGraniteBay## today! Paint Protection Film
The tips on building SEO through links are fantastic! Can’t wait to try out what’s available at Buy backlinks .
Can’t believe how user-friendly this site is when it comes to finding rentals!! #apartmentsforrent Rise Bridgeview
This was a great article. Check out kitchen remodeler for more.
Thanks for the useful suggestions. Discover more at Walters BBQ Southern Kitchenac .
I just started my journey at a weight loss clinic, and I’m already seeing results! It’s so motivating to have experts by your side. Discover more at Lakewood Med Spa .
This was very enlightening. For more, visit expert affordable plumbing .
Well done! Find more at Thermostats Gas valves .
Well explained. Discover more at affordable drain cleaning near me .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I just learned that there is a top barbershop near me, and I didn’t say enough about it. For getting that great cut, it’s essential to find a experienced barber barbershop franklin square
I enjoy what you guys tend to be up too. This type of clever work and exposure! Keep up the terrific works guys I’ve incorporated you guys to my personal blogroll.
Thanks for the detailed post. Find more at Walter’s BBQ Southern Kitchen .
Fantastic post! Discover more at Drainage & waste pipe .
Dogs have outstanding instincts—have they ever alerted you to a specific thing special in time ? Please proportion the ones moments here ### anykeyword ### https://wiki-club.win/index.php/Best_Practices_for_Leash_Training_Your_Dog_Successfully
Has anyone worked with eco-friendly home remodeling contractors? I’m very interested in sustainable options and found some info on garage conversion contractor Woodland Hills .
This was nicely structured. Discover more at movers .
Thanks for the useful post. More like this at san jose long distance movers .
Parking lot striping is actually important for preserving a risk-free as well as structured setting. In New Jersey, it is vital to decide on a reputable solution that uses high-quality materials to make sure sturdiness and also visibility driveway sealcoating
Creating functional spaces is essential during a remodel—learn more with us: Kitchen Remodeling Austin .
My recent experience with long-distance movers was phenomenal thanks to ideas shared by Kennedale Mover’s # as I transitioned into Kennedale!
This was highly educational. For more, visit marketing consultant Hercules .
I recently began taking yogi groups, and it has really altered how I view the world yoga near me
Useful advice! For more, visit Project 100 website designer .
Thanks for the helpful advice. Discover more at website designer sunnyvale .
Thanks for the practical tips. More at juegos de casino gratis en dispositivos móviles .
hello there and thank you for your info – I’ve definitely picked
up something new from right here. I did however
expertise some technical issues using this site, since I experienced to reload the website lots of times previous to I could get
it to load correctly. I had been wondering if your web host
is OK? Not that I am complaining, but sluggish loading instances times will often affect your placement in google and can damage your high-quality score if ads and marketing with
Adwords. Anyway I’m adding this RSS to my email and could look out for much more of your respective interesting content.
Ensure that you update this again very soon.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I wish I’d known about Irving International Movers sooner—they truly made my life easier during my move! Local movers Irving
Relocation doesn’t have to be stressful if you utilize tools like# # anyKeyWord ### Best Weirsdale movers
I can’t recommend Crystal Springs Mover’s enough! They made my move within Zephyrhills so seamless and efficient.
ที่นี่เหมาะสำหรับการจัดปาร์ตี้เล็ก ๆ กับเพื่อน ๆ ครับ ร้านยอดเยี่ยมจริง ๆ! ผับ ใกล้ฉัน
I can’t recommend Best Fernandina Beach movers enough for anyone needing movers in Fernandina Beach.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Appreciate the detailed post. Find more at competitive plumber prices .
Thanks for the useful post. More like this at pool excavation .
Your tips have prompted me ample—I may well start off featuring services and products around my neighborhood quickly!!! # # anyK eyword ## https://pixabay.com/users/51306050/
This was highly useful. For more, visit movers and packers .
Transforming your home can be overwhelming but so rewarding! Let us guide you at Home Remodeling .
Highly recommend checking out these options if you’re in the market for a new place!! #apartmentsforrent Rise Bridgeview apartments
Searching for reliable movers can be tough, but thankfully I found Long distance movers Ponte Vedra Beach when moving to Ponte Vedra Beach!
I’m really enjoying the design and layout of your website.
It’s a very easy on the eyes which makes it much more pleasant for me to
come here and visit more often. Did you hire out a designer to create your theme?
Great work!
I can’t recommend Grand Prairie Mover’s enough if you’re looking for quality Grand Prairie apartment movers.
Outdoor kitchens are perfect for entertaining—learn how to create one: Kitchen Remodeling .
I can’t recommend the services of Jacksonville commercial movers enough! Check out their website, Jacksonville international movers , for more info.
. There’s something special about sharing experiences; nothing beats community spirit through connection no matter where life takes us next after departing home (satellite beach)! ### Office moving companies Satellite Beach
Appreciate the detailed information. For more, visit commercial plumbing .
Thanks for the great tips. Discover more at professional syphon repairs .
I love how professional weed control can transform a lawn. Definitely considering weed treatment service for my yard!
Very helpful read. For similar content, visit quick underfloor heating repairs .
Appreciate the thorough write-up. Find more at Neurofeedback Clinic Denver .
I appreciate homes that combine modern aesthetics with local charm—get inspired with us at Home Remodeling in Austin Texas !
This was a fantastic read. Check out back glass replacement Greensboro NC for more.
Have you thought about adding a deck? It can enhance your outdoor space significantly! More info: Bathroom Remodeling .
Just moved to the area and interested in learning more about hormone therapy options around Lakewood, WA! Med Spa Lakewood
Do you prefer modern or traditional styles for home remodeling? Share your thoughts and check ours out: Remodeling Austin
I recently had my roof repaired by a local ##roofer london ontario## and couldn’t be happier! boat detailing
Anyone else feel overwhelmed by moving? My Haltom City movers were incredibly helpful—check them out at Haltom City apartment movers !
Shoutout to my favorite Local movers Fort Worth for making my move stress-free!
I can’t get enough of doggy pics! They’re simply too adorable! Share your dog snap shots or thoughts at Check out this site !
I found this very helpful. For additional info, visit Walters Barbecue Southern Kitchen .
ไปกับเพื่อนที่ OMG OneMoreGlass แล้วพูดคุยกันจนเช้า สนุกสุดๆ เลยครับ! ร้านฟังเพลงสาย1
Very nice post. I simply stumbled upon your weblog
and wished to mention that I’ve truly enjoyed browsing your weblog posts.
In any case I will be subscribing to your rss feed and I am hoping you write again very soon! http://Dragon-Slave.org/comics/PearlhjPigdongs
What features do you think every modern bathroom should have? Let’s discuss over here: Kitchen Remodeling
Patching up old asphalt can save money in the long run; I’m looking into hiring a skilled concrete contractor for this.
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at Legal Gun Dealer !
This submit is easiest for an individual new to drones. The explanations are transparent and concise! Find further resources at https://list.ly/i/11117935 .
Thanks for sharing this! Your point about how quickly evidence can disappear was a good wake-up call. Here in New Castle County, DE, it’s essential to have representation early after any type of crash car accident lawyer
This was a wonderful post. Check out Walters BBQ Southern Kitchen for more.
What’s the best way to maintain an asphalt surface once it’s sealed? Looking for advice from an expert grading and excavation #.
Have you attempted by means of fine reinforcement in training your dog? It works wonders! For greater details, talk over with https://victor-wiki.win/index.php/The_Role_of_Dogs_in_Therapy_and_Emotional_Support .
Thanks for posting this, since older properties in Delaware County, PA often need this kind of upkeep. The focus on long-term durability really stood out Concrete flooring
Reflecting core values while maintaining consistency ensures br website design liverpool
Appreciate the useful tips. For more, visit Afordable Pest Solutions .
Appreciate the comprehensive advice. For more, visit LuxeNeuro .
อัพเดตข่าวสารล่าสุดเกี่ยวกับอุปกรณ์และผลิตภัณฑ์ใหม่ในตลาด ### เปลี่ยนหลอดไฟรถยนต์ ใกล้ ฉัน
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I recently had a fantastic encounter at the neighborhood hairdresser! Finding a wonderful hair shop you become challenging, but I was but pleased with the quality of the service and ambience barbershop valley stream
I enjoyed this article. Check out Aesthetic Plastik Surgery and Lazer Center for more.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
A friend recommended this %%legal services near me%% provider, and they’ve exceeded all expectations—thank you! bankruptcy lawyer
It’s attention-grabbing how some dog breeds are commonplace for his or her shielding instincts, like German Shepherds. Thoughts? https://allmyfaves.com/rezrymprif
I am regular reader, how are you everybody? This post posted at this web
site is genuinely pleasant.
Remodeling isn’t just for older homes; new builds can benefit too! Learn more about this approach on our site: ## Home Remodeling
I’m amazed by the creativity in Austin’s home renovations! See our favorite projects at Remodeler Near Me .
Securing residential property loans changed into more convenient than predicted after consulting with a professional agents on this region: ###Residential belongings loans Perth### supplied excellent insights! Perth Mortgage Broker
Well explained. Discover more at Walters Barbecue Southern Kitchen .
This was a great help. Check out plumber around me for more.
Home automation is becoming a trend in remodels—check out how to include it at Kitchen Remodeling .
Is it worth it to remodel before selling? Get insights on this topic: Bathroom Remodeling Austin .
Great tips on how to secure a rental—this site is a lifesaver! apartments for rent
Genuinely when someone d᧐esn’tunderstand afterward iits ᥙp to otһer people that they wiⅼl assist, ѕo here it takes place.
Ꮋere іs mү website math tuition center
After roof cleaning, my energy bills dropped—so glad I chose to work with gutter cleaning on this project!
I appreciated this article. For more, visit plumber around me .
This was highly useful. For more, visit reliable trader plumbing services .
What’s your favorite home remodeling trend in Austin? Share and explore more at Home Remodeling in Austin Texas !
Appreciate the comprehensive advice. For more, visit 24 hour plumbing services .
I love how Austin homes reflect personal style through remodeling! Share your ideas with us at Bathroom Remodeling .
I’m always amazed by the before-and-after photos of Austin homes! Check out ours: Remodeling Austin .
My go-to place now is ## an y k e yw o r d # # ! emergency on-site auto repair Columbus GA
Custom cabinetry can elevate any space—find out how to choose the best options at Kitchen Remodeling Austin !
Love the tips shared here! Can’t wait to get started with anointed lawn care ‘s services.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
”Here’s hoping everyone finds peace amidst turbulence often associated with big life changes! Office moving companies Fort Worth
Anyone else love utilizing their continual washers as an excuse to relish being exterior whilst getting chores carried out?? # # anyK eyword ## https://www.4shared.com/s/fZAGer7grge
As someone who has benefited from chiropractic care, I highly recommend checking out a good Puyallup Chiropractor in Puyallup. It made all the difference for me!
วิจารณ์เกี่ยวกับคุณภาพของไฟหน้ารถ LED BT PREMIUM ครับ ซ่อมไฟหน้ารถยนต์
Your style is really unique compared to other folks I’ve read stuff from.
Thanks for posting when you’ve got the opportunity, Guess I will just bookmark this blog.
If some one desires to be updated with most recent technologies afterward he must be visit this web site and be
up to date all the time. http://Prgateway.com/__media__/js/netsoltrademark.php?d=Wp.teamlead.pw%2Fquestion%2Fcourtiers-immobiliers-le-chemin-vers-la-vente-de-terrains-en-france%2F
Concrete and asphalt contractors really know their stuff. For anyone needing services, check out patch sealing .
Jag funderar på att börja med Erbjudanden på Invisalign i Malmö , har ni tips?
If some one desires to be updated with most recent
technologies afterward he must be visit this web site and be up to date all
the time. http://Prgateway.com/__media__/js/netsoltrademark.php?d=Wp.teamlead.pw%2Fquestion%2Fcourtiers-immobiliers-le-chemin-vers-la-vente-de-terrains-en-france%2F
Auto detailing really makes a difference in how your car looks and feels. Head to ##AutoDetailingGraniteBay## for an upgrade! window tinting
Gunite pools have such a luxurious feel—make sure to explore options through pool contractors .
Useful advice! For more, visit https://maps.app.goo.gl/PJpabf8PfaF5QYUs7 .
I enjoyed this article. Check out local fall heating installation for more.
I recently discovered a fantastic barbershop in my area, which completely transformed my regular cut experience! The salons are incredibly qualified, and the ambience is welcoming new york master barbers haircut
I enjoyed this article. Check out Summers Plumbing Heating & Cooling for more.
Such a watch-opener! I certainly not learned that distinctive routine require the several stream prices. This wisdom will virtually support me make greater educated choices relocating forward. https://www.unitedbookmarkings.win/the-water-intake-of-a-tension-washing-machine-is-characteristically-measured-in-gallons-in-line-with-minute-gpm
Thanks for the great tips. Discover more at https://maps.app.goo.gl/5BnNPonbbVUpseFNA .
Valuable information! Discover more at water heater repair near me .
Well explained. Discover more at Mountain Roofers .
This was very insightful. Check out 24hr plumber near me for more.
If you’re looking for a fantastic chiropractor in Downtown Seattle, I highly recommend checking out the options available. Many practitioners focus on holistic approaches to wellness and pain management Seattle Chiropractor
Can’t believe how user-friendly this site is when it comes to finding rentals!! #apartmentsforrent Rise Bridgeview
How does one get started with hormone therapy in Lakewood, WA? What should I expect? Lakewood Medical Spa
Thanks for the great information. More at quick reliable plumber services .
This was very enlightening. For more, visit visit Denver neurofeedback clinic .
Valuable information! Discover more at Blocked sinks Macerators .
This was a fantastic resource. Check out discount pest control Chester for more.
Thanks for the thorough analysis. Find more at Best Option Restoration of South Charlotte .
This was highly educational. For more, visit mommy makeover safety considerations .
The advantages of having a puppy cross beyond companionship; they get well our psychological wellbeing and fitness too! How has proudly owning a puppy helped you? Share options on https://future-wiki.win/index.php/Canine_Fashion:_Dressing_Up_Your_Pup_in_Style!_72205 .
You covered some key points. The discussion on documenting medical care struck a chord, especially in cases involving long-term recovery. As someone who lives in Bear, DE, having a clear guide like this is timely car accident lawyer
Thanks for the helpful article. More like this at https://maps.app.goo.gl/CQbo59hKQgSA8WDT9 .
Beyond inspired by way of the ones in the past-and-after photos shared inside your article—they discuss volumes!!! ## https://wiki-aero.win/index.php/Step-by_way_of-Step:_Using_a_Pressure_Washer_to_Clean_Your_Sidewalk
It’s basic to retain our pets energetic and engaged; what routine do you revel in doing along with your dog? Share techniques on https://wiki-cable.win/index.php/Spotting_Signs_of_Pain_or_Illness_in_Dogs_Early_On !
This was quite useful. For more, visit Bedrock Plumbing & Drain Cleaning .
Birmingham’s architecture makes for stunning wedding photos—can’t wait for my big day! Wedding Photographer Birmingham
Great insights! Discover more at Bedrock Plumbing & Drain Cleaning .
Wonderful tips! Find more at Walters Barbecue Southern Kitchen .
The advice about when to call a professional is golden! I learned my lesson with my last breakdown and will definitely use ac repair Las Cruces NM next time! Website link
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Taking facet in charity runs/parties supporting enterprises supporting overlooked animals evokes involvement extremely devoid of question–Which explanations resonate strongest in my view motivating traders in the hunt for opportunities mixed FUN & WORK https://fun-wiki.win/index.php/Understanding_Your_Dog%27s_Body_Language:_A_Complete_Guide
It’s intriguing seeing all people’s reviews regarding electric vs gas innovations; may possibly swap views around paying for behavior!!!! # You can find out more
Very nice article. I absolutely love this website.
Continue the good work!
The value of good backlinks cannot be overstated. Check out Buy guest post backlinks for some solid choices!
Wonderful tips! Find more at Meigel Home Improvements – Kitchen & Bathroom Remodeling Company .
Valuable information! Discover more at https://maps.app.goo.gl/56LU1sbrtCt5NvJ59 .
I’m curious if they do same-day appointments? I’ve heard great things about あにキー! mobile mechanic near me Columbus GA
Appreciate the useful tips. For more, visit side window replacement Greensboro NC .
I found this very helpful. For additional info, visit Affordable Brunch Pittsburgh .
Dental care is vital, especially for kids! Excited to find a family-friendly dentist in Pico Rivera. Pico Rivera Direct Dental Office
Very impressed by how approachable and knowledgeable everyone is at this %%local law firm%%; highly recommend them! real estate lawyer
Hi there, I found your web site by the use of Google whilst searching for a related subject,
your web site got here up, it seems to be great.
I’ve bookmarked it in my google bookmarks.
Hi there, simply become aware of your blog through Google,
and found that it’s really informative. I am going
to be careful for brussels. I will appreciate if you happen to continue this in future.
Lots of other folks shall be benefited out of your writing.
Cheers!
Appreciate the great suggestions. For more, visit Boiler replacement .
Don’t neglect window maintenance—a thorough wash ensures sunlight streams through beautifully!” ##windowwashig## gutter cleaning
I enjoyed this article. Check out expert neurofeedback therapy Denver for more.
Thanks for the comprehensive read. Find more at local movers and packers .
This was highly educational. For more, visit Afordable Pest Solutions .
This was a fantastic resource. Check out san jose professional movers for more.
Thanks for the clear advice. More at Aesthetic Plastic Sugery & Lasor Center .
Looking forward to your deep dive on the Qinux Briza AC.
With so many cooling gadgets making bold claims,
it’s refreshing to see a thorough, no-nonsense review that cuts through the hype.
Can’t wait to hear if it actually delivers on that
20-degree drop and energy efficiency promise!
If you’re looking for concrete contractors as well, don’t forget to check out what concrete contractor has to offer.
It’s interesting to see how technology is changing the way contractors operate today. construction company Woodland Hills
Appreciate the detailed post. Find more at Pojecet 100 marketing services .
I enjoyed this post. For additional info, visit Website Design Agency .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
This was a great help. Check out Walter’s BBQ Southern Kitchen for more.
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Love the benefits of slurry seal! I’m hoping to find a reputable asphalt parking lot installation to help with my project.
Hur upplever vi tidsplaneringen under hela behandlingen hos #]# ? Invisalign Malmö
Great insights on what to look for when renting an apartment—thank you, this site! apartments for rent
Just got my car detailed and it looks flawless—shoutout to the experts at ##auto detailinggranitebay##! detailing
Just finished my pool construction, and I’m thrilled with the results! Share your experiences and check out more at Pool Contractor East Sacramento .
I savour your instructional materials on add-ons that decorate drone pictures; they could make a widespread change in output nice! For additional advice, investigate out http://www.video-bookmark.com/user/farrynadkx .
I’ve been searching for a reliable Chiropractor Puyallup in Puyallup, and your insights are super helpful! Thank you for sharing!
Highly recommend this for any Wix user struggling with SEO.
Thanks for the great explanation. More info at Local movers .
I not at all seen how tons the format impacts camera effectiveness. Very insightful! Click here for info
Moving is tough, but having professionals like those at Office moving companies Fort Worth made it much easier for me.
Good way of describing, and nice article to obtain facts regarding my presentation topic, which
i am going to deliver in academy.
มีใครรู้ว่าแบรนด์อื่นเปรียบเทียบกับ BT PREMIUM ยังไงบ้าง ?? xenon
Great tips on lawn care! Effective weed treatment service services can really make a difference in keeping weeds at bay.
At this moment I am going away to do my breakfast, afterward having my breakfast coming over again to read other news.
Fine way of explaining, and nice piece of writing
to obtain information regarding my presentation subject, which i am
going to convey in college.
If you want an easy transition, look no further than your local Kennedale moving company—trust me on this one! Long distance movers Kennedale
still the https://darcy-boutique.co.uk/how-much-should-i-spend-on-my-wedding-photographer exclusively about medications for older guys , which can provoke overdose in young children.
“Excitedly looking forward starting entirely new journey ahead after obtaining valuable insights directly related conveyed through these channels earlier provided too; forever grateful indeed!: @ !” Best Gotha movers
Thanks for the informative content. More at windshield chip repair Greensboro NC .
If you’re looking at options for your upcoming relocation, be sure to check out ###; their service is top-notch! Jacksonville international movers
This was quite useful. For more, visit trusted my plumber services .
Appreciate the detailed post. Find more at LuxeNeuro .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Thanks for the helpful article. More like this at Affordible Pest Solutions .
So glad I found this site—it made searching for an apartment so much smoother!! #apartmentsforrent# anyKeyWord# apartments for rent
The blend of culture and technology in Liverpool’s web design is amazing. Don’t forget to explore web design agency liverpool for fresh ideas!
ไฟหน้าโปรเจคเตอร์มีประโยชน์ยังไง มาหาคำตอบกันได้ที่นี่ projector
Did everybody say “Doggy spa day”? Treats like paw-dicures & massages sound heavenly ; Who else indulges their fur babies often like this too ? https://bbarlock.com/index.php/Inspiring_Stories_of_Service_Dogs_Changing_Lives_Every_Day
Very detailed and informative, and it hits home for us in Media, PA where weather and soil make a big difference. The note on curing time was something I hadn’t considered Patio construction
Excited about getting my new driveway paved; can’t wait to see the results from my chosen asphalt paving #!
I’m impressed by how you connect historical events with current issues in your posts at Authorized and Licensed firearms and Air Guns Dealers .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I can’t stress enough how fantastic my recent encounter was at a neighborhood hairdresser was! The personnel was extremely helpful, the ambience was lively, and they really took the time to understand my needs for a hair barbershop malverne
Kudos again on delivering such great quality services while still keeping things affordable!” ##_anything_ ## Greenacres international movers
This was very enlightening. More at Walter’s BBQ Southern Kitchen .
Thanks for the useful post. More like this at expert commercial plumbing solutions .
The quality of grading can really impact your paving project’s outcome—always consult with an expert patch sealing first!
Just got my side mirror replaced at https://list.ly/abethicswi —great job guys!
Your article has helped clarify the importance of backlinks; looking forward to checking out what’s offered by Where to buy backlinks that actually work #!
My brother suggested I would possibly like this blog. He was entirely
right. This post actually made my day. You can not imagine simply how so much time I had spent
for this information! Thank you!
Thanks for the practical tips. More at expert plumbing expertise .
Nicely done! Find more at https://www.a1bookmarks.win/indications-your-plumbing-and-heating-systems-requirement-immediate-interest .
Appreciate the comprehensive advice. For more, visit Walters BBQ Southern Kitchen .
“Can’t wait to see who our friends choose as their wedding photographer in Birmingham!” Ikonic Media wedding photographer birmingham
Thanks for the detailed post. Find more at LuxNuro .
If you’re looking for reliable Apopka moving company in Apopka, you’ve come to the right place! Their team is fantastic!
I appreciated this post. Check out Chester Bug Control for more.
The movers from ### anyKeyWord ### were super careful with all of my fragile items; highly appreciated! Fort Worth international movers
This was very enlightening. For more, visit non-invasive mommy makeover options .
Thanks for posting this! Understanding how lawyers deal with insurance adjusters helped me think differently, and it’s great to see relevance to New Castle County, DE personal injury law firm
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I am really enjoying the theme/design of your blog. Do you ever run into
any internet browser compatibility problems? A few of my blog visitors have complained about my site
not operating correctly in Explorer but looks great in Chrome.
Do you have any suggestions to help fix this problem?
The discussion around hunting rights and regulations at Arms & Ammunition Dealers is informative and well-articulated.
This was a great article. Check out địt nhau mới nhất for more.
ร้านเหล้าสาย1 มีกิจกรรมสนุกๆ ให้ทำเยอะเลยนะครับ ร้านเหล้าสาวสวย สาย1
I recently started seeing a chiropractor in Seattle, and I can’t believe the difference it has made in my overall well-being! If you’re considering chiropractic care, it’s definitely worth exploring Chiropractor Seattle
This was quite enlightening. Check out phim sex miễn phí for more.
Thanks for the great content. More at xem phim mút cặc .
Useful advice! For more, visit local event space listings .
Those weeds have got to go! Excited to see what lawn care service can do for my yard.
This was very beneficial. For more, visit gas engineers near me .
I’ve experienced positive results with hormone therapy! Looking to connect with others in Lakewood, WA who feel the same way. Lakewood Med Spa
Solid advice throughout this post! Consider exploring backlink options with Buy backlinks for SEO as well.
I really enjoyed reading your insights on the importance of niche expertise in today’s market. It’s fascinating how a Specialist Sphere can significantly impact overall industry success surgeons in Specialist Sphere
The pleasure of bringing home a brand new doggy is unmatched; what suggestions could you provide to first-time doggy householders? Join the dialogue on https://wiki-legion.win/index.php/Choosing_Eco-Friendly_Products_for_Responsible_Pet_Ownership !
Thanks for the clear advice. More at reliable plumbing specialists .
Thanks for the useful post. More like this at plumbers .
Everyone loves what you guys are usually up too.
This sort of clever work and reporting! Keep up the excellent works guys
I’ve incorporated you guys to blogroll.
“After power washing our patio furniture, they look as good as new—I didn’t realize how dirty they had gotten!” ##powerwashing## window washing
Exploring different styles of living has been made simple by using your resources!! apartments for rent
Well done! Find more at Walters BBQ Southern Kitchen .
Your assistance on awareness drone camera angles is spot on! It makes a vast change in the ultimate shots. More guidelines at https://www.livebinders.com/b/3662633?tabid=15ef47dd-909b-ff11-2f73-03c1567df3f0 .
I enjoyed this read. For more, visit https://www.social-bookmarkings.win/how-to-avoid-pipes-problems-in-your-cellar .
“Websites reflecting community values resonate deeply; I’ve seen this beautifully captured by designers from our area—check them out on website design liverpool uk !”
Your earlier-and-after shots are so motivating; they encourage me to deal with the ones hard backyard cleaning jobs with my pressure washer!! https://escatter11.fullerton.edu/nfs/show_user.php?userid=8991126
Thanks for the useful suggestions. Discover more at hvac contractors near me .
ไฟหน้าแบบไหนที่เหมาะกับสภาพถนนในเมืองไทยที่สุดครับ?? เปลี่ยน ไฟ หน้า รถ ราคา
Thanks for the insightful write-up. More like this at hvac companies .
“Great job explaining slurry seal benefits—it’s something I hadn’t considered before! Looking forward to learning more through resources like those from grading and excavation .”
Right away I am ready to do my breakfast, when having my breakfast coming over again to read more news.
Pretty nice post. I just stumbled upon your
weblog and wished to say that I’ve truly enjoyed surfing around your
blog posts. In any case I will be subscribing to your feed and I hope you
write again soon!
The process of getting released on bond can be overwhelming, but your article simplifies it so well! Thanks for sharing these insights; I’ll keep my eye on Alamance bail bonds. Alamance bail bonds
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
This was highly educational. For more, visit plumbing companies .
Thanks for the clear breakdown. More info at household cleaning services near me .
I started giving Pawbiotix to my dog last month and noticed a big improvement
in his digestion and energy. Definitely doesn’t feel like a scam
— it actually works!
Thanks for the thorough article. Find more at Affordable Neurofeedback Denver .
Anyone know if there are any dentists offering free consultations in Pico Rivera? Direct Dental office
I enjoyed this post. For additional info, visit Afordable Pest Solutions .
“How do you find inspiration? Your creativity shines through every image!” google.com
Thanks for the helpful article. More like this at Aesthetic Plastik Surgery and Lazer Center .
This was very enlightening. For more, visit movers .
If you haven’t explored what’s available yet, you’re missing out on some great finds!!! #apartmentsforrent# anyKeyWord## apartments for rent
It’s encouraging to see platforms like Legal Gun Dealer that address both sides of the gun debate thoughtfully.
Appreciate the detailed information. For more, visit san jose office movers .
If you’re looking for relief from back pain or just want to improve your overall well-being, I highly recommend visiting a chiropractor in Seattle. They offer personalized treatments that can make a significant difference Chiropractor Seattle
The personalized plans at weight loss clinics really helped me achieve my goals. If you’re looking for guidance, I highly recommend exploring Medical Spa Lakewood !
This was a wonderful post. Check out wordpress designer for more.
This is very insightful. Check out san jose website designer for more.
Great advice on backlinking strategies! I’ll definitely consider using services like Buy backlinks for real estate websites moving forward.
Thanks for the great explanation. Find more at 24 hour plumber .
What’s the best way to prepare kids for their first visit to the dentist, especially if it’s somewhere like Pico Rivera? Pico Rivera dentist
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Thanks for the detailed post. Find more at scotts valley movers .
Great insights! Find more at Excavating contractor .
Thank you to the crew at https://unsplash.com/@dorsonfewv for taking care of my car’s auto glass issues so efficiently!
I recently took my family to Family Chiropractic Puyallup, and it has made a significant difference in our overall health. The staff is incredibly knowledgeable and caring, making us feel comfortable throughout the process Chiropractor Puyallup
I enjoyed this read. For more, visit https://www.blaze-bookmarks.win/understanding-bathroom-pipe-equipments .
I just could not depart your website before suggesting that I really loved
the usual info a person supply for your visitors? Is gonna be
again often to inspect new posts
Appreciate the thorough analysis. For more, visit checkatrade plumbers .
Thanks for the insightful write-up. More like this at water heater repair near me .
Thanks for the great tips. Discover more at ac service .
Great job! Find more at LuxNeuro .
Appreciate the comprehensive insights. For more, visit Aesthetic Plastik Surgery and Lazer Center .
This was a great article. Check out commercial pest management Chester for more.
Very helpful read. For similar content, visit fremont movers .
This was a wonderful post. Check out home hvac replacement for more.
Great job! Discover more at spa near me .
The resources available for understanding firearm accessories are excellent, especially those listed on Arms & Ammunition Dealers .
ใครเคยเจอปัญหากับไฟหน้ารถ LED บ้าง? แชร์ประสบการณ์หน่อยครับ เปลี่ยน ไฟหน้ารถยนต์ ราคา
Thanks for the clear advice. More at weed dispensary washington dc .
รู้สึกว่าร้านเหล้าสาย1 มีโปรโมชั่นดีๆ เยอะเลยครับ ร้านเหล้าจัดวันเกิด สาย1
I love this topic! Water is one of these necessary aid, and realizing how many gallons consistent with minute I really need will assist me use it wisely. Keep up the enormous work! https://www.alphabookmarks.win/to-with-ease-clean-a-deck-a-force-washer-with-a-psi-differ-of-2500-to-3000-is-ideal
What are the wonderful instruction suggestions for widespread breeds like Mastiffs or Great Danes? Help mandatory! http://www.video-bookmark.com/user/kittanmyhh
Attractive section of content. I just stumbled upon your website and in accession capital to assert that I get actually enjoyed account your blog posts.
Any way I’ll be subscribing to your augment and even I achievement you access consistently quickly.
I enjoyed this read. For more, visit Walter’s BBQ Southern Kitchen .
Helpful suggestions! For more, visit drain plumbers near me .
The importance of quality backlinks can’t be stressed enough; check out Manual backlink service for reliable services!
hey there and thank you for your information – I’ve definitely
picked up something new from right here. I did however expertise a
few technical points using this website, since I experienced to reload the website many times previous to I
could get it to load properly. I had been wondering
if your web host is OK? Not that I’m complaining, but
slow loading instances times will often affect your placement in google and can damage your high
quality score if advertising and marketing with Adwords.
Well I am adding this RSS to my email and can look out for much more of your respective exciting content.
Ensure that you update this again very soon. http://Dragon-Slave.org/comics/TamikavrConybearepm
Well explained. Discover more at housekeeping services near me .
hey there and thank you for your information – I’ve definitely picked
up something new from right here. I did however expertise a few technical points using this website, since I experienced
to reload the website many times previous to I could
get it to load properly. I had been wondering if your web
host is OK? Not that I’m complaining, but slow loading instances times will often affect your placement
in google and can damage your high quality score if advertising and marketing with Adwords.
Well I am adding this RSS to my email and can look out for
much more of your respective exciting content.
Ensure that you update this again very soon. http://Dragon-Slave.org/comics/TamikavrConybearepm
Nice post. I was checking constantly this blog and I am impressed!
Very helpful info particularly the last part 🙂 I care for such info a lot.
I was seeking this certain info for a long time. Thank you and best of luck.
I love how Austin homes reflect personal style through remodeling! Share your ideas with us at Kitchen Remodeling Austin .
Well explained. Discover more at Walters BBQ Southern Kitchen .
Great article|Solid writeup|Really appreciated this breakdown. Your explanation of general contractor roles gave me some clarity. In Humble, TX, where I’ve seen all types of construction work evolve, this perspective fits perfectly Office Building Construction
I found this very interesting. For more, visit plumbing services .
This was a great article. Check out affordable home plumbing for more.
Have any entertaining adventures taken region even though travelling with pets ? From road trips to vacation trips, permit’s switch reviews the following ### anykeyword ### https://web-wiki.win/index.php/Creating_a_Cozy_Sleeping_Space_for_Your_Furry_Friend_46784
When it comes to real estate transactions, having a knowledgeable ##real estate lawyer## is essential for smooth dealings. #RealEstate real estate lawyer london ontario
Loved learning approximately the various factors influencing digital camera effectiveness—very instructional publish!! https://page-wiki.win/index.php/From_Entryways_to_Backyards:_Key_Areas_for_Security_Camera_Setup
I enjoyed this read. For more, visit Leaking radiator valves .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Don’t forget about curb appeal when remodeling! Tips available at Remodeler Near Me .
I really enjoyed reading your insights on the importance of niche expertise in today’s market. It’s fascinating how a Specialist Sphere can significantly impact overall industry success contact Specialist Sphere
I get pleasure from looking new toys that keep my dog entertained; what’s their prominent toy precise now? Swap toy instructional materials on https://sierra-wiki.win/index.php/Pet-Friendly_Landscaping_Ideas_for_Happy_Pups !
Curious about trending paint colors for 2023? Explore them with us here: Home Remodeling
I was able to find good info from your articles.
Thanks for the helpful advice. Discover more at phim sex hot nhất .
Valuable information! Discover more at địt nhau hot nhất .
I’m amazed by the creativity in Austin’s home renovations! See our favorite projects at Kitchen Remodeling .
I enjoyed this read. For more, visit trailer địt nhau .
Loved how you covered both basics and pro tips, which makes it super valuable for folks around Media, PA who are planning upgrades. Thanks for explaining expansion joints so clearly Concrete contractors
Great job highlighting the benefits of quality insulation solutions like high return options; it’s something every homeowner should consider seriously in Rolling Hills Estates, CA! rockwool insulation
Home automation is becoming a trend in remodels—check out how to include it at Home Remodeling in Austin Texas .
Shoutout to everyone working hard at #anything#; your dedication is evident! Garland Mover’s
Has anyone tried the cheap movers in Gotha? I’d love to hear your experiences! I discovered some options through Long distance movers Gotha .
What features do you think every modern bathroom should have? Let’s discuss over here: Bathroom Remodeling
Paragraph writing is also a excitement, if
you know then you can write otherwise it is complicated to write.
Is it worth investing in a vinyl fence? I’m looking at options from some local Surrey fencing companies. Fortress Fencing Inc
Thanks for the insightful write-up. More like this at kitchen plumbing specialists .
Great insights! Discover more at LuxNuro .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
I highly recommend Ponte Vedra Beach moving companies if you need budget-friendly movers in Ponte Vedra Beach.
The drivers from Albuquerque vehicle shippers are always friendly and professional!
Thanks for the useful post. More like this at hvac maintenance .
This is highly informative. Check out Affordible Pest Solutions for more.
I can’t recommend Irving full service movers enough if you’re looking for a dependable moving service in Irving.
The emphasis on responsible marketing practices in the industry highlighted by Authorized and Licensed firearms and Air Guns Dealers is important for future growth.
Thanks for the helpful article. More like this at local celebration venue rental .
Appreciate the great suggestions. For more, visit medical massage .
Exploring new neighborhoods? This site has great listings for apartments for rent! Rise Bridgeview apartments
Remodeling isn’t just for older homes; new builds can benefit too! Learn more about this approach on our site: ## Remodeling Austin
This was quite informative. More at https://www.alphabookmarks.win/the-benefits-of-regular-pipes-system-and-heating-system-purges .
This was a wonderful guide. Check out pigeon removal near me for more.
Well done! Find more at hvac companies near me .
Thanks for the valuable insights. More at Bathroom Remodelers .
What i don’t realize is if truth be told how you’re now not actually
a lot more smartly-liked than you may be now. You are very intelligent.
You recognize thus significantly on the subject of this subject, made
me individually believe it from so many numerous angles.
Its like men and women don’t seem to be involved until it is
something to accomplish with Lady gaga! Your own stuffs
great. All the time care for it up!
ggbet
Thanks for the useful post. More like this at local indoor air quality testing .
Appreciate the detailed post. Find more at Walters BBQ Southern Kitchen .
Thanks for the useful post. More like this at trusted same day plumber .
I liked this article. For additional info, visit https://www.bookmarkidea.win/tips-for-lowering-your-water-and-home-heating-costs .
Lighting fixtures can make or break a room—choose wisely! Find tips on selection here: Remodeler Near Me .
This was a great article. Check out hvac companies for more.
Useful advice! For more, visit LuxeNeuro .
Incredibly insightful post; honestly replacing how I’ll frame of mind outside chores shifting ahead!!! # # anyK eyword ## https://online-wiki.win/index.php/What_You_Should_Know_About_Renting_vs_Buying_a_Pressure_Washer
Do you need help deciding between tile or hardwood flooring? Get advice from our experts: Home Remodeling
This was highly useful. For more, visit Leaking radiator valves .
Appreciate the great suggestions. For more, visit professional rodent control Chester .
I appreciate homes that combine modern aesthetics with local charm—get inspired with us at Kitchen Remodeling !
Are you considering open-concept living? Learn about its pros and cons here: Home Remodeling in Austin Texas
The kitchen is the heart of the home! Find out how to remodel yours at Bathroom Remodeling Austin .
I liked this article. For additional info, visit home cleaning services near me .
A pressure washing machine with round 2000-2500 PSI is ideal for so much decks. Just needless to say to keep the nozzle at a protected distance! For more tips, see https://www.bookmarkingqueen.win/the-water-consumption-of-a-pressure-washing-machine-is-basically-measured-in-gallons-in-step-with-minute-gpm .
I appreciate homes that combine modern aesthetics with local charm—get inspired with us at Remodeling Austin !
Don’t forget about curb appeal when remodeling! Tips available at Bathroom Remodeling .
It’s interesting to see how technology is changing the role of real estate agents today. Explore more insights at realtors chattanooga tn .
This was very beneficial. For more, visit Walters BBQ Southern Kitchenac .
Great article! Buying backlinks can really boost your site’s visibility. I recommend checking out Buy guest post backlinks for some excellent options.
I found this very helpful. For additional info, visit appliance repair quotes .
Really enjoyed the post! Understanding how lawyers deal with insurance adjusters helped me think differently, especially since New Castle County, DE has its own legal nuances personal injury law firm
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Thanks for the great tips. Discover more at plumbing and heating near me .
It’s the best time to make a few plan for the future and it’s time to be happy.
I’ve read this post and if I may just I want to suggest you
some fascinating issuues or tips. Peerhaps you can write next
articles relatinhg to his article. I want to learn more things approximately it!
Takee a look at my web page Esenyurt ingilizce kursu
This was very enlightening. For more, visit Central heating installations .
This article made me rethink our upcoming move—definitely checking out Local movers Weirsdale for better options!
”No matter where life leads next—always prioritize safety first when considering future travels ahead together alongside trusted partners encountered herein!” Rancho Cordova auto transport companies
Just had my third treatment at Sculpted MD Wheat Ridge, absolutely loving the results from their med spa services!
The staff at Sculpted MD Wheat Ridge makes every visit special, best med spa near me without question Is Sculpted MD taking new clients for laser treatments?
Pressure washers are useful for getting rid of stubborn grime and dust. Can’t wait to are trying some of these innovations! https://www.instapaper.com/read/1854776898
Thanks for the clear advice. More at affordable blocked drain solutions .
Thanks for the thorough analysis. More info at local movers and packers san jose .
This was a fantastic read. Check out ac service for more.
I needed to thank you for this fantastic read!! I certainly loved every
little bit of it. I have got you saved as a favorite to check out new stuff you post…
Great insights! Find more at movers and packers san jose .
If you’re searching for the best dentist near me in Chicago, I highly recommend checking out bite club chicago. They have an amazing team that prioritizes patient comfort and care, and I’ve always had a great experience there! dentist near me
Love the direction here.
Found some fantastic deals on rentals that I wouldn’t have seen otherwise—thank you!!! #apartmentsforrent# anyKeyWord# apartments for rent Greensboro
I enjoyed this read. For more, visit website designer sunnyvale .
Howdy would you mind stating which blog platform you’re using?
I’m planning to start my own blog in the near future but I’m having a
difficult time making a decision between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different
then most blogs and I’m looking for something completely unique.
P.S Apologies for getting off-topic but I had to ask!
This was very insightful. Check out website design services for more.
This was highly informative. Check out air conditioner repair for more.
เครื่องดื่มสร้างสรรค์มากมายที่ร้านเหล้าสาย1 ครับ ร้านนั่งชิล ใกล้ฉัน
ทดสอบความสว่างของไฟหน้ารถ LED ตัวใหม่ พบว่าสุดยอดจริงๆ! ไฟ โปรเจคเตอร์
Appreciate the thorough insights. For more, visit reliable commercial plumbing .
This was highly educational. More at locations for neurofeedback services in Denver .
پروتئین وی ایزوله ایزوفیت ناترکس، حاوی ۲۵ گرم پروتئین وی ۱۰۰٪ ایزوله در هر سروینگ است که با روش میکروفیلتراسیون پیشرفته تولید شده و جذب سریع دارد.
Great job! Find more at Aesthetic Plastic Sugery & Lasor Center .
I was amazed by how much my Anchorage lawyer knew about handling car accidents! Their expertise was invaluable—find them at Car accident lawyer .
This was very enlightening. For more, visit Afordable Pest Solutions .
Valuable information! Discover more at household cleaner near me .
Who knew fixing windows could be this easy? Thanks once again – will recommend widely @ anyone. https://giphy.com/channel/lipinnjusm
Your recent post about the impact of legislation on gun dealers at Popular Gun Dealers was enlightening. Thanks for sharing!
Navigating insurance claims alone can be overwhelming; consider hiring experts from Car Accident Lawyer # for guidance.
I’m searching for a cosmetic dentist in Pico Rivera for some whitening treatments. Any suggestions? Direct Dental in Pico Rivera
The experience with my car accident case improved dramatically once I hired a lawyer from Injury Lawyer .
Appreciate the comprehensive advice. For more, visit Walter’s BBQ Southern Kitchen .
Appreciate the detailed information. For more, visit checkatrade approved plumbers .
Can’t recommend enough these %%legal services near me%%; they’ve made such an impact on my case’s outcome already! lawyers london
So many beautiful spaces available right now; it’s hard to choose just one!! #apartmentsforrent apartments for rent
“Stunning images from recent weddings around Birmingham! They really showcase the city’s charm.” Ikonic Media wedding photographer birmingham
This was very insightful. Check out best local brunch in Pittsburgh for more.
I appreciated this article. For more, visit affordable shower drain repairs .
I enjoyed this post. For additional info, visit reliable emergency plumbing services .
This was highly educational. For more, visit LuxeNeuro .
This was highly useful. For more, visit cheap plumbing and heating .
Thanks for the valuable insights. More at Aesthetic Plastic Sugery & Lasor Center .
Thanks for the thorough analysis. Find more at adu los altos .
I appreciate the variety of styles offered by fencing companies in Surrey—so many choices! Best Fence contractor in Surrey CA
Thanks for the practical tips. More at Affordable Pest Solutions .
This handbook on drone flight patterns changed into eye-beginning! It will improve my expertise really! Want to be informed greater? Visit https://padlet.com/devpage7egmvu/bookmarks-3j9b7zyj3jdbr0g2/wish/lkROZP1brgXkWjMg .
Valuable information! Find more at movers .
This was a wonderful guide. Check out reliable my plumber for more.
Your recent post about the impact of legislation on gun dealers at Arms & Ammunition Dealers was enlightening. Thanks for sharing!
I enjoyed this read. For more, visit Event Space .
Great job! Find more at 24 hour local plumbers .
For anyone looking for quality workmanship, the plumbers at licensed plumbers are among the top choices in Coquitlam!
Great article|Solid writeup|Really appreciated this breakdown. Your explanation of pre-construction planning gave me some clarity. In Humble, TX, where I’ve seen all types of construction work evolve, this perspective fits perfectly Construction company
Local experts make all the difference when it comes to effective plumbing solutions! reliable plumbing contractors
Are there any actual health problems that assured breeds are susceptible to that we must be acutely aware of? https://padlet.com/devpage7kztvw/bookmarks-zpuh831hejshtlxh/wish/LNV1Q7d52jqDZmq3
Really enjoyed this read, especially since many homeowners in Delaware County, PA overlook small cracks until they get worse. I liked the reminder to always check for underlying damage Foundation installation
Appreciate the thorough write-up. Find more at Pittsburgh brunch on weekends .
ไฟหน้ารถ LED BT PREMIUM ทำให้การขับขี่กลางคืนปลอดภัยขึ้นมากเลยครับ ร้านแต่งไฟรถยนต์ ใกล้ฉัน
Awesome article! Discover more at hvac repair near me .
I found this very interesting. For more, visit Leaking washing machines .
This was quite informative. For more, visit Thermostats Gas valves .
Great insights! Find more at air conditioning repair .
Great insights! Find more at cheap car hire .
I’ve seen too many people settle for less after an accident. Always consult a Injury Lawyer before making any decisions!
I recently used a ##Vancouver plumbing service## and was impressed with their professionalism. It’s great to have dependable local plumbers. best tank replacement services
This was very beneficial. For more, visit hvac contractors near me .
Thanks for the thorough article. Find more at Appliance repairs .
I’ve been struggling with sensitive skin for years; your tips give me hope! I’ll check out gentle options from facials near me .
I’m curious about the costs of long distance movers in Fernandina Beach. Found some useful information at Metro Mover’s Fernandina Beach to guide my budget!
El casino platin no hace mucho fue creado en el territorio de España, y Bwin App rápido gira velocidad.
Shoutout to $$for making my recent relocation so affordable without compromising quality! Smooth Moving’s
Thanks for the clear breakdown. More info at maid service near me .
A shoutout to all the hardworking long-distance movers based in Satellite Beach – you guys are lifesavers! Office moving companies Satellite Beach
Great tips on how to secure a rental—this site is a lifesaver! apartments for rent
Your take on accent walls has inspired me to spruce up my living room! Can’t wait to try it out! Virtual Interior Design Services
Great job! Find more at need a plumber .
I enjoyed this read. For more, visit Aesthetic Plastic Sugery & Lasor Center .
หากใครกำลังมองหาร้านเหล้าในกรุงเทพฯ ขอแนะนำให้ไปลองที่OMG OneMoreGlass กันนะครับ ! # #anyKeyword## ผับสาย1 รับจัดวันเกิด
My recent move to Titusville was a success thanks to the professionals at Titusville commercial movers ! Highly recommended!
Can you share more about the tools needed for floor restoration? I’m ready to dive in! Commercial Floor Restoration
Well done! Find more at Afordable Pest Solutions .
I appreciate how informative your posts are about dementia care in the UK! I found even more resources at dementia care .
I found your article on self-defense laws at Authorized and Licensed firearms and Air Guns Dealers to be very informative and timely!
Great read! The financial benefits of high return insulation are hard to ignore—I’m convinced it’s worth a shot for my home renovation project! attic insulation near me
Having reliable movers can change everything during an office relocation; thanks for emphasizing that point so well! Optimo Moving’s Yulee
Wonderful beat ! I would like to apprentice while you amend your
site, how could i subscribe for a blog website?
The account aided me a acceptable deal. I had been a little bit acquainted of this your
broadcast offered bright clear concept
Involving an experienced ###real estate lawyer### protects buyers and sellers alike during negotiations and contracts signing processes! #NegotiationSuccess bankruptcy lawyer
This was a fantastic read. Check out weed dispensary washington dc for more.
Thanks for the insightful write-up. More like this at movers chattanooga .
Shoutout to the team at A1 Auto Transport Santa Rosa for their professionalism during my recent car shipment from Santa Rosa!
Everyone should consider #Rockledgemovingcompany## if they’re looking for reliable movers! Cheap movers Rockledge
Thanks for the useful post. More like this at plumbing leak detection .
Thanks for the great explanation. Find more at home hvac replacement .
..empowering— local plumbing service
Grateful for #AnyKeyWord#’s expertise in handling tricky auto glass replacements smoothly and efficiently. https://www.hometalk.com/member/179099092/albert1829876
I constantly spent my half an hour to read this web
site’s articles or reviews everyday along with a cup
of coffee.
tvbet
Thanks in support of sharing such a good opinion, post is nice, thats why i have read it fully
This was very well put together. Discover more at Landlord certificates .
Demo slot Pragmatic Play dan demo slot PG Soft tempat latihan gratis buat ngulik semua fitur permainan slot online.
Gratis, tanpa perlu mikirin dompet. Pragmatic Play punya game
hits kayak Gates of Olympus atau Sweet Bonanza yang grafisnya juara, PG Soft jagonya bikin slot mobile
yang animasinya halus banget kayak Mahjong Ways 2. Main demo itu bikin makin jago
dan pede sebelum beneran gas pakai uang asli. Gas cobain sekarang!
This was a great article. Check out mommy makeover procedure for more.
I found this very interesting. Check out Boiler service & maintenance for more.
This was quite useful. For more, visit ac service .
Thanks for posting this. I found your take on contractor-client communication especially eye-opening. Being in Humble, TX, it’s great to see local-relevant construction topics like this Veterinary Clinic Construction
Thanks for the valuable insights. More at https://evaelfie.cam/user/seannarpwp .
Very informative article. For similar content, visit Chester Rodent Control .
Thanks for the useful suggestions. Discover more at heating plumbing near me .
I simply read about the web link between oral health and cardiovascular disease. It’s critical to care for our teeth! Discover a lot more at Direct Dental office .
Well done! Find more at san jose professional movers .
If you’re unsure about DIY fixes, consult with an experienced ###Vancouver plumber### before attempting anything complicated. reliable water heater services by contractors
This was nicely structured. Discover more at home cleaning services near me .
Definitely going to share this with my buddies; all of us want smooth sidewalks in our group! https://rapid-wiki.win/index.php/Creative_Ways_to_Freshen_Up_Your_Sidewalk_Without_Power_Washing_41070
This is highly informative. Check out website design services for more.
Wanting justice after being wronged is completely valid; working alongside proficient attorneys allows victims’ voices finally heard!! Car Accident Attorney
I had such peace of mind during my recent relocation because of tips shared on ##yourURL#! Jacksonville full service movers
After my accident in Anchorage, I was lost on what to do next. Thankfully, I found an amazing car accident lawyer who guided me through the process. Look into Car accident lawyer for helpful resources.
Your tips on winterizing roofs are invaluable! It’s crucial to prepare before snow hits. For more seasonal advice, check out roofing company millersville .
I enjoyed this article. Check out website designer san jose for more.
If you ever face urgent repair needs, don’t hesitate to call your local expert plumber in Kelowna for assistance.
This was very insightful. Check out swimming pool removal for more.
After my accident, hiring a Auto Accident was one of the best decisions I made. They really fought for my rights!
whoah this weblog is wonderful i love studying your articles.
Keep up the good work! You know, many individuals are
searching around for this info, you can help them greatly.
Is there anything else targeted one may still look out for whilst deciding to buy 2d-hand electricity washers?? Asking for assistance!!! # # anyK eyword ## https://tango-wiki.win/index.php/Pressure_Washing_Tips_for_Concrete_Surfaces:_Everything_You_Need_to_Know
Great tips! For more, visit affordable syphon installation .
“I’ve seen this all over lately and was wondering if it was legit or just hype. Thanks for the breakdown—might give it a shot before it disappears again.”
This is something more people should know. I found it interesting how you touched on how trauma plays into compensation, and it’s good to raise awareness. Being from Bear, DE, I’ve seen how small details can make or break a case, so this really hit home motorcycle accident lawyer
Many homeowners wonder if anyone can service a heat pump. While some minor issues might be fixable on your own, it’s always best to consult with a certified technician for more complex problems Visit this website
This was highly educational. More at https://vdomkino.ru/user/lefwennrjl .
“Incredible imagery that captures both intimacy and magnificence at weddings.” https://www.google.com/maps?cid=11358797318047951201
Thanks for the valuable insights. More at long distance movers .
Hey are using WordPress for your blog platform?
I’m new to the blog world but I’m trying to get started and set up my own. Do you require any coding
knowledge to make your own blog? Any help would be greatly appreciated!
Investment opportunities arise from strategic collaborations built upon mutual respect fostered between clients relying upon expert guidance offered along journeys filled with challenges ahead—I plan venturing back regularly seeking updates featured realtors chattanooga tn
Hey there I am so happy I found your website, I really found you by mistake, while I was searching on Google for something else, Regardless I am here now and would just like
to say many thanks for a incredible post and a all round thrilling blog (I also love the theme/design),
I don’t have time to go through it all at the moment but
I have bookmarked it and also included your RSS feeds, so when I have time
I will be back to read a great deal more,
Please do keep up the excellent work.
Nicely detailed. Discover more at emergency dishwasher leaks .
This was very enlightening. For more, visit phim hiếp dâm .
Thanks a lot, Numerous facts.
Your encouragement to embrace imperfections resonates deeply with me—it’s such an important part of self-love and care as well as discovering unique finds via websites like ##anyKeyword#! facials near me
Really enjoyed reading this post; it does a fantastic job breaking down why we should all consider upgrading to high-return options at home!! batt insulation
I appreciate the detailed overview of gun safety practices shared on your site, Authorized and Licensed firearms and Air Guns Dealers . Education is key!
Exploring all avenues available allows individuals maximize potential outcomes–consulting qualified professionals never hurts!! Car Accident Lawyer
I appreciate how user-friendly this site is when searching for apartments for rent. Rise Bridgeview
Whoa quite a lot of excellent info!
Wishing everyone similar success stories via ongoing relationships developed alongside approachable experts offering proficient support throughout their rehabilitation phases following unfortunate incidents involving vehicles:” #anythingKeyWord# Personal injury chiropractors
I have an understanding of the step-by-step guide on drone camera settings. It makes it more easy for novices like me! More facts would be determined at https://kaput-arithmetic-5ec.notion.site/22df509247228046be5eee5ae6d1c323?source=copy_link .
Thanks for any other informative blog. The place else could I am getting that type of information written in such a perfect manner?
I’ve a challenge that I am just now running on, and I have been on the glance out for such info.
Don’t let fear hold you back from seeking legal help after an accident; consult with a friendly Accident Lawyer today.
This was very enlightening. For more, visit car rental .
This was highly helpful. For more, visit my plumber .
Home office designs have become so important recently; what features do you think are essential? Tampa Kitchen Designer
Thank you for addressing standard misconceptions approximately safety digital camera placements; very enlightening!! https://atomic-wiki.win/index.php/Understanding_Field_of_View:_Optimizing_Your_Camera_Setup
Very helpful read. For similar content, visit near me plumber .
Clearly presented. Discover more at quick gas safety checks .
I enjoyed this article. Check out coolsculpting for more.
Appreciate the detailed information. For more, visit moving near me .
I appreciated this post. Check out sunnyvale adu for more.
It’s fascinating how different climates can affect flooring materials, especially during restorations—great insight you provided here! Floor Cleaning Service
Hello there! This blog post couldn’t be written any better!
Reading through this article reminds me of my previous roommate!
He continually kept preaching about this. I will forward this post to
him. Pretty sure he’s going to have a good
read. Many thanks for sharing!
https://doce-88.com
Appreciate the detailed information. For more, visit cannabis dispensary .
It’s so important to keep communication open with loved ones who have dementia, and there are tips on this at domiciliary care .
Pleaѕe let me know if yߋu’re looҝing for a author fоr yߋur blog.
You have sⲟmе reallү gгeat posts and I thnk I w᧐uld be ɑ good asset.
Іf yoᥙ ever ԝant to tаke some оf the load оff, I’d reаlly lіke tօ write somе material foг your blog in exchange fоr a link
Ьack to mine. Please send me an email if іnterested.
Regardѕ!
Feel free tⲟ surf t᧐ my webpage; English Tuition Singapore
This was highly useful. For more, visit local plumbers .
The emphasis on responsible marketing practices in the industry highlighted by Authorized and Licensed firearms and Air Guns Dealers is important for future growth.
This was very enlightening. For more, visit heater installation .
Have you seen how well these structures age? Copper copper cupolas only get better with time! cupola on garage
Really clear and concise info, and the timing couldn’t be better for homeowners in Delaware County, PA. The explanation of patching techniques was spot on Patio construction
Great job! Discover more at https://gofilm.cc/user/clarusdqwd .
Howdy! This article could not be written much better!
Going through this post reminds me of my previous roommate!
He constantly kept preaching about this. I most certainly will
forward this article to him. Pretty sure he will have a great read.
Thank you for sharing!
My casino’s VIP perks are amazing.
my blog – https://gunnerhtrm94837.sharebyblog.com/35593189/get-lucky-with-plinko
Loved the way you explained this. I found your take on project timelines especially relevant. As someone from Humble, TX, it’s great to see local-relevant construction topics like this Commercial Construction
Makes navigating complexities surrounding laws seem manageable knowing assistance readily available whenever needed most urgently lawyers london ontario
인사드립니다! 이건 좀 주제에서 벗어나지만, 물어보고 싶었습니다.
링크를 교환하거나 게스트 글를 작성하는 데 관심 있으신가요?
제 사이트는 당신과 같은 토픽을 다루고 있어서 서로에게 큰 도움이 될 거라고
느낍니다. 관심 있으시면 메일을 보내주세요.
당신에게서 소식을 기다립니다! 멋진 블로그입니다!
Hey! I know this is kinda off topic however I’d figured
I’d ask. Would you be interested in exchanging links or maybe guest writing a blog article
or vice-versa? My website discusses a lot of the same topics
as yours and I think we could greatly benefit
from each other. If you happen to be interested feel free to shoot me an email.
I look forward to hearing from you! Terrific blog
by the way!
Thanks for the informative content. More at professional kitchen plumbing installation .
Appreciate the thorough write-up. Find more at trusted leaking dishwasher repairs .
The bond we percentage with our dogs steadily lasts a lifetime; what testimonies do you cherish such a lot with yours? Reflect with us on https://victor-wiki.win/index.php/Pet-Friendly_Landscaping_Ideas_for_Happy_Pups .
I had no idea that old wiring could be such a fire hazard! Thanks for the heads-up! electrician near me
My current experience with an oral implant was surprisingly positive! If you’re curious concerning this treatment, look into details on Pico Rivera Dentists .
Very well done article—glad to discover just how impactful good choices regarding our home’s temperature control systems can be!! rockwool insulation
Yоu neeԁ to take part in ɑ contest for
one ߋf thе greatest blogs ᧐n the net.
I wіll recommend thiѕ website!
Мy blog post: best math tutor (Gene)
Thanks for the insightful write-up. More like this at Outside taps .
Hello, There’s no doubt that your website could possibly be having
browser compatibility issues. Whenever I look
at your website in Safari, it looks fine however,
when opening in Internet Explorer, it has some overlapping issues.
I simply wanted to give you a quick heads up!
Aside from that, great website!
This is actually super intriguing… I’ve always thought lottery wins were just pure luck, but hearing how this
software uses real math and stats changes my
perspective. It’s not a guarantee, but
if it can boost the odds even a little, that’s worth checking out.
Thanks for the honest breakdown!
Great article! I recently used a plumbing service in Bethlehem and they were fantastic. plumbers
Today, I went to the beach with my children. I found
a sea shell and gave it to my 4 year old daughter and
said “You can hear the ocean if you put this to your ear.” She placed the shell to her
ear and screamed. There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is completely
off topic but I had to tell someone!
https://mrbet-88.com
I found this very interesting. Check out Kitchen plumbing for more.
Did you know that routine visits to a Mesquite chiropractor can help prevent injuries? So smart! Car accident chiropractor
Very nice article, totally what I was looking for.
Whenever someone asks about finding a plumber in Coquitlam, I always direct them to check out best Coquitlam plumbing contractors first!
You said it nicely.!
Really enjoyed your take on fixing minor issues rather than calling someone right away—it empowers us as homeowners!! electrician
I’m glad you mentioned potential noise issues with certain models post-installation; it’s something to consider early on! water heater repair Holly Springs
Thank you for the good writeup. It in reality was once a enjoyment
account it. Look complex to far brought agreeable from you!
By the way, how could we communicate?
This was very beneficial. For more, visit professional plumber rates .
Incredibly thankful receiving knowledge shared focusing specifically around innovative designs integrated seamlessly aiming boosting aesthetics improving functionality maximizing returns seen afterward resulting positively enhancing value added during roofing near me
It’s encouraging to see platforms like Firearms Accessories that address both sides of the gun debate thoughtfully.
Never underestimate how important it is having reliable experts in your corner like #! plumber near me
Seriously impressed by how well things turned out thanks to &nbp; plumbing services
Open dialogue between clients & attorneys fosters stronger bonds ultimately leading successful outcomes achieved collectively together!! Auto Accident Lawyer
ร้านเหล้าสาย1 มีกิจกรรมสนุกๆ ให้ทำเยอะเลยนะครับ ร้านนั่งชิล สาย1
Excited about getting my new fence installed soon! Hoping for great service from a local company. maps.app.goo.gl
It’s great how you explain energy ratings; consumers should definitely pay attention as they impact long-term costs ! Find out additional information regarding ratings through ### any keyword### ! water heater installation
I love my dentist in Pico Rivera! They always make me feel comfortable during my visits. Highly recommend! Pico Rivera Dentists
After using Hialeah international movers, I can say they are the best in the business! Don’t hesitate to check out Hialeah FL Mover’s !
It’s essential to document everything and have an truck accident on your side for legal support.
Thanks for the great explanation. More info at san jose commerical movers .
Appreciate the comprehensive advice. For more, visit movers san jose .
Appreciate the useful tips. For more, visit Sunnyvale website designer .
Gaining newfound appreciation after diving deep into crucial elements listed throughout each section relating specifically towards determining best practices involving reliable solutions offered within realm of o ce an sid ev eh icl et ra ns po rtation West Coast Auto Transport Oceanside
What’s up mates, pleasant article and pleasant arguments commented here, I am genuinely enjoying by these.
Immediate legal advice is critical following a car crash! Anchorage has some top-notch lawyers—check out their websites like Alaska injury lawyer for more info.
Sempre recomendo aos amigos experimentarem os clássicos – eles se apaixonam imediatamente também! #recomendação # provedores
Finally found an apartment with everything I wanted—thanks to this site! Rise Bridgeview
This was a fantastic resource. Check out scotts valley local movers for more.
Excellent explanation overall. Your point about quality control really hit home. In Dallas County, Texas, I’ve seen how those factors directly affect both residential and commercial projects Commercial Construction
Thanks for the thorough article. Find more at local marketing services .
Kudos to the **#plumber** who came out last week; he did an amazing job on my sink. Valparaiso plumbers
Such encouraging advice here—I’m ready to take action with help from ### when needed.” plumber near me
เพลงเพราะมากที่ร้านเหล้าสาย1 ทำให้สนุกสุดๆ เลยครับ ร้านเหล้าสาย1 รับจัดวันเกิด
Hello to every body, it’s my first visit of this weblog; this
webpage carries amazing and in fact fine information in favor of visitors.
I always check reviews before selecting a A1 Auto Transport Cincinnati for shipping my car, especially ones based in Cincinnati.
Thank you for advocating for safe storage practices through your content at Suppressors & Gun Silencers Online !
Just wanted to share how smooth my car shipment went through a top vehicle shipping agent in Santa Rosa: A1 Auto Transport Santa Rosa !
I’m really impressed by how knowledgeable and attentive this lawyers london ontario # has been throughout my case.
Reading these tips makes me want to ensure my water heater is functioning optimally – thanks, and shoutout to water heater installation lees summit
Great resource! Definitely bookmarking this page for future reference regarding # Baltimore auto shipping
Your recommendations on tools needed for basic electrical repairs are extremely helpful—thanks a lot! electrician englewood
Thanks for the great content. More at commercial plumbers near me .
My friends are always asking about my new setup; I feel like I’m spreading the word on how great these units are!! #TanklessAdvocate Taylors water heater repair
Just wanted to proportion my successful journey with window opportunity! The system transformed into smoother than I estimated. For these thinking of that it, don’t neglect about to speak about with Roofing contractor for pro education.
This was a fantastic read. Check out fremont movers for more.
Every time I need a new design or writing task completed, I turn to Fiverr! It’s truly the fiverr I’ve ever used.
If I were to build a domicile in Austin, I’d completely choose a custom builder to convey my imaginative and prescient to existence! top accounting firms near me
I appreciated this post. Check out https://audioknigi-torrent.top/user/annilareqb for more.
Valuable information! Find more at washing machine appliance service .
Loved learning more about energy efficiency through improved installations such as these; excited about potential changes ahead!! Garage door insulation
I’m so glad I chose Salem electrical services for my project; they exceeded my expectations! Visit them at electrical repair .
Thanks for the insightful write-up. More like this at Blocked drains .
I was suggested this web site by my cousin. I am
not sure whether this post is written by him as nobody else know
such detailed about my difficulty. You are amazing! Thanks!
: Together forging bonds strengthened ideals shared promoting positive change influencing lives positively enriching existence experienced throughout journey traveled leading fruitful outcomes attained deserving recognition honorably bestowed upon all plumbing services
Don’t hesitate reaching out since everyone deserves access towards experienced guidance provided effortlessly through companies like plumber near me
Cheers. An abundance of knowledge.
If you’re looking at long-term rentals, don’t miss these fabulous options available here!! #apartmentsforrent Rise Bridgeview
It was my first time trying a women-only massage, and I was deeply moved by the thoughtfulness
at 강남토닥이.
The process of buying or selling a home can be overwhelming, but a skilled real estate agent can make it easier! Visit realtors for additional resources.
This website truly has all of the information and facts I wanted
about this subject and didn’t know who to ask.
This was very beneficial. For more, visit https://belarena.by/user/angelmuuvh .
Great insights! Discover more at sex tre em .
What a stuff of un-ambiguity and preserveness of
precious know-how concerning unexpected feelings.
Great job simplifying complex concepts related to heating systems; very approachable writing style!【# # anykeyword】 water heater installation Holly Springs
Grateful learning ways enhancing energy efficiency through simple changes suggested throughout discussion…we can all implement those easily right away folks!! ## residential hvac company
Always good to be reminded about patch testing new products; it saves so much trouble later on—great tip here! Find patch-friendly items at chemical peels !
Hopefully many more years ahead working closely together—so excited!!!! plumbers
Thanks for breaking down the costs associated with hiring an electrician. I had no idea there were so many factors! It’s crucial to compare prices from “electrical companies near me” to ensure you’re getting a fair deal. electricians near me
Fantastic content that emphasizes safety and proper procedures; going forward with ## electrician
Article writing is also a fun, if you be acquainted
with afterward you can write if not it is complicated to write. http://alhjaz.org/redirector.php?url=http://dragon-Slave.org/comics/CarlodoAlderbv
Great service from local pros like &nbp; plumbing services
Appreciate the useful tips. For more, visit 24 7 plumber near me .
Article writing is also a fun, if you be
acquainted with afterward you can write if not
it is complicated to write. http://alhjaz.org/redirector.php?url=http://dragon-Slave.org/comics/CarlodoAlderbv
Hello, this weekend is fastidious in support of me, because this occasion i am reading this
enormous educational paragraph here at my house. https://Arriswebz.club/story.php?title=les-productions-diverso-conception-et-production-devenements
ถ้าอยากหาที่พักผ่อน ร้านเหล้าสาย1 นี่แหละใช่เลยครับ ร้านชิลสาวสวย สาย1
Your analysis of online vs. brick-and-mortar sales at Pistol wholesalers & distributors provided great clarity on current trends.
This was a wonderful post. Check out Walters BBQ Southern Kitchen for more.
พูดถึงการใช้งานไฟหน้ารถ LED BT PREMIUM มีใครมีปัญหาบ้างไหมครับ ?? ร้าน ทํา ไฟหน้ารถยนต์ ใกล้ ฉัน
پروتئین وی ایزوله انیمال یونیورسال نوتریشن، مکملی با کیفیت بالا است که در هر سروینگ ۲۵ گرم پروتئین ایزوله و ۵.۶ گرم BCAA دارد.
Appreciate the info shared here! For repairs, I’m sticking with the trusted team at water heater installation in Lee’s Summit.
Your take on using natural ventilation methods alongside conventional systems sparked some ideas—because who wouldn’t want fresh air flowing through their homes without relying solely on machines?! # # anyKeywords # # furnace repair
hello there and thank you for your information – I have definitely picked up anything new from right here.
I did however expertise several technical points using this site, as I experienced to reload the site many times previous
to I could get it to load properly. I had been wondering if your hosting is OK?
Not that I’m complaining, but sluggish loading instances times will often affect your placement in google and could damage your high quality score if advertising and marketing with Adwords.
Anyway I am adding this RSS to my email and could look out for much more of your respective
interesting content. Ensure that you update this again soon.
The use of bold colors can be intimidating; do you have tips on how to approach them confidently? Modern Interior Designer Tampa
Thanks for finally talking about > Certain Scores May Predict Which Trauma
Patients Face High Risk of Multiple Infections – Healthcare Hygiene magazine < Liked it!
If you live in Poway and need an honest assessment of your HVAC needs, reach out to the folks at licensed hvac company poway !
Instead focusing solely financial gains nurturing relationships cultivated over time yields far greater returns investment made cultivating trust loyalty mutual respect fostering connections meaningful impactful lasting impressions etched heart souls roofing services london ontario
The UK has some fantastic initiatives for dementia care. You can learn more about them on palliative care .
It’s amazing how much difference a restored floor can make in a room’s ambiance. Great tips! Flooring Contractor
Thanks for posting this, especially for those of us in Delaware County, PA dealing with cracked or aging concrete. The resurfacing vs. replacement comparison was super helpful Decorative concrete
Thanks for sharing your insights on what makes great wedding photography—I learned so much!” Wedding Photographer Birmingham
Loved your insights on warranty options when selecting a new water heater—definitely helps in decision-making! water heater installation Holly Springs
Thanks for the comprehensive read. Find more at Plumbing and heating .
I just used plumbers for some plumbing work at my rental property and was very pleased with their service.
Well explained. Discover more at Leaking boilers .
The guys at the fencing company really know their stuff—they helped me choose the perfect design for my yard! maps.app.goo.gl
Very helpful read. For similar content, visit Blocked sinks Macerators .
This was highly useful. For more, visit stylish corporate event venues .
This was a great help. Check out plumbing companies for more.
Replacing your windows can upload cost to your home and escalate strength efficiency! I realized most from roofing contractor approximately the exact-pleasant alternatives potential.
Super content regarding all things related to heating & cooling systems; definitely think about reaching out to ### ## trusted hvac contractors
Hello to every one, for the reason that I am genuinely
eager of reading this webpage’s post to be updated daily.
It carries fastidious data. http://dragon-Slave.org/comics/RicoooFerrarohs
Highly descriptive post, I liked that a lot. Will there be a part 2?
Hello to every one, for the reason that I am genuinely eager of reading this webpage’s post to be updated daily.
It carries fastidious data. http://dragon-Slave.org/comics/RicoooFerrarohs
The resources available for firearm training found at Guns: Pistols, Rifles, Shotguns & More are essential for new owners!
I’ve always been skeptical about chiropractic care but am willing to give it a try after hearing so many positive stories from friends about their experiences with Gig Harbor chiropractors! Gig Harbor Chiropractor
The journey itself enriches lives immensely thus motivating others aspire achieve greatness themselves encouraging exploration pathways unlocked freely flowing seamlessly throughout networks crafted imaginatively emphasizing themes expressed electrician in englewood
I learned so much about maintaining my water heater from water heater installation , especially for repairs available in Taylors!
I love how Fiverr connects clients with freelancers from all over the world. It’s really the best platform out there! Visit fiverr for tips.
I always thought installing a water heater was straightforward, but your tips have opened my eyes to potential pitfalls! Visit tankless water heater repair for guidance!
This was very beneficial. For more, visit tap replacement options .
Helpful suggestions! For more, visit phim sex nhật bản .
How do you handle lowball offers when selling? Strategies are discussed at cash for homes michigan .
So glad that there are qualified professionals offering botox services right here in Red Bank # # anyKeyWord # # botox near near me
Nicely done! Find more at car rental toronto .
Unquestionably believe that that you said. Your favorite reason appeared to be on the
net the simplest thing to be aware of. I say to you, I definitely get irked whilst people consider concerns that they just do not recognise about.
You managed to hit the nail upon the top as smartly as outlined out the
entire thing without having side effect , other people could take a signal.
Will likely be back to get more. Thanks
“Can’t wait until moving forward again soon alongside such dedicated individuals who understand essential requirements within homes too!” Honest Heating & Air Conditioning Repair
Wonderful tips! Discover more at https://kintop.ru/user/dorsonxctt .
Thanks for the clear advice. More at affordable plumbers near me .
Great job! Discover more at https://days.ge/user/merianmtfu .
My friend had a tough time after her car accident until she hired an Anchorage lawyer. They were incredibly helpful! Learn more at Anchorage injury attorney .
The connection between lint buildup and fire risk is alarming! Thanks for bringing attention to this topic—check out Dryer Exhaust Duct Cleaning !
การเลือกไฟหน้ารถ LED ต้องดูอะไรบ้าง? หลอดไฟ รถ
Does anyone know if Valparaiso plumbers offers emergency services in Valparaiso?
Honestly, I wasn’t expecting this, but it really caught my attention. The way everything came together so naturally feels both surprising and refreshing.
Sometimes, you stumble across things without really searching, and it
just clicks. It reminds me of how little moments can have an unexpected impact
This was a great article. Check out mommy makeover transformation for more.
Loved reading this article filled with helpful tips and tricks about HVAC systems! Make sure to check out hvac contractor for services around San Diego!
Thanks for the thorough article. Find more at LuxNuro .
บริการดีเยี่ยมและเครื่องดื่มคุณภาพ ที่ร้าน OMG OneMoreGlass ไม่ทำให้ผิดหวังเลยครับ! ผับแอนด์เรสเตอรองท์ สาย1
I appreciate how you addressed both DIY and professional options for carpet care—very balanced approach! carpet cleaning near me
Thanks for the thorough analysis. More info at Affordible Pest Solutions .
Everyone deserves chance receive equal opportunities afforded along routes traversed henceforth ultimately leading towards success stories told far & wide eventually celebrated wholeheartedly amongst peers alike too real estate lawyer london ontario
Great job! Discover more at local plumbers .
Loved reading through everything related directly to smart choices individuals might make surrounding their upcoming projects involving rooftops – such useful knowledge ! Don’t forget though – reach out via ### anykeyword### . roofer
Thanks for the detailed post. Find more at local movers and packers san jose .
Looking for affordable electrical repair services? Look no further than electrical services englewood in Englewood!
Caught an issue early because of tips from #AnyKeyWord# – happy to share it with others needing #waterheaterrepair# water heater installation Taylors
It’s interesting to see how technology is changing the role of real estate agents today. Explore more insights at real estate agent Ooltewah .
Thanks for the detailed guidance. More at sunnyvale web designer .
This was a great article. Check out professional reliable plumbing for more.
Thanks for the clear breakdown. More info at commerical movers .
Great insights! Discover more at web design agency san jose .
This was highly helpful. For more, visit Project 100 Marketing agency .
”Wondering if there would be noticeable differences between various installations depending upon brand choice… any feedback welcomed here please??? ## hvac services lake oswego
Well done! Find more at pool demolition .
This article is a gem! Bookmarking it for future reference when contacting plumbing services .
Your commitment to educating potential buyers about different firearm types is commendable, as seen on worlds largest online paintball store .
ขอแนะนำเมนูเด็ดของร้านเหล้าสาย1 ให้ทุกคนได้ลองกันนะครับ สถานที่เที่ยวกลางคืนสาย1
Thanks for the clear breakdown. More info at versatile wedding venues .
Hopefully, we’re all inspired now after reading this piece—to become proactive instead of reactive concerning our home environments moving forward.【# # anykeyword】 water heater replacement
Well explained. Discover more at professional neurofeedback treatment services Denver .
Love how you included a section on men’s skincare—it’s so important too! Great finds available at chemical peels !
Thanks for the valuable article. More at best mommy makeover clinic .
Thanks for shedding light on what affects the cost of electrical work! It’s great to have a rough idea before reaching out to professionals. For local help, visit electrical companies near me! electricians near me
Thanks for the great information. More at Walter’s BBQ Southern Kitchen .
“Birmingham couples have such an array of talented photographers at their disposal!” google.com
After my recent accident, I learned that hiring an attorney is essential for navigating personal injury claims effectively! Visit Car accident lawyer to connect with experts.
Really enjoyed reading this post; it does a fantastic job breaking down why we should all consider upgrading to high-return options at home!! Blown-in insulation
Vous avez abordé des points essentiels concernant la agence digitale Lozère que je n’avais jamais considérés.
Remembering key details like those mentioned helps ensure smoother processes down life’s unexpected paths too!!!# anyKeyWord# tankless water heater repair
This was very enlightening. More at commerical movers .
Real estate is such a dynamic field, and having an expert agent makes all the difference during transitions! Explore more strategies at Chattanooga TN property agents !
Appreciate the thorough insights. For more, visit dishwasher leakage solutions .
เมนูอาหารที่ OMG OneMoreGlass รสชาติดีมาก ทำให้การดื่มสนุกขึ้นเยอะ! ผับสาย1
Thanks for the great tips. Discover more at emergency plumbing prices .
The importance of functionality in design cannot be overstated! Great insights here! Florida Interior Designer
Appreciate the thorough analysis. For more, visit expert power flushing .
This was very enlightening. For more, visit https://www.instapaper.com/read/1854740312 .
Anyone else love their new HVAC system from a Poway contractor? I got mine installed by hvac repair poway .
Your advice on staging homes for sale is spot on! best realtor for sellers
The craftsmanship involved in floor restoration truly deserves recognition—what a skilled trade! Floor Cleaning Service
Appreciate the thorough analysis. For more, visit spacious venues for celebrations .
This was a fantastic resource. Check out water damage cleanup South Charlotte for more.
The staff at my dentist’s office in Pico Rivera are so friendly and helpful—definitely recommend them! Direct Dental PIco Rivera
Well done! Discover more at shower refinishing .
Been using Nitric Boost Ultra for a month now and honestly, my
energy levels are way more stable. Not just for workouts—feels like
a full-body upgrade.
I love how you broke down the costs associated with hiring a plumber—very informative! Valparaiso plumbers
The market trends discussed at Pistol wholesalers & distributors are fascinating! It’s interesting to see how consumer preferences evolve.
Well explained. Discover more at Walters BBQ Southern Kitchen .
I appreciate the advice on finding local contractors—supporting small businesses is key! hvac company
Appreciate the detailed information. For more, visit blocked drain plumber .
I appreciated this article. For more, visit Tankless Water Heater Replacement Services .
Thanks for the valuable insights. More at https://www.overthemonster.com/users/FosterPlumbing/ .
Great insights! Discover more at phim sex .
I appreciate that you included links to further resources; it’s always nice to have more information at hand! water heater repair
I found this very interesting. For more, visit https://maps.app.goo.gl/uya2XCd1aMavthoP6 .
Thanks for the detailed guidance. More at best roof installation near me .
This is very insightful. Check out Foster Plumbing & Heating for more.
Les normes écologiques devraient-elles être prises en compte lors du choix d’une nouvelle agence? # # anyKey word ## agence web Mende professionnelle
ความคิดเห็นส่วนตัวว่าการใช้งานจะเป็นอย่างไรเมื่อเปรียบเทียบกับแบบเก่า ### เปลี่ยน ไฟหน้ารถยนต์ ราคา
Anyone else had to deal with water heater repairs? Taylors has some great options! Visit tankless water heater repair for recommendations.
Have you heard about latest trends revolving around modern-day installations?If interested check out resources provided under# AnyKeyWord#. electrician in englewood
Appreciate the thorough insights. For more, visit emergency plumber .
Kudos again reminding everyone why investing wisely into quality alternatives offered locally ensures greater satisfaction experienced long-term whilst avoiding unnecessary headaches caused later down road resulting from poor choices made upfront roofing company
If you’re looking for quality service, look no further than tankless water heater repair for your water heater repairs in Lee’s Summit!
Thanks for the thorough article. Find more at local plumber pricing .
”Would love feedback concerning timing when booking services from those top-tier local providers!” %% anyKeyWord%% Albuquerque auto transport companies
Wondering if virtual reality experiences enhance engagement rates among potential clients exploring listings???? Innovative applications outlined showcasing effectiveness presented conveniently through __#anything_# sell my house fast in michigan
Thanks for the clear breakdown. Find more at Denver based neurofeedback sessions .
This was a great help. Check out Aestheic Plastic Surgery & Laser Centre for more.
Is there a specific age when one should start considering Botox? I’m looking into botox treatment red bank in Red Bank.
Corporate lawyers specialize not only in contract management but also strategic advice impacting overall business success ! #StrategicAdvice lawyers london
Great tips! For more, visit indoor air quality testing expert .
I’m excited about sharing this recommendation because # # anyKeyWord# deserves all the praise they get as local experts! Bethlehem plumbers
Hello! Someone in my Myspace group shared this
site with us so I came to take a look. I’m definitely loving the information. I’m bookmarking and
will be tweeting this to my followers! Fantastic blog and great style and design.
I am in fact happy to glance at this webpage posts which includes
lots of helpful facts, thanks for providing these statistics. https://Delo-Press.ru/bitrix/redirect.php?event1=click_to_call&event2=&event3=&goto=https://Ctpedia.org/index.php/Article_Title
I am in fact happy to glance at this webpage posts which includes lots of helpful facts, thanks
for providing these statistics. https://Delo-Press.ru/bitrix/redirect.php?event1=click_to_call&event2=&event3=&goto=https://Ctpedia.org/index.php/Article_Title
Thanks for the insightful write-up. More like this at plumbers in the area .
each time i used to read smaller posts that as well clear their motive, and that is also happening with this paragraph which I am reading here.
The idea of with the aid of necessary oils in cleaning is advantageous! Not in basic terms does it odor magnificent, however it also includes sturdy for you. I’ll investigate out House Cleaning Company for greater methods to incorporate them!
Are there any eco-friendly fencing options offered by local companies in Surrey? Fencing company Surrey CA
After my car accident, I was recommended to a Gig Harbor Chiropractor, and it made all the difference in my recovery process! Chiropractor Gig Harbor
So glad I found this article before my next home renovation project! plumbing services Valparaiso
You packed this post with great advice, especially since concrete work in Media, PA comes with unique challenges. I found the section on driveway grading particularly useful Patio construction
This blog offers such valuable insights! For HVAC solutions in San Diego, be sure to visit san diego hvac company .
A big shout-out goes towards folks responsible behind scenes ensuring smooth deliveries happen regularly!!! Oakland vehicle shippers
This was a wonderful post. Check out loan agency new orleans for more.
Hello, i think that i saw you visited my blog thus
i came to go back the want?.I’m attempting to find issues to improve my website!I guess its
ok to use a few of your ideas!!
I am genuinely happy to read this blog posts which contains lots of valuable
data, thanks for providing such statistics.
I enjoyed this read. For more, visit https://atavi.com/share/xcs2rhz1dvaym .
Very satisfied with the response time from my local electrician via electrical contractor vancouver .
If I’m looking for a $5,000 bond with a bondsman in Burlington, NC, what should I expect to pay upfront? Any insights would be appreciated! For more details, visit bail bondsman near me. The original source
Thanks for the helpful advice. Discover more at Wedding Venue .
Thanks for breaking down the costs associated with professional carpet cleaning services—very informative! carpet cleaning service near me
Thanks for the thorough article. Find more at Denver therapy options for neurofeedback .
Appreciate the insightful article. Find more at cheap car hire toronto .
My friend just installed a tankless heater and loves it! Can’t wait to hear more about her experience. water heater repair Taylors
Thanks for sharing your expertise on electrical systems! It’s comforting to know there’s help out there when needed. electrician in englewood
I appreciated this post. Check out Pittsburgh brunch dining options for more.
After my recent accident, I learned that hiring an attorney is essential for navigating personal injury claims effectively! Visit Car accident lawyer to connect with experts.
Appreciate the comprehensive advice. For more, visit Chester Bug Control .
I love your suggestions on DIY roofing repairs! They seem manageable even for beginners. Find more DIY tips at roofing company .
Hey there, I think your website might be having browser compatibility issues.
When I look at your blog site in Safari, it looks fine but when opening in Internet Explorer,
it has some overlapping. I just wanted to give you a quick heads up!
Other then that, great blog!
Thanks for the thorough analysis. Find more at sex tre em .
I appreciate the advice on finding local contractors—supporting small businesses is key! hvac contractor lake oswego
Just wanted to drop a line about how amazing ### anykeyword ### has been for my home repairs. plumbing company justin
Enjoyed your insights into residential electrical systems; I’ve decided I’ll reach out to ## Salem electrical services
Thanks for the insightful write-up. More like this at http://www.staniforthfamily.com/forum/member.php?action=profile&uid=370134 .
Thanks for the clear breakdown. More info at professional blocked toilet services .
Appreciate the helpful advice. For more, visit plumbing .
Thanks for the thorough analysis. Find more at expert emergency plumbing .
The step-by-step guide is exactly what I needed for my DIY project! Appreciate the clarity. water heater installation Holly Springs
This article really sheds light on what to expect when hiring an electrician electrical contractor
Thanks for the insightful write-up. More like this at unique event venues near me .
Seller disclosures are crucial in Michigan real estate transactions! Learn more about them at sell your house fast for cash michigan .
It’s incredible how much market analysis goes into being a successful real estate agent! Thanks for shedding light on this aspect—more insights at Chattanooga real estate agents .
Nicely detailed. Discover more at heater repair .
I didn’t realize how vital regular maintenance checks would be until reading through this—such valuable info!!!# anyKeyWord# water heater repair
Thank you for addressing common misconceptions about firearms on Sports Air Guns, Airgun manufacturers, suppliers & exporters ! It’s crucial to clear up misinformation.
L’importance du design dans la agence digitale Lozère ne peut pas être sous-estimée, merci d’en parler !
Very detailed and informative, especially since concrete work in Media, PA comes with unique challenges. I liked the focus on foundational stability Concrete installation
Just watched this review and I’m honestly impressed.
I’ve been dealing with sciatic pain for months, and it’s great to hear that
Arialief targets the root cause instead of just numbing the pain. Definitely considering giving it a try!
Nicely done! Find more at Walters BBQ Southern Kitchen .
Thanks for the helpful advice. Discover more at http://delphi.larsbo.org/user/cassinfids .
If you want an straightforward shifting knowledge, achieve out to empresa de mudanças em jundiaí # for your entire transport wishes in Jundiai!
I currently used mudanças em Jundiaí for my place of job relocation in Jundiai, and their staff turned into exceedingly official and valuable.
I can’t believe how many options there are for bridal shoots in Birmingham—exciting times ahead! Ikonic Media wedding photographer birmingham
For quality service without breaking the bank, consider giving a call over to # # anyKeywod ###—worth it!” hvac company poway
I never believed in chiropractic care until I tried it! A Gig Harbor Chiropractor truly changed my life. Car accident chiropractor
Thanks for the detailed post. Find more at commercial movers san jose .
This was beautifully organized. Discover more at local movers san jose .
If you need a trustworthy vehicle shipping agent in Santa Rosa, definitely reach out to Santa Rosa car transport .
Just moved to Pico Rivera and need a local dentist. Any suggestions? Direct Dental Clinic
Valuable information! Discover more at https://question-ksa.com/user/marachxljt .
This was very insightful. Check out web designer sunnyvale for more.
Appreciate the useful tips. For more, visit commercial movers scotts valley .
Having comprehensive knowledge concerning legal matters influencing housing transactions strengthens confidence levels amongst clients feeling empowered moving forward throughout processes undertaken diligently side-by-side with trusted advisors—they’ll realtors chattanooga tn
Loved reading this article filled with helpful tips and tricks about HVAC systems! Make sure to check out hvac company san diego for services around San Diego!
Thanks for the thorough analysis. More info at https://usellbuybid.com/user/profile/3303475 .
This was a fantastic resource. Check out https://qa.laodongzu.com/?qa=user/cynhadrxkx for more.
Very helpful read. For similar content, visit San Jose website design .
If you’ve been struggling with bad breath like I was, give Prodentim a try.
It’s the only thing that’s worked for me — feels amazing to have lasting freshness!
Thanks for highlighting the importance of regular maintenance for HVAC systems! I’ll be more diligent now. hvac contractor
I found this very interesting. Check out Hercules marketing consultant for more.
Nicely detailed. Discover more at abogado .
Thanks for the valuable article. More at Aesthetic Plastic Sugery & Lasor Center .
เพลงเพราะมากที่ร้านเหล้าสาย1 ทำให้สนุกสุดๆ เลยครับ ร้านนั่งชิล สาย1
Excellent tips on energy efficiency! High return insulation seems like a smart investment for homeowners in Rolling Hills Estates. expanded polystyrene
I’m excited to explore advanced techniques once I’m comfortable with the basics!! mindful pilates studio aventura
Thanks for the thorough article. Find more at LuxeNeuro .
Just finished my fence installation with a local Surrey fencing company—very satisfied! maps.app.goo.gl
If you’re feeling lost after a car crash, remember that there are professionals who can help you reclaim your life and benefits! Explore options at Anchorage injury attorney .
A water heater maintenance schedule is essential! I’ll definitely start keeping track now. water heater repair
Thanks for the detailed guidance. More at Afordable Pest Solutions .
I do not know whether it’s just me or if everyone else experiencing problems with your website.
It appears as if some of the text on your posts are running off the screen. Can somebody else please comment and let me know if this is happening to them too?
This may be a problem with my web browser because I’ve had this happen before.
Kudos
Thanks for sharing your info. I truly appreciate your efforts
and I will be waiting for your further write ups thank you once
again.
Appreciate you posting this! Your point about how quickly evidence can disappear was a good wake-up call. Here in New Castle County, DE, it’s essential to know your rights quickly after any type of crash car accident lawyer
I enjoyed this post. For additional info, visit same day plumber .
This was highly educational. For more, visit blocked drain removal experts .
Don’t let a broken water heater ruin your day! Check out water heater installation Taylors for the best repair services in Taylors.
I am extremely impressed with your writing skills as well as with the
layout on your blog. Is this a paid theme or did you modify it yourself?
Either way keep up the excellent quality writing, it’s rare to
see a nice blog like this one today.
Appreciate the detailed information. For more, visit office movers .
If you’re moving soon, trust me, you need to call Local movers Brandon – they are the best!
I’d love more insights into designing functional entryways that also make strong first impressions!! # # anyKeyWord # Tampa Interior Designer
It’s fantastic to see more people focusing on sustainable roofing options! For eco-friendly solutions, visit Roofing contractor .
Your manual on creating miraculous time-lapse films with drones used to be especially successful! I’ll certainly do this strategy soon! Learn greater at https://t7tel.mssg.me/ .
Just cleaned my patio fixtures with a pressure washer and they appearance state-of-the-art again—so effortless and immediate! Click here for more
Thank you for some other excellent post. Where else may anyone get that type
of info in such an ideal way of writing?
I have a presentation next week, and I’m on the look for such information.
Ultimately encouraging superior relationships constructed amongst humans/pets leads enriching lives past creativeness experienced st https://mighty-wiki.win/index.php/Selecting_the_Best_Toys_for_Different_Dog_Breeds_and_Sizes_81474
My HVAC system was acting up, but thanks to trusted hvac contractors , it’s working perfectly again!
As a caregiver, finding the right support is key. I found some excellent options listed on home health care .
Le design responsive est incontournable, surtout avec l’essor du mobile ! solutions web Lozère
The community aspect surrounding floor restorations is inspiring too; it’s nice seeing people support each other! Floor Polishing Service
I fully grasp how committed the crew at mudança em Jundiaí is to featuring best provider for the period of strikes—equally residential and commercial.
If you’re in desire of efficient relocating prone in Jundiaí, be certain that to review out what’s sold by way of empresa de mudanças em jundiaí !
The discussion around hunting rights and regulations at Sports Air Guns, Airgun manufacturers, suppliers & exporters is informative and well-articulated.
The right contractor can make all the difference in your remodel! We can help you find one at Kitchen Remodeling Austin .
I appreciated this post. Check out affordable mommy makeover for more.
Anyone knows if there are any emergency plumbing services available in Bethlehem? plumbing services
I’m regularly in the hunt for new recipes for selfmade puppy treats! What’s your favourite? Let’s swap rules at https://wiki-room.win/index.php/Traveling_by_way_of_Car_with_a_Pet%3F_Here%E2%80%99s_What_You_Need!_23103 .
Thanks for the thorough article. Find more at Denver Neurofeedback Therapy .
This was quite informative. For more, visit abogado .
Fantastic article! It’s crucial to understand the basics of plumbing before a crisis hits. Plumbing Paramedics
Thank you for sharing this valuable information! If you’re from San Diego and need HVAC solutions, consider checking out hvac repair service san diego .
Nicely detailed. Discover more at Walters BBQ Southern Kitchen .
Valuable information! Discover more at Affordable Pest Solutions .
The question about whether electricians can make $50 an hour is intriguing! I guess it depends on their skills and location. If you’re looking for dependable electricians near me, don’t forget to compare rates and services! electrical contractor
Wonderful items fгom yοu, man. I һave tаke notе your stuff prior tо and you аre just extremely magnificent.
І аctually like wһat үou have acquired гight here, ceгtainly ⅼike what you
ɑrе stating and the bеst way through wһіch you say it.
You make it entertaining and you continue to tаke care of to keep іt sensible.
I cant wait to learn fаr moгe from you. That is ɑctually a tremendous website.
Ꭺlso visit my web blog … Kaizenaire math tuition singapore
This was quite informative. For more, visit air conditioning replacement .
What’s your favorite home remodeling trend in Austin? Share and explore more at Home Remodeling !
Have you seen the latest bathroom designs? Check them out on our site: Bathroom Remodeling Austin !
Appreciate the thorough analysis. For more, visit gas plumber near me .
hi!,I like your writing so much! percentage we keep
up a correspondence extra approximately your post on AOL?
I need a specialist on this space to solve my problem.
Maybe that’s you! Taking a look ahead to peer you.
Great insights! Discover more at quick gas safety checks .
I’m so glad I found this post! The idea of investing in high return insulation is very appealing and practical for my area. Spray foam insulation
Do you prefer modern or traditional styles for home remodeling? Share your thoughts and check ours out: Kitchen Remodeling
Hi there mates, its impressive piece of writing about tutoringand entirely explained, keep it up all the time. http://Kawarfoundation.biz/__media__/js/netsoltrademark.php?d=Baradundental.CO.Kr%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D540201
This was quite useful. For more, visit phim hiếp dâm .
Landscaping can complement your home’s design beautifully; check out ideas on our site: Home Remodeling in Austin Texas
The analysis of social media’s influence on public perception of firearms discussed at Firearms Accessories was insightful!
Exploring different styles of photography has been eye-opening as we plan our big day in beautiful Birmingham! https://www.google.com/maps?cid=11358797318047951201
Great tips on preparing my car for shipping in Jacksonville! Thanks a lot! Jacksonville car moving companies
This was very informative, as concrete surfaces in Delaware County, PA take a beating from seasonal changes. The resurfacing vs. replacement comparison was super helpful Concrete installation
Thanks for the great tips. Discover more at local car accident attorney .
The Michigan real estate market has some unique trends. Stay informed by visiting cash for homes michigan !
”Did anyone else feel overwhelmed when dealing with repairs before finding specialists like #?” plumbing services
With so many options available today, it’s important we find trusted sources, just like we see reflected upon testimonials highlighting effectiveness showcased surrounding those working alongside### Any KeyWord### botox service
The efficiency of my home has improved drastically thanks to the services of # # anyKeyWord # # . Thank you! hvac company
Hey there! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Thank you
I appreciate all the valuable information shared here about maintaining safe connections in older homes!!! # # anykeyword # # Cornerstone Services
I liked this article. For additional info, visit Power flushing .
If you ever need quick fixes around the house, just call electrical contractor vancouver ; they are reliable!
I’ve seen such a lot of adorable blended breeds nowadays! Which ones stand out to you? https://www.instapaper.com/read/1845908741
It’s amazing how many people find relief from chronic pain through chiropractic adjustments! Grateful for the professionals we have here in Gig Harbor! Car accident chiropractor
Thanks for breaking down the costs associated with water heater installation—very eye-opening! water heater installation
This was highly educational. For more, visit Walter’s BBQ Southern Kitchen .
I’m gone to say to my little brother, that he should also go to see this webpage on regular basis to get updated from most up-to-date news update.
Sharing personal stories about caregiving can inspire others; let’s spread awareness through sites like quality elderly home care !
I’ve currently started out decluttering, and it feels so freeing! Your submit stimulated me even more. I’m excited to see what else I can locate on House Cleaning Services .
Such thorough coverage of safety considerations during installation—much appreciated! Visit water heater repair lees summit for safety tips!
This was a wonderful post. Check out affordable toilet repair for more.
Thanks for the insightful write-up. More like this at shower drain cleaning services .
I am regular visitor, how are you everybody? This
paragraph posted at this web site is genuinely pleasant.
Real estate agents really do know the ins and outs of the market. Thanks for highlighting their importance! More information at realtors Ooltewah .
Thanks for the detailed post. Find more at Aesthetic Plastik Surgery and Lazer Center .
Grateful every day that we decided on going through this company; true lifesavers when it comes down fixing heating systems are # # aniykeyowd # #! hvac contractor poway
Looking for sturdy movers in Jundiai? empresa de mudanças em jundiaí is the reply! They deliver height-notch provider at any time when.
Moving doesn’t have to be overwhelming if in case you have the top workforce! Check out mudança em Jundiaí for powerful transferring capabilities.
부산여성전용마사지 덕분에
다시 나다워졌어요.
Wonderful tips! Find more at abogados .
Your insights into DIY skincare are refreshing! I’m interested in finding ingredients online, especially from beauty salon barnsley .
Thanks for the helpful article. More like this at Afordable Pest Solutions .
Sometimes witnessing aggressive sporting activities related to dogs sparks pleasure amongst lovers alike–Which events draw audiences close at the same time showcasing notable proficiency displayed for the period of competitions this day? https://wiki-mixer.win/index.php/How_to_Prepare_Your_Home_for_a_New_Puppy_Arrival
What’s your favorite home remodeling trend in Austin? Share and explore more at Remodeler Near Me !
Very useful post. For similar content, visit reliable trader plumbing services .
I are not able to have faith how a whole lot I’ve learned from simply one article—you’ve got you have got coated all principal bases the following, thanks once more!! ##anythingKeywords## https://tiny-wiki.win/index.php/Where_Should_You_Point_Your_Security_Cameras%3F_Expert_Insights
Does anyone know if trusted hvac contractors offers emergency HVAC services? I might need one soon!
Thanks for the thorough analysis. Find more at hvac installation .
Had a fantastic experience with the friendly staff at plumbers #.
”Just got a quote from an HVAC contractor, and I’m shocked at how affordable it is compared to last time!!! $$ Need more info!! #HVACcontractor $$ Looking forward!!! $$ Great discussion!! $$ # hvac company
Have discovered splendid eco-friendly manufacturers offering sustainable items geared in the direction of pampering doggies not too long ago?! Let’s compare environmentally awake offerings achieveable in the present day in combination! https://post-wiki.win/index.php/Travel_Safety_Tips_for_Dogs_on_Airplanes_and_Trains_86365
Hi there! This article couldn’t be written much better!
Looking at this article reminds me of my previous roommate!
He continually kept talking about this. I am going to forward
this article to him. Pretty sure he’s going
to have a great read. I appreciate you for sharing! http://Team.Clubxtrem.net/profile.php?mode=viewprofile&u=42891
Have you seen the latest bathroom designs? Check them out on our site: Kitchen Remodeling !
Hi there! This article couldn’t be written much better! Looking
at this article reminds me of my previous roommate!
He continually kept talking about this. I am going
to forward this article to him. Pretty sure he’s going to have a great
read. I appreciate you for sharing! http://Team.Clubxtrem.net/profile.php?mode=viewprofile&u=42891
Thanks for the practical tips. More at loan agency new orleans .
Thinking of adding a second story? It’s a great way to gain space—learn more here: Bathroom Remodeling Austin !
I can’t get enough of the industrial style; it’s so unique and edgy! Any tips on pulling it off? Tampa Kitchen Designer
The artistry behind each step taken throughout various processes involved reflects passion felt deeply by those committed within this field. Floor Cleaning Service
The tips for new gun owners on Imported Pistols are incredibly helpful! Great resource for beginners.
Is it worth it to remodel before selling? Get insights on this topic: Kitchen Remodeling Austin .
The kitchen is the heart of the home! Find out how to remodel yours at Remodeling Austin .
I found this very interesting. For more, visit sex tre em .
Do you think it can be valuable to spend money on dear models if simplest used at times—or will mid-range suffice??? # # anyK eyword ## https://escatter11.fullerton.edu/nfs/show_user.php?userid=8990131
อยากรู้ว่า BT PREMIUM เหมาะกับรถรุ่นไหนบ้างครับ ?? ร้านซ่อม ไฟรถยนต์ ใกล้ฉัน
Is anyone else passionate about improving dementia support systems? Let’s discuss insights from home care services !
Your point regarding emotional intelligence in negotiation processes was compelling; it truly affects outcomes significantly—explore further insights into this topic at best realtors in Chattanooga TN !
Thanks! The info on payout times was valuable. I recently joined casino play Online and the cashout reached my bank in less than two hours. Plus the welcome bonus of 150% helps extend the bankroll. Anyone chasing quick withdrawals should have a look. Good luck!
This blog has made me rethink my entire approach to home cleanliness; thank you for all the insights regarding carpet care and upkeep strategies! carpet cleaning service
Thanks for the practical tips. More at Walter’s BBQ Southern Kitchen .
Le choix d’un CMS peut impacter énormément le travail d’une agence web, qu’en pensez-vous ? services d’agence web Lozère
Always remember to hire licensed electricians! I found mine through # anykeyword # and they did an excellent job fixing my issues in Englewood! electrician englewood
This was quite helpful. For more, visit colchones en Albacete .
I appreciate your emphasis on safety during water heater installation. It’s often overlooked! water heater replacement
Thanks for the clear breakdown. Find more at LuxeNeuro .
I always find your posts enlightening and packed with useful information! real estate agent commissions
Wonderful tips! Find more at community pest management Chester .
This was very enlightening. More at plumbing leak detection .
Love how you broke down the strategy into simple steps—makes it much less intimidating for newcomers like me! https://source-wiki.win/index.php/Keeping_It_Simple:_Basic_Tools_for_Effective_Manual_Concrete_Cleaning
Appreciate the detailed post. Find more at Walters Barbecue Southern Kitchen .
This was a fantastic read. Check out Bathroom refurbishments for more.
I’m not sure exactly why but this web site is loading
extremely slow for me. Is anyone else having this problem or is it a issue on my
end? I’ll check back later and see if the problem still exists.
Fantastic points made here! High return insulation seems like a no-brainer for anyone looking to improve energy efficiency in their homes in Rolling Hills Estates, CA! fiberglass insulation
Nothing beats the competencies of empresa de mudanças em jundiaí relating to specialist moving expertise in Jundiai!
I take pleasure in your techniques on add-ons that increase drone photography; they may be able to make a good sized difference in output excellent! For further suggestion, look at various out https://padlet.com/devpage7fnjdd/bookmarks-nso23ux5vmjx8kze/wish/pRxDZ45j5Y28W183 .
Just finished a sizeable domestic cross with ### anyKeyWord###—their potency is unmatched in this enterprise! mudança em Jundiaí
If you might be in Jundiai and want shifting amenities, trust me—go along with mudanças em Jundiaí for a dilemma-loose knowledge!
Thanks for the informative post. More at https://maps.app.goo.gl/yC3uf9xyFnANUy9E8 .
Your focus on youth education about guns and safety is so necessary, especially through platforms like Imported Pistols .
Valuable information! Discover more at https://maps.app.goo.gl/TLhtZWwednG674uVA .
Thanks for the detailed guidance. More at Summers Plumbing Heating & Cooling .
Love seeing a focus not just on aesthetics but also functionality when it comes to discussing roofs!! # # anyKeyWord ## roofing contractor
Anyone else have horror stories about bad plumbers? It’s great we can share experiences and learn which ones are solid choices around here, like those found serving us well right here at home: our beloved town of Bethlehem! plumber near me
Thanks for the useful suggestions. Discover more at water damage cleanup services .
Thanks for the great tips. Discover more at roof repair .
My partner and I stumbled over here from a different web address
and thought I might check things out. I like what I see so
i am just following you. Look forward to exploring your web page repeatedly.
Appreciate the comprehensive advice. For more, visit local door companies near me .
Wonderful tips! Discover more at https://maps.app.goo.gl/Ne8fM3eu1akFw6es7 .
Valuable information! Discover more at Tankless Water Heater Installation Near Me .
For all my electrical needs, I trust electrician near me completely!
Kudos to the team at Progressive Heating & Air for being so reliable and efficient!
This was quite informative. More at https://maps.app.goo.gl/D6JE8YjtmxatsWz46 .
This was a great article. Check out Walter’s BBQ Southern Kitchen for more.
Very helpful read. For similar content, visit https://maps.app.goo.gl/yBjQeeQvqKfZF63g6 .
Couldn’t imagine traversing path alone without outst custom home
Wondering if any fencing companies in Surrey provide free estimates? That would be super helpful! https://maps.app.goo.gl/zFoBM7QV13WaedDn7
Thanks for the great content. More at local same day plumber .
This is something more people should know. I liked how you touched on the emotional impact of injuries, a part that many forget to account for. Being from Bear, DE, I’ve seen how important good legal advice is, so this really hit home pedestrian accident lawyer
Appreciate the thorough analysis. For more, visit https://maps.app.goo.gl/rUt5jEbkW8DhcpeUA .
Well done! Discover more at roof replacement services near me .
Has anyone tried respite care services? There’s useful info about this at skilled home health care that might help!
Thanks for sharing these useful suggestions on deciding upon the correct strain washing machine for more than a few obligations! Very informative! https://www.instapaper.com/read/1854909100
This was nicely structured. Discover more at surrounding area brunch spots Pittsburgh .
Clearly presented. Discover more at Sink leaking .
Thanks for the great explanation. More info at Summers Plumbing Heating & Cooling .
This was highly helpful. For more, visit https://www.nunesmagician.com/users/Homeimprovements56/ .
If you want peace of mind regarding your hot water supply, visit #AnyKeyWord# today! Taylors water heater repair
It’s great to see more discussions on electrical safety! For those in Glendale, check out Electrician Glendale !
Fantastic job sharing these important details about ensuring proper installation ; neighborhoods surrounding glendale could greatly benefit contacting firms listed under # # anyKeyWord # Electrical Contractor Glendale Arizona
It’s great to see more discussions on electrical safety! For those in Glendale, check out Electrician Glendale Arizona !
Such useful information about home wiring! Don’t forget to look at Electrician if you’re in Glendale!
Fantastic information on identifying electrical hazards in the home! Very useful for homeowners. electrician near me
Wonderful tips! Find more at 24 hour plumber .
Magnificent goods from you, man. I’ve keep in mind
your stuff previous to and you’re simply too magnificent.
I really like what you have got right here, certainly like what you’re saying and the way by which you are
saying it. You make it enjoyable and you continue to take care
of to stay it smart. I can’t wait to read far more from you.
This is really a terrific web site.
This was a great article. Check out http://julia4tied.de/member.php?action=profile&uid=180867 for more.
I’m really interested to know what people think about using botox as preventative care vs corrective care # # anyKeyWord # # red bank botox clinic
This blog post is super informative! I’m keeping the info handy for when I need help from Justin plumbers .
If you’re searching for quality HVAC work in Lake Oswego, don’t hesitate to call hvac company near me !
I had my outdoor lighting installed by Salem electrical services, and they did a fantastic job! Find them at electrical repair .
Nicely done! Find more at 24 7 plumber near me .
ความสะอาดของร้านเหล้าสาย1 ทำให้รู้สึกมั่นใจในการใช้บริการมากขึ้นครับ ร้านเหล้าสาย1 เพลงเพราะ
Fantastic post! Discover more at car hire .
This was quite informative. For more, visit Aesthetic Plastic Sugery & Lasor Center .
Great job! Find more at colchones .
Thanks for the thorough article. Find more at best roofing contractors .
It’s interesting to see how electrician rates can vary across different regions. In Charlotte, NC, I’ve noticed that labor costs seem to be competitive electrical contractor
Attractive section of content. I just stumbled upon your website and in accession capital to assert that I get actually
enjoyed account your blog posts. Anyway I will be subscribing to your feeds and even I achievement you access consistently rapidly. http://dragon-slave.org/comics/KathyerStonorkn
Attractive section of content. I just stumbled upon your
website and in accession capital to assert that I get actually enjoyed account your blog posts.
Anyway I will be subscribing to your feeds and even I achievement you
access consistently rapidly. http://dragon-slave.org/comics/KathyerStonorkn
Finding knowledgeable professionals like those at # # anyKeyWord# has made all the difference during repairs! plumbers Bethlehem
Impressive depth showcased throughout every paragraph reinforces credibility surrounding both expertise levels displayed alongside thorough research efforts undertaken behind scenes leading up toward publication date itself. Holly Springs water heater repair
มีใครอยากแชร์รูปไฟหน้ารถ LED ของตัวเองบ้าง? ร้าน เปลี่ยน หลอดไฟ led รถยนต์ ใกล้ ฉัน
Remodeling can be a great investment—learn more about it at Remodeler Near Me !
This was a great article. Check out cheap plumbers near me for more.
For anyone in Lee’s Summit needing water heater assistance, I highly recommend checking out water heater installation lees summit .
Nicely done! Discover more at heater installation .
I’m impressed by how you connect historical events with current issues in your posts at Arms & Ammunition Dealers .
Sustainable materials are key for modern remodeling—learn more about them at Home Remodeling .
If some one wishes to be updated with most recent technologies
therefore he must be pay a visit this web page and be up to
date all the time. http://Dragon-Slave.org/comics/ShawneewrBarriosnj
If some one wishes to be updated with most recent technologies
therefore he must be pay a visit this web page
and be up to date all the time. http://Dragon-Slave.org/comics/ShawneewrBarriosnj
The kitchen is the heart of the home! Find out how to remodel yours at Kitchen Remodeling .
Just wrapped up a project with a great #roofing contractor#. Highly recommend them! roofing services london ontario
Homebuyers should never underestimate the power of a good real estate agent! This article was very informative—check out affordable realtors for more!
Just had an energy audit done by an HVAC contractor from Poway, and they recommended licensed hvac company poway for any future work.
Just performed due to #`#` anyKeyWord #`#, and I can’t exhibit how grateful I am for his or her professionalism in the course of my flow!” empresa de mudanças em jundiaí
I’ve used a couple of relocating providers ahead of, yet none compare to the performance of mudança em Jundiaí . Great for each residential and commercial needs!
Thanks for the thorough article. Find more at Springboro roofing companies .
I’m always amazed by the before-and-after photos of Austin homes! Check out ours: Bathroom Remodeling Austin .
Just finished by using mudanças em Jundiaí for my home relocation—well suited service all around!
Appreciate the helpful advice. For more, visit Landlord certificates .
This was a fantastic resource. Check out shower refinishing near me for more.
Thank you for the auspicious writeup. It in fact was
a amusement account it. Look advanced to far added agreeable from you!
By the way, how can we communicate?
Really glad you covered this topic, since finding quality info like this locally in Media, PA isn’t always easy. Your explanation of reinforcement techniques was super helpful Patio construction
This was a great article. Check out best roofing services company for more.
Thanks for the thorough article. Find more at roofing contractors .
Thanks for the great tips. Discover more at car accident lawyer near me .
Thanks for the thorough analysis. More info at hormone replacement therapy for women palm desert .
This was very beneficial. For more, visit Walter’s BBQ Southern Kitchen .
Appreciate the thorough information. For more, visit best gutter repair near me .
Just did some research and found that clogged vents can cause health issues too—thankful for services like those offered by Dryer Vent Cleaning Seattle #!
I always find your posts enlightening and packed with useful information! best real estate agent for buyers
The last time I called a plumbers in Valparaiso, they were so efficient!
This is highly informative. Check out Bedrock Plumbing & Drain Cleaning for more.
This was a fantastic resource. Check out Bathtub resurfacing for more.
Selling your house in Michigan can be overwhelming, but with the right tips, it can be a breeze! Check out cash for homes michigan for great resources.
A reputable car accident attorney will guide you through each step of the process confidently! georgia accident attorney
This was a wonderful guide. Check out custom mommy makeover packages for more.
This is very insightful. Check out Kitchen remodeler contractor for more.
Your breakdown of state-by-state regulations at Popular Gun Dealers is a much-needed guide for gun owners.
This was quite useful. For more, visit Fort Worth roofing companies .
Knowing someone has your back makes daunting tasks less intimidating overall…which is why trusting experts like these will prove beneficial later down road ahead!! Apopka apartment movers
This was very beneficial. For more, visit https://www.acid-bookmarks.win/how-to-repair-a-slow-draining-sink-and-a-slow-heating-area .
A good relationship with your real estate agent can lead to better deals and smoother transactions! Explore tips on this topic at real estate agent Ooltewah .
Thanks for the valuable article. More at Walter’s BBQ Southern Kitchen .
This was quite informative. More at Mikita Door & Window – Long Island Door Installation .
Sunscreen is a must-have in any routine! Thanks for the reminder. I recently discovered some fantastic sunscreens at facials near me .
Makes me want to go check my own unit right now—I’ll be sure not to neglect it any longer!# # anykeyword ## tankless water heater repair
Thanks for the thorough analysis. More info at https://www.bestbookmarks.win/why-you-might-need-a-gas-plumber-near-me .
Accidents can happen in the blink of an eye. It’s crucial to stay alert on the road! truck attorneys
Reading these tips makes me want to ensure my water heater is functioning optimally – thanks, and shoutout to water heater repair
After my recent accident, I learned that hiring an attorney is essential for navigating personal injury claims effectively! Visit Car accident lawyer to connect with experts.
Your article has made me realize that many small repairs can be done without professional help—very encouraging info! electrician englewood
The gentle flow between movements makes every session feel fluid and seamless!!! # # anyKey word # # Aventura Pilates
Combien de temps devrait prendre la création d’un site par une bonne agence web selon vous ? communication numérique Lozère
Have you tried combining fillers with your Botox treatment? What was your experience? botox treatment red bank
Could you elaborate on the differences between various sanding techniques used in restoring hardwood? Flooring Contractor
Had a minor electrical issue, and Salem electrical services solved it quickly! Highly recommend visiting Salem electrical services for their expertise.
Great insights! Find more at gutter repair .
Sharing personal stories about caregiving can inspire others; let’s spread awareness through sites like elderly care !
This was a great help. Check out emergency water leak repair for more.
Had an emergency situation arise right before our scheduled date—but they accommodated us without blinking!” Explore additional services offered by quality movers like this one over on # # 任何关键字 # # ! Little Elm Mover’s
Love how you’ve discussed the impact of layout on mood and functionality in spaces! Florida Interior Designer
The effectivity of the crew at empresa de mudanças em jundiaí in the time of my recent movement was marvelous! Highly endorse their services.
Moving is on no account elementary, however having seasoned movers from mudança em Jundiaí made each of the difference for my circle of relatives. Highly suggest their facilities!
Does any individual use their potential washer in general for the period of iciness months too, or is it strictly hot weather tools?? https://musescore.com/user/104718163/
잠실 윈 가라오케를 찾고 계시다면 윈가라오케를 주목하세요.
서울 송파구 잠실동에 위치한 윈가라오케는 10년 이상 꾸준히
사랑받아 온
This was nicely structured. Discover more at quick gas safety checks .
“Such lovely captures of love stories happening right here in our city!” Ikonic Media wedding photographer birmingham
My family has relied on the plumbers from plumbing services for years now – always reliable and professional.
Thanks for the great information. More at exploring brunch menus in Pittsburgh .
I can’t believe how quickly ### responded to my call! They’re the best plumbers in town! plumbing services Valparaiso
Excellent beat ! I wish to apprentice even as you amend your website, how could i subscribe for a weblog site?
The account helped me a acceptable deal. I were a little bit acquainted of this your broadcast
offered shiny clear idea
Do you prefer modern or traditional styles for home remodeling? Share your thoughts and check ours out: Kitchen Remodeling Austin
Open shelving is becoming more popular in kitchens—get inspired with us at Remodeler Near Me .
Thanks for the great tips. Discover more at Boiler breakdowns .
Thanks for the helpful article. More like this at affordable boiler replacement .
Appreciated hearing perspectives shared emphasizing significance tied closely between ongoing training conducted amongst contractors engaged daily within field ensuring skill sets sharpened continuously adapting meet demands evolving l roof repair
Appreciate the useful tips. For more, visit blocked drain plumber .
Staying organized becomes crucial ensuring no detail overlooked throughout entire duration litigation efforts ongoing continuously! georgia car accident attorney
I never believed in chiropractic care until I tried it! A Gig Harbor Chiropractor truly changed my life. Chiropractor Gig Harbor
This post highlights the importance of insulation in maintaining comfort and reducing energy costs. I’ll definitely consider high return insulation for my home in Rolling Hills Estates, CA! Garage door insulation
I’m taking into consideration renting a pressure washer for my spring cleaning—impressive recommendations for first-timers here! https://wiki-cafe.win/index.php/Pressure_Washer_Attachments:_What_You_Need_for_Every_Job
Hey There. I discovered your blog using msn. This is an extremely neatly written article.
I will make sure to bookmark it and return to read extra
of your helpful information. Thank you for the post. I will definitely
return.
Is it beneficial to offer incentives like closing cost assistance when selling your home?? Check insights on this topic via selling a house as is in michigan
This is highly informative. Check out emergency plumber prices for more.
I love how Firearms Accessories promotes a balanced view on gun rights and responsibilities. Well done!
Thinking of adding a second story? It’s a great way to gain space—learn more here: Home Remodeling in Austin Texas !
เมนูเครื่องดื่มที่ร้านเหล้าสาย1 มีให้เลือกหลากหลายมากๆ ครับ ร้านเหล้าหนุ่มหล่อ สาย1
Kitchen islands are a hot trend—learn how to incorporate one into your remodel at Kitchen Remodeling Austin !
There are many factors that influence the cost of #roof replacement london ON#; make sure you understand them before starting your project. roof replacement
“This kind of community support makes all the difference during stressful times like relocations!” Fort Worth full service movers
If you’re considering a new water heating system, definitely look into going tankless – you won’t regret it! water heater repair
Excellent communication and service from the electricians at vancouver electrical contractors .
Thanks for the helpful article. More like this at Comprehensive pest management Chester .
Great advice on preparing adequately before taking off on an adventure abroad; also check into comprehensive coverage options available via: travel agency Ann Arbor !
Watching motion pictures showcasing gifted pooches performing tricks creates smiles in all places —Is there ONE trick/act that keeps spell binding audiences on line nowadays according TO YOU ? https://victor-wiki.win/index.php/Inspiring_Stories_of_Service_Dogs_Changing_Lives_Every_Day
This is a must-read for anyone considering DIY electrical work. So many great tips! electrician near me
Witnessing breathtaking stunts carried out via agile border collies has turn out to be rather enjoyable by using social media channels; Which breeds amaze YOU normally right through performances showcased? https://oscar-wiki.win/index.php/Seasonal_Care_for_Dogs:_Keeping_Your_Pup_Safe_Year-Round
The staff at Cheap movers Richardson # were incredibly friendly and professional throughout my moving process!
Appreciate the thorough insights. For more, visit phim sex hàn quốc .
It’s fascinating how much difference just a few units of botox can make—amazing results! botox service
This blog is a treasure trove of information on all things roofing! Keep up the great work! roofing contractor
Appreciate the comprehensive advice. For more, visit instant payday loans new orleans .
Yourr mthod of telling the whole thing in this paragraph is actually fastidious, all
be ablpe tto effortlessly be aware of it, Thanks a lot.
Here iis my webpage – instagram şifresiz takipçi
This is quite enlightening. Check out https://www.plurk.com/p/3hh8rcyl35 for more.
Useful advice! For more, visit https://maps.app.goo.gl/RfRgjeNRHWjBMUvYA .
I found this very helpful. For additional info, visit https://maps.app.goo.gl/R7J185obAT4YSRBE9 .
Great beat ! I wish to apprentice at the same time as you amend your website, how
can i subscribe for a weblog website? The account aided me a acceptable deal.
I had been tiny bit familiar of this your broadcast offered shiny clear idea
pgwin
Great tips on plumbing maintenance! It’s crucial to keep everything in check. Check out plumbing services Bethlehem for professional help!
Fantastic insights into common issues like leaks and strange noises from the heater—very relatable! water heater replacement
Caring for a loved one with dementia can be challenging. I found some useful guides on reliable home care services that really helped me navigate this journey.
Thank you for providing a platform that encourages responsible discussions about firearms and their use, such as seen on Sports Air Guns, Airgun manufacturers, suppliers & exporters .
Excellent article. Keep posting such kind of information on your
page. Im really impressed by your blog.
Hey there, You have performed an incredible job. I will certainly digg it and individually recommend to my friends.
I’m confident they will be benefited from this web site.
I recently had my backyard fenced by a local company in Surrey, and the quality is outstanding! Best Fence contractor in Surrey CA
Appreciate the detailed post. Find more at Walters Barbecue Southern Kitchen .
This review really opened my eyes—no pun intended .
I’d seen iGenics ads claiming to fix vision in just
a week, and it honestly sounded too good to be true. Glad you broke down the Yale
research and gave a realistic perspective. Super helpful!
Homebuyers should never underestimate the power of a good real estate agent! This article was very informative—check out real estate agent for more!
There’s certainly a great deal to know about this issue.
I really like all the points you made.
Great insights! Discover more at abogados en A Coruña .
Finally, a review that isn’t afraid to dig into the facts instead of just hyping
the product! The way you broke down the ingredients and the science (or lack of it) behind Sugar Defender was super eye-opening.
Appreciate the honesty!
Useful advice! For more, visit Leaking radiator valves .
If you’re in want of helpful relocating capabilities in Jundiaí, ascertain to envision out what’s furnished by using empresa de mudanças em jundiaí !
I just couldn’t go away your website prior to
suggesting that I really enjoyed the standard info an individual
provide in your guests? Is going to be again steadily in order
to inspect new posts
Transporting an entire place of business can also be daunting, but now not with the guide of mudança em Jundiaí ! Their commercial options are magnificent!
Feel free to ask questions before hiring someone; trust me when I say you’ll love working with # # anyKeywod ###.” trusted hvac contractors
The proposal of the usage of a must-have oils in cleaning is staggering! Not best does it scent terrific, but additionally it is proper for you. I’ll look at various out House Cleaners for extra tactics to incorporate them!
Thanks for the insightful write-up. More like this at bundled mommy makeover options .
Thanks for the useful post. More like this at washing machine appliance service .
Appreciate the detailed insights. For more, visit professional commercial pest control Chester .
A nicely-positioned digital camera may want to stop so many topics—thanks for highlighting that point on your article! https://mag-wiki.win/index.php/Choosing_the_Right_Lenses_for_Optimal_Camera_Positioning
I not at all conception approximately the significance of battery life administration while flying drones! Great reminder! For further insights, payment out https://www.symbaloo.com/mix/bookmarks-onbn .
Hello! I know this is somewhat off topic but I was wondering if you knew
where I could get a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having problems finding one?
Thanks a lot!
Anyone else impressed by how organized the crew from Cheap movers Garland was during their move?
This was quite useful. For more, visit Walters BBQ Southern Kitchen .
สาวกขับรถกลางคืนต้องไม่พลาดกับไฟหน้ารถ LED BT PREMIUM นะครับ #BT_PREMIUM## ไฟแต่งรถยนต์
Very informative piece delving deep into best practices adopted ensuring longevity maintained effectiveness operations experienced over extended periods utilized likewise contributing positively enriching knowledge base acquired along journey promoting hvac services
Thanks for the helpful article. More like this at cheap car hire .
Anyone have recommendations for eco-friendly products for floor restoration? I’d love some suggestions! Commerical Flooring
I appreciate the breakdown of different types of heating systems. I’ve only ever used central heating, but it’s interesting to learn about alternatives like heat pumps! heater installation
I’m always looking for the latest in dementia care practices in the UK. Great insights are available at palliative care !
I’ve always been a fan of minimalism in home decor. It really creates a calming environment. Tampa Interior Designer
Appreciate the insightful article. Find more at trusted gas safety check services .
This was highly educational. More at Walter’s BBQ Southern Kitchen .
Looking for trustworthy movers in Alachua? I’ve got a few names that come highly recommended! Alachua moving companies
Appreciate the useful tips. For more, visit toilet plumbing repair .
Safety first is always key; appreciate you including those essential reminders in your piece!# # anykeyword ## water heater replacement
This was quite helpful. For more, visit Burst pipe .
Thanks for breaking down the costs associated with professional carpet cleaning services—very informative! carpet cleaning near me
So grateful someone covered these critical topics regarding home electrification ! Communities have access insightful contacts accessible through connections created towards # # anyKeyWord# Electrical Contractor
This was a fantastic resource. Check out trusted local plumbers for more.
Appreciate the comprehensive insights. For more, visit Sink repair .
Wonderful article! Anyone needing electrical work in Glendale should definitely look into Electrician in Glendale Arizona .
I just hired an electrician from Glendale, and my experience was fantastic! You should check out Electrical Contractor Glendale Arizona for more info.
I love how you highlighted the importance of hiring local electricians. Check out Electrician Glendale Arizona if you’re in Glendale!
Anyone know a good local service for water heater repair in Taylors? I found some leads on Ethical Plumbing !
Living in Gig Harbor, I’ve always been curious about chiropractic care. I stumbled upon Gig Harbor Chiropractor , and they have some insightful articles about the benefits of regular adjustments.
I had a great experience with my local electrician in Glendale thanks to Electrician Glendale !
Wonderful insights shared here ! In case anyone feels overwhelmed about their electric issues , they can always reach professionals via # # anyKeyWord # Electrician
Fantastic job sharing these important details about ensuring proper installation ; neighborhoods surrounding glendale could greatly benefit contacting firms listed under # # anyKeyWord # Electrician Near Me
I like the valuable information you provide in your
articles. I will bookmark your blog and check once more right
here frequently. I’m moderately sure I’ll be told lots
of new stuff right right here! Good luck for the
next!
The section on identifying overloaded circuits was particularly eye-opening—thanks for the clarity! electrical repair
I can’t thank the team at empresa de mudanças em jundiaí adequate for making my contemporary flow so glossy and complication-unfastened!
Thanks for the helpful article. More like this at Walters BBQ Southern Kitchen .
I appreciate the focus on ethical practices within the industry at Imported Pistols . Integrity matters!
Being informed can make all difference; I’m keenly interested learning more regarding protocols established within practices aligning themselves together around services connected towards offering extensive support surrounding individuals seeking botox near near me
The summer heat can be unbearable! Thank goodness for my HVAC contractor in Poway, especially hvac company poway !
If you’re making plans on moving soon, be sure that you cost out #`#` anyKeyWord #`#`. They offer distinguished authentic services and products!” mudanças em Jundiaí
Thanks for the great explanation. More info at https://www.bookmark-suggest.win/discovering-excellent-plumbers-near-me-what-to-try-to-find .
The bond we share with our puppies normally lasts a life-time; what recollections do you cherish maximum with yours? Reflect with us on https://tango-wiki.win/index.php/How_to_Keep_Your_Dog_Mentally_Stimulated_at_Home .
# anykeyword # responded quickly and professionally when we encountered serious wiring issues. electrical company vancouver
Amazing perspectives shared revealing transformative power architecture holds reshaping urban l Chattanooga realtors near you
This article covered so many relevant topics surrounding best practices adopted over time; any individual currently living nearby ought make contact through utilizing resources offered via ### ## licensed hvac company san diego
Wonderful tips! Discover more at abogados A Coruña .
Planning to sell your house with pets? Tips on how to manage showings are available at sell your house fast for cash michigan !
Thankful for the excellent service from my go-to Valparaiso plumbers in Valparaiso!
Who else is tired of dealing with old pipes? Time to upgrade with help from Bethlehem plumbers !
The influence of cultural tourism on global understanding is remarkable! Read more insights at travel agent Ann Arbor .
This was quite useful. For more, visit colchones Albacete .
The aftermath of an auto accident can feel isolating; don’t hesitate to seek legal counsel from experts like those at Auto Accident Lawyer .
มีใครเคยมีประสบการณ์ไม่ดีจากการใช้ไฟหน้ารถ LED บ้าง? ร้านซ่อม ไฟรถยนต์ ใกล้ฉัน
Thanks for sharing tips on estimating stucco repair costs! It’s good to know that I can calculate the materials and labor beforehand. Definitely going to reach out to a Stucco contractor Fort Saskatchewan for a quote. Find more info
If you’ve been involved in an auto accident, don’t hesitate to reach out to a qualified lawyer who understands Alaska laws—find one at Anchorage injury attorney !
The importance of a good listing description cannot be underestimated! Henderson real estate trends
This is quite enlightening. Check out Aestheic Plastic Surgery & Laser Centre for more.
I appreciated this post. Check out Affordable Pest Solutions for more.
I found this very helpful. For additional info, visit same day leaking dishwasher repair .
Love the inspiration of the usage of baskets for firm! They actually assist care for order in busy families. Thanks for sharing; I’m excited to discover greater at House Cleaning Company !
Thanks for the helpful article. More like this at LuxeNeuro .
It’s amazing how art and music therapy can benefit those with dementia! Read more about these therapies at personalized domiciliary care .
It’s an amazing post in support of all the online viewers; they will obtain advantage from
it I am sure.
Thank you for addressing common misconceptions about firearms on guns for sale ! It’s crucial to clear up misinformation.
The low-impact aspect of Pilates makes it perfect for those recovering from injuries! pilates studio near me
Well done! Find more at Walters Barbecue Southern Kitchen .
Do you think that making an investment seriously prematurely pays off long-term or would waiting until later turn out wiser financially??? # https://musescore.com/user/104734615/
I’m amazed at how compact my new tankless water heater is – perfect for our small home! Ethical Plumbing
Appreciate the comprehensive insights. For more, visit professional leak detection .
Great insights! Find more at abogados en A Coruña .
Do you know what to do after a car accident? Check out the insights at truck injury lawyer !
I have an understanding of your concepts on components that adorn drone pictures; they could make a colossal difference in output exceptional! For similarly recommendation, investigate out https://atavi.com/share/xcp64mz1ilsr1 .
I’m curious about trying out some natural cleaners instead of chemical ones after reading your recommendations—excited to experiment! carpet cleaning service Mission Viejo, CA
Thanks for the detailed guidance. More at phim hiếp dâm .
The statistics you shared about electrical fires were shocking but necessary reading; everyone should be aware!! electrician Salem
”Looking for recommendations on reputable contractors who specialize in energy-efficient installations!!! ## hvac contractor lake oswego
This is very insightful. Check out https://www.emergbook.win/discovering-great-plumbers-near-me-what-to-seek for more.
Thanks for shedding light on what affects the cost of electrical work! It’s great to have a rough idea before reaching out to professionals. For local help, visit electrical companies near me! electrical companies near me
This was quite useful. For more, visit affordable plumbing line services .
Thanks for the useful suggestions. Discover more at colchones Albacete .
Having multiple canine brings double (or triple) the pleasure—how do they get along at the same time ? Let’s chat approximately sibling dynamics amongst doggies over ### anykeyword ### https://alpha-wiki.win/index.php/The_Top_10_Most_Popular_Dog_Breeds_in_15793
Thanks for breaking down the different types of roofing materials! If you’re looking for quality installation, don’t forget to visit roofing services .
Valuable information! Discover more at Aesthetic Plastic Sugery & Lasor Center .
This was quite enlightening. Check out Affordible Pest Solutions for more.
Taking proactive measures limits exposure unnecessary delays caused unforeseen circumstances arising suddenly unexpectedly leading potential complications further delaying completion timelines originally discussed beforeh roofing services london ontario
Just wanted to share my positive experience with a local plumber in Bethlehem who helped with my kitchen renovation! plumbing services
The step-by-step guide is exactly what I needed for my DIY project! Appreciate the clarity. water heater installation
Thanks for the detailed post. Find more at Walter’s BBQ Southern Kitchen .
Just had my first chiropractic appointment in Gig Harbor, and I feel amazing! If you’re looking for relief, check out Car accident chiropractor for some great information on local services.
Thanks for the great information. More at Denver based neurofeedback clinic .
Valuable information! Discover more at toilet plumber .
Your post has inspired me to take charge of my home’s plumbing needs more confidently! water heater repair lees summit
This was a fantastic resource. Check out gas safety assessment for more.
If you’re in the hunt for authentic movers in Jundiai, look no extra than empresa de mudanças em jundiaí —they’re comfortably the absolute best!
Thank you for emphasizing the importance of using a professional service every now and then—so true! carpet cleaning service
I’ve used numerous transferring capabilities sooner than, yet none compare to the effectivity of mudança em Jundiaí . Great for the two residential and advertisement wishes!
Appreciate the helpful advice. For more, visit local central heating specialists .
Moving offices can be daunting, but with the right team, it can be a breeze. I found great help from Cheap movers Fort Liberty when I moved my business in Fort Liberty.
The team at licensed hvac company was prompt and professional when handling my HVAC issues—thank you, Poway!
Anyone else impressed by sheer dedication displayed consistently exhibited professionalism demonstrated unwavering commitment delivering exceptional quality results consistently achieved meeting expectations surpassed ultimately culminating fulfilling Glendale international movers
Thanks for the informative post. More at Walters BBQ Southern Kitchenac .
So grateful for the appliance repair team in Arlington! They helped me out when my washer broke down unexpectedly. google.com
Just achieved driving #`#` anyKeyWord #`#, and I can’t express how thankful I am for their professionalism all over my pass!” mudanças em Jundiaí
Thanks for sharing insights on HVAC maintenance! If you’re in San Diego, you should consider hvac contractor for your needs.
Love watching community come alive invigorated motivated inspired empowered ready tackle whatever lies ahead knowing resources available guidance support reassurance felt throughout journey taken together collectively seeking better tomorrow filled Margate Mover’s
The emotional toll of an accident can be heavy; having legal support helps lighten the load! car accident attorney
Plumbing issues can be stressful, but with plumber near me , I felt at ease knowing they were handling it.
I never realized how vast the topic of roofing could be until now; thank you for expanding my knowledge base!! roof repair
Thanks for the valuable insights. More at https://www.bookmark-tango.win/exactly-how-to-fix-a-clogged-shower-drain-and-an-ineffective-heating-unit .
The tips for maintaining firearms shared at Pistol wholesalers & distributors are practical and easy to follow.
A friend recommended # # anyKeyWord# # when I mentioned needing movers—I’m glad she did! Long distance movers Jamaica
Highly recommend plumbers Justin for all your plumbing needs in Justin!
Had such a smooth transition thanks to the amazing team at ### anyKeywod###–highly recommended! Bronx moving companies
Do special dog breeds adapt more desirable to colder climates than others? I’d like to be taught extra approximately this! read more
Appreciate the comprehensive insights. For more, visit hvac near me .
Thanks for the clear advice. More at Affordable Brunch Pittsburgh .
Every case is unique—personalized attention from a skilled attorney is key after any auto wreck! Explore options at car accident representation # now!
Amazing perspectives shared revealing transformative power architecture holds reshaping urban l realtors near me
Wonderful tips! Discover more at ac service .
This blog encourages me to take better care of my skin! I’m eager to explore further resources like those at beauty salon barnsley .
Your approach towards explaining maintenance needs after initial setups helps ensure longevity—excellent point raised here! water heater replacement
Appreciate the comprehensive insights. For more, visit abogados en A Coruña .
This post really emphasizes the importance of communication with your real estate agent! Thanks for sharing these tips—check out more at Chattanooga realtors .
I’ve had great experiences with international travel insurance. It really paid off during my last trip! For more info, see travel agent Ann Arbor .
Don’t hesitate sharing more articles like these—they’re genuinely appreciated by all homeowners tackling similar challenges!!!# anyKeyWord# lees summit water heater repair
การเปลี่ยนมาใช้ไฟหน้ารถ LED BT PREMIUM ทำให้รถดูทันสมัยขึ้นครับ หลอด ไฟ หน้า รถ led
Thanks for the valuable article. More at affordable leaking dishwasher services .
Don’t enable termites take over your own home! I came across advantageous answers by using Mosquito Control Wildwood, NJ that helped me regain handle of my belongings in Cape May Court House.
This was quite useful. For more, visit tienda de colchones .
Rodents had been inflicting havoc in my storage, yet after hiring https://maps.app.goo.gl/eMWYBJiUsixRUJzE6 , these pesky critters are long gone for nice! Great service and professionalism.
I would love advice on how often one should schedule follow-up appointments after initial injections done through professionals like those at ### any keyword### botox near near me
It’s refreshing to see a site like Sports Air Guns, Airgun manufacturers, suppliers & exporters that values education over sensationalism in the firearms debate.
O sistema de recompensas do Vá para o site para quem joga video slots é bastante atrativo.
Commercial pest offerings are a must for businesses in Brick! I found an glorious service as a result of Termite Treatment Toms River, NJ that extremely understands the local pest topics.
Fantastic tips on finding a good electrician! In Salem? Go with Cornerstone Services !
I always spent my half an hour to read this
blog’s articles every day along with a mug of coffee.
Rodent complications can amplify temporarily, so or not it’s high-quality to behave rapid! If you’re in Broomall and desire rodent keep an eye on, look at various out the companies awarded through https://maps.app.goo.gl/CAv1C2pMXxTktdNQ7 .
This was quite informative. For more, visit Affordible Pest Solutions .
The best part about living in Englewood is the access to skilled electricians listed at electrician near me .
Appreciate the useful tips. For more, visit home cleaning companies near me .
The point of provider I bought from ##Rodent Control Pawtucket## was significant! They took care of my rodent difficulty efficiently and have been very legitimate. https://maps.google.com/maps?ll=41.865088,-71.402779&z=16&t=h&hl=en&gl=US&mapclient=embed&cid=12737174504955965871
The section discussing common signs that indicate repair needs was particularly valuable; I’ve experienced some of those issues firsthand and didn’t realize they were red flags before reading this post! air conditioning repair
Thanks for the great explanation. Find more at payday loans new orleans la .
For effective residential or commercial transport answers in Jundiai, seem no in addition than mudança em Jundiaí !
Awesome article! Discover more at local plumbers recommended .
Just got my HVAC system installed by licensed hvac company and couldn’t be happier with the results!
How long does it typically take to install a fence with professional help? Curious about timelines! https://maps.app.goo.gl/zFoBM7QV13WaedDn7
I adore eclectic decor styles, but how do you avoid making them look chaotic? Any tips? Virtual Interior Design Services
Thanks for the helpful advice. Discover more at quick reliable plumber services .
I appreciate how informative your posts are about dementia care in the UK! I found even more resources at palliative care .
This was very beneficial. For more, visit LuxeNeuro .
You covered some key points. The discussion on documenting medical care struck a chord, especially if treatment is ongoing. As someone who lives in Bear, DE, having a clear guide like this is incredibly useful pedestrian accident lawyer
Anyone used a Grand Island moving company lately? Maybe I should try Grand Island full service movers ?
This was quite informative. More at security guard company .
Just wanted to share how satisfied I am with the service from licensed hvac company san diego !
I enjoyed this read. For more, visit hvac repair .
Thanks for shedding light on who to contact when my AC isn’t working—it’s so important to know where to turn, especially places like ac repair Las Cruces NM! ac repair near me
Tapping into collective knowledge builds stronger foundations ensuring better outcomes overall—grateful indeed knowing about plumbers Bethlehem
Appreciate the detailed post. Find more at medical weight loss clinic palm desert .
This was a wonderful post. Check out https://www.hotel-bookmarkings.win/comprehending-and-utilizing-a-p-trap-in-pipes for more.
Hmm it looks like your website ate my first comment (it was super long) so I
guess I’ll just sum it up what I had written and say,
I’m thoroughly enjoying your blog. I too am an aspiring blog
writer but I’m still new to everything. Do you have any tips for first-time blog writers?
I’d genuinely appreciate it.
Thanks for the useful post. More like this at same day plumber near me .
Wonderful insights shared here ! In case anyone feels overwhelmed about their electric issues , they can always reach professionals via # # anyKeyWord # Electrician Glendale Arizona
I’ve been curious about the average rates electricians charge in North Carolina. It’s great to see discussions like this! Knowing that electricians in Charlotte NC can have varying rates helps when budgeting for my home renovation electrical companies near me
Good to know about local resources! For electrical services in Glendale, look at Electrical Contractor Glendale Arizona .
Hi there! I understand this is sort of off-topic but
I had to ask. Does managing a well-established website like yours
take a lot of work? I’m brand new to writing a blog however I
do write in my journal daily. I’d like to start a blog so
I can easily share my personal experience and views online.
Please let me know if you have any kind of recommendations or tips for new
aspiring blog owners. Thankyou!
Great insights on electrical safety! If anyone needs an electrician in Glendale, AZ, visit Electrician Near Me for excellent service.
Keep this going please, great job!
This was a fantastic resource. Check out Walter’s BBQ Southern Kitchen for more.
Wonderful collection of ideas presented here surrounding efficient repairs versus replacements necessary occurring frequently across homes nationally ; likewise locals can see whom specializes around them accessing resources located under Electrician
I know this if off topic but I’m looking into starting my own blog and was curious what all is required to get setup?
I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% certain. Any recommendations or advice
would be greatly appreciated. Thank you
Did you realize that canines can lend a hand curb strain tiers significantly? What calming options do you use with yours? Talk about it over at https://fair-wiki.win/index.php/Understanding_the_Canine_Sense_of_Smell:_How_It_Works !
This was very enlightening. For more, visit abogado .
I’m impressed, I have to admit. Seldom do I encounter a blog that’s both
equally educative and engaging, and without a
doubt, you have hit the nail on the head. The problem is an issue that not enough folks are speaking intelligently about.
I am very happy I came across this in my hunt for
something relating to this.
Thanks for the useful post. More like this at plumbing & heating near me .
Austin homeowners are so creative with their remodels! Discover more innovative designs on our site: Bathroom Remodeling Austin .
Asking questions are actually nice thing if you are
not understanding something completely, except this paragraph presents pleasant understanding yet.
Well explained. Discover more at local plumbing companies .
Can anyone recommend affordable yet quality ##roofing services london ontario##? roofers london ontario
I love listening to approximately distinct names other people supply their puppies; what’s the story at the back of your dog’s call? Share it over at https://mega-wiki.win/index.php/Canine_Enrichment_Activities_That_Will_Keep_Them_Busy_All_Day!_69174 !
Valuable information! Discover more at local roofing companies .
I can’t get adequate of pup photos! They’re simply too cute! Share your puppy graphics or stories at https://noon-wiki.win/index.php/Exploring_the_Benefits_of_Raw_Diets_for_Dogs !
I found the best residential electrician through electricians in vancouver and couldn’t be happier with the service.
This was quite useful. For more, visit underfloor heating system repairs .
This is highly informative. Check out colchones en Albacete for more.
If you may have a advertisement estate in Ambler, don’t wait unless pests turned into a drawback! Contact Rodent Control Ambler, PA for preventative amenities that avert your business pest-loose.
Appreciate the detailed insights. For more, visit reliable gas safety services .
Thanks to info from #AnyKeyWord#, I’m now well-prepared if my own system ever fails. Taylors water heater repair
Have you all seen how many celebrities rave about their Botox treatments? It’s definitely a trend now! botox red bank
I recently had a great experience with appliance repair in Arlington, TX. Highly recommend local services! appliance repair Arlington TX
I’m glad I found this blog! For those in need of an electrician, check out electrician near me in Salem.
Valuable information! Discover more at Top Brunch Pittsburgh .
Dealing with stubborn clogs? Trust me, you want help from experts like ### instead of DIY methods! plumbers
I found this very interesting. For more, visit benefits of neurofeedback treatment in Denver .
If you’re planning a move in Jamaica, I highly recommend checking out Best Jamaica movers for reliable services!
Appreciate the deep dive into how Mitolyn actually works.
I like that it doesn’t rely on stimulants, and the focus on mitochondrial support makes it
stand out. Thanks for keeping it real and science-based!
I found your article on self-defense laws at Pistol wholesalers & distributors to be very informative and timely!
Got some great maintenance tips from # # anyKeyWord # # —so helpful for keeping my system running efficiently! Rancho Bernardo Heating & Air
This was highly informative. Check out https://www.apu-bookmarks.win/searching-for-shower-repair-service-providers-near-me for more.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
This was very enlightening. More at Walters BBQ Southern Kitchenac .
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at worlds largest online paintball store !
This was quite informative. For more, visit hvac repair .
What does everyone recommend doing beforehand before starting actual installation processes?? Asking because I’ve heard horror stories… # lake oswego hvac company
Friendly reminder showing appreciation towards everyone initiating discussions around Quailty FIrst Buildee today—they’ve opened doors leading towards endless possibilities ahead!!!!!!!! Navigation directives follow through shortly should y’all wish best custom home builder
The tips on preventing pipe bursts are really helpful! I’ll remember to contact Bethlehem plumbers if anything goes wrong.
Your post makes me want to hit the beach right now! Any suggestions for unique coastal activities? travel agency myrtle beach
If you’re unsure about how to proceed after a car accident in Anchorage, reach out to an experienced attorney today. Visit Car accident attorney for guidance.
Just tried a reformer Pilates class for the first time, and I’m hooked! pilates studio
Who knew that proper insulation could lead to such significant savings? I’ll be looking into high return options for my home in Rolling Hills Estates, CA! Blown-in insulation
Appreciate the thorough insights. For more, visit expert heating service .
Just moved with empresa de mudanças em jundiaí and couldn’t be happier! Their crew was friendly, professional, and effective.
Love following your weblog as it continues me excited about holding not solely cleanliness but additionally getting better property value!!! # # anyK eyword ## Browse around this site
This support on drone flight patterns changed into eye-beginning! It will increase my qualifications really! Want to be informed greater? Visit https://www.bookmarkidea.win/adjust-the-camera-settings-in-line-with-your-setting .
For those seeking quality installation and service, you should definitely reach out to # # anyKeywod ###.” licensed hvac company poway
My friends were amazed at how quickly things started moving once I got my **# # anyKeyWord** involved! Injury Lawyer
The variety of serums available today is astonishing—I’m overwhelmed but excited to try them out after reading your guide! Discover more options at laser hair removal !
Valuable information! Find more at reliable plumbing .
Great job! Discover more at licensed plumber .
Is it just me or does everyone rely on their HVAC more during these hot months? Thanks, hvac contractor !
Great job! Discover more at Walters BBQ Southern Kitchen .
It’s nice knowing there’s a reputable **#plumber** available 24/7 in our area. plumbers
Great roundup of inspiring travel blogs—be sure to check out what else is available at: travel agency Ann Arbor
Wouldn’t go anywhere else but ### anykeyword ### when it comes to plumbers! plumbing services
Awesome article! Discover more at abogado .
Every story shared about successful restorations encourages others not just locally but across communities worldwide. Commerical Flooring
This was a wonderful post. Check out colchones en Albacete for more.
This was very enlightening. More at local emergency plumbing services .
Your exploration of historical roofing methods was fascinating—I never knew there was such variety over time! For modern solutions, visit roof repair !
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrical Contractor
Thankful for your insights into wiring safety practices; just wanted to share that if anyone needs an expert they can always find good ones through links like those at Electrician Near Me
I always read your posts for helpful info! For electrical services in Glendale, don’t miss Electrician in Glendale Arizona .
Consider sharing an apartment with friends to save money while enjoying great company! apartments for rent
Excellent resource sharing; you never know when you’ll need an electrician so locals should keep the info from this post along with links like those from Electrician Near Me
Quality articles or reviews is the important to be a focus
for the people to go to see the website, that’s what
this site is providing.
Whether hosting birthdays or casual get-togethers alike, people always rave about experiences shared because engaging together creates lasting impressions!” ### waterslides rentals near me
This was quite informative. More at home cleaning services near me .
This was a wonderful post. Check out affordable plumbing for more.
The role of technology in dementia care is fascinating! There are some great discussions on this topic at professional home care services .
I love the idea of multifunctional furniture, especially in small apartments. Great suggestions! Florida Interior Designer
I’m so happy with my new fence from this Surrey company; it really enhances my property! Fencing company Surrey CA
This was highly useful. For more, visit quick plumber response .
Thanks for the great tips. Discover more at Aesthetic Plastik Surgery and Lazer Center .
Appreciate the detailed information. For more, visit 24 hr plumber .
Thanks for the thorough analysis. More info at rent a car toronto .
“Do you also do engagement shoots? Would love more information about packages!” https://www.google.com/maps?cid=11358797318047951201
Your beforehand-and-after footage are so motivating; they inspire me to address these difficult outdoors cleaning jobs with my stress washing machine!! Visit this link
I found this very interesting. Check out find a plumber for more.
What are some common mistakes people make when hiring an HVAC contractor? Let’s share experiences! hvac company lake oswego
Excellent point about understanding warranties and what they cover; it’s crucial when investing in a new system! water heater installation
Your focus on youth education about guns and safety is so necessary, especially through platforms like Stallion Guns .
Thanks for sharing those packing hacks; rolling clothes really does save space in luggage! myrtle beach travel agent
Thanks for the thorough analysis. Find more at High Line Roofing, Fort Worth Roofers .
Thanks for the thorough analysis. Find more at LuxNuro .
What are the best tips for maintaining results after a Botox treatment from botox red bank ?
It’s fascinating how technology has improved carpet cleaning machines over the years—thanks for highlighting that! carpet cleaning service Mission Viejo, CA
I appreciate your tips on outdoor lighting; it really enhances curb appeal! electrician Salem
I can’t believe how quickly my issue was resolved by the team from electrical contractor vancouver !
Let’s continue fostering connections cultivating relationships built upon trust integrity ensuring everyone benefits collective efforts culminating shared successes realized each milestone celebrated together heartfelt appreciation expressed gratitude professional hoover portable toilet rental
Using respectable movers like the ones from empresa de mudanças em jundiaí makes each of the change—quite endorse their green treatments!
Thanks for the useful suggestions. Discover more at affordable blocked toilet repair .
Wondering whether it’s worth hiring someone outside family circle ?I suggest checking credentials linked up alongside our community members using# any key word#. electrician in englewood
Had a great experience with an HVAC repair from trusted hvac contractors —highly recommend them to anyone in Poway.
How much do bail bondsmen actually make in Alamance? I’ve been curious about their earnings and this post sheds some light on it. Time to check out Alamance bail bonds! Alamance bail bondsmen
I enjoyed this read. For more, visit ductless air conditioner repair near me .
This was a wonderful post. Check out Outdoor Event Venue for more.
If you might be on the search for mudança em Jundiaí , I surprisingly put forward their competent relocating suggestions in Jundiai for either residential and commercial necessities!
Wonderful work! That is the kind of information that are supposed
to be shared across the internet. Disgrace on the search
engines for no longer positioning this submit higher!
Come on over and consult with my site . Thanks =)
Thanks for sharing this valuable information! I’m curious about the installation process of high return insulation in Rolling Hills Estates. cellulose insulation
Useful advice! For more, visit colchones .
Really appreciated getting perspective shared throughout which highlights necessity underst hvac services san diego
I am really enjoying the theme/design of your web site.
Do you ever run into any web browser compatibility issues?
A handful of my blog visitors have complained about my blog
not working correctly in Explorer but looks great in Safari.
Do you have any recommendations to help fix this issue?
Nearly 70% of the men in the world are facing the problem of erectile dysfunction whether temporarily or permanently.
It’s essential to find a trustworthy Valparaiso plumbers in Valparaiso, especially for emergencies.
Thanks for the clear advice. More at affordable plumbing .
It’s heartening knowing there are dedicated professionals out there helping those affected by unfortunate events like car crashes!!! accident attorneys
Wonderful collection of ideas presented here surrounding efficient repairs versus replacements necessary occurring frequently across homes nationally ; likewise locals can see whom specializes around them accessing resources located under Electrical Contractor
Navigating insurance claims after a car accident can be tricky. A good lawyer from lawyers will ensure you get what you’re owed without unnecessary stress.
Awesome article full of practical advice on hiring electricians; locals might find what they need at Electrician Near Me
Wow this is really insightful information; it’s hard finding good electricians sometimes but I’ve seen positive reviews about those at Electrical Contractor Glendale Arizona
Wonderful tips! Find more at Chester Bug Control .
This was a great article. Check out safe mommy makeover for more.
Thanks for highlighting these issues ; locals facing similar challenges should connect with skilled individuals available through # # anyKeyWord # Electrician in Glendale Arizona
Really appreciate how well-informed plumber near me
This was very enlightening. For more, visit https://lockdowntheatre.net/user/blandailrx .
Valuable perspectives shared here within context we all need more education surrounding electricity & its usage ; local residents shouldn’t hesitate contacting teams affiliated via # # anyKeyWord # Electrician Near Me
Hi! I could have sworn I’ve been to this website before but after browsing through a few of the articles I realized it’s new to me.
Anyways, I’m definitely pleased I discovered it and I’ll be bookmarking it
and checking back often!
Real estate agents do so much behind the scenes that buyers often don’t realize until it’s too late! Discover more about their roles at experienced realtors Chattanooga TN .
I love how you keep your audience updated with current events in the gun industry through your posts at Suppressors & Gun Silencers Online !
Thank you for providing a platform that encourages responsible discussions about firearms and their use, such as seen on Stallion Guns .
Appreciate the thorough write-up. Find more at Neurofeedback Therapy Denver .
A great lawyer will fight for your rights and help you get what you deserve! vehicular accident lawyer
Your recommendations for tech tools every agent should use are fantastic—thanks for sharing! real estate agent advice
Appreciate the detailed information. For more, visit https://maps.app.goo.gl/9r1dXAVePs8KFAeEA .
Appreciate the helpful advice. For more, visit dishwasher repair services .
Thanks for the useful suggestions. Discover more at Walter’s BBQ Southern Kitchen .
This is quite enlightening. Check out dishwasher repair services for more.
Every time I need plumbing help, I call Justin plumbers without hesitation.
Love how quiet our new unit operates compared to the old one – such peaceful showers now!! #SoHappy tankless water heater repair
If you want quality work done, look no further than Salem electrical services! Visit their site at electrician .
The counsel about climate prerequisites affecting drone performance is needed for planning flights! Thanks for sharing that insight! More details may also be found out at https://www.bookmarking-keys.win/always-apply-native-rules-and-checklist-when-flying-your-drone-digital-camera .
I not ever learned how much a blank residence can impression my temper! Thanks for sharing these ideas on sustaining a tidy area. I’ll actually examine out House Cleaning Service for more suggestion!
Thanks for sharing your expertise on electrical systems! It’s comforting to know there’s help out there when needed. electrician englewood
This was a fantastic resource. Check out hormone replacement therapy for women palm desert for more.
Love the emphasis on both appearance and hygiene when it comes to carpets—great perspective! carpet cleaning service near me
This was beautifully organized. Discover more at kitchen sink drain .
I visit day-to-day some web pages and sites to read articles or reviews, however this
weblog offers quality based writing.
Having proficient provider animals really opens our eyes toward several counsel roles awarded by means of carrier-orientated breeds ; which function impresses YOU most concerning strengthen given by way of these robust companions? Website link
This was highly helpful. For more, visit reliable plumbing and heating services .
Can’t believe how much easier everything became once started communicating directly with representatives dedicated providing exceptional customer service throughout entire endeavor ! # # anyKeyWord ## Dallas commercial movers
I can’t believe how smooth my move was thanks to Ocala apartment movers ! Best movers in Ocala.
My friend just had their HVAC replaced, and they’re thrilled with the results! #HVAClife #contractor hvac services
This was highly useful. For more, visit plumbing contractors near me .
It’s amazing how many people overlook their water heaters until it’s too late. Great reminder! water heater installation Holly Springs
Thanks for the thorough article. Find more at Walters Barbecue Southern Kitchen .
This article highlights essential tips that every homeowner should know about finding plumbing services in Bethlehem! plumbing services
Just got settled into my new place thanks to # # anyKeyWord # #—they were amazing! Premier Mover’s Jamaica
“Your post made me think about adding personalized touches throughout the shoot day.” https://www.google.com/maps?cid=11358797318047951201
Well done! Discover more at Bathroom refurbishments .
Undoubtedly impressed witnessing transformations unfold steadily each passing moment illustrating power resilience enhancement exhibited consistently illuminating paths forward brightened hopes sparked dreams ignited fervently encouraging everyone embrace Cheap movers Hempstead
Moving can really take its toll physically and emotionally—thankful for professionals atagrandislandMovingCompanywho make it manageable!! # # anyKeyWord ## Long distance movers Grand Island
The impact of diet and exercise on dementia is an interesting topic! Explore more about it at compassionate elderly care .
I enjoyed this post. For additional info, visit tienda de colchones .
If you’re on a tight budget moving in Brooklyn, check out Brooklyn full service movers for great deals.
The effectivity of empresa de mudanças em jundiaí certainly stands proud! They taken care of my finished circulation smoothly and professionally.
Thanks for posting this! Understanding how lawyers deal with insurance adjusters helped me think differently, and it’s great to see relevance to New Castle County, DE accident lawyer
Shoutout to # # anyKeyword # # for helping me with my air conditioner install—great work! hvac company
Your blog really opened my eyes about the importance of regular checks; looking forward to working with ### anykeyword### soon. Dryer Vent Cleaning Seattle
After dealing with multiple issues, I finally found a trustworthy garage door company that resolved everything efficiently! Best Garage door company in New Caney TX
“I appreciate how well organized #Anykeyword was during our entire moving process.” Olive Mover’s Macclenny
This was quite enlightening. Check out https://sipse.ru/user/gardenqhci for more.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Such practical advice on dealing with stubborn stains; I’ll be sure to keep these tips handy for emergencies! carpet cleaning near me
I can not end raving approximately ###—their group’s dedication to targeted visitor pride is incredibly commendable. mudança em Jundiaí
For any San Diego homeowner, having a dependable HVAC service like hvac company near me is essential.
Appreciate the great suggestions. For more, visit medical spa near me .
Thanks for the useful suggestions. Discover more at private security near me .
This was quite informative. For more, visit Aesthetic Plastic Sugery & Lasor Center .
No more strain about shifting way to powerful features from mudanças em Jundiaí #! Check them out when you’re moving soon.
Appreciate the comprehensive advice. For more, visit rehab .
Hi, Neat post. There’s a problem with your web site in web explorer,
could test this? IE still is the market leader and a large part of people will omit
your great writing because of this problem.
This was very enlightening. For more, visit real estate agent near me .
Thanks for the helpful article. More like this at payday loans new orleans la .
Local #plumbers are worth their weight in gold; contact a trusted Valparaiso plumbers # today!
Has anyone used an appliance repair service recently? I’m looking at options around Arlington TX. appliance repair Arlington TX
Appreciated reading these guidelines presented today ; if everyone living around glendale searched properly they’d find assistance listed under # # anyKeyWord # Electrician Near Me
Does insurance usually cover visits to a chiropractor in Gig Harbor? I’d love to know before making an appointment! Chiropractor Gig Harbor
Portable bathroom rentals can make or break an outdoor event! Trust me, go with quick hoover porta potty rental service for your next event in Hoover.
“Appreciate how you broke this down without the usual hype. I was curious about GlucoBerry but skeptical about all the glowing reviews online. Your honest look at the ingredients and how they support blood sugar gave me a much clearer picture.”
Quick response times and great service make me a fan of ### anykeyword ###! plumbers Justin
It’s refreshing reading material that educates consumers effectively on best practices ; locals really ought connect with professionals available via # # anyKeyWord # Electrician Glendale Arizona
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrician
The importance of mental health awareness in relation to firearm ownership highlighted on Buy Suppressors & Gun Silencers Online is vital!
This was quite informative. More at 24 hour plumber .
This was a fantastic resource. Check out expert shower fitting for more.
It’s enjoyable seeing everyone’s reviews with regards to electrical vs gas concepts; could substitute views around procuring behavior!!!! # Visit this site
Your guide on water heater installation is very helpful! I’ll definitely keep this in mind. Visit tankless water heater repair for expert advice!
Great tips! For more, visit residential cleaning services near me .
Love the customer service at residential hvac company ! They truly care about their clients’ HVAC needs.
Love the thought of simply by baskets for corporation! They sincerely assistance sustain order in busy families. Thanks for sharing; I’m excited to explore greater at House Cleaning Company !
Exploring mindfulness practices alongside physical training through pilates enhances overall well-being!!!# anyKey word ## pilates studio near me
Looking into ways community involvement enhances visibility among prospective clients searching homes???? Engaging initiatives showcased illustrating successful outcomes available through __#anything_# sell my house fast in michigan
This was a wonderful post. Check out colchones for more.
Wonderful tips! Discover more at abogado .
The thrill of planning a new trip makes me want to expand my travel bucket list even more! myrtle beach travel agent
If you’re considering Botox in Red Bank, do your research first to find the best place! botox treatment red bank
Thanks for the informative content. More at emergency blocked toilet fix .
Appreciate the detailed post. Find more at full-service mommy makeover .
The installation of my tankless water heater was quick and easy. Best decision ever! water heater repair
Thanks for the detailed post. Find more at expert plumbing firms .
A good auto accident lawyer won’t just represent you—they’ll advocate for your well-being! Read more at Auto Accident Lawyer .
Such valuable information on negotiating with buyers and sellers through an experienced real estate agent—thanks for sharing this gem! Visit realtors in Ooltewah for further details!
This was quite useful. For more, visit emergency plumber .
Love this advisor! The video demonstration in point of fact helped visualize the process even more suitable! https://smart-wiki.win/index.php/Your_Comprehensive_Guide_to_Non-Pressure_Washing_Sidewalk_Maintenance
The potency of #`#` anyKeyWord #`#` made my traumatic relocation think like a walk within the park!” empresa de mudanças em jundiaí
Amazing explanations given regarding common pitfalls encountered during DIY projects surrounding installation/repair work as well – neighbors located nearby might want take advantage tapping into expertise sourced directly via ### ## hvac contractor
The interviews with industry experts featured on Pistol wholesalers & distributors are a fantastic addition to the discussion.
I look forward to seeing more content that explores the intersection of technology and firearms regulation over at ##anyKeyword#! Buy Suppressors & Gun Silencers Online
Thanks for highlighting these issues ; locals facing similar challenges should connect with skilled individuals available through # # anyKeyWord # Electrician Near Me
This was quite informative. More at ac companies near me .
Moving doesn’t have got to be overwhelming when you’ve got the properly staff! Check out mudança em Jundiaí for effectual relocating features.
Excellent writing showcasing importance prioritizing safety while managing household appliances effectively ; individuals wishing follow-up should access directories leading towards # # anyKeyWord# Electrician in Glendale Arizona
Excellent points made regarding community engagement by agents—it fosters trust and loyalty. find a Las Vegas realtor
This is highly informative. Check out ac contractors for more.
Seriously impressed observing attention given surrounding responsibility assumed ensuring health/safety concerns addressed adequately each time projects arise requiring specialized skillsets deployed effectively without fail ultimately yielding positive roofing services
This was beautifully organized. Discover more at Water heater repair .
You made a compelling case for why we should invest in professional services at least once a year—totally agree! carpet cleaning service near me
Agora estou animado para experimentar os novos caça-níqueis na próxima vez que acessar # anyKeyWord #! https://www.anobii.com/en/0176a9ba292fee4573/profile/activity
Excellent points about electrical maintenance! For residents of Glendale, AZ, check out Electrician Near Me .
Couldn’t imagine traversing path alone without outst custom homes sherman oaks
Moving can be a hassle but not with the help of Best Ocala movers ! Fantastic experience in Ocala.
A friend recommended a fantastic fencing service based right here in Surrey, CA—can’t wait to call them! Fencing company Surrey CA
Appreciate the detailed insights. For more, visit http://prosochi.ru/user/gordanqjid .
What’s Taking place i am new to this, I stumbled upon this I have found It absolutely helpful and it has
aided me out loads. I hope to contribute & aid other users like its aided me.
Good job.
Finally feeling optimistic regarding affordability challenges faced during life changes thanks largely attributed towards Hempstead moving companies
I was impressed with the efficiency of the commercial electrician I hired through electrician vancouver .
This was very beneficial. For more, visit car hire .
It’s amazing how much value a new, stylish garage door can add to your home—I’ll be consulting with my favorite local team soon! Garage door company New Caney TX
I just learned about some great tips for finding trustworthy ##roofing services london ontario## in our area. roofing services london ontario
Fostering inclusive conversations guides individuals navigate complexities encountered amidst journeys undertaken illuminating pathways revealing truths buried deep within hearts nurturing resilience strengthened fortified courageously embracing affordable botox red bank
My energy bills have decreased significantly since I switched to a tankless system. So worth it! Ethical Plumbing
That is a really good tip particularly to those new to the blogosphere.
Short but very accurate info… Thank you for sharing this one.
A must read article! https://www.ipsorgu.com/site_ip_adresi_sorgulama.php?site=blitribe.com/doku.php%3Fid%3Dlocation_de_bateau_a_magog%3Aexplo_ez_la_douceu_du_lac_memph_emagog
Just wanted to share my positive experience with Brooklyn full service movers as my Brooklyn movers!
All things considered reflectively speaking hindsight being 20/20 hindsight reflects very positively upon decision made collectively choosing wisely wisely indeed selecting carefully whom partner alongside undertaking various tasks requiring specialized electrician Salem
. Shoutout again to %%ANYKEYWORD%%—they made our entire transition smooth and easy Local movers Palm Harbor
Thanks for the useful suggestions. Discover more at https://univer-novaja-obschaga-v1.tnt-lordfilm.net/user/aubinamocf .
That is a really good tip particularly to those new
to the blogosphere. Short but very accurate info… Thank
you for sharing this one. A must read article! https://www.ipsorgu.com/site_ip_adresi_sorgulama.php?site=blitribe.com/doku.php%3Fid%3Dlocation_de_bateau_a_magog%3Aexplo_ez_la_douceu_du_lac_memph_emagog
This was quite enlightening. Check out residential cleaning services near me for more.
Been using Nitric Boost Ultra for a few weeks and I can seriously feel the difference in my endurance at the gym.
Plant-based and effective—loving it so far!
Being component of local rescue efforts guarantees limitless lives kept day-to-day – Is volunteering a specific thing near satisfactory FOR YOU also excited about assisting others? https://qqpipi.com//index.php/The_Evolution_of_Domestic_Dogs:_From_Wolves_to_Companions_75360
Thanks for the practical tips. More at commercial real estate agent .
Dogs have such an excellent feel of scent! It’s attention-grabbing how they use it in their day after day lives. Discover extra proof at https://wiki-cafe.win/index.php/Building_a_Strong_Bond_with_Your_Rescue_Dog_62919 .
What an informative article! I learned so much about lighting setups in a video recording studio. video recording studio
Sometimes witnessing competitive activities concerning dogs sparks excitement amongst fanatics alike–Which events draw audiences near although showcasing great skills displayed in the course of competitions these days? https://fast-wiki.win/index.php/The_Importance_of_Hydration_in_Maintaining_Canine_Health
Your site has been a valuable resource during my research into firearms law, especially with clarity from Suppressors & Gun Silencers Online !
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
This was highly informative. Check out same day plumbing services for more.
Nicely detailed. Discover more at quick plumber response .
I appreciate how you provided resources where readers can find additional help regarding their own unique situations!! # # anyKeyWord ## roofing company
Your insights are priceless! Looking forward to the use of Sully’s Pressure Washing by means of Winston-Salem Roof Cleaning .
Seeking rehabilitation post-accident is vital not just for physical recovery but also for mental well-being! georgia injury attorney
Thanks for the great content. More at colchones Albacete .
This was very well put together. Discover more at abogados Coruña .
Thanks for posting this. I found your take on contractor-client communication especially relevant. Being in Humble, TX, this kind of info helps me keep pace with best practices Construction company K Austin & Associates
Wonderful post with practical tips that every beginner should read before traveling! myrtle beach travel agent
I’m impressed with the community engagement you encourage at Stallion Guns . It’s important to foster responsible discussions.
Anyone else think it’s essential to support local businesses, including construction services? google.com
“Looking forward towards supporting this business even more—they deserve recognition within our community over here thanks again ̶” Honest Heating & Air Conditioning Repair
This was a wonderful post. Check out pool installation services for more.
Thanks for the helpful article. More like this at reliable plumbing specialists .
Nicely detailed. Discover more at https://xn—-itbabotjnldew9c3cj.xn--p1ai:443/user/jakleyugaj .
An effective ### anykeyword ### will keep you informed throughout your case—communication is key! car accident legal advice
I liked this article. For additional info, visit https://www.livekavkaz.ru/user/oranceckkz .
I can see why acceptable positioning subjects lots—it could possibly virtually make or holiday your surveillance efforts!! https://wiki-cafe.win/index.php/Step-by_way_of-Step_Guide_to_Installing_and_Positioning_Your_Home_Security_Cameras
It’s essential to have a reliable property management team in Fort Myers. Property Management Companies
Excellent information Many thanks.
Shoutout to mudança em Jundiaí for his or her implausible shifting prone! They absolutely care approximately their buyers.
What’s the best time of year to get Botox treatments? Considering scheduling with botox red bank .
Great knowledge with ### anyKeyWord### all over my latest administrative center relocation—pretty advocate them! mudanças em Jundiaí
The aerial pictures guidance you shared are somewhat necessary! I’m excited to are trying them out. Learn extra at https://www.play-bookmarks.win/to-use-a-drone-digicam-comfortably-leap-through-familiarizing-your-self-with-the-controls-and-settings .
Planning a festival? Don’t forget to check out event hoover portable bathroom rental for your portable toilet needs.
Thanks for the clear breakdown. More info at hvac contractors near me .
Hi! Quick question that’s completely off topic. Do you know how to make
your site mobile friendly? My blog looks weird when viewing from my
iphone 4. I’m trying to find a theme or plugin that might be able to resolve this problem.
If you have any recommendations, please share. Many thanks! http://Tour-Is.Co.kr/bbs/board.php?bo_table=free&wr_id=1259123
Your organizational hacks are lifesavers! They make every part quite a bit more effective and stress-loose, and I’m keen to uncover extra at House Cleaning .
Well done! Find more at toilet plumbers near me .
If you live in Poway and need an honest assessment of your HVAC needs, reach out to the folks at licensed hvac company !
I’m interested in how chiropractic care can improve posture, especially with so much time spent sitting at a desk. Recommendations for Gig Harbor chiropractors? Car accident chiropractor
Excellent strategies uncovered throughout this discussion regarding energy efficiency – owners residing within SD must explore offerings available at ### ## hvac repair service san diego
This was quite useful. For more, visit 24 7 emergency plumber .
I found this very interesting. Check out https://daltonlngc652.theglensecret.com/what-to-do-when-your-check-engine-light-comes-on-in-bonney-lake-12 for more.
I found your comparisons between different weapon types very eye-opening, particularly those featured at Imported Pistols .
Appreciate the thorough insights. For more, visit a plumber .
Quality garage doors make such a difference! I love mine from a local Houma company. American Garage Doors
My dream trip to Machu Picchu is still on my travel bucket list, but I’ll get there one day! myrtle beach travel agency
Appreciate the detailed information. For more, visit best weight loss programs palm desert .
Shoutout to the hardworking crew at Cheap movers Glendale # – you guys rock!
Hearing countless success stories motivates us all pushing boundaries further opening doors leading us towards successful outcomes sought after repeatedly throughout journeys undertaken facilitated primarily through connections established closely between Lotus Health & Aesthetics
Great insights! Discover more at plumbing companies near me .
I adore the way that pilates courses not just help the body, but they also help to maintain cognitive quality and psychological harmony yoga class
Appreciate the detailed information. For more, visit phim sex hay .
Moving day went smoothly thanks to the wonderful team at this Hilliard moving company! For details, visit Cheap movers Fort Liberty !
Renters insurance is often overlooked but super important; protect yourself and your belongings! Rise on McClintock
This was very beneficial. For more, visit trusted blocked toilet specialists .
Thanks for the helpful advice. Discover more at ac tune up near me .
Thanks for the insightful write-up. More like this at General Plumber .
Your post has convinced me that regular carpet maintenance is essential for health as well as aesthetics—thank you! carpet cleaning service near me
Just entire making use of mudança em Jundiaí for my domicile relocation—just right provider all around!
Anyone know how to find licensed contractors who specialize in commercial roofs? https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
Moving can also be nerve-racking, yet with mudanças em Jundiaí , you could possibly have confidence that your belongings are in desirable palms. Highly propose their helpful answers!
Thank you for raising awareness about dryer vent issues! Dryer Exhaust Duct Cleaning offers great services in Seattle.
Looking for ideas on how to make my home more appealing? A chic new design from my favorite garage door company might do the trick! Garage door company
The resources available for understanding firearm accessories are excellent, especially those listed on Guns: Pistols, Rifles, Shotguns & More .
I adore the way that yoga groups promote emotional clarity and emotional equilibrium in addition to improving bodily well-being. It’s amazing to see how a few meetings may alter one’s outlook on life yoga class
Hosted playgroups where more than one domestic dogs romp around freely ensures never-ending laughter emerges traditionally—Do take part quite often inside of identical group occasions hosted within reach?? https://xeon-wiki.win/index.php/Canine_Health_Myths_Debunked:_What_Every_Owner_Should_Know
I was pleasantly surprised by the cleanliness of the portable toilets provided by best porta potty rental company near hoover in Hoover, AL!
This was super helpful. The discussion on documenting medical care struck a chord, especially in cases involving long-term recovery. As someone who lives in Bear, DE, having a clear guide like this is incredibly useful Personal injury attorney
This was quite helpful. For more, visit floor insulation .
This was highly useful. For more, visit Kitchen sink plumbing .
Nicely done! Find more at kitchen and bathroom taps .
Regular repairs is prime to fending off predominant blank-u.s.afterward! Your insights are spot-on; I’m going to examine House Cleaning for ongoing cleansing suggestions.
“Asheville has so much potential; let’s embrace responsible development together!” Best Construction Services in Asheville
This was a wonderful post. Check out custom home builders near me for more.
Pilates has been a game-changer for my pregnancy workouts. So grateful for it! pilates studio near me
Wonderful tips! Discover more at https://qa.laodongzu.com/?qa=user/zardiahbsl .
Well done! Discover more at security guards for hire .
Thanks for the helpful advice. Discover more at hrt near me .
Interested exploring affordable upgrades enhancing overall attractiveness homes prior listings??? Cost-effective approaches highlighted thoroughly through __#anything_# cash for homes michigan
This was a great article. Check out colchones for more.
The tips for new gun owners on firearms accessories for any gun or rifle are incredibly helpful! Great resource for beginners.
“Has anyone faced unexpected costs with their air conditioning repairs? Would love some insight.” Air conditioning contractor
This kind of info is always valuable, especially with how injury lawsuits play out in Annapolis, MD. I didn’t realize how important timing is. Have you noticed any trends in Annapolis courts around these cases? Get more clarity here: Medical malpractice .
Appreciate the comprehensive insights. For more, visit power flushing for radiators .
Thanks for the detailed guidance. More at payday loans new orleans la .
Thanks once again; this turned into such an informative examine that honestly enhances one’s knowledge of sustaining cleanliness exterior!!! # # anyK eyword ## https://camrusxswh.livejournal.com/profile/
Currently it looks like WordPress is the preferred blogging platform available
right now. (from what I’ve read) Is that what you’re using on your blog?
This was quite helpful. For more, visit https://trickpriyo.com/user/golivemsom .
Wow, learning about the impact of climate on roofing choices was eye-opening—definitely something to consider in future projects! More insights at roof replacement .
Your blog inspires me to look deeper into the creative talent we have here in Birmingham for weddings. Ikonic Media wedding photographer birmingham
Well explained. Discover more at expert sink solutions .
“I adore properties that blend modern design with historical charm; finding these unique spaces has been easy thanks to my searches on # # any Keyword # # .” myrtle beach travel agency
This was a wonderful post. Check out ac contractors for more.
Thanks for the informative post. More at affordable commercial plumbers .
The documents approximately climate prerequisites affecting drone overall performance is critical for making plans flights! Thanks for sharing that perception! More main points might be located at https://www.a1bookmarks.win/finally-practice-constantly-to-improve-your-abilities-with-the-two-piloting-and-pictures-systems .
If you’re looking for fast service, you can’t go wrong with one of the many reputable garages here in Houma! American Garage Doors
I’m always inspired by new travel stories. You should check out travel agent laurel for incredible adventures!
This was a great help. Check out local leaking dishwasher specialist for more.
. Consider joining local groups or forums—they often share valuable tips and available rentals! apartments for rent Tempe
Thanks for the practical tips. More at phim sex nhật bản .
“If you’re in need of repairs or replacements, remember that investing in quality pays off big time.” Garage door company New Caney TX
Couldn’t assist yet understand rising popularity surrounding medicine animals proposing emotional aid as neatly–How moneymaking ARE these interactions relating to mental well-being cognizance campaigns in this day and age? https://wiki-planet.win/index.php/Adventures_in_Canine_Agility_Training:_A_Beginner%E2%80%99s_Journey
I found this very interesting. For more, visit https://andresmakc591.lucialpiazzale.com/choosing-the-right-tires-in-bonney-lake-wa-2 .
Dogs bring households jointly in beautiful approaches; how has having a pet inspired kinfolk dynamics in your house? Let’s chat about it on Browse this site .
Recently, I took a yoga school at my neighborhood, and it has transformed both my body and mind. I’ve discovered that the blend of natural engagement and meditation has made me more aware of my breath and presentness in each moment hotworx yoga classes
I always find valuable information at Pistol wholesalers & distributors regarding responsible weapon ownership. Keep it up!
Thanks for the great explanation. More info at venta de colchones .
The FAQs section at Pistol wholesalers & distributors is a great resource for anyone looking to learn more about gun laws.
Appreciate the comprehensive insights. For more, visit Appliance repairs .
I enjoyed this read. For more, visit Power flushing .
Helpful suggestions! For more, visit abogados en A Coruña .
Just moved my industrial with the assist of empresa de mudanças em jundiaí , and I couldn’t be happier with the carrier provided!
Moving doesn’t must be a headache! Contact mudanças em Jundiaí for useful and specialist shifting companies.
The effectivity of mudança em Jundiaí throughout my recent circulation used to be useful! Professionalism at its fine.
If you’re looking for local support groups for dementia, there are great listings at quality elderly care !
Best decision ever was hiring # 1 ! ! . local pressure washing companies Tampa Bay Pressure Washing
This article is very informative! Are there any warranties available for roofs in Montgomery? https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
I fully agree that yoga sessions are a fantastic way to enhance both physical and mental well-being. The feeling of belonging and encouragement you receive in a class can really improve your practice hotworx yoga
The importance of choosing the right color for roofs was an interesting point! Great article overall! roofing contractor
Have you ever participated in a local tradition while traveling abroad? It’s such an enriching experience travel agent myrtle beach
This was quite helpful. For more, visit 24 hour plumber .
Seriously excited about collaborating with quality first builders—everything they touch seems magical when it comes to design! home builder sherman oaks
Thanks for the clear breakdown. More info at http://fh7980px.bget.ru/member.php?action=profile&uid=79122 .
The potential hazards of not knowing where your utilities are located are too high—thank you, Utility Locating , for advocating safety!
I’ve forever been interested in the various puppy breeds! Which breed do you believe is the so much dependable? https://www.bookmark-step.win/dog-bites-enlarge-in-summer-time-months
Helpful suggestions! For more, visit Roof inspection services .
It’s essential to read reviews before renting an apartment; they can provide valuable insights! apartments for rent
This was very beneficial. For more, visit ac tune up near me .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Awesome article! Discover more at https://maps.app.goo.gl/nkd6ZMDAh86t2QLH7 .
The analysis of social media’s influence on public perception of firearms discussed at Arms & Ammunition Dealers was insightful!
This was beautifully organized. Discover more at https://forums.hostperl.com/member.php?action=profile&uid=286571 .
Great insights! Discover more at https://parsesh.ir/user/brittafntx .
I appreciated this article. For more, visit affordable plumbing repair .
I enjoyed this read. For more, visit neurofeedback clinics near Denver .
If you’re feeling warm spots in your home, don’t hesitate to contact an AC repair service in Gilbert! https://www.google.com/maps?cid=12717811348265145193
I’m considering quartz countertops for my remodel—have others had good experiences with them? kitchen remodel contractors Watertown
Looking for helpful transport solutions in your industrial? Look into what empresa de mudanças em jundiaí has to present—wonderful for commercial actions in Jundiaí.
This was beautifully organized. Discover more at Walters BBQ Southern Kitchenac .
For anyone considering Houston vehicle transport, do your research first! It’s worth it! Houston auto transport
Great job! Discover more at https://airvent.kz/user/tiableevvq .
I’ve used a number of transferring products and services before, however none examine to the potency of mudanças em Jundiaí . Great for both residential and commercial necessities!
Thank you ###for making our fresh movement so delicate; in fact browsing ahead to recommending you all around Jundiai! mudança em Jundiaí
I found your article on self-defense laws at Arms & Ammunition Dealers to be very informative and timely!
Appreciate the comprehensive advice. For more, visit reliable plumbers nearby .
Fantastic beat ! I wish to apprentice while you amend your web site, how can i subscribe for a blog web
site? The account helped me a acceptable deal.
I had been tiny bit acquainted of this your broadcast offered bright clear idea
I recently began taking yogi courses, and it has absolutely altered how I view the world. The mix of real activity, mindfulness, and group help is extraordinary hotworx yoga class
I found this very interesting. For more, visit http://www.underworldralinwood.ca/forums/member.php?action=profile&uid=474201 .
This was a great help. Check out plumbing and heating installations for more.
Just wrapped up another meeting with quality first builders—I feel like I’m finally making progress on my dream home! Thanks, guys! new construction homes
Aw, this was a very nice post. Spending some time and actual effort to create a good article…
but what can I say… I procrastinate a lot and
never manage to get anything done.
Appreciate the thorough information. For more, visit LuxNuro .
Great job! Discover more at natural supplements for hormone balance palm desert .
This is highly informative. Check out Walters BBQ Southern Kitchen for more.
Superb blog! Do you have any helpful hints for aspiring
writers? I’m hoping to start my own site soon but I’m a
little lost on everything. Would you suggest starting with a free platform like WordPress or go for a paid option? There are so many choices out there that I’m completely overwhelmed ..
Any ideas? Thank you!
Finding balance between ambition pursuing goals set forth diligently striving achieve success coupled alongside appreciation beauty simplicity found everyday existence reminds us why we embarked journeys initially reminding ourselves purpose behind chosen travel agency laurel
I’ve heard great things about the craftsmanship of construction services in Asheville. Can anyone share experiences? https://www.google.com/maps/place/?q=place_id:ChIJWcJBcYaaxkIRwHALPBFcbsU
I enjoyed this article. Check out Walters Barbecue Southern Kitchen for more.
I can’t believe the amenities some luxury vacation rentals offer! Spa services, private chefs, you name it! Check it out at myrtle beach travel agency .
So true about the risks of mold in homes! After my mold inspections inspection, I feel much more informed and prepared.
This was quite helpful. For more, visit cheap car rental toronto .
Have skilled pleasant surprises from unforeseen acts carried forth by loyal partners demonstrating affection unconditionally all through more than a few situations shared–Can relate personally in opposition to such anecdotes?? https://page-wiki.win/index.php/Creating_an_Effective_Training_Schedule_That_Fits_Your_Lifestyle_42205
Helped me know that having the proper detergent could make each of the difference whilst tackling powerful stains!! # # anyK eyword ## https://arthurztxg421.cavandoragh.org/how-to-start-a-pressure-washing-business-a-step-by-step-plan
Your breakdown of state-by-state regulations at Stallion Guns is a much-needed guide for gun owners.
This was quite enlightening. Check out affordable appliance repairs for more.
I’ve just begun taking yogic groups, and I can’t emphasize enough how revolutionary the practice has been for both my body and mind yoga class
Thanks for the clear breakdown. Find more at Leaking dishwashers .
I’m grateful for the contributions made by various authors featured on your site; they bring unique insights to discussions about guns. Pistol wholesalers & distributors
“Looking forward to transforming my space with new doors! Already have a great idea thanks to recommendations from friends.” https://smart-wiki.win/index.php/The_Role_of_Insulation_in_Energy-Efficient_Garage_Doors
Thanks for the insightful write-up. More like this at Slab leak repair .
This was quite helpful. For more, visit best roofers near me .
Awesome article! Discover more at phim sex hay .
I just adore how canines are such loyal partners! They truly make each and every second unusual. Check out https://blast-wiki.win/index.php/Understanding_the_Different_Types_of_Barks_and_What_They_Mean for some titanic puppy care advice!
I liked this article. For additional info, visit Walters BBQ Southern Kitchen .
Every day presents an opportunity to improve, and pilates always reminds me of that!!!# anyKey word ## Miami Pilates
What’s the best way to choose a Grand Island moving company? I’ve heard great things about Grand Island full service movers .
This was a wonderful post. Check out gutter repair near me for more.
This was a wonderful guide. Check out water heater repair for more.
Thanks for the helpful article. More like this at shower refinishing near me .
“The convenience of having a remote-controlled garage door installed is life-changing!” Garage Door Company in Houma LA
Fantastic post! Discover more at Afordable Pest Solutions .
Great job! Find more at car accident lawyers .
If you’re making plans a transfer in Jundiaí, don’t hesitate to succeed in out to empresa de mudanças em jundiaí —their crew is marvelous!
Thanks for the clear breakdown. More info at non-invasive mommy makeover options .
How do local school districts impact home sales in Michigan? Insights are available at sell your house michigan .
Ground Penetrating Radar (GPR) is revolutionizing the way we explore subsurface structures! Its non-invasive nature allows for detailed analysis without disrupting the surface, making it an invaluable tool in construction, archaeology 811 dig
Just moved my place of business with the aid of mudanças em Jundiaí . Their seasoned staff made the course of seamless and stress-unfastened!
I can’t believe how many amazing places are on my travel bucket list. What’s your top pick? travel agency myrtle beach
Nicely detailed. Discover more at Fort Worth roofing companies .
Your focus on youth education about guns and safety is so necessary, especially through platforms like Bulk Ammunition, Gun Parts, & More! .
This was highly educational. For more, visit Toronto bathtub reglazing .
Hi there! I could have sworn I’ve been to this web site before but after
looking at some of the posts I realized it’s new to me.
Anyways, I’m definitely happy I found it and I’ll be book-marking it and checking
back regularly!
Great insight are provided in this post! It’s crucial to possess trustworthy restoration providers for pcs, game consoles, and phones because we are increasingly reliant on them for both work and leisure Smartphone repair
This was highly educational. More at LuxNeuro .
This post is fantastic for any individual new to drones. The factors are clear and concise! Find further supplies at https://www.tool-bookmarks.win/practice-delicate-and-delicate-maneuvers-even-as-flying-your-drone .
Excellent perspectives into the value of quick fixes for our gadgets! Addressing problems as quickly as possible can save us from bigger issues down the road, whether it’s a computer, gaming system, or telephone Laptop fixing
Couldn’t have asked for better service than what I received from # # a ny keyword # #! shattered phone screen
بک لینک ها چه هستند ؟
بک لینکها لینکهایی
هستند که از یک وبسایت به وبسایت دیگر اشاره میکنند.
این لینکها به عنوان یک تأییدیه از
طرف سایت منبع به سایت مقصد تلقی میشوند و به بهبود رتبهبندی
موتورهای جستجو کمک میکنند.
شما میتوانید این بک لینک هارا به صورت طبیعی در
طولانی مدت با استفاده از لینک های منبع بقیه وب سایت ها به سایت خود بدست
آورید و یا لینک سایت خود را در سایت های دیگه
قرار دهید که به این عمل خرید بک لینک گفته
میشود . به طور کلی، هرچه یک وبسایت بک لینکهای با کیفیت
بیشتری داشته باشد، احتمال بیشتری
دارد که رتبه بالاتری در نتایج جستجوهای گوگل و سایر موتورهای جستجو کسب کند.
. A little patience goes a long way when renting; sometimes, great places pop up unexpectedly! Rise on McClintock
Appreciate the thorough write-up. Find more at inpatient .
This was very enlightening. For more, visit rv repairs near me .
Свежая и проверенная база для эффективного продвижения вашего сайта средствами
Хрумера и ГСА!
Преимущества нашего предложения:
– Качественная база проверенных площадок для мощного SEO-прогона.
– Готовые успешные базы — мгновенный эффект
без риска и разочарований.
-Возможность создать уникальную базу под ваши конкретные критерии.
“Strategic making plans and execution are significant in finance; reap insights from experts thru ###anymKeyWord###.” Outsourced CFO solutions
Appreciate the detailed post. Find more at private event locations .
I’ve discovered that taking a course at my neighborhood has transformed both my pilates exercise and entire well-being. The party atmosphere’s strength really enhances the experience, making it more of a holistic journey than just a workout hotworx yoga
Really enjoyed this piece! It’s perfect timing as we plan our next property renovations. Commercial Roofing in Montgomery IN
I found this very interesting. Check out https://devincmuf946.bearsfanteamshop.com/winter-car-maintenance-checklist-for-buckley-roads-6 for more.
“Moving is never fun—but having great movers like ### any Keyword### makes it manageable.” Jacksonville full service movers
Thanks for highlighting the importance of safety features in garages! Will bring this up with my next visit to the local garage door company. Garage door company New Caney TX
Great job! Find more at home electrical services .
Appreciate the detailed insights. For more, visit Chester pest treatment .
Your analysis of online vs. brick-and-mortar sales at firearms accessories for any gun or rifle provided great clarity on current trends.
Thanks for the valuable article. More at Aesthetic Plastik Surgery and Lazer Center .
بک لینک ها چه هستند ؟
بک لینکها لینکهایی هستند که از یک وبسایت به وبسایت دیگر اشاره میکنند.
این لینکها به عنوان یک تأییدیه از
طرف سایت منبع به سایت مقصد تلقی
میشوند و به بهبود رتبهبندی موتورهای جستجو کمک میکنند.
شما میتوانید این بک لینک هارا به صورت طبیعی در طولانی
مدت با استفاده از لینک های منبع بقیه وب سایت ها به سایت خود بدست آورید و یا لینک سایت خود را در سایت های دیگه قرار دهید که به این عمل خرید بک لینک گفته
میشود . به طور کلی، هرچه یک وبسایت بک لینکهای با کیفیت بیشتری داشته باشد، احتمال
بیشتری دارد که رتبه بالاتری در نتایج جستجوهای گوگل و سایر موتورهای
جستجو کسب کند.
Truly humbled experiencing insightful exchanges revolving around sustainable practices implemented effortlessly throughout meetings occurring alongside Quailty FIrst Buildee recently— home builder sherman oaks
If you’re planning any excavation work, don’t forget to contact an expert like Utility Locating . Their services can save you a lot of trouble down the line.
Excellent write-up How heavily rely on our tech, from cellphones to video games, and how crucial it is to keep them in top shape is wonderful iPhone repair services
Thanks for the detailed guidance. More at Walters Barbecue Southern Kitchen .
I love how you demystified the process of getting a new roof installed; it seems less daunting now!! # # anyKeyWord ## roofing services
I just had a fantastic experience with a neighborhood repair shop that specializes in mobile repairs, laptop repairs, and video sport repairs. It’s amazing how quickly they identified the problem with my computer and fast restored it to normal operation PC repair services
If you want a tender moving adventure, select mudanças em Jundiaí ! Their team is super and is familiar with methods to get the task achieved properly.
Thanks for the great explanation. Find more at professional corporate event spaces .
The history behind traditional clothing in various cultures is so intriguing! Discover more about it at travel agent laurel .
Trust me, hiring mudança em Jundiaí should be among the pleasant selections you make at some stage in your pass.
“Understanding your marketplace situation and coins pass is fundamental to achievement; locate aid as a result of ###anymKeyWord###.” Part-time CFO consulting
I adore how well-trained and skilled instructors are both accommodated in vinyasa sessions. The interaction between the participants really enhances the experience. There is also a sense of support and group in each session hotworx yoga class
Adore how actionable insights provided often lead better decision-making overall during crucial moments needing quick turnaround times when relocating cars! Hats off team 🙌🏽💥:@## Houston auto shippers
I never thought about how preventative maintenance could save money long-term until reading this post! Best Air Conditioning Repair in Gilbert Arizona
Thanks for the practical tips. More at https://maps.app.goo.gl/WJ6d2LBabh5frrSr7 .
I’m curious if anyone has tried open-concept kitchens—how’s the experience been? contractor for kitchen remodel Watertown
Very informative article. For similar content, visit phim sex hay .
The staff at # # anyKey word # # were professional and friendly throughout our entire move! Best Clearwater movers
Hi this is somewhat of off topic but I was wondering if blogs use WYSIWYG editors or if you have to
manually code with HTML. I’m starting a blog soon but have
no coding knowledge so I wanted to get guidance
from someone with experience. Any help would be enormously appreciated!
Your take on international gun laws compared to US laws was fascinating and well-researched, thank you, Buy Suppressors & Gun Silencers Online !
I appreciate the focus on ethical practices within the industry at guns for sale . Integrity matters!
Incredible teamwork by everyone at #Anykeyword made transitioning locations effortless. Macclenny full service movers
“I love how many options we have when it comes to choosing styles and colors for our garages.” Best Garage Door Company in Houma LA
Dogs look drawn towards unique events—they’ll gravitate in the direction of things they take pleasure in so much ! Does YOURS educate certain interests incessantly ? Join discussions wherein we look at preferences found amongst our pups right here ### https://page-wiki.win/index.php/The_Joys_of_Training_Your_Dog_in_Obedience_Classes
I appreciate your suggestions on how to meet locals while traveling! So valuable! myrtle beach travel agent
This was very beneficial. For more, visit https://maps.app.goo.gl/kBCAtUTc6Epwevdp7 .
Appreciate the thorough insights. For more, visit Walters Barbecue Southern Kitchen .
Great job! Discover more at Chester Pest Management .
. Keep an eye on seasonal market trends—they can significantly affect rental prices and availability! apartments for rent Tempe
This was nicely structured. Discover more at Aesthetic Plastik Surgery and Lazer Center .
Appreciate the useful tips. For more, visit inpatient .
This was very enlightening. More at security company .
Clearly presented. Discover more at med spa near me .
Thanks for the useful suggestions. Discover more at home builders near me .
What are the perfect classes programs for good sized breeds like Mastiffs or Great Danes? Help obligatory! https://www.oscarbookmarks.win/dogs-beg-the-question-is-there-instruction-purchasable-for-our
If you’re planning any excavation work, don’t forget to contact an expert like Utility Locating . Their services can save you a lot of trouble down the line.
This was a wonderful post. Check out homes for sale las vegas for more.
This was quite useful. For more, visit LuxNeuro .
Anyone else agree that hiring professionals from a Grand Island moving company saves tons of time? Check out Best Grand Island movers !
The resources for understanding different types of firearms at worlds largest online paintball store are invaluable for enthusiasts.
A nearby repair support for my game console recently gave me an awesome experience. Correctly before a large games championship, it was acting up, and I had no idea where to change PC repair services
This is highly informative. Check out Walters Barbecue Southern Kitchen for more.
Can anyone share their success stories after upgrading their commercial roofs? https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
The contrast among different drone models changed into exceptionally priceless! It helped me settle upon the top one for my necessities. Check out greater at https://www.bookmarking-online.win/always-comply-with-regional-regulations-and-pointers-whilst-flying-your-drone-digital-camera .
“The insights won from specialist CFOs are helpful; gain knowledge of more at Virtual CFO services !”
Thanks for the valuable insights. More at pest management services Chester .
This was very beneficial. For more, visit Aesthetic Plastik Surgery and Lazer Center .
Pretty great post. I just stumbled upon your weblog and wished
to mention that I’ve truly enjoyed browsing your blog posts.
After all I’ll be subscribing on your rss feed and I’m hoping you write once more very soon!
I adore the advantages of taking vinyasa courses! They not just help with natural mobility, but they also give you a great possibility to unwind and be mindful. It’s remarkable how a regular activity may affect your mood hotworx yoga classes
Have you ever participated in a canine educate or occasion? It sounds so enjoyable! Learn more about local hobbies at https://wiki-square.win/index.php/Exploring_the_Benefits_of_Raw_Diets_for_Dogs .
The diversity of perspectives showcased in your articles makes for an enriching experience when visiting Buy Suppressors & Gun Silencers Online .
I love how a new garage door can transform the look of a home. Time to find a reputable garage door company! Garage door company New Caney TX
Thanks for the detailed post. Find more at car rental toronto .
Appreciate the detailed information. For more, visit medical weight loss clinic .
There are such a lot of myths about puppies available! What misconceptions have you ever heard? Let’s debunk them collectively at https://wool-wiki.win/index.php/Why_Regular_Exercise_is_Crucial_for_Your_Dog%E2%80%99s_Health !
Always ask about lease agreements thoroughly; understanding each clause will benefit you! Rise on McClintock
Great post! Mold inspection is so crucial for maintaining a healthy home environment. I recently had a mold inspections inspection done, and it made a huge difference!
Useful advice! For more, visit Buckley auto repair .
Just tried a reformer Pilates class for the first time, and I’m hooked! pilates studio near me
มีวิธีตรวจสอบคุณภาพของไฟหน้ารถ LED อย่างไรบ้าง? เปลี่ยน ไฟหน้ารถ ใกล้ ฉัน
Utility locating can save time and money in the long run! Highly recommend reaching out to 811 dig if you’re starting a project.
I appreciated this post. Check out professional neurofeedback specialists Denver for more.
This was a great help. Check out Walters BBQ Southern Kitchen for more.
If you’re trying to save money on your move, consider using Best Clearwater movers for cheap rates.
สาวกขับรถกลางคืนต้องไม่พลาดกับไฟหน้ารถ LED BT PREMIUM นะครับ #BT_PREMIUM## ร้านไฟรถยนต์ ใกล้ฉัน
This was very enlightening. For more, visit affordable event spaces .
My entertainment console recently had a great experience with a local repair service. I made the irritating decision to seek help after a few annoying weeks of dealing with continuous crashes Laptop fixing
Thanks for the insightful write-up. More like this at DSH Homes and Pools .
I love how many quality air conditioning services we have here in Gilbert! It makes keeping cool so much easier. Air Conditioning Repair in Gilbert Arizona
Every company proprietor could agree with CFO prone for stronger economic management. Part-time CFO consulting has fine innovations!
Wonderful suggestions shared in this post—check out additional content available at: travel agent laurel
I’ve been taking yoga lessons for a few decades, and I can’t even begin to convey how transformative the experience has been! My freedom has improved, and I’ve even noticed a considerable drop in stress levels hotworx yoga class
fantastic points altogether, you just won a new reader.
What could you suggest about your put up that you just made some days
ago? Any sure?
Grateful existence places dedicated uplifting spirits while nurturing physical appearances bolstering confidence levels dramatically impacting lives positively overall journey undertaken toward achieving desired transformations ultimately leading authoritative coolsculpting
Don’t let high prices hold you back from achieving your dream body. Explore the affordable CoolSculpting deals at accredited coolsculpting services and make your transformation a reality.
Thanks again team for helping me feel comfortable during laser hair removal—it truly changed how confident I feel when wearing shorts again!!# # anyKeyWord # # trusted coolsculpting
Very informative! I think everyone should consider a mold inspection, especially if they live in humid areas. My experience with mold inspections near me was eye-opening.
Anyone comprehend if there are selected brands everyday extraordinarily effectively among mavens as opposed to casual customers?? # # anyK eyword ## https://writeablog.net/rauteriyjx/10-essential-accessories-every-pressure-washer-owner-needs
Looking into downsizing options post-sale?? Resources connecting sellers with suitable housing solutions provided via _##anything_# sell your house fast for cash michigan
The analysis of social media’s influence on public perception of firearms discussed at Arms & Ammunition Dealers was insightful!
Loving all these innovative storage solutions being shared for small kitchens—it makes everything functional yet stylish as well! kitchen cabinet renovation Watertown
Thanks for sharing this; it helps demystify the process of hiring contractors locally! google.com
Thanks for the insightful write-up. More like this at phim sex .
Well done! Find more at Aesthetic Plastik Surgery and Lazer Center .
Thanks for the insightful write-up. More like this at Affordable Pest Solutions .
This was nicely structured. Discover more at liên kết tải vua99 .
Appreciate the great suggestions. For more, visit local toilet repair .
“Repaired by an expert team—couldn’t believe how quick and smooth everything went!” Best Garage door company in New Caney TX
CoolSculpting treatment is a game-changer for those struggling with stubborn fat. Visit authoritative coolsculpting and start your transformation journey today!
Great ideas on cleaning concrete sidewalks! I not ever knew how positive a stress washer can be. I’ll most likely do that out. Additional resources
Honestly could rave endlessly about how transformative experiences have been thus far reaping rewards gained through consistent efforts made alongside professionals working here 💪✨ #AmericanLaserMedSpa-Midland# reputable coolsculpting
The benefits surrounding **coolsculpt treatment options** are indeed endless!! Who wouldn’t want this?? # # anyKeyWord # top-rated coolsculpting provider
Appreciate the detailed information. For more, visit https://cineblog01.rest/user/rondocpqnc .
You covered some key points. The discussion on documenting medical care was a good reminder, especially after a slip-and-fall or car crash. As someone who lives in Bear, DE, having a clear guide like this is incredibly useful Personal injury attorney The Sharma Law Firm
“I can’t wait to dive into another summer filled with joy—I’ll definitely be exploring more waterslide rentals here!” # # anyKeword #” bounce house clearwater
Thanks for the informative post. More at reliable plumbing solutions .
I love that you mentioned bringing a beach blanket! It makes such a difference for comfort. myrtle beach travel agency
. Just signed my lease and am already dreaming about how I’ll decorate each room in my new space! Rise on McClintock
Anyone thinking of starting a DIY project should definitely consider hiring professionals like Underground utility locating services to locate utilities first!
This was quite helpful. For more, visit http://www.bonjourdewi.com/bb/member.php?action=profile&uid=353980 .
Do you believe you studied it can be quintessential to put money into luxurious units if simplest used once in a while—or will mid-vary suffice??? # # anyK eyword ## https://wiki-global.win/index.php/How_To_Choose_the_Right_Cleaning_Solution_For_Your_Surface_Type
It’s a shame you don’t have a donate button! I’d most
certainly donate to this excellent blog!
I guess for now i’ll settle for bookmarking and
adding your RSS feed to my Google account.
I look forward to new updates and will share this blog with my Facebook group.
Chat soon! http://Themodernbusinessschool.com/__media__/js/netsoltrademark.php?d=dtyzwmw.com%2Fcomment%2Fhtml%2F%3F111870.html
Fantastic post! Discover more at expert neurofeedback services in Denver .
Appreciate the thorough write-up. Find more at front door replacement .
สีของแสงไฟหน้ารถ LED BT PREMIUM สวยงามมากครับ ไฟหน้ารถยนต์
Roofing projects often generate significant debris. Renting a dumpster from dumpster rental orlando with proven results in Orlando will streamline the clean-up process.
Excellent perspectives into the value of regular repair for our tools! It’s so simple to overlook minor problems before they escalate to key issues Android phone restoration
Being ableto customize spice levels suits both adventurous eatersand those who prefer milder flavors perfectly. indian buffet in spokane valley
Just had my roof replaced by a fantastic company in Carlsbad! They did an amazing job. Visit expert roof replacement for more info.
Appreciate your stance on promoting responsible ownership and usage of firearms at Sports Air Guns, Airgun manufacturers, suppliers & exporters .
Great blog here! Also your site loads up fast!
What web host are you using? Can I get your affiliate link to your host?
I wish my site loaded up as quickly as yours lol
This was nicely structured. Discover more at professional corporate event spaces .
This was a great help. Check out local plumber pricing for more.
This was a great article. Check out http://fh7980px.bget.ru/member.php?action=profile&uid=79124 for more.
Thanks for the comprehensive read. Find more at https://sonnik.nalench.com/user/cillenncdc .
“It’s always nice to support small businesses like those providing quality service for our garages!” google.com
Appreciate the useful tips. For more, visit hormone replacement therapy .
“Choosing the precise economic associate is significant; discover concepts at Chief financial officer services .”
This thought-provoking write-up about the importance of choosing the best childcare for your children recently struck me. Finding a setting that promotes both learning and social creation is essential daycare near me
This was nicely structured. Discover more at Aesthetic Plastic Sugery & Lasor Center .
การเลือกซื้อไฟหน้ารถ LED ควรพิจารณาอะไรบ้าง ?? #BT_PREMIUM## ร้านซ่อม ไฟรถยนต์ ใกล้ฉัน
I adore your explanations of the advantages of vinyasa lessons! It’s incredible how they can improve both physical and mental well-being. Finding the right course is crucial for everyone looking to strengthen their practice or begin afresh hotworx yoga
This was a fantastic read. Check out ev charger installation greensboro nc for more.
The cost per outlet is something many homeowners overlook. Your breakdown helps clarify what to budget for when hiring electricians near me. electrical companies near me
I completely agree that regular mold inspections can save lives and property. My experience with mold inspections near me was very thorough!
This was a great article. Check out https://duvidas.construfy.com.br/user/aubinaktdm for more.
This was highly useful. For more, visit LuxeNeuro .
I just discovered that underground utility locating can prevent expensive repairs later on. Kudos to Utility Locating for spreading the word!
Thanks for the great explanation. More info at Walters BBQ Southern Kitchen .
Thanks for the great information. More at https://hammerfjord.com/member.php?action=profile&uid=44754 .
I just had a positive experience having my phone repaired, which made me consider how crucial it is to have trustworthy repair service for our products iPhone repair services
Appreciate the thorough information. For more, visit Walters BBQ Southern Kitchenac .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
CoolSculpting is a revolutionary treatment that can help you achieve the arms of your dreams. Discover how at dependable coolsculpting .
I liked this article. For additional info, visit phim sex nhật bản .
Excellent article! How frequently do we concentrate on our devices for daily tasks, games, and communication is amazing. One of them you seriously sabotage our lifestyles when it breaks downward Desktop computer repair
ใครมีเทคนิคในการดูแลรักษาไฟหน้ารถ LED แชร์หน่อยครับ! ไฟแต่งรถยนต์
I’ve learned that being flexible with move-in dates can open up more rental opportunities—try it! Rise on McClintock
I recently visited American Laser Med Spa in El Paso, and the experience was fantastic! Highly recommend! high-quality coolsculpting treatments
Looking for a trusted Coolsculpting provider in Midland? Look no further than expert-driven coolsculpting therapy . They have a great track record.
This thought-provoking post about the value of quality daycare for early youth advancement just struck me. How much of an effect may a nurturing environment have on children’s social and learning abilities is exciting daycare in parsippany
This was a great article. Check out drainage plumbers near me for more.
มีใครอยากแชร์รูปไฟหน้ารถ LED ของตัวเองบ้าง? ไฟรถยนต์
Nicely done! Find more at dishwasher appliance repairs .
I love that you’re focusing on local issues like commercial roofing—thank you! Best Commercial Roofing in Montgomery IN
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at Authorized and Licensed firearms and Air Guns Dealers !
Every bite taken represents culmination efforts put forth striving excellence achieving highest st indian buffet in spokane valley
Great job! Discover more at blocked drain plumber .
My recent home renovation in Asheville was a breeze thanks to professional construction services! https://www.google.com/maps/place/?q=place_id:ChIJWcJBcYaaxkIRwHALPBFcbsU
Very helpful read. For similar content, visit tải vua99 miễn phí .
Say goodbye to unwanted fat with the help of CoolSculpting! Visit accredited coolsculpting services to learn about its incredible benefits and take the first step towards a new you.
I appreciate this insight on mold inspections. It’s amazing how much hidden mold can affect our health. I trust mold inspections for thorough inspections!
This was very insightful. Check out Pittsburgh Weekend Brunch for more.
Feeling refreshed after each session reminds me importance investing quality time into self-care routines regularly!! #InvestInYourselfForLongTermBenefits!! Anykeyword### accredited coolsculpting services
This was quite helpful. For more, visit Aesthetic Plastic Sugery & Lasor Center .
Great tips on maintaining garage doors! I’ll definitely be calling my local garage door company for a check-up soon. Garage door company
Useful advice! For more, visit my plumber .
Thanks for the helpful advice. Discover more at interior painting .
Thanks for the helpful article. More like this at roofers .
This was highly useful. For more, visit 24 hour plumbing service .
This was very well put together. Discover more at medical spa near me .
This was highly educational. For more, visit air conditioning companies .
Love that you just’re educating home owners approximately their roofs—it’s so very important and regularly overlooked—looking out ahead to contacting %%anyKeyword%%! Softwash Roof Cleaning
Just got my vehicle tinted at Clear View Glass and Tint, couldn’t be happier with how it turned out—definitely worth it! auto tint near me
This really clarified a few things for me. Your point about budget management really resonated. Being in Dallas County, Texas, I know firsthand how crucial those processes are Construction company
Great post! Keeping our homes cool is a priority with Gilbert’s extreme temperatures. https://www.google.com/maps?cid=12717811348265145193
Do you have any video of that? I’d like to
find out some additional information. https://gemini.envs.net/x/dragon-slave.org/comics/NoemiljPikeys
I found out the tough method how important it is to have legal support after a car crash. If you remain in Irvine, don’t think twice to reach out to a certified attorney through Car accident lawyer near me .
Do you have any video of that? I’d like to find out some additional information. https://gemini.envs.net/x/dragon-slave.org/comics/NoemiljPikeys
Nicely done! Find more at LuxeNeuro .
This was highly educational. More at roofing companies Springboro OH .
It’s amazing how much technology has improved utility locating services! Thanks for leading the way, 811 dig .
Just got a quote from a local garage door specialist — very reasonable prices for such quality work! Garage Door Company in Houma LA
Great tips on preventing mold! It’s always best to be proactive with a mold inspections near me inspection rather than reactive.
This is my first time go to see at here and i am
genuinely impressed to read everthing at one place.
Appreciate the comprehensive insights. For more, visit Preferred Reglazing .
This was a fantastic resource. Check out shower refinishing near me for more.
Great job! Discover more at Body Symmetry MD in Palm Desert .
Thanks for the thorough article. Find more at private space for celebrations .
Awesome article! Discover more at https://beaujmqc939.almoheet-travel.com/choosing-the-right-tires-in-bonney-lake-wa-19 .
Useful advice! For more, visit https://echo-wiki.win/index.php/Free_Casino_Play_Could_Be_Beneficial_For_Many_Reasons .
Thanks for highlighting eco-friendly options for beachgoers! We should all do our part to keep beaches clean. myrtle beach travel agency
Well done! Find more at emergency plumbing prices .
Great job! Find more at roofing contractors near me .
The diversity of perspectives showcased in your articles makes for an enriching experience when visiting Arms & Ammunition Dealers .
Very informative article. For similar content, visit Burst pipes .
. Just realized how beneficial having roommates can be regarding both savings and companionship while renting. Rise on McClintock apartments for rent
Great job! Find more at quick emergency plumbing help .
I enjoyed this read. For more, visit Aesthetic Plastic Sugery & Lasor Center .
The beauty behind renovation stories lies within personal narratives woven together through each choice made along that transformative path…!! ### anyKeyWord ## kitchen renovation costs Watertown
This was quite informative. For more, visit Chester Rodent Control .
If you’re associated with an automobile mishap in Irvine, it’s essential to have the right legal representation. A proficient Car accident lawyer near me can help you browse the intricacies of your case.
“Every small company must always keep in mind hiring a pro CFO; discover recommendations at Chief financial officer services .”
การใช้ไฟหน้ารถ LED ในฝนตก เป็นยังไงบ้าง? ร้านหลอดไฟรถยนต์ ใกล้ฉัน
Appreciate the thorough insights. For more, visit Kitchen remodeler contractor .
Thanks for the insightful write-up. More like this at window replacement near me .
Do your research on clinics; there are some really reliable options for CoolSculpting available in Lubbock now! reputable coolsculpting
I’m really excited about starting my journey with CoolSculpting at American Laser Med Spa! ethical coolsculpting
ไฟหน้ารถ LED กับการขับขี่กลางคืน เป็นยังไงบ้างครับ? เปลี่ยน ไฟ หน้า รถ ราคา
Looking for personalized coolsculpting treatments in Midland? Trust the experts at credible coolsculpting treatments to help you achieve your desired body shape.
Appreciate the thorough write-up. Find more at https://www.toro-bookmarks.win/indicators-your-pipes-demands-immediate-interest .
I found this very interesting. Check out Walters Barbecue Southern Kitchen for more.
Führerschein kaufen. Wir bieten absolut alle Führerscheinklassen in Deutschland an, von Klasse A Zweirädern bis Klasse D Unterklassen für Pkw, inklusive Unterklassen B und C für Pkw und Lkw. Weitere Informationen zu den Führerscheinklassen finden Sie unter Führerschein kaufen
https://www.drivingpermits.de/fuhrerschein-kaufen/
Excavation safety should never be overlooked! Always consult with experts like Utility Locating before starting any project.
Führerschein kaufen. Wir bieten absolut alle Führerscheinklassen in Deutschland an, von Klasse A Zweirädern bis Klasse D Unterklassen für Pkw, inklusive Unterklassen B und C für Pkw und Lkw. Weitere Informationen zu den Führerscheinklassen finden Sie unter Führerschein kaufen
https://www.drivingpermits.de/registrierten-fuhrerschein-kaufen/
อยากรู้ว่าไฟหน้ารถ LED ใช้งานได้นานแค่ไหน? ร้านเปลี่ยนหลอดไฟรถยนต์ ใกล้ฉัน
Thanks for the helpful article. More like this at https://www.golf-bookmarks.win/the-advantages-of-a-water-pressure-regulatory-authority-and-heating-timer .
Does anyone know if there are special regulations impacting electric cars being shipped via HOUSTON’s carriers??? Would love clarity here!!!# # anyKeyWord# #” Vehicle Quick Transport’s Houston
If you’re looking for the best auto tint near me in Phoenix, Clear View Glass and Tint is the place to go! auto tint near me
Helpful suggestions! For more, visit find event spaces .
This is very insightful. Check out Corgi plumbers for more.
Excellent advice on how to pick the right style of garage doors! I’ll be discussing options with my local garage door company soon. Garage door company
Are there specific signs that indicate my AC is low on freon, and what should I look for? hvac contractor near me Home page
Thanks for the thorough analysis. Find more at https://parsesh.ir/user/tyrelaxpsc .
Appreciate you posting this, especially on what steps to take immediately after a crash. Locals often underestimate the need for medical follow-up Personal injury attorney
“It’s good to know that inspections can prevent costly repairs down the line.” Commercial Roofing in Montgomery IN
I found the information on flat roofs versus pitched roofs really enlightening! roof repair
Want to get rid of those love handles once and for all? CoolSculpting can help you achieve a more defined waistline. Visit trusted coolsculpting for exceptional results.
Every bite transported me straight back home—thankful for places like this reminding us where we came from . indian buffet in spokane valley
The spicy tuna roll at Ginger Bistro is a must-try if you’re looking for some of the best sushi around St Augustine! Sushi
“I adore properties that blend modern design with historical charm; finding these unique spaces has been easy thanks to my searches on # # any Keyword # # .” myrtle beach travel agency
For those who haven’t yet visited, trust me, you need to check out what American Laser Med Spa offers—you won’t regret it! dependable coolsculpting
This was highly useful. For more, visit phim hiếp dâm .
. Don’t underestimate taking time off work specifically dedicated solely toward viewing potential rentals. apartments for rent
Wow, wonderful weblog layout! How lengthy have you ever been blogging for?
you make blogging look easy. The entire look of your website is wonderful, let alone the content
material! http://dtyzwmw.com/comment/html/?137080.html
“Thanks again to # anykeyword#—they went above and beyond during my move!” Dade City moving companies
I think this is one of the most important information for me.
And i’m glad reading your article. But want to remark on few general things, The website style is ideal,
the articles iss really great : D. Good job,
cheers
My website – Mersin boşanma avukatı
This was a great article. Check out 24 7 plumber in my area for more.
Thanks for the helpful advice. Discover more at delicious brunch in Pittsburgh .
This was quite informative. For more, visit quick blocked drain help .
I’m curious to find out what blog system you are utilizing?
I’m having some small security issues with my latest website and I would like
to find something more secure. Do you have any suggestions?
Such an important topic! I had no idea that mold could pose such risks until I got my mold inspections inspection last year. Highly recommend it!
This was quite informative. For more, visit https://trickpriyo.com/user/fraziggype .
پروتئین وی کینگ رونی کلمن، یک پروتئین وی با کیفیت بالا و ترکیبی از وی ایزوله، هیدرولیزه و کنسانتره است که در هر پیمانه ۳۵ گرم پروتئین، تنها ۱.۵ گرم چربی و ۴ گرم کربوهیدرات دارد.
Fantastic post! It’s so essential to have legal representation if you get into a mishap in Irvine. I discovered my attorney through Car accident lawyer near me , and they were wonderful!
Strongly agree that clear communication between contractors and clients leads toward successful outcomes every time!!! # # anykeyword ## accredited roof repair
Speaking c crash lawyer
Your breakdown of state-by-state regulations at Sports Air Guns, Airgun manufacturers, suppliers & exporters is a much-needed guide for gun owners.
If you haven’t tried their dim sum yet, you’re missing out on one of the best experiences at Ginger Bistro! chinese restaurant
The last time I rented a dumpster, I used info from strategic waste management orlando #—it made choosing so much simpler.
Loved the detail you shared. The section on documenting the accident scene is something many overlook. Being from New Castle County, DE, I know how time-sensitive local legal steps can be car accident lawyer
This was a wonderful guide. Check out investing in a mommy makeover for more.
This was quite helpful. For more, visit power washing near me .
Grateful there’s awareness being raised around common issues faced locally concerning cooling/heating appliances alike … https://www.google.com/maps?cid=12717811348265145193
This was quite helpful. For more, visit local checkatrade plumbers .
Nicely done! Find more at plumbing companies near me .
A knowledgeable motorcycle accident legal representation can help you understand your rights following an accident.
Did you understand that having a vehicle accident lawyer can significantly increase your chances of getting reasonable payment? If you’re in Irvine, think about reaching out to a specialist through Car accident lawyer near me .
Appreciate the detailed information. For more, visit LuxeNeuro .
I love assisting nearby companies like Sully’s Pressure Washing for home features like window cleansing! Window Washing
If you want peace of mind while digging, make sure you hire experts like 811 dig to locate utilities first.
Looking for a great sushi place? Check out Ginger Bistro in St Augustine; their menu is extensive and everything is delicious! Sushi near me
“Do you have tips on how to manage timelines effectively during a build?” google.com
This was a great help. Check out https://maps.app.goo.gl/Ji1s7tRz7BmxPGyN7 for more.
Thanks for raising awareness about mold inspections! I just scheduled mine with mold inspections near me and feel much more secure in my home now.
Thanks for the informative content. More at Walters Barbecue Southern Kitchen .
สนใจจะเปลี่ยนเป็นระบบไฟหน้าใหม่ ต้องดูตรงไหนบ้าง?? ร้านทําไฟรถยนต์ ใกล้ฉัน
Looking for reliable plumbers? Visit affordable plumbing service ; they’ve got a solid list of vetted Coquitlam plumbing contractors.
Thanks for the great tips. Discover more at https://maps.app.goo.gl/mDei2j1BsjTSYTUt8 .
Say goodbye to unwanted fat and hello to a more sculpted body with CoolSculpting! Discover its benefits at skilled coolsculpting technicians and start your journey today.
This was very enlightening. For more, visit 24 hour plumbing service .
I adore the way that yoga sessions promote both physical and mental well-being! The right balance can be achieved by combining breathing power, meditation, and postures yoga
If you’re facing frequent leaks, it might be time to consult with a professional ##Vancouver plumber## about your options. Vancouver water heater service providers
Laser hair removal at endorsed coolsculpting sounds like a game changer for summer!
Valuable information! Discover more at Affordible Pest Solutions .
This was quite useful. For more, visit Aestheic Plastic Surgery & Laser Centre .
This was highly useful. For more, visit https://maps.app.goo.gl/4gr3NGcn7rq6QD6C7 .
I appreciated this article. For more, visit https://maps.app.goo.gl/1QGL6DfX2X9AwhZt9 .
This was highly useful. For more, visit https://maps.app.goo.gl/2X2LyMcW2JdzrpEC8 .
Is there a specific time of year that’s best for certain treatments offered by AmericaLaserMedSpa –Midland, like skin rejuvenation or hair removal? dependable coolsculpting
This was a fantastic read. Check out gas fitters for more.
Do pals/kin more often than not ask “What breed matches MY standard of living leading?” ;Have ideas geared up after discovering very well ahead of advising doable destiny proprietors? https://mill-wiki.win/index.php/Canine_Communication:_How_Dogs_Talk_to_Us_and_Each_Other
This was a fantastic resource. Check out drain cleaning plumber for more.
The creativity involved in making new combinations of moves keeps me engaged!! pilates studio
Learning completely different command cues enables seamless conversation among folks/pets alike –What instructions efficient taught YOUR Furry Friends at some point of experiences shared between others? https://xeon-wiki.win/index.php/Signs_That_Your_Dog_is_Unhappy_and_How_to_Help
Very useful post. For similar content, visit Bathtub resurfacing near me .
Clear steps outlined regarding packing efficiently made all pertinent details easy-to-follow throughout reading experience thanks greatly—they’re super helpful indeed please don’t neglect visiting back again over @ %% myrtle beach travel agent
Just finished renovations and couldn’t be happier with my choice of ##plumbing services in Kelowna#. best Kelowna plumber
Excellent article! It’s amazing how quickly tech can become so important in our routine lives, and breaking something can be a real pain Android phone restoration
I enjoyed this read. For more, visit Walters BBQ Southern Kitchen .
Looking for a cozy place to call home? Check out the amazing options available! apartments for rent Tempe
Thanks for the thorough analysis. Find more at https://maps.app.goo.gl/yRCHncB6jXQiiKz39 .
Excellent insight into the importance of keeping our tools up! Regular checkups can enhance a computer’s longevity and increase functionality, whether it’s a game console, phone, or other device Desktop computer repair
Educating people about underground utilities is so important; thank you, anyKeyWord]# # ,for being at the forefront of this movement! Utility Locating
Shoutout to the amazing team at for their excellent service in Houma! google.com
Thanks for the helpful article. More like this at Walters BBQ Southern Kitchenac .
Great reminder that having a strong North Carolina accident attorney can make or break your case.
Such an incredible journey so far—thank you, #2 , for making this experience enjoyable and effective skilled coolsculpting technicians
เรื่องเสียงเวลาขับรถด้วยไฟหน้า LED เป็นอย่างไรบ้าง ? #BT_PREMIUM## ไฟหน้า led
Great insights! Find more at plumbers near me prices .
Appreciate the detailed insights. For more, visit my local plumber .
It’s vital to understand your rights after an accident. Hiring a knowledgeable car accident lawyer in Irvine might be the very best choice you make. Explore alternatives at Car accident lawyer near me !
Thanks for the helpful article. More like this at plumbing contractors near me .
Just started a new skincare regimen recommended by the experts at American Laser Med Spa—excited to see results! competent coolsculpting procedures
I recently began taking yoga classes, and it has transformed both my body and mind. A unique environment for personal development is created by the blending of physical postures, breathing control, and meditation hotworx yoga class
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic CO
This is precisely what I essential! I’m going to persist with your regulations for my new abode defense manner. https://shed-wiki.win/index.php/**How_High_Should_You_Mount_Your_Security_Camera%3F_Expert_Insights**
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch and coffee near me
ผมใช้ไฟหน้ารถ LED มา 6 เดือนแล้ว สุดยอดจริงๆ เปลี่ยนหลอดไฟรถยนต์ ใกล้ฉัน
Thanks for the comprehensive read. Find more at Drainage & waste pipe .
Great dialogue on the ethics of drone images and respecting privateness rights! A must-examine for all drone enthusiasts! More insights at https://www.bokkmarking-signs.win/always-follow-local-rules-and-checklist-whilst-flying-your-drone-camera .
It’s necessary to understand your rights after an accident. Employing an experienced automobile accident attorney in Irvine might be the best choice you make. Explore alternatives at Car accident lawyer near me !
ข้อเสียของการใช้ไฟหน้ารถ LED คืออะไร? ร้าน เปลี่ยน ไฟ หน้า รถยนต์ ใกล้ ฉัน
I can’t recommend A+ Gutters enough! They did an amazing job on my home’s gutters in Jacksonville. gutters near me
If you’re located near Jacksonville and need pool screen repairs, look no further than A+ Gutters! lanai screen repair near me
Nicely detailed. Discover more at water heater repair near me .
This is such an eye-opener! Many don’t realize how harmful mold can be until they get a proper mold inspections near me inspection done.
The emphasis placed upon flexibility while traveling is essential; loved your take on that—thank you; there’s even more guidance available at %%ANYKEYWORD%%! myrtle beach travel agent
Craving sushi? Make sure to stop by Ginger Bistro in St. Augustine – it’s a hidden gem for sure! Sushi
Your blog is incredibly insightful about HVAC systems! I’ll definitely look into finding a reliable hvac repair san diego in San Diego.
The process of finding an apartment can be overwhelming, but it’s also exciting! Rise on McClintock
Thanks for the thorough article. Find more at Chester commercial extermination .
This was quite helpful. For more, visit Aestheic Plastic Surgery & Laser Centre .
The reviews for different Grand Island moving companies were really helpful in making my decision! Long distance movers Grand Island
I appreciate the information on commercial roofing warranties. Very helpful! https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
My recent experience with an Asheville builder was nothing short of fantastic—professional and timely. google.com
As globalization continues shaping our world increasing awareness cultures inspires curiosity leading us closer together celebrating uniqueness thriving harmoniously across borders documented keenly throughout narratives accessible right away linked indian restaurant spokane valley
Great work on this article. The section on timeline management was spot-on. Around Dallas County, Texas, those practices are essential for smooth builds Construction company
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Massage therapy for wellness in Aurora
I’m blown away by the difference in these CoolSculpting before and after pictures. It’s incredible how this treatment can transform your body! skilled coolsculpting technicians
Thanks for the practical tips. More at trusted heating installation .
ราคาของไฟหน้ารถ LED BT PREMIUM คุ้มค่ามากจริงๆ ครับ ร้าน ทํา ไฟ หน้า รถยนต์ ใกล้ ฉัน
Knowledgeable advocates provide resources needed empowering those affected regain control life again despite hardships endured previously!!!##### lawyer
We are looking for a lot of data on this item. In the meantime, this is the perfect article I was looking for . Please post a lot about items related and I am waiting for your article. And when you are having difficulty writing articles, I think you can get a lot of help by visiting my .
I recently had a sluggish computer and a game console that simply haven’t turn on, all of which caused me to experience various issues with my devices phone repair services
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Family-friendly brunch in Pittsburgh
Excellent article! How frequently do we get our devices for granted before they fail, is remarkable. Reliable maintenance services are necessary whether it’s a system acting slowly, a game system that won’t boot up, or a telephone with a dented screen Computer repair
This was very enlightening. For more, visit https://www.bright-bookmarks.win/the-advantages-of-hiring-qualified-pipes-and-home-heating-specialists .
– Thinking about trying underarm laser hair removal—has anyone done this with #ANYKEYWORD#? reputable coolsculpting
I love how you demystified the process of getting a new roof installed; it seems less daunting now!! # # anyKeyWord ## roofing contractor
I liked this article. For additional info, visit https://www.foodtrader.nl/user/profile/89364 .
Underground utility locating is such a crucial service for construction projects. It’s great to see companies like Underground utility locating services making it easier for builders to avoid costly mistakes!
Wonderful tips! Find more at Walter’s BBQ Southern Kitchen .
Keep this going please, great job!
This blog is incredibly helpful! I’m now convinced of the importance of scheduling regular mold inspections with mold inspections to ensure a safe living environment.
I’ve been taking yoga classes for a few months, and the results have been incredible! My agility has improved as well, and my anxiety levels have decreased considerably. I adore how each program feels like a mini-daily break hotworx yoga
It’s essential to maintain realistic expectations when considering CoolSculpting, as individual results and potential side effects can vary. endorsed coolsculpting
Gilbert’s heat is no joke! I’m glad I found a great AC repair service nearby. Everest Air LLC
Thanks for the great information. More at total mommy makeover experience .
Did you know that most car accidents happen within five miles from home? Stay vigilant and learn more at car accident claims !
I found an excellent garage door company in Houma that did a quick and affordable job! Best Garage Door Company in Houma LA
I found this very helpful. For additional info, visit professional plumber in my area .
This was very insightful. Check out Plumbers near me for more.
This was a great help. Check out Leaking toilets for more.
Does insurance cover any part of the cost for CoolSculpting at American Laser Med Spa? That would be helpful to know! skilled coolsculpting technicians
St Johns County residents should definitely check out A+ Gutters for their patio screen needs! pool screen repair
The variety of options at Ginger Bistro makes it my favorite spot for sushi in St. Augustine and Palm Coast! Sushi
I’ve always found that it’s important to have a trustworthy repair shop for my gadgets Android phone restoration
I recently had a great practice with a local t repair business that specializes in anything from phone repairs to computer repairs PC repair services
อยากรู้ว่าไฟหน้ารถ LED ใช้งานได้นานแค่ไหน? bt premium auto xenon รามอินทรา
I found this very interesting. Check out Walter’s BBQ Southern Kitchen for more.
Did all and sundry say “Doggy spa day”? Treats like paw-dicures & massages sound heavenly ; Who else indulges their fur toddlers in some cases like this too ? https://romeo-wiki.win/index.php/Socializing_Puppies:_The_Key_to_a_Well-Adjusted_Adult_Dog
If you want efficient service without breaking the bank on your AC repairs, definitely choose Summit Services in Bluffton! Worth every penny; learn more at hvac service near me .
This article discusses the benefits of hiring a roofing contractor who specializes in green roof maintenance certified roof installation
“So many knowledgeable professionals here; I’m impressed by their expertise!” north park dentist
How does it work if someone wants to make payments on their bond? That’s definitely something worth diving deeper into, especially at places like Alamance bail bonds! follow this link
My recent root canal was so much easier than expected thanks to my amazing dental team from #### anyKeyWord ##### san diego dentists
It’s essential to have a cosmetic dentist you trust. I found mine at cosmetic dentist near me in Escondido!
Wonderful tips! Find more at LuxeNeuro .
Sooo excited finally establishing connections friends/peers during this challenging time feels nice knowing aren’t alone anymore!!! 💕🤗💞❤️🌈 celebrate little wins big victories even when things seem tough sometimes:) Remember stay strong rely support dentist in oceanside
I love my new window tint from Clear View Glass and Tint in Phoenix! Fantastic service and quality! auto tint near me
Biryani is life, and I found some amazing variations online—check them out over ## indian street food spokane valley
I enjoyed this post. For additional info, visit Boiler repairs .
ใช้ BT PREMIUM มานานแล้ว ชอบแสงสว่างที่มันให้มากครับ ร้าน ตั้งไฟหน้ารถยนต์ ใกล้ ฉัน
This was very beneficial. For more, visit local fall heating installation .
I’ve been taking yoga classes for a few months, and the results have been outstanding! My flexibility has improved as well, and my anxiety levels have decreased considerably. I adore how each session feels like a mini-daily break yoga
Your recommendation to keep a travel journal is such a great way to document experiences! myrtle beach travel agency
Appreciate the thorough information. For more, visit https://www.bookmark-fuel.win/solutions-for-a-clogged-bathroom-what-really-works .
If you’re looking for reliable electrical work, I highly recommend Summit Services as the best electrician in Bluffton, South Carolina! Electrician Bluffton
I always use trusted dumpster rental orlando when I need a construction dumpster in Orlando. They never disappoint!
มีวิธีตรวจสอบคุณภาพของไฟหน้ารถ LED อย่างไรบ้าง? ร้าน แต่ง ไฟ รถยนต์ ใกล้ ฉัน
The area on modifying software program techniques changed into super important! It’s top to know what tools are accessible. Explore added at https://www.bookmark-url.win/after-shooting-portraits-and-films-take-time-to-check-your-footage-on-a-bigger-reveal .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic Aurora expertise
I’m interested in learning more about waterproofing options for roofs in our climate. https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch places near me
I found this very interesting. For more, visit Walter’s BBQ Southern Kitchen .
Very informative article. For similar content, visit i need a plumber .
What’s up, yeah this article is in fact fastidious and I have learned lot of things from it regarding blogging.
thanks.
This was very enlightening. More at Bonney Lake oil Change .
Thanks for the practical tips. More at cheap plumber .
The bond between people and puppies is quite specified and original! How did you meet your hairy chum? Share the tale at https://zoom-wiki.win/index.php/How_to_Create_a_Daily_Routine_that_Works_for_You_and_Your_Dog_62671 .
Learning distinctive command cues permits seamless verbal exchange among persons/pets alike –What commands a hit taught YOUR Furry Friends all through reports shared among others? https://remote-wiki.win/index.php/Dealing_with_Separation_Anxiety_in_Dogs:_Helpful_Strategies
I enjoyed this read. For more, visit Leaking radiator valves .
I found this very helpful. For additional info, visit professional commercial plumbing .
The atmosphere at American Laser Med Spa makes all the difference during treatments—check them out via dependable coolsculpting !
If you’re in search of an empathetic car accident lawyer, take a look at what’s available through Personal injury attorney .
Say goodbye to stubborn fat and hello to a more sculpted physique with Coolsculpting treatments from expert coolsculpting services – your trusted Midland provider.
My games pc recently had an incredible encounter with a nearby repair factory. After a annoying week of specialized issues, I brought it in for repairs, and the team was extremely educated iPhone repair services
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic massage therapy
Excellent article! It’s crucial to keep our devices in top condition, whether they’re our apps, gaming devices, or laptops. Being able to depend on these devices for both labor and amusement, having a trustworthy restoration company can be everything Computer maintenance services
I just realized about the Basenji breed and their unusual barkless trait—so fascinating! https://www.yankee-bookmarkings.win/6-issues-that-we-should-take-into-consideration-prior-to-deciding-to-buy-a
My travel bucket list keeps growing! Just added Iceland and its stunning landscapes! travel agency myrtle beach
This was a great article. Check out phim sex hay for more.
This was quite informative. For more, visit 24 7 plumber in my area .
Fantastic breakdowns on various marketing channels—Social Cali of Rocklin seems like an expert in navigating them all! knowledgeable affiliate marketing agencies
Thanks for the clear breakdown. Find more at Boiler breakdowns .
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Top brunch restaurants in Pittsburgh
I recently got my car tinted at Clear View Glass and Tint in Phoenix, and I couldn’t be happier with the results! auto tint near me
The potential hazards of not knowing where your utilities are located are too high—thank you, Utility Locating , for advocating safety!
I love that American Laser Med Spa offers such innovative treatments like CoolSculpting. endorsed coolsculpting is definitely on my radar!
Thanks for sharing this, especially with how legal liability play out in Annapolis. The statute of limitations part was eye-opening. How do you see this evolving with new insurance laws in MD? Get more clarity here: Car accident .
I was blown away by how quick and professional Summit Services was during my recent HVAC repair. Great job! Air conditioning repair
I enjoyed this post. For additional info, visit Walters Barbecue Southern Kitchen .
What a treasure trove of information ! Individuals residing near glendale searching assistance should definitely consider connecting experts mentioned throughout including # # anyKeyWord # Electrician Glendale
It’s crucial to have a trustworthy electrician. In Glendale, I found mine through Electrician Near Me !
Love the focus on DIY safety tips! Remember to reach out to professionals like those at Electrical Contractor if you’re in Glendale!
Car mishaps are stressful enough without needing to handle legal issues alone. A great vehicle mishap lawyer in Irvine can help ease that tension– check out Car accident lawyer near me for more information!
Appreciated reading these guidelines presented today ; if everyone living around glendale searched properly they’d find assistance listed under # # anyKeyWord # Electrician Glendale Arizona
Thanks for the clear breakdown. Find more at https://checkmakeup.com/user/mechalfkte .
Great insights on electrical safety! If anyone needs an electrician in Glendale, AZ, visit Electrical Contractor Glendale Arizona for excellent service.
..communities— trusted Coquitlam plumbing companies
This was a fantastic read. Check out plumbing and heating repairs for more.
I called Summit Services for an emergency issue in Hilton Head Island, and they were quick to respond and fix it! Electrician near me
It’s crucial to have reliable ###Vancouver plumbing companies### on speed dial for those unexpected issues! trusted water heater servicing
Appreciate the useful tips. For more, visit quick same day plumber .
This is highly informative. Check out car accident lawyer near me for more.
Great process breaking down frustrating issues into achievable portions of statistics—it makes a change!! https://wiki-triod.win/index.php/**Choosing_the_Right_Spot:_How_to_Mount_Your_Security_Camera_Effectively**
This was quite useful. For more, visit Pittsburgh Brunch Menu .
For anyone near Palm Coast, don’t miss out on enjoying some incredible sushi at Ginger Bistro—it’s a game changer! Sushi near me
If you’re looking for the best ##pool screen## repair in Jacksonville, A+ Gutters is the place to go! They did an amazing job on my pool area. lanai screen repair near me
Anyone else love discovering hidden gems among local #Plumber contractors? So many great options! expert plumbers in Kelowna
Thanks for the useful suggestions. Discover more at LuxNuro .
When facing tough choices regarding medical bills & lost wages due damages incurred due negligence – reach out ASAP!!!##### truck accident lawyer
Recently, I took a yoga class that certainly altered my outlook on natural well-being and mindfulness. The instructor stressed the value of relating breathe and motion, which made each pose feeling more grounded and deliberate yoga
If you’re planning any excavation work, don’t forget to contact an expert like Utility Locating . Their services can save you a lot of trouble down the line.
This was a great article. Check out DSH Homes and Pools for more.
This was quite enlightening. Check out http://www.lvovvv.ru/user/ossidyiexy for more.
Great article! It’s crucial to understand the factors that influence roofing costs. When considering contractors, I always recommend getting multiple quotes to ensure you’re not overpaying roofers near me
This was very insightful. Check out http://gamesgrom.com/user/lipinnuacs for more.
This was very beneficial. For more, visit Walters BBQ Southern Kitchenac .
What’s the first-class means to refreshing cussed stains from concrete employing a drive washer? I desire professional information! https://squareblogs.net/flaghyqbdr/the-evolution-of-pressure-washers-from-invention-to-innovation
Hey! Someone in my Myspace group shared this site with us so I came to
take a look. I’m definitely loving the information. I’m bookmarking and will
be tweeting this to my followers! Wonderful blog and outstanding style and design. http://www.innerforce.co.kr/?document_srl=2422043
Well done! Find more at https://chasti-kinos.online/user/brendatwxl .
Watching films showcasing talented pooches appearing methods creates smiles all over the world —Is there ONE trick/act that maintains pleasing audiences online in recent times according TO YOU ? https://oscar-wiki.win/index.php/Building_a_Strong_Bond_with_Your_Rescue_Dog_55430
Appreciate the insightful article. Find more at https://www.rankbookmarkings.win/exactly-how-to-set-up-a-new-bathroom-seat .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Aurora’s leading massage therapists
Dogs have an uncommon capability to adapt; how does yours control variations in events or ecosystem? Let’s chat about adaptability on https://wiki.fc00.ru/index.php?title=The_Importance_of_Hydration_in_Maintaining_Canine_Health_75000 .
Quality articles or reviews is the important to attract the viewers too pay a quick visit
the web page, that’s what this web page is providing.
my page; kas private boat trip
I am truly grateful to the owner of this web site who has shnared this impressive article
at at this time.
Here iis my page – kas private boat trip
Couldn’t agree more; seriously considering making that call today about scheduling my first consult regarding cool sculpt services available through american laser med spa!! endorsed coolsculpting
From appetizers to desserts, every dish at Ginger Bistro shines—best choice for Chinese cuisine without question! chinese food
Great insights! Discover more at https://telegra.ph/Choosing-the-Right-Tires-in-Bonney-Lake-WA-Choosing-the-Right-Tires-in-Bonney-Lake-WA-07-13 .
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Outdoor brunch seating in Pittsburgh
I enjoyed this read. For more, visit Walters BBQ Southern Kitchen .
Love discovering about green alternatives—it’s fine figuring out we will be able to avoid our environment easy responsibly!!! ## https://wiki-burner.win/index.php/From_Grimy_to_Gleaming:_Cleaning_Your_Sidewalk_Without_Pressure_Washing
I just recently had to hire a car accident lawyer in Irvine after a crash, and it made all the distinction. They were experienced and helpful throughout the process. Have a look at Car accident lawyer near me for more information!
Dreaming of a flatter stomach? CoolSculpting can help eliminate stubborn belly fat and reveal a more sculpted abdomen. Visit ethical coolsculpting for personalized treatment options.
Appreciate the thorough insights. For more, visit plumber .
This blog is a must-read for homeowners! Mold inspections are essential, and the service from mold inspections near me was top-notch.
Loving the advice shared here about home safety; if anyone’s looking for reliable service in Glendale don’t hesitate to call on the experts at Electrical Contractor
Incredible compilation showcasing diverse experiences shared surrounding common obstacles faced repeatedly encouraging positive dialogue promoting growth collectively focused achieving milestones reached through collaboration prioritizing transparency Electrician in Glendale Arizona
This post is so informative! For electrical issues in Glendale, AZ, I always turn to Electrician Glendale Arizona .
Appreciate the thorough information. For more, visit commercial plumbing .
Midland’s Coolsculpting centers boast a team of experts who are dedicated to helping you achieve your body goals. proficient coolsculpting specialists
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrical Contractor Glendale Arizona
Awesome article full of practical advice on hiring electricians; locals might find what they need at Electrician
This post has so much useful information; if you’re looking for electricians near me go ahead and check out the team at Electrician Near Me
I recently had a great experience with a neighborhood repair shop that specializes in cellphone repairs, video sport repairs, and computer repairs Computer maintenance services
This is very insightful. Check out professional commercial pest control Chester for more.
Excellent insights into the value of maintaining the best possible equipment! Being thus dependent on servers, video games, and phones these days is essential, but having a trustworthy restoration service is essential Cell phone fixing
I’m so glad I chose American Laser Med Spa in El Paso for my laser hair removal; it was worth every penny! trusted coolsculpting
The team at experienced roofing firm is reliable, efficient, and dedicated to providing top-notch roofing solutions in Carlsbad. I’m glad I chose them for my project.
For anyone searching for reliable gutter solutions, check out A+ Gutters; they’re the best around St Johns County! gutters near me
Navigating insurance claims after an automobile mishap can be challenging. A specialized legal representative can help alleviate that concern. Learn more at Car accident lawyer near me for expert recommendations in Irvine!
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Massage therapy near me
If you are in Winston-Salem and need window cleansing, I notably propose Sully’s Pressure Washing. They did a extraordinary task! Window Cleaning Service
Great breakdown, Alex. I’ve been looking for a solid broker
with both MetaTrader and cTrader support — didn’t know FxPro had its own platform too.
That Trust Score really caught my eye. Appreciate the
honest take on the pricing!
This was very well put together. Discover more at phim sex .
I found this very interesting. Check out trusted kitchen plumbing for more.
Helpful tips on home electricity management! For experts in Glendale, visit Electrical Glendale Arizona !
I adore yoga’s transformative authority. It promotes emotional clarity and emotional balance as well as increasing flexibility and stamina. I’ve found that enrolling in typical yoga sessions has substantially improved my total well-being yoga
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch events Pittsburgh
Thanks for the practical tips. More at Denver Neurofeedback Treatment .
What are your techniques on using difficult water as opposed to comfortable water when operating force washers?? Any options?? # # anyK eyword ## Great site
Awesome place filled with awesome people doing awesome work!!! Every aspect exceeded my expectations & then some!! :# # anyKeyWord ## proficient coolsculpting specialists
If you want peace of mind while digging, make sure you hire experts like Utility Locating to locate utilities first.
Awesome read! Mold can lead to serious problems if left unchecked; that’s why I trust mold inspections near me for all my inspection needs.
Helpful tips on home electricity management! For experts in Glendale, visit Electrician Glendale !
This was highly useful. For more, visit Walter’s BBQ Southern Kitchen .
ใช้ไฟหน้ารถ LED BT PREMIUM แล้วไม่ต้องเปลี่ยนบ่อยๆ ดีใจมากครับ ร้านตั้งไฟหน้ารถยนต์ ใกล้ฉัน
Excellent essay It’s remarkable how frequently we take our products for granted until something goes wrong Laptop fixing
If you’re searching for quality HVAC repair services near me, I highly recommend Summit Services in Bluffton! They do amazing work! Learn more at ac service .
Recently had major fixes done by an incredible #### Vancouver Plumbing Service ##### and couldn’t be happier! professional hot water tank replacement Vancouver
The team I found through emergency plumbing service Coquitlam was fantastic! They are definitely some of the best Coquitlam plumbing contractors I’ve worked with.
Thanks for the helpful article. More like this at Pest Control Chester .
This is very insightful. Check out average plumber prices for more.
If your PS5 won’t turn on, trust me—head to PS5 Repair Near Me for a speedy solution.
Excited about starting orthodontic treatment! Thanks, Dentist of SD! dentist near me
I love my grace dental in Oceanside! They always take such good care of me.
Anyone else love their results from Dr Brilliant DDS ? I’m thrilled with mine!
Learning so much already just browsing through various patient testimonials linked back towards this site: ## north park smiles
Experience the benefits of CoolSculpting sessions at expert-driven coolsculpting therapy and enjoy a body you’ll be proud to show off.
I love how easy it is to rent a recycling dumpster in Orlando through top-rated dumpster rental orlando . Their customer service is top-notch!
Thanks for the useful suggestions. Discover more at local plumbing companies .
I’ve been practicing yoga for a while, and I’ve found that taking various courses genuinely helps me understand the art. I enjoy looking at different styles, from Hatha to Vinyasa, and observing how each group produces its own distinctive electricity hotworx yoga class
Thanks for the clear breakdown. More info at Walters Barbecue Southern Kitchen .
A friend had her water heater repaired by an excellent local #plumbing service in #Kelowna—will definitely reach out! professional plumbing contractors in Kelowna
For anyone needing a skilled electrician in Bluffton, I can’t recommend Summit Services enough – they are amazing! Electrician
I enjoyed this post. For additional info, visit LuxNeuro .
I think more people need to understand the risks involved in digging without locating utilities first. Companies like Utility Locating are essential for preventing disasters.
Cars and truck mishaps are difficult enough without needing to handle legal problems alone. An excellent automobile accident lawyer in Irvine can assist relieve that tension– take a look at Car accident lawyer near me for more information!
”Can’t help but smile every time I leave after my session!” credible coolsculpting treatments
Personal injury cases require expertise and compassion; many top attorneys can be found at Local law firms .
ไฟหน้ารถ LED ช่วยประหยัดพลังงานได้จริงหรือเปล่า? ร้าน ไฟ
Thanks for the detailed guidance. More at 24 7 plumber .
I simply learned about the Basenji breed and their distinguished barkless trait—so remarkable! https://www.echobookmarks.win/history-of-the-pit-bull
I appreciated this article. For more, visit https://limefilm.cc/user/kenseyogzs .
If you haven’t yet chosen an HVAC contractor, do yourself a favor and visit hvac contractor san diego # today!
This was highly useful. For more, visit Walters BBQ Southern Kitchenac .
Thanks for the clear breakdown. Find more at expert 24 7 plumbing .
Anyone else think that sharing plates makes for the best dining experience? Love trying bites from everything; let’s find great shareable options suggested by experts on indian cuisine spokane valley !
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic personalized care
This was a wonderful guide. Check out https://maps.app.goo.gl/S23gr3cnAzptbSkN7 for more.
Very useful post. For similar content, visit roof installation .
I’m planning on scheduling an appointment at American Laser Med Spa – Midland soon! Excited! experienced coolsculpting providers
My **# # anyK e yword # #** was proactive and always kept me informed; communication is so important in these cases! motorcycle crash lawyer
I can’t get enough of Ginger Bistro’s sweet and sour pork! It’s the best Chinese restaurant I’ve found near Palm Coast. You have to try it! chinese near me
Incredible compilation showcasing diverse experiences shared surrounding common obstacles faced repeatedly encouraging positive dialogue promoting growth collectively focused achieving milestones reached through collaboration prioritizing transparency Electrician Glendale
I just recently needed to work with a vehicle accident legal representative in Irvine after a crash, and it made all the difference. They were knowledgeable and supportive throughout the process. Take a look at Car accident lawyer near me for additional information!
This is such timely advice! Residents of Glendale should definitely consider contacting Electrician Near Me for help.
Awesome article! Discover more at phim sex hay .
Great job! Discover more at https://www.silversevensens.com/users/OptionRestoration45/ .
Kudos for tackling this subject effectively ! Homeowners experiencing difficulties would benefit knowing where they can find qualified guidance through resources like # # anyKeyWord # Electrician in Glendale Arizona
I found out your counsel on shooting in exclusive lighting circumstances very informative! Can’t wait to take a look at them out. More details at https://www.click-bookmark.win/always-comply-with-native-rules-and-checklist-when-flying-your-drone-camera .
Very informative article. For similar content, visit clogged toilet service near me .
I always read your posts for helpful info! For electrical services in Glendale, don’t miss Electrical Contractor Glendale Arizona .
The staff’s friendliness and expertise made my experience at American Laser Med Spa for laser hair removal enjoyable! endorsed coolsculpting
Thanks for the practical tips. More at affordable same day plumbing .
Such useful information about home wiring! Don’t forget to look at Electrical Contractor if you’re in Glendale!
If you’re looking for a reliable electrician in Glendale, Arizona, I highly recommend checking out Electrician .
Thanks for providing such helpful content; it’s perfect for residents looking for electrical solutions in Glendale like me who found it through Electrician Near Me
I’ve heard about the theta state in meditation circles, but I didn’t realize top performers actually use it too.
Super interesting!
This was very beneficial. For more, visit professional clogged shower drain .
hi!,I really like your writing so a lot!
proportion we be in contact more approximately your article on AOL?
I require an expert in this space to unravel my problem.
Maybe that is you! Taking a look forward to look you.
Great tips! For more, visit Ready Roof Inc. .
I just had a wonderful practice with a neighborhood repair shop that specializes in cellphone repairs, video gameplay repairs, and computer repairs Cell phone fixing
This was quite informative. More at https://maps.app.goo.gl/uCQajg6ZshPLYTPW8 .
Training classes are fine for socialization—what lessons have worked optimal for you and your domestic dog? Exchange thoughts over at https://golf-wiki.win/index.php/Fun_Facts_About_Dogs_That_Will_Make_You_Smile!_43842 !
It is perfect time to make some plans for the future and it is time to be happy.
I’ve read this post and if I could I wish to suggest you few interesting things or tips.
Maybe you can write next articles referring to this article.
I desire to read more things about it!
The bond we share with our canine in general lasts a life-time; what stories do you cherish so much with yours? Reflect with us on https://romeo-wiki.win/index.php/Pros_and_Cons_of_Crate_Training_Your_Puppy_40460 .
Fantastic post! Discover more at Meigel Home Improvements – Kitchen & Bathroom Remodeling Company .
Just wanted to share how awesome A+ Gutters is! They fixed my gutters quickly and efficiently in St Augustine. gutters near me
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
This was quite informative. For more, visit mommy makeover consultation .
Great insights! Find more at https://www.belogour.news/user/gertonqadt .
Anyone else had success stories after taking their devices into macro repir lately? I’d love hearing all about them! pc repair
This was beautifully organized. Discover more at shower refinishing services .
Valuable information! Discover more at trusted roofing services near me .
Looking for the best HVAC service near me? Summit Services did wonders for my air conditioning unit! hvac repair
This was a wonderful guide. Check out https://lordfilmy2025.org/user/beliasdovz for more.
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch places near me
This was quite informative. More at trusted remodeling company near me .
Your methods for preserving a pressure washer are valuable—I’ve had mine clog up prior to, and it used to be complex! Homepage
Appreciate the detailed information. For more, visit Denver neurofeedback treatment options .
Nicely done! Find more at local tap specialists .
Thanks for the valuable insights. More at Ready Roof Inc. .
The expertise offered by companies like 811 dig is invaluable for both homeowners and contractors alike.
Excellent insights into the importance of proper fixes for our software devices! It’s amazing how quickly things may go wrong with devices, games consoles, or laptops, but the right repair company can give them new life Computer maintenance services
Excellent article! How crucial our gadgets have become to our routine existence is amazing iPhone repair services
Useful advice! For more, visit local roofing companies near me .
Personal injuries require thorough legal knowledge; that’s why researching local firms on platforms like Car accident law firm near me is so helpful.
Thanks for the detailed post. Find more at spacious venues for celebrations .
Great post! It’s so crucial to have legal representation if you get into a mishap in Irvine. I found my lawyer through Car accident lawyer near me , and they were wonderful!
This is such valuable information! If anyone needs electrical help in Glendale, I recommend Electrician Near Me .
Great job! Find more at Afordable Pest Solutions .
Nice tips shared ; make sure you’ve got contacts ready incase you need fast reliable service from qualified people like those featured at # # anyKeyWord # Electrical Contractor Glendale Arizona
This was a wonderful post. Check out Aesthetic Plastik Surgery and Lazer Center for more.
Great article! I found an amazing electrician through Electrician Glendale Arizona right here in Glendale.
Appreciate the insightful article. Find more at 24 7 plumber .
Thanks for the useful suggestions. Discover more at Clogged toilet repair .
Lovebeingpartofthiscommunitybecauseeveryonehereisso supportiveandencouragingwheneverI sharemyjourneythroughtheirservicesavailablehere@americalasermedspa !! # # anyKeyWord# # ethical coolsculpting
Yours was an eye-opening experience reading today about current trends impacting residential lifestyles significantly leaving lasting impressions notably reminding us why we must adhere regulations set forth adhering timelines outlined ensuring smooth Electrician
Kudos for tackling this subject effectively ! Homeowners experiencing difficulties would benefit knowing where they can find qualified guidance through resources like # # anyKeyWord # Electrician Near Me
Appreciate the detailed information. For more, visit shower refinishing services .
Thanks for the useful suggestions. Discover more at emergency same day plumber .
Valuable perspectives shared here within context we all need more education surrounding electricity & its usage ; local residents shouldn’t hesitate contacting teams affiliated via # # anyKeyWord # Electrical Contractor
This was very enlightening. For more, visit best window replacement .
Wish I had examine this faster—my concrete has been begging for some TLC, and now I’m able to offer it some love! https://magic-wiki.win/index.php/Why_Manual_Cleaning_is_Better_for_Some_Types_of_Concrete_Surfaces
I appreciated this post. Check out auto repair Buckley for more.
Thanks for the great tips. Discover more at Foot Hills Paving .
This was a wonderful post. Check out Walter’s BBQ Southern Kitchen for more.
I’ve tried other pressure washing services before, but All Seasons is by far the best in Cape Coral! Pressure Washing Company
Just got my windows tinted at Clear View Glass and Tint in Phoenix. The difference is incredible! Highly recommend their service! auto tint near me
I love how effective strain washers are when compared to traditional cleaning systems. Great learn! https://kilo-wiki.win/index.php/The_Evolution_of_Pressure_Washers:_From_Invention_to_Innovation_94134
You won’t find better pressure washing services in Tampa than at home pressure washing near me Tampa Bay Pressure Washing .
After my recent accident, I felt overwhelmed. Fortunately, I discovered a great automobile accident attorney in Irvine who guided me every action of the method. Highly suggest taking a look at Car accident lawyer near me !
This blog has opened my eyes to the significance of drainage systems in roofs during installation—thank you! Check out authoritative roofing solutions for more!
I strongly recommend contacting a professional service like Underground utility locating services if you’re planning any renovations!
This really hits home. I’ve always felt like I was doing everything
right but still not moving forward financially.
Definitely curious to learn more about this mental reprogramming angle!
Anyone else find laser facials addicting after trying them once? Thank you, American Laser Med Spa – Midland, for introducing me to this fabulous treatment option!! # # anyKeyWord # approved coolsculpting clinic
This was a fantastic resource. Check out Sani flo for more.
It’s refreshing to see non-invasive options like CoolSculpting gaining popularity—can’t wait to explore this further with # # anyKeyword # #. expert-driven coolsculpting therapy
Don’t let moving day overwhelm you; hire local professionals who know the area well—learn more via Cheap movers Mulberry !
Well done! Find more at Walters BBQ Southern Kitchenac .
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrician Glendale
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Pain relief massage near me
This really shed light on a common situation, especially when it comes to minor crash injuries. So many overlook the importance of the police report Personal injury attorney
มีใครอยากแชร์รูปไฟหน้ารถ LED ของตัวเองบ้าง? ร้าน ไฟ
Personal injury cases require expertise; local law firms listed at Local law firms have the experience you need.
Cleanliness rapidly influences sturdiness-grateful any individual addressed such precious facets-I’ll join instantly at %. Roof Cleaning Service
Appreciate the thorough insights. For more, visit bay area car wraps .
This was a wonderful post. Check out construction companies for more.
Really valuable info. The section on client communication was especially important. In Dallas County, Texas, working with a knowledgeable general contractor can really make or break a project Construction company
I found this very helpful. For additional info, visit quick central heating installations .
Hopeful others achieve concept following along discussions revolving round recommendations top valuable navigation pathways coming into new realms surrounding securing satisfactory protections placed forth effectively-out there channels selling Home Insurance
Every breed has its quirks – what is one precise issue approximately your puppy’s personality that regularly makes each person snigger ? Let’s replace studies over ### anykeyword ### https://wiki-planet.win/index.php/Dogs_Who_Doodle:_The_Rise_of_Designer_Breeds_40994
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch restaurants near me
This is quite enlightening. Check out Pittsburgh brunch value deals for more.
The technology used at American Laser Med Spa – Midland is top-notch. Very impressed! professional coolsculpting clinic
Excellent insights into the value of regular maintenance for our tools! It’s so simple to overlook minor problems before they escalate to significant issues phone repair services
Valuable perspectives shared here within context we all need more education surrounding electricity & its usage ; local residents shouldn’t hesitate contacting teams affiliated via # # anyKeyWord # Electrical Contractor
После арендаторов, которые прожили там пять лет,
состояние жилья оказывалось так себе; я решила освежить ремонт.
Here is my blog :: https://krasnodar.helpmens.ru
If you’re unsure about DIY fixes, consult with an experienced ###Vancouver plumber### before attempting anything complicated. hot water tank maintenance
Thanks for the great tips. Discover more at affordable leak detection services .
Just wanted to share how happy I am after hiring a plumber through experienced plumbers #; they made everything so hassle-free in Coquitlam.
Useful advice! For more, visit sex tre em .
Don’t let financial constraints hinder your journey towards a slimmer figure. Explore the affordable CoolSculpting cost options at reputable coolsculpting and make your dream body a reality.
Thanks for the thorough analysis. More info at local dishwasher repairs .
If you’re feeling stiff or sore after sitting all day at work—definitely consider visiting a chiropractor near you like those in Mesquite, TX! Premier Injury Clinics Mesquite – Auto Accident Chiropractic
Kids love bouncing, and so does everyone else; great choice by going with # anyKeywords #. bounce house water slide rentals
Thank you for shedding light on the significance of having a trustworthy trucking accident attorney !
This was quite informative. More at Aesthetic Plastic Sugery & Lasor Center .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic massage
Loved your insights on drone upkeep! Keeping my camera in accurate form is mandatory. For added tips, go to https://www.random-bookmarks.win/utilize-varied-flight-modes-sold-by-way-of-your-drone-for-the-various-filming-kinds .
Appreciate the comprehensive advice. For more, visit Foot Hills Paving .
I appreciated this post. Check out Kitchen plumbing for more.
Excellent article! It’s crucial to stay informed about typical issues that arise with our equipment with the rapid advancement of technology Computer maintenance services
Excellent insight into how crucial standard upkeep is for our tools! It’s crucial to keep our servers, match computers, and phones in bottom condition to prevent surprising losses given the rapid advancement of technology Smartphone repair
While CoolSculpting is generally well-tolerated, some individuals may experience temporary swelling, redness, or bruising in the treated area after the procedure, which should fade over time. endorsed coolsculpting
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch and bottomless mimosas Pittsburgh
Appreciate the thorough insights. For more, visit Kitchen sink plumbing .
Great tips! For more, visit floral decor for wedding .
Anyone else taken advantage of seasonal promotions or discounts? Would love insight on those experiences. credible coolsculpting treatments
Love this blog! If you’re looking for electricians in Glendale, be sure to check out Electrician in Glendale Arizona .
Excellent post! It’s so crucial to have legal representation if you get into an accident in Irvine. I found my attorney through Car accident lawyer near me , and they were fantastic!
Wonderful insights shared here ! In case anyone feels overwhelmed about their electric issues , they can always reach professionals via # # anyKeyWord # Electrical Contractor Glendale Arizona
Good to know about local resources! For electrical services in Glendale, look at Electrician Glendale .
Educating myself about proper hygiene habits became fun rather than stressful due mainly due exploring materials gathered across ### Any Keyword ### san diego dentists
Just got braces from my # anykeyword#(in oceansid#)—excited for this journey! grace dental oceanside
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrician Glendale Arizona
Amazing how quickly things improve once you decide to invest time into oral health; grateful I found guidance here: ## north park smile
”Feeling confident recommending friends family alike towards utilizing resources available within macro repirs network moving forward!” ipad repair
If you’re in Glendale and searching for a dependable electrician, I suggest visiting Electrician .
Cosmetic dentistry can really boost your confidence. Glad to see great options like escondido cosmetic dentist in Escondido!
Glad to see more emphasis on professional standards; folks needing assistance with their wiring should contact the specialists over at Electrician Near Me
This was highly educational. For more, visit water heater repair near me .
Thanks for the clear breakdown. More info at air conditioning maintenance near me .
This was highly useful. For more, visit roofers .
Appreciate the comprehensive advice. For more, visit Disabled WC .
Thanks for highlighting these issues ; locals facing similar challenges should connect with skilled individuals available through # # anyKeyWord # Electrical Contractor
I appreciated this post. Check out Affordible Pest Solutions for more.
This was a great article. Check out Aestheic Plastic Surgery & Laser Centre for more.
Having access to knowledgeable legal professionals makes all the difference during tough times; check out ###anything### for lawyers near you! Car accident attorney
Thanks for the comprehensive read. Find more at https://elliotlchs972.theburnward.com/why-buckley-drivers-shouldn-t-ignore-that-check-engine-light-5 .
The staff at American Laser Med Spa are so knowledgeable about CoolSculpting! Highly recommend them! certified coolsculpting specialists
Appreciate the detailed post. Find more at construction companies .
For anyone looking for an electrician near me, Summit Services is the answer in Bluffton! Great work every time! Electrician Bluffton
If you’re in St. Augustine and craving Chinese food, Ginger Bistro is a must-visit. You won’t be disappointed! chinese restaurant
Nicely detailed. Discover more at phone lookup tool .
I’ve been putting off my roof repairs forever; this article pushed me to take action—thanks so much—I’ll reach out to # anykeyword# soon! certified roofing contractor
Thanks for the helpful advice. Discover more at professional emergency plumbing .
This was very insightful. Check out Mr. Clean Power Washing, LLC for more.
Great job! Discover more at local underfloor heating services .
Great job! Discover more at security service .
I appreciated this post. Check out phim sex hàn quốc for more.
Your focus on youth education about guns and safety is so necessary, especially through platforms like Authorized and Licensed firearms and Air Guns Dealers .
Great insights on stucco costs! I never knew how many factors could influence the price of a stucco job. It’s essential to gather multiple estimates from Stucco contractor Fort Saskatchewan to make an informed decision. Check out the post right here
The Coolsculpting providers in Midland prioritize your safety and satisfaction throughout your treatment journey. authoritative coolsculpting
These are actually great ideas in concerning blogging.
You have touched some fastidious things here. Any way keep up wrinting.
Appreciate the helpful advice. For more, visit https://stack.amcsplatform.com/user/britteoijh .
Looking for dependable gutter services? Look no further than A+ Gutters in St Augustine—they’re the best around! gutters near me
I needed to thank you for this very good read!! I absolutely loved every little bit of it.
I’ve got you book marked to check out new things you post…
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic professional massages
Great job! Discover more at best air conditioning maintenance .
Great insights! Find more at affordable plumbers in my area .
This was quite informative. For more, visit http://hqarea.altervista.org/Upload/member.php?action=profile&uid=216058 .
Tried a crypto deposit, it was instant!
My website – https://elliotygpm64959.like-blogs.com/35536387/plinko-mania-win-big
Heat pumps can struggle when temperatures drop below 30°F, causing them to lose efficiency. If you’re noticing performance issues, it might be time to call a technician. For reliable repairs and advice, look into heat pump repair Middlefield CT. Click here for more info
Couldn’t agree greater approximately how a lot less demanding lifestyles will become with a first-rate pressure tool like this handy!! https://list.ly/usnaerczlj
การเลือกซื้อไฟหน้ารถ LED ควรพิจารณาอะไรบ้าง ?? #BT_PREMIUM## ร้านทําไฟรถยนต์ ใกล้ฉัน
Excellent essay Knowing how to handle computer inspection, game console repairs, and smartphone inspection can save a lot of headaches, but it’s always a concern when our devices break down Desktop computer repair
Did you understand that having an automobile mishap attorney can considerably increase your possibilities of getting fair compensation? If you’re in Irvine, consider connecting to a specialist through Car accident lawyer near me .
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch near downtown Pittsburgh
Fantastic insight provided here – loved every bit of it ! Neighbors encountering problems could gain significant help by tapping into resources found over at # # anyKeyWord # Electrician
Excellent points about electrical maintenance! For residents of Glendale, AZ, check out Electrician Glendale Arizona .
If you’re in search of an empathetic car accident lawyer, take a look at what’s available through Car accident attorney .
This is such timely advice! Residents of Glendale should definitely consider contacting Electrician Near Me for help.
If you’re facing frequent leaks, it might be time to consult with a professional ##Vancouver plumber## about your options. best water heater repair services Vancouver
Thanks for the informative post. More at emergency plumber near me .
Very informative post ! If someone’s searching around glendale area , they shouldn’t miss seeing what solutions await through # # anyKeyWord # Electrical Contractor
The tips for new gun owners on Stallion Guns are incredibly helpful! Great resource for beginners.
..empowering— Coquitlam plumbing contractor services
Well explained. Discover more at zero-cost phone search .
This was quite informative. More at trusted same day plumber .
Your article is super helpful especially regarding emergencies; keep bystanders safe and call experienced electricians like those from Electrical Contractor
I learned the tough way how crucial it is to have legal assistance after an auto accident. If you’re in Irvine, do not think twice to connect to a certified attorney through Car accident lawyer near me .
Thanks for the helpful advice. Discover more at http://v985223a.beget.tech/index.php?action=profile;area=forumprofile;u=192085 .
The contrast between extraordinary drone fashions used to be awfully impressive! It helped me prefer the top one for my needs. Check out extra at https://www.bookmarking-jet.win/to-use-a-drone-digital-camera-competently-beginning-by-using-familiarizing-your-self-with-the-controls-and-settings .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Effective pain management near me
Excellent article! It’s incredible how crucial it is to have trustworthy rebuild services for our devices. Specialist repairs can save us time and money whether it’s a pc acting slowly, a gaming console that won’t turn on, or a phone with a cracked screen Desktop computer repair
I just had a wonderful practice with a nearby software restoration business that specializes in everything from phone repairs to computer repairs Smartphone repair
Metal roofing provides excellent protection against extreme weather conditions, including heavy rain and strong winds. Safeguard your property with a reliable metal roof from reputable roofing contractor .
My friend recommended Clear View Glass and Tint, and now I see why—they’re simply the best in Phoenix for auto tints! auto tint
Thanks for the insightful write-up. More like this at same day plumber near me .
Just wanted to share that Summit Services is the go-to for anyone looking for a reliable “Electrician” in Hilton Head Island. You won’t be disappointed! Electrician near me
With havin so much content do you ever run into any issues
of plagorism or copyright violation? My website has a lot of exclusive content I’ve either
created myself or outsourced but it appears a lot of it is popping it up
all over the internet without my authorization. Do you know any methods to help reduce content from
being ripped off? I’d truly appreciate it.
This was very beneficial. For more, visit foothills paving and maintenance .
What a great resource! Anyone needing an electrician in the Phoenix area should definitely check out Electrician Glendale
Dogs love variety in their walks—what targeted routes do you take with yours? Share fashionable strolling spots on https://mag-wiki.win/index.php/Exploring_the_Benefits_of_Raw_Diets_for_Dogs_57711 .
I learned so much about what to expect from a motorcycle accident law firm in this article!
Very descriptive blog, I enjoyed that bit. Will there be a part 2?
Giving again closer to shelters is helping shop lives day to day in addition spreading underst https://xeon-wiki.win/index.php/How_to_Choose_the_Right_Name_for_Your_New_Puppy_25206
This was very beneficial. For more, visit clogged shower drain solutions .
I’ve noticeable such a lot of lovable blended breeds not too long ago! Which ones stand out to you? https://www.oscarbookmarks.win/fox-terrier-care-and-coaching
Does all and sundry recognise if there are any ongoing promotions with ##Affordable Hot Water Systems Mandurah##? Top Hot Water Systems Mandurah
The right ##personal injury attorney## not only fights for your rights but also helps you heal from the trauma of an accident. personal injury attorney
Thanks for the practical tips. More at furniture movers atlanta .
I use Ctbeauties and it really help me find good call girl ads in my city. The site is simple and fast. Many profiles with real info and photos. Also my friend post her ad here and she get many calls. It’s good site for both user and girls.
Nashik Call Girls
Great job! Find more at plumbing companies near me .
you are truly a excellent webmaster. The website loading pace is incredible.
It sort of feels that you are doing any unique trick.
Also, The contents are masterpiece. you’ve performed a fantastic activity on this matter! http://Bibsonomyz.club/story.php?title=les-productions-diverso-conception-et-production-devenements
you are truly a excellent webmaster. The website loading
pace is incredible. It sort of feels that you are doing any unique
trick. Also, The contents are masterpiece. you’ve
performed a fantastic activity on this matter! http://Bibsonomyz.club/story.php?title=les-productions-diverso-conception-et-production-devenements
Appreciate the comprehensive advice. For more, visit Boiler breakdowns .
Awesome article.
I perpetually think like I’m coming into a modern homestead perfect after having my home windows cleaned by using # # anyKeyWord # # Window Cleaning Company
Kudos to the amazing team at ## towing services 24/7
Công nghệ AI được BJ88 trang chủ ứng dụng để cải thiện mọi khía cạnh của trải nghiệm người dùng. Chatbot thông minh có thể xử lý hầu hết các yêu cầu hỗ trợ. Hệ thống gợi ý cá nhân hóa dựa trên hành vi người dùng. Phát hiện gian lận tự động với độ chính xác cao. Tối ưu hóa hiệu suất hệ thống theo thời gian thực. Phân tích cảm xúc từ phản hồi của người dùng. Dự đoán xu hướng thị trường để điều chỉnh dịch vụ. Tự động hóa các quy trình vận hành. Cá nhân hóa giao diện theo sở thích từng người. Phân tích rủi ro tự động cho các giao dịch. Tối ưu hóa chiến dịch marketing dựa trên dữ liệu. Hỗ trợ ra quyết định thông qua phân tích dữ liệu lớn.
I found this very interesting. Check out foothills paving and maintenance for more.
Just had my antique warm water manner changed by using ##Mandurah Hot Water Systems, WA##, and it works like a allure now. Cheap Hot Water System services Mandurah
Local law firms often provide personalized services that big ones can’t match; discover them through Car accident law firm near me !
Fantastic publish highlighting the benefits of refreshing roofs; will certainly hold Sully’s Pressure Washing in intellect because of %%anyKeyword%%! Roof Washing
This was quite informative. For more, visit private security companies near me .
Thanks for the thorough article. Find more at shower drain clogged .
Loved this piece. Your point about scope changes really resonated. In Dallas County, Texas, I’ve seen how those factors directly affect both residential and commercial projects Retail Space Construction
Thanks for the informative content. More at reliable gas safety services .
Nicely done! Find more at average plumber prices .
This was quite informative. For more, visit service for reverse number lookup .
Your article has opened my eyes to better digicam placement! Thank you for sharing this vital information! https://mighty-wiki.win/index.php/**How_to_Mount_a_Security_Camera_on_Brick,_Wood,_and_Vinyl_Siding**
Wonderful article! Anyone needing electrical work in Glendale should definitely look into Electrical Contractor Glendale Arizona .
Very important topic you are discussing here; many residents may benefit from knowing where they can find quality electricians such as those listed under # # anyKeyWord # Electrician in Glendale Arizona
Thanks for the clear breakdown. More info at local roofing contractors near me .
I love how you highlighted the importance of hiring local electricians. Check out Electrician if you’re in Glendale!
I love how you highlighted the importance of hiring local electricians. Check out Electrician Glendale if you’re in Glendale!
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Massage therapy in Aurora
It’s great to see more discussions on electrical safety! For those in Glendale, check out Electrician Near Me !
Thanks for the comprehensive read. Find more at cheap plumbing and heating .
Thanks for the useful post. More like this at Buckley auto repair .
Great info on property owners insurance plan for brand new consumers in Cape Coral! I’ll obviously inspect out LP Insurance Solutions. Homeowners Insurance Cape Coral
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Vegan brunch options in Pittsburgh
Great insights! Find more at emergency water leak repair .
Wow this is really insightful information; it’s hard finding good electricians sometimes but I’ve seen positive reviews about those at Electrical Contractor
What are tricks human beings use whilst tackling greater components like driveways well with no wasting an excessive amount of time??? # # anyK eyword ## https://500px.com/p/devpage7vmyxj
So glad I chose Cheap movers Mulberry for my long distance move! Their professionalism is top-notch.
This was very beneficial. For more, visit reliable plumbers near me .
Looking for specialized assistance after a car crash? There are great options available through Personal injury law firms # that cater specifically to your needs!
I found this article incredibly insightful! The way you explained the nuances of the Specialist Sphere really resonated with me. It’s fascinating how specialized knowledge can impact various industries minimally invasive procedures in specialist spheres
This was a wonderful post. Check out moving company for more.
Very informative article. For similar content, visit heating system installations .
This was a fantastic resource. Check out appliance troubleshooting services for more.
If there may be one element I’ve realized raising canines, that’s staying power—how tremendous has endurance been in the course of YOUR travel ? Join discussions relating to growth due to challenges here ### anykeyword ### https://lima-wiki.win/index.php/Understanding_Your_Dog%27s_Body_Language:_A_Complete_Guide
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic CO massage and pain relief
Does someone comprehend if there are any ongoing promotions with ##Affordable Hot Water Systems Mandurah##? Mandurah Hot Water Systems
Loving every single tip presented along each step taken against revitalizing hardscapes open air—it feels lucrative already!!!! ## Go to this site
Great experiences happen when visiting those recommended by others—I’m grateful for insights shared on ### Any Keyword ### san diego smile makers
Best oceansides dentist is hands down one of my favorite healthcare providers!!! ### anykeyword ## surf smiles dentistry
Fantastic tips on maintaining a healthy roof—excited to reach out to Avalon Roofing Services after reading this!! accredited roofing professionals
Thanks for the great explanation. More info at Foot Hills Paving .
Have you ever tried agility exercise along with your dog? It’s this kind of enjoyable way to bond! Find resources on beginning agility schooling at https://wiki-zine.win/index.php/Understanding_Canine_Aging:_Caring_for_Older_Dogs .
Thanks for the comprehensive read. Find more at useful techniques for phone number lookup .
This was very beneficial. For more, visit checkatrade plumbers .
This blog has every part I needed to recognise approximately beginning with a drive washer—thank you for sharing your capabilities! https://post-wiki.win/index.php/The_Benefits_of_Regularly_Pressure_Washing_Your_Home%E2%80%99s_Exterior_25358
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Walter’s BBQ Southern Kitchen hours
Valuable perspectives shared here within context we all need more education surrounding electricity & its usage ; local residents shouldn’t hesitate contacting teams affiliated via # # anyKeyWord # Electrical Contractor Glendale Arizona
I always take my friends to Ginger Bistro when they’re in town—it never fails to impress with its amazing flavors! chinese near me
Thanks so much for taking time put together such detailed guidance regarding wiring matters ; surely everyone needing assistance locally ought explore options available from # # anyKeyWord # Electrician Near Me
Hopefully more people will discover ways they can improve their homes thanks to # dependable dumpster rental orlando
Such a well-written article , thanks ! It gives individuals peace knowing that quality assistance exists nearby – just check it out via links leading towards # # anyKeyWord # Electrician
This is such timely advice! Residents of Glendale should definitely consider contacting Electrician Near Me for help.
This was quite informative. For more, visit Leaking toilet .
Appreciate the thorough analysis. For more, visit emergency plumber .
It’s remarkable in favor of me to have a web page, which is valuable in support of my experience.
thanks admin
I’m curious about how long installations from ##Hot Water System installations## in Mandurah sometimes take? Qualified Hot Water Systems plumber Mandurah
Your article has inspired me to absorb drone photography as a interest! Excited to be trained extra options from you! Visit https://www.bright-bookmarks.win/finally-apply-recurrently-to-improve-your-talents-with-the-two-piloting-and-images-procedures for greater info.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
มีใครอยากแชร์รูปไฟหน้ารถ LED ของตัวเองบ้าง? ร้าน แต่ง ไฟรถยนต์ ใกล้ ฉัน
Valuable information! Discover more at checkatrade plumbing reviews .
Exploring different cultural perspectives toward liability creates deeper understanding within communities—thankful for pieces like those created by # evenAnyword car crash attorney
Thanks for the great content. More at drain plumbers near me .
So this is what they mean when they say ‘in the zone’—theta waves might be the real secret sauce!
I strongly recommend A+ Gutters for anyone needing gutter installation or repair in St Johns County! gutters
Thanks for the useful suggestions. Discover more at custom home builders dallas tx .
Excellent points about electrical maintenance! For residents of Glendale, AZ, check out Electrician Glendale Arizona .
Thanks for the useful post. More like this at sex tre em .
Fascinating exploration into various facets concerning electric issues we often overlook daily ; nearby citizens are encouraged pursue expertise located using links pointing towards # # anyKeyWord # Electrical Contractor
Appreciate the detailed information. For more, visit personal injury attorneys in Port Jefferson .
My coder is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the
expenses. But he’s tryiong none the less. I’ve
been using WordPress on a number of websites for about a year and am concerned about switching to another
platform. I have heard fantastic things about blogengine.net.
Is there a way I can transfer all my wordpress content into it?
Any help would be really appreciated!
Great job! Discover more at Foot Hills Paving .
Well done! Find more at trusted trader plumbers .
Thank you for advocating for safe storage practices through your content at 煞笔 !
My friend suggested visiting a dedicated ##pediatric dentist##, and it was the best decision ever! kids orthodontist
Useful advice! For more, visit air conditioning companies .
Great insights! Find more at competitive plumber prices .
Positive dental experiences in childhood lead to better oral health habits later on; find a supportive local braces dentist near me for your child.
A visit to the ##kids orthodontist## helped us understand what our child needs for their smile journey! braces for kids
This was very well put together. Discover more at gutter repair near me .
I was once inspired via the services of the ##Mandurah Hot Water Systems gurus## who got here to install my formula. Highly put forward them! Affordable Hot Water Systems Mandurah
After searching for the best auto tint, I finally found Clear View Glass and Tint in Phoenix—definitely worth it! auto tint near me
Great job! Discover more at https://blogfreely.net/erwineomen/winter-car-maintenance-checklist-for-buckley-roads-6wsb .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic Aurora expertise
Appreciate your stance on promoting responsible ownership and usage of firearms at fa轮 .
I appreciated this article. For more, visit https://maps.app.goo.gl/3saifxNXsdWm4UMi9 .
Looking for reliable service? Choose Summit Services; they’re consistently rated as the best electricians near me! Electrician
This was highly useful. For more, visit professional syphon repairs .
Thanks for the thorough article. Find more at http://delphi.larsbo.org/user/naydieqnec .
Expressing gratitude extends beyond mere words—we owe thanks especially when acknowledging efforts devoted into ensuring success achieved collectively amongst participants drawn together united under ideals rooted deeply within principles emphasizing tiranga invite code 2757419478643
Have you ever owned an exclusive breed like the Saluki or Borzoi, and how did they in shape into relations existence? https://www.random-bookmarks.win/9-details-for-picking-the-finest-cat-urine-cleanser
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Walter’s BBQ Southern Kitchen location
This was quite enlightening. Check out emergency vet for more.
My last-minute decision paid off when I found @AnyWebsite@ offering fast & efficient #longbeachcartransportation#. So glad I reached out last week! Long Beach car shippers
Having read this I believed it was rather enlightening. I appreciate you finding the time and energy to put this
article together. I once again find myself spending a lot of time both reading and commenting.
But so what, it was still worth it!
The way you explained common issues was super helpful—I can’t wait until I’m able now, finally, after reading this, reach out and hire my nearest ### anykeyword### contractor nearby today! trusted hvac contractors
I appreciated this article. For more, visit professional reliable plumbing .
Every breed has its quirks – what’s one pleasing issue approximately your canine’s personality that invariably makes every person laugh ? Let’s alternate stories over ### anykeyword ### Go to the website
Useful advice! For more, visit phone lookup online free .
Appreciate the helpful advice. For more, visit plumbing services .
I liked this article. For additional info, visit professional syphon repairs .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Pain relief and massage therapy in Aurora
Visiting the right ##kids orthodontist## can make all the difference when it comes to your child’s smile journey. kids orthodontist
Wonderful tips! Find more at Denver sessions for neurofeedback .
I love how 成人自拍 promotes a balanced view on gun rights and responsibilities. Well done!
Great tips! For more, visit private event venue rental .
What a great resource you’ve provided here about bail bonds! Those looking for support should definitely contact ## no money down bail bonds las vegas
This was a great article. Check out https://www.coast-bookmarks.win/the-significance-of-expert-drainpipe-cleaning-and-home-heating-providers for more.
A good relationship with your ###pediatric dentist### is crucial; it fosters trust and encourages lifelong oral health habits in children. kids orthodontist
This was quite informative. For more, visit Commercial Paving Contractor Wheat Ridge .
Thanks for the comprehensive read. Find more at professional power flushing .
Appreciate the comprehensive advice. For more, visit ac replacement company .
Personal injury law can be complex; that’s why finding the right attorney is key—consider visiting Car accident law firm for local leads.
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Vegan brunch options in Pittsburgh
Why people still make use of to read news papers when in this technological globe the
whole thing is accessible on net?
ไฟหน้ารถ LED ราคาแพงไหม? คุ้มค่าหรือไม่? เปลี่ยนไฟหน้ารถยนต์ ใกล้ฉัน
After using several towing companies, I can confidently say that towing service stands out from the rest!
Really appreciate this breakdown, especially with how personal injury claims work in Annapolis, MD. I didn’t realize how important timing is. How do you see this evolving with new insurance laws in MD? Get more clarity here: Slip and fall lawyer .
Don’t let an outdated roof affect the energy efficiency of your home. Carlsbad Roofing Contractor can help you choose and install an energy-efficient roofing solution. certified roof installation
The flavors of South Indian cuisine are so distinct and delicious—have you explored that side of Indian food? indian street food spokane valley
This was quite enlightening. Check out professional reverse number identification for more.
Very useful post. For similar content, visit Sani flo .
Have any original adventures taken place at the same time as traveling with pets ? From highway trips to vacations, let’s change experiences here ### anykeyword ### https://wiki-global.win/index.php/How_Music_Can_Help_Calm_Anxious_Dogs_During_Thunderstorms_55834
This was quite helpful. For more, visit Denver Neurofeedback Services .
I found this very interesting. For more, visit Roofers in Greenville SC .
I appreciate articles like this that educate readers about their rights and options following automobile incidents! georgia car accident lawyer
Thanks for the thorough article. Find more at Walters Barbecue Southern Kitchen .
I’m curious approximately how long installations from ##Hot Water System installations## in Mandurah more commonly take? Affordable Hot Water Systems Mandurah
Appreciate the great suggestions. For more, visit Wheat Ridge Paving Company .
Can’t believe how affordable the repairs were at Mac Repair compared to others in town. ps5 repair
I found this very interesting. For more, visit 24 7 emergency plumber .
If you’re ever in doubt, always consult with an experienced ##anyKeyword# after an accident! motorcycle wreck lawyer
Great blog here! Also your web site so much up fast!
What web host are you using? Can I am getting your associate
hyperlink on your host? I wish my site loaded up as quickly
as yours lol
Visit my site: ซื้อผักสลัดออนไลน์
The diversity of perspectives showcased in your articles makes for an enriching experience when visiting 迷藥 .
Don’t underestimate the value that an experienced #dui lawyer baco raton# brings when navigating these challenging issues; they are invaluable! personal injury attorney
This was beautifully organized. Discover more at Mr. Clean Power Washing, LLC .
Hmm is anyone else encountering problems with the pictures on this blog loading?
I’m trying to find out if its a problem on my end or if it’s the blog.
Any responses would be greatly appreciated. https://vapers.In.ua/proxy.php?link=https://wp.teamlead.pw/question/les-differentes-sortes-de-pelouse-guide-par-choisir-le-gazon-parfait-par-votre-jardin-2/
I found this very interesting. Check out affordable 24 7 plumber for more.
I’m impressed by how you connect historical events with current issues in your posts at 激情妹 .
Nicely done! Discover more at https://maps.app.goo.gl/tcxhzSvHm8wfr9Cr8 .
Does a person recognise if there are any ongoing promotions with ##Affordable Hot Water Systems Mandurah##? Hot Water Systems Mandurah, WA
This was highly informative. Check out Boiler replacement for more.
The kindness of our ##childrens dentists## has taken away all my child’s fears about going to the dentist. childrens dentists
Thank you, public adjusters of Arizona, for the incredible support during my insurance claim! https://www.google.com/maps?cid=13210929340122306639
Navigating braces is much easier with the help of an experienced ###braces dentist### who knows how to handle kids’ needs. braces for kids
This was very enlightening. For more, visit Corgi plumbers .
Love following your web publication since it assists in keeping me excited by conserving no longer best cleanliness but also making improvements to assets worth!!! # # anyK eyword ## https://record-wiki.win/index.php/DIY_Pressure_Washing:_Tips_and_Tricks_for_a_Professional_Finish
Seeking advice from experts at your local ###PediatricDentist### can help address any concerns regarding braces or other treatments. braces dentist near me
I appreciated this article. For more, visit plumbers close to me .
If you’re in search of an empathetic car accident lawyer, take a look at what’s available through Personal injury attorney .
Recently moved to Mission Valley; looking for highly-rated dentists nearby. Sunshine Dental
Wondering how different cultures perceive approaches taken concerning matters relating strictly toward oral hygiene maintenance practices adopted routinely observed periodically across diverse demographics residing along coastal regions overall ?? Excited grace dental
“What should I ask during consultations with potential contractors?” Advosy Roofing and Construction
With havin so much written content do you ever run into any issues of plagorism or copyright infringement?
My blog has a lot of completely unique content I’ve either authored myself or outsourced but it appears
a lot of it is popping it up all over the web without my permission.
Do you know any ways to help protect against content from being ripped off?
I’d really appreciate it.
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic CO therapeutic massage services
I liked this article. For additional info, visit LuxeNeuro .
Love that they have vegetarian options too at Ginger Bistro – something for everyone! chinese near me
Thanks for the valuable insights. More at quick emergency plumbing help .
Thanks for the practical tips. More at Outdoor Event Venue .
If you’re looking for legal advice, start searching for the best local ##personal injury attorney near me## and explore your options! personal injury lawyer
Very informative article. For similar content, visit online reverse phone number lookup .
Appreciate the thorough write-up. Find more at foothills paving and maintenance .
This was beautifully organized. Discover more at complete mommy makeover packages .
Just finished a job with A+ Gutters—they were professional and did a fantastic job on my gutters in St Augustine. gutters near me
Finding clarity amidst chaos often begins simply reaching out towards reliable contacts openly inviting discussions centered around solutions encouraged throughout ### anykeyword# ! car accident attorneys in atlanta ga
Thanks for the clear advice. More at checkatrade approved plumbers .
If you’re in a bind, don’t forget approximately the immediate reinforce from #Emergency Hot Water System upkeep Mandurah#—they are lifesavers! Mandurah Hot Water System service
Appreciate the thorough insights. For more, visit Walter’s BBQ Southern Kitchen .
Exploring options like clear aligners through local experts in ##braces for kids## has been enlightening! kids orthodontist
Thanks for the clear breakdown. More info at sex tre em .
Nicely detailed. Discover more at LuxeNeuro .
I just adore how puppies are such dependable partners! They somewhat make every moment exceptional. Check out https://fair-wiki.win/index.php/Creating_a_Cozy_Sleeping_Space_for_Your_Furry_Friend_11563 for a few appropriate puppy care suggestions!
I love how sleek my car looks after getting tinted at Clear View Glass and Tint! The best choice in Phoenix for sure. auto tint near me
If your child needs orthodontic work, make sure to consult with an experienced braces dentist near me for the best results.
If you’re in Glendale and searching for a dependable electrician, I suggest visiting Electrician Glendale .
Just noticed some ahead of-and-after footage from Mobile Pressure Washing —thoughts-blowing results!
Car accidents can be overwhelming, but having a good car accident attorney can make all the difference. Find one near you through Personal injury law firms .
The stability among aesthetics and performance in inserting cameras is fundamental—I savor you citing it!!! ##anythingKeywords## https://city-wiki.win/index.php/**Tips_for_Testing_and_Adjusting_Mounted_Security_Cameras_After_Installation**
Everyone deserves justice following a vehicle collision; find representation that understands this principle at Atlanta Car accident lawyer #.
I’m planning a move to Haltom City soon. Any advice on the best movers? I found some insights at Haltom City full service movers that might help!
I enjoyed this post. For additional info, visit Walters BBQ Southern Kitchenac .
This is very insightful. Check out payday loans new orleans la for more.
This was very enlightening. For more, visit Foothills Paving .
This was highly educational. More at https://www.deltabookmarks.win/the-benefits-and-drawbacks-of-various-kinds-of-pipes-and-heating-equipments .
Walking my puppy is considered one of my favorite on daily basis workouts! What does yours seem to be? Share data on on foot routines at https://wiki-cable.win/index.php/Preparing_Your_Pet_for_Emergencies:_A_Safety_Checklist !
Summit Services impressed me with their professionalism and expertise. Best electrician around Hilton Head Island! Electrician
Just were given my new warm water technique installed through ##Professional Hot Water Systems Mandurah##. The difference is outstanding! Hot Water Systems in Mandurah
Has anyone used a Palmdale moving company recently? I found some great suggestions at Palm Bay vehicle shippers .
Your commitment to firearm safety education at 白虎阴穴 is commendable! Keep spreading awareness.
Thankful for your insights into wiring safety practices; just wanted to share that if anyone needs an expert they can always find good ones through links like those at Electrical Glendale Arizona
Well done! Discover more at Walters BBQ Southern Kitchen .
คุณสมบัติเด่นของไฟหน้ารถ LED BT PREMIUM คืออะไร ?? ร้าน เปลี่ยน โคม ไฟ หน้า รถยนต์ ใกล้ ฉัน
Thanks for the clear breakdown. More info at https://www.bookmark-friend.win/the-value-of-a-dependable-plumbing-and-heater .
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic Best massage therapy options near me
This was a fantastic read. Check out toilet plumber for more.
I admire how you highlighted the value of getting a pre-flight tick list! It’s whatever every pilot should still keep on with. Discover more sources at https://www.generate-bookmark.win/always-keep-on-with-neighborhood-regulations-and-directions-while-flying-your-drone-camera .
The packing services offered by my #DaytonaBeachMovingCompany# made everything so much easier! Mover And Truck Daytona Beach
Preventing rear-end collisions is something every driver should focus on—arm yourself with knowledge available on this topic through links from car crash attorney !
Thanks for the great tips. Discover more at best mommy makeover clinic .
I’m not that much of a online reader to be honest but your
sites really nice, keep it up! I’ll go ahead and
bookmark your site to come back down the road. Many thanks
This was very enlightening. For more, visit plumber prices .
Excellent coverage of a tricky subject; keep bail bonds las vegas nv
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Brunch Pittsburgh
Had an amazing experience with my recent residential dumpster rental through top-rated dumpster rental orlando —fast and reliable service.
Finding the right representation, like a trusted ##personal injury attorney boca raton##, can significantly impact your case outcome. personal injury attorney near me
ชอบที่ไม่ต้องเปลี่ยนหลอดบ่อยๆ หลังจากใช้ BT PREMIUM มา #BT_PREMIUM## ร้านไฟหน้ารถยนต์ ใกล้ฉัน
ยินดีที่จะได้รับความคิดเห็นจากทุกคนเกี่ยวกับประสบการณ์ที่ผ่านมา ### ร้านไฟหน้ารถยนต์ ใกล้ ฉัน
Wonderful collection of ideas presented here surrounding efficient repairs versus replacements necessary occurring frequently across homes nationally ; likewise locals can see whom specializes around them accessing resources located under Electrician in Glendale Arizona
I had an emergency last week, and the electrician from Electrician Near Me in Glendale was a lifesaver!
What a treasure trove of information ! Individuals residing near glendale searching assistance should definitely consider connecting experts mentioned throughout including # # anyKeyWord # Electrical Contractor Glendale Arizona
Appreciate the comprehensive advice. For more, visit best plumbing .
Just had my windows washed by Sully’s in Winston-Salem, and I’m thrilled with the outcome! Professional and friendly service. Window Cleaning Company
Thanks for providing such helpful content; it’s perfect for residents looking for electrical solutions in Glendale like me who found it through Electrician
I love how you highlighted the importance of hiring local electricians. Check out Electrician Near Me if you’re in Glendale!
True Balance Pain Relief Clinic has the best massage therapist. I always leave feeling rejuvenated and relaxed!
I found the perfect massage therapist near me at True Balance Pain Relief Clinic True Balance Pain Relief Clinic relaxing treatments
Expert opinions matter when determining fault or liability—seek them out through resources offered via ### anykeyword# . car accident attorneys in atlanta ga
Very informative article. For similar content, visit LuxNeuro .
With havin so much content do you ever run into any issues of plagorism or copyright
infringement? My blog has a lot of exclusive content I’ve either authored myself or outsourced but it seems a lot of it is popping it up all over the web without my authorization. Do you know any methods to help reduce content from being
ripped off? I’d really appreciate it.
Thanks for the helpful advice. Discover more at toilet plumbers near me .
Thanks for the insightful write-up. More like this at https://elliotmtme328.fotosdefrases.com/why-regular-oil-changes-in-bonney-lake-can-save-you-thousands-8 .
I just got my car tinted at Clear View Glass and Tint in Phoenix, and the results are fantastic! Highly recommend! auto tint
Starting braces early with the right guidance from experts in ##braces for kids## is such a smart move. braces dentist
Just had my previous scorching water system replaced by way of ##Mandurah Hot Water Systems, WA##, and it works like a attraction now. Hot Water Systems in Mandurah
If you’re facing legal issues and need information about bail bonds in Burlington, NC, understanding what you’ll pay upfront is key. For detailed answers regarding the costs of $1000 or other bonds, check out bails bond near me! bails bond near me
Thanks for the detailed post. Find more at Walters BBQ Southern Kitchenac .
I just hired an electrician from Glendale, and my experience was fantastic! You should check out Electrician Glendale Arizona for more info.
Wonderful tips! Find more at Aestheic Plastic Surgery & Laser Centre .
Excellent insights into how weather changes can impact home safety regarding water damage. Water Damage Restoration
Such a comprehensive guide to electrical services; readers from Arizona might want to bookmark this along with checking out the services offered by Electrical Contractor
Recently had some plumbing work done and was thrilled with the service! Check out commercial plumbing scotts valley for similar results.
Can’t wait explore new chapters unfolding shortly after unraveling twists involved prior engagements discovered along way together collectively navigating challenges faced together daily basis Haltom City full service movers
Walter’s BBQ Southern Kitchen has the best brunch in Pittsburgh. The flavors are incredible!
I love finding a brunch spot near me like Walter’s BBQ Southern Kitchen Pittsburgh brunch takeout
My experience with our local children’s dentist has been fantastic; they truly know how to connect with kids! pediatric dentist
Kudos given towards shedding light onto often overlooked aspects surrounding motor vehicle accidents—it benefits society greatly overall similarly across different demographics too! Atlanta Car accident lawyer
Thanks for the helpful article. More like this at emergency shower installation .
Valuable information! Discover more at passion bagnole .
If you’re searching for quality towing services in Monroe NY, take it from me and choose ## towing service
Wonderful tips! Find more at Walters BBQ Southern Kitchen .
Anyone else love with the aid of their potential washers as an excuse to get pleasure from being open air at the same time getting chores executed?? # # anyK eyword ## https://bitinesdza.livejournal.com/profile/
Wonderful tips! Find more at trusted plumbing line experts .
Looking for ##Mandurah Hot Water System service##? This vicinity has a few of the surest shopper studies on the town! Mandurah Hot Water Systems near me
Finding an understanding #dui lawyer baco raton# made all the difference when dealing with my legal issues; highly recommend seeking out their expertise! personal injury attorney near me
Appreciate the great suggestions. For more, visit LuxNuro .
Great tips on working with insurance claims! Public adjusters really provide that extra layer of support. Select Adjusters LLC
I appreciated this post. Check out https://foro.animeunderground.es/member.php?action=profile&uid=194489 for more.
I found the best deals on local movers in Palmdale through Palmdale full service movers . Highly recommended!
Every participant in the Tiranga games represents hope and aspiration for countless others; it’s inspiring! tiranga invite code 2757419478643
This was a great article. Check out Social Event Venue for more.
Certain partnerships formed evolve organically cultivated gradually establishing solid footing grounded principles underpinning ethos values driven collective vision steering ship navigated turbulent waters experienced adept sailors weathering stormy seas Seville apartment movers
I love these roofing ideas! In Mesa, AZ, there are great contractors who can help bring your vision to life. Best Roofing Contractor Mesa AZ
Dogs have a different method of creating everyday suppose brighter! How does your puppy deliver pleasure into your lifestyles? Tell us on https://speedy-wiki.win/index.php/Traveling_with_Your_Dog:_Tips_for_a_Smooth_Journey !
Great insights! Discover more at Paving and Resurfacing Contractor Wheat Ridge .
Great piece addressing contemporary challenges faced within households today ; communities would do well reaching professionals showcased through sites like # # anyKeyWord # Electrician Near Me
Very helpful read. For similar content, visit plumbing contractors near me .
Thanks for sharing such valuable information; it’s helpful for many homeowners! Check out Electrical Contractor Glendale Arizona if you’re near Glendale!
This was nicely structured. Discover more at Sani-flo .
This was highly educational. For more, visit reliable water leak repairs .
It’s refreshing reading material that educates consumers effectively on best practices ; locals really ought connect with professionals available via # # anyKeyWord # Electrician Near Me
My family and I were thrilled with the professionalism of Summerlin moving companies during our move to Summerlin.
ใครมีภาพติดตั้งไฟหน้ารถ LED BT PREMIUM มาแชร์กันหน่อยครับ ร้าน ตั้งไฟหน้ารถยนต์ ใกล้ ฉัน
ทำไมถึงควรเลือกใช้ไฟหน้าโปรเจคเตอร์แทนหลอด LED ธรรมดา? อ่านได้ที่นี่ครับ ร้านทําไฟรถยนต์ ใกล้ฉัน
A supportive atmosphere at our local ###braces dentist### has helped ease my child’s nerves about treatment. braces dentist near me
The insights from respectable CFO services shall be invaluable. Don’t omit out on what Fractional CFO consulting has to be offering!
Thanks for the great explanation. Find more at Walters Barbecue Southern Kitchen .
The analysis of social media’s influence on public perception of firearms discussed at 性爱图库 was insightful!
It’s hard to find experienced people in this particular subject, but you seem like you know what you’re talking about!
Thanks
Our new ##braces dentist near me### provided us with detailed information on what to expect during treatment – super helpful! pediatric dentist
Kids orthodontists truly understand how to make dental visits fun for children. Have you found a great pediatric dentist nearby?
Appreciate the thorough insights. For more, visit custom home builders dallas .
I love how you highlighted the importance of hiring local electricians. Check out Electrical Contractor if you’re in Glendale!
Clearly presented. Discover more at local same day plumber .
Thank you for providing a platform that encourages responsible discussions about firearms and their use, such as seen on 门按摩 .
This serves as great encouragement reminding victims they’re not alone—they deserve proper representation throughout difficult times ahead always! georgia car accident lawyer
Thanks for the detailed post. Find more at Aesthetic Plastik Surgery and Lazer Center .
I found this very interesting. Check out passion-bagnole.com for more.
Helpful suggestions! For more, visit affordable dishwasher repairs .
Is there a particular breed you’d advise for individual who travels most often yet nonetheless wishes a bushy accomplice? https://www.logo-bookmarks.win/canine-diabetes-is-your-puppy-at-probability
I recently had a great experience with a dentist in San Diego; highly recommend them! Sunshine Dental
I couldn’t believe how painless getting fillings can be—thankful for finding such skilled professionals via #### anyKeyWord ### best SD dentist
Great tips! For more, visit emergency plumber .
If you want authentic flavors and fresh ingredients, Ginger Bistro is the place to go! chinese food
Dogs make first rate training session companions—what health routines contain them ? Let’s inspire each and every other by means of sharing exercise hacks the following ### anykeyword ### Homepage
I’ve been researching cosmetic procedures available through various nearby ### anykeyword#; so much valuable information out there! Dr Todd Brilliant DDS
Just left my appointment at the dentist near me in Oceanside and couldn’t be happier with the care!
After visiting a cosmetic dentistry in North Park, I feel more confident than ever!
มาสำรวจความแตกต่างระหว่างชนิดของหลอดไข่กันเถอะ ร้านเปลี่ยนไฟหน้ารถยนต์ ใกล้ฉัน
Recently, I came across an intriguing article that discusses the importance of selecting the ideal nursery for your children. It’s like a important choice that can have an affect on their interpersonal skills and earlier creation daycare in parsippany
This was quite informative. More at LuxeNeuro .
รออ่านรีวิวจากผู้ใช้คนอื่นๆ ว่าแต่ละรุ่นเป็นอย่างไรกันบ้าง?? ร้านแต่งไฟรถยนต์ ใกล้ ฉัน
Really impressed by how organized my #VehicleShippingAgent# was when handling my shipment at Sinton auto shipping
If you’re near Jacksonville and searching for the best gutter solutions, check out A+ Gutters—you won’t be disappointed! gutters
This was very beneficial. For more, visit commercial plumbing companies .
Efficient monetary making plans starts off with the exact CFO—in finding yours thru Part-time CFO consulting .
I enjoyed this article. Check out Aesthetic Plastik Surgery and Lazer Center for more.
Nicely done! Find more at Foot Hills Paving .
Just had my windows tinted at Clear View Glass and Tint, and it’s made a huge difference in how cool my car stays. Highly recommend! auto tint
This was quite helpful. For more, visit tap maintenance .
I found this very interesting. For more, visit Walters Barbecue Southern Kitchen .
I recently had a fantastic experience with Summit Services! They truly are the best Electrician for all your electrical needs in Hilton Head Island.
Helpful suggestions! For more, visit leaking pipe .
I liked this article. For additional info, visit https://www.seo-bookmarks.win/comprehending-bathroom-flexi-pipeline-use .
Thanks for the thorough analysis. More info at LuxNeuro .
Clearly presented. Discover more at phim sex .
This was a great help. Check out professional dishwasher repair for more.
I’m so grateful we found an efficient and caring ##braces dentist near me## who prioritizes children’s comfort! braces for kids
Hopeful others obtain notion following alongside discussions revolving round suggestions finest winning navigation pathways entering new nation-states surrounding securing satisfactory protections positioned forth easily-obtainable channels promoting Home Insurance Cape Coral
CFO offerings aren’t only for sizable groups! Small corporations can advantage too—investigate out Outsourced CFO solutions .
Top of India serves the best butter chicken I’ve ever had! Don’t miss out, visit spokane valley indian restaurant near me for details.
Really informative content material; it really is clean you’ve got placed lots of concept into making it handy for readers like us! https://wiki-book.win/index.php/Where_Should_You_Point_Your_Security_Cameras%3F_Expert_Insights_12204
This was highly helpful. For more, visit local celebration venue rental .
Appreciate the thorough insights. For more, visit shower drain cleaning services .
Great insights! Find more at foothills paving and maintenance .
I wish more parents knew about the benefits of visiting specialized ###childrens dentists### early on – it makes a world of difference later! pediatric dentist near me
The process of renting a dumpster was seamless thanks to comprehensive waste solutions orlando —highly recommend their services!
Thanks for the helpful article. More like this at https://ronaldinho-gaucho.org/user/eblicidmxo .
Communication was outstanding throughout the process. They responded quickly to my inquiries and kept me updated on scheduling, which I greatly appreciated. window cleaning tampa Tampa Bay Pressure Washing
Such well-written material around an often confusing subject; it’s nice knowing there are resources like no money down bail bonds las vegas
Appreciate having access to 24/7 towing services like those offered by ## towing service
Appreciate the comprehensive advice. For more, visit Walters BBQ Southern Kitchen .
This was a fantastic resource. Check out Auto repair Bonney Lake for more.
Thank you for addressing common misconceptions about firearms on 胡海峰 ! It’s crucial to clear up misinformation.
I enjoy reading about the value of high-quality nursery facilities! It is so important for the development of children in those earlier years. A optimistic surroundings encourages understanding, as well as fostering relationships that will last a life daycare in parsippany
Thank you for addressing the importance of community involvement in discussions about guns at 给你爽 !
Heya i’m for the first time here. I found this board and I find It truly useful
& it helped me out a lot. I hope to provide something again and aid others such as you aided me.
Thanks for the informative content. More at custom home builders near me .
Looking for an improve? Check out the recent types feasible as a result of ##Best Hot Water System providers Mandurah##. Affordable Hot Water Systems Mandurah
Thanks for the informative content. More at WC cistern installation .
This was a wonderful post. Check out top mommy makeover clinics for more.
Explore different ways settlements occur within varying scenarios detailed comprehensively found via ### anykeyword# . atlanta accident claim lawyer
Regular visits to our beloved ###braces dentist### have made all the difference in our family’s oral health journey! kids orthodontist
The beauty behind renovation stories lies within personal narratives woven together through each choice made along that transformative path…!! ### anyKeyWord ## kitchen cabinet remodel Watertown
Meri Sejal is one of the most admired companions at Jaipur Escort Service. Known for her grace, poise, and charming personality, she specialises in offering an elite companionship experience tailored for discerning gentlemen. Whether it’s a social event or a private rendezvous, Pooja delivers elegance, discretion, and unforgettable moments.
Jaipur Escort Service
Thanks for the useful post. More like this at certified plumber .
I fully comprehend the value of locating the ideal daycare for our young children. It can be overwhelming for kids when there are so many selections available daycare
Thank you for sharing such vital assistance approximately ##Hot Water Systems Mandurah close to me##—very informative! Qualified Hot Water Systems plumber Mandurah
This was quite informative. For more, visit emergency drain plumber .
Meri Sejal is one of the most admired companions at Bangalore Escort Service. Known for her grace, poise, and charming personality, she specialises in offering an elite companionship experience tailored for discerning gentlemen. Whether it’s a social event or a private rendezvous, Pooja delivers elegance, discretion, and unforgettable moments.
Bangalore Escort Service
Solid explanation, especially since not everyone in MD knows their rights. That explanation of settlement vs. court was spot on. How does this compare to Baltimore or DC laws? Check out more examples and insights at: Personal injury lawyer .
Meri Sejal is one of the most admired companions at Mumbai Escort Service. Known for her grace, poise, and charming personality, she specialises in offering an elite companionship experience tailored for discerning gentlemen. Whether it’s a social event or a private rendezvous, Pooja delivers elegance, discretion, and unforgettable moments.
Mumbai Escort Service
Appreciate the detailed insights. For more, visit real estate agents near me .
Appreciate the great suggestions. For more, visit LuxNuro .
Thank you for advocating for safe storage practices through your content at 亂倫 !
Thanks for the insightful write-up. More like this at local power flushing experts .
Cheers, I like this.
Take a look at my site; https://r12Imob.store/index.php?page=user&action=pub_profile&id=443723
Need an electrician? Summit Services is the answer! Their team is knowledgeable and friendly, making them the top choice for me. Electrician
This was quite useful. For more, visit affordable 24 7 plumber .
The challenge of capturing motion in still images fascinates me; how do you approach it? Dive into techniques over at western ma photographer !
Appreciate the comprehensive insights. For more, visit mommy makeover transformation .
Valuable information! Find more at Cold water tanks .
I think the admin of this website is genuinely working hard in favor of his web site, for the reason that here every information is quality based material.
ใช้ไฟหน้าโปรเจคเตอร์แล้วรู้สึกมั่นใจในการขับขี่มากขึ้นครับ เปลี่ยน ไฟ หน้า รถ ราคา
This was very enlightening. More at cheap plumbers near me .
Best decision ever was hiring # 1 ! ! . tampa bay pressure washing Tampa Bay Pressure Washing
Thanks for the great information. More at Walters Barbecue Southern Kitchen .
Thanks for the informative content. More at underfloor heating troubleshooting .
Appreciate the insightful article. Find more at LuxNuro .
I appreciate the tips on roof inspections! I’ll make sure to check out accredited roofing professionals for more guidance.
Remodeling isn’t just about aesthetics but embracing practicality alongside creativity intertwined throughout each chosen element/decision made…!!!### anyKeyWord ## kitchen remodeling Watertown
I appreciated this post. Check out reliable plumbing and heating experts for more.
Appreciate the thorough write-up. Find more at roofers fort worth tx .
Great blog here! Also your site loads up very fast!
What web host are you using? Can I get your affiliate link
to your host? I wish my site loaded up as quickly as yours lol http://grindstoneavenue.com/__media__/js/netsoltrademark.php?d=10-day.net%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D1658757
Having someone knowledgeable by your side is crucial during difficult times; consider reaching out via ### anykeyword### . atlanta car accident lawyer
Great blog here! Also your site loads up very fast!
What web host are you using? Can I get your affiliate link to your host?
I wish my site loaded up as quickly as yours lol http://grindstoneavenue.com/__media__/js/netsoltrademark.php?d=10-day.net%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D1658757
The right local connections can lead you to an exceptional ##personal injury attorney boca raton### who truly cares about your case. personal injury lawyer
Hopefully this encourages others continue voicing thoughts shared related towards mutual interests concerning transportation possibilities surfacing amongst discussions promoted earlier spotlighting relevance established linked together focusing primarily Sinton car transport
I liked this article. For additional info, visit Wheat Ridge Driveway Paving .
อยากรู้วิธีติดตั้งไฟหน้ารถ LED ทำเองได้ไหม? ร้านไฟรถยนต์ ใกล้ฉัน
The long-term effects of untreated water damage are scary! Prevention is key. https://www.google.com/maps?cid=2172986856869809528
I wish more people would share their experiences regarding ### no keyword ### St. Augustine commercial movers
If you are having quandary along with your warm water device, do not hesitate to call ##Emergency Hot Water System upkeep Mandurah##—they kept my day! Mandurah Hot Water Systems, WA
Impressed thoroughly witnessing commitment displayed time after time toward ensuring safe delivery without fail-this reflects true dedication exemplified through collective efforts stemming back decades within community itself led primarily thanks those Local movers Melrose
I just read your post about the crucial role of childcare in early childhood enhancement, and I couldn’t believe more! Daycare not only provides a safe haven for kids daycare in parsippany
Wow, this paragraph is good, my younger sister is analyzing these things, so I am going to tell her.
This was a wonderful guide. Check out gutter repair near me for more.
Thanks for the thorough analysis. More info at atlanta movers .
This was a fantastic read. Check out Landlord certificates for more.
Very useful post. For similar content, visit unusual brunch spots in Pittsburgh .
Thanks for the detailed guidance. More at best roofing services company .
I’ve never heard of a dental probiotic before, but it makes sense to focus on balancing the mouth’s bacteria instead of
wiping everything out. Would love to see how ProDentim compares to traditional products!
I’m impressed with the community engagement you encourage at 炸药 . It’s important to foster responsible discussions.
A solid understanding of state laws regarding auto accidents is key; lawyers provide this expertise effortlessly! atlanta car accident lawyers
Exploring options like clear aligners through local experts in ##braces for kids## has been enlightening! pediatric dentist
Gilbert’s summer heat can be tough on cooling systems—make sure yours is ready with timely inspections! Everest Air LLC
This was quite informative. For more, visit front door replacement .
เกร็ดเล็กๆ น้อยๆ เกี่ยวกับการใช้งานและดูแลรักษา?? ร้าน ไฟหน้ารถยนต์ ใกล้ ฉัน
Appreciate the thorough analysis. For more, visit roofing contractors .
“They took care of everything—it was such relief to have an expert public adjuster on my side.” Public Adjuster Arizona
What role does proper drainage play concerning roof longevity? Anyone know? Advosy Roofing and Construction
Just bought my new scorching water technique installed with the aid of ##Professional Hot Water Systems Mandurah##. The difference is super! Mandurah Hot Water Systems experts
This was a fantastic read. Check out price of mommy makeover for more.
หากคุณสนใจเรื่องเทคนิคการขับขี่ปลอดภัย ต้องไม่พลาดเรื่องนี้ ร้าน ตั้งไฟหน้ารถยนต์ ใกล้ ฉัน
Nicely done! Discover more at emergency gas plumber services .
I found this very interesting. For more, visit construction companies .
I enjoyed this post. For additional info, visit window replacement .
When dealing with insurance companies, having an experienced car accident attorney is crucial—explore options at Car accident law firm near me .
Thanks for the useful post. More like this at expert dishwasher repairing .
Thanks for the great tips. Discover more at commercial plumbers near me .
This thought-provoking essay about the importance of choosing the best childcare for your children late struck me. Finding a setting that promotes both learning and social creation is essential daycare near me
I was impressed by the speed of the appliance repair team in Arlington, TX. They were in and out in no time! google.com
Heya just wanted to give you a quick heads up and let youu know
a few of the pictures aren’tloading properly. I’m nnot sure why but I thibk its a linking issue.
I’ve tried it in two different browsers and both show
the same results.
Feel free to surf to my web blog; design and build contractors east london
Anyone else addicted to trail riding? I’ve found so many cool spots via Esterillos horse tours
Efficient economic planning starts off with the desirable CFO—uncover yours thru Chief financial officer services .
Thanks for the practical tips. More at Kitchen remodeler .
Appreciate the thorough information. For more, visit http://kino.online-windows.ru/user/arvicayzci .
This was a fantastic resource. Check out roofing companies for more.
Shoutout to Winter Haven commercial movers for making my recent move so easy and budget-friendly!
Incredible tons of awesome tips!
Visit my web site: https://r12Imob.store/index.php?page=user&action=pub_profile&id=443813
Just wanted to share my experience— towing services 24/7 was incredibly helpful when I needed emergency towing last weekend.
Getting expert advice from a good ##dui lawyer baco raton## can provide clarity during times of uncertainty after legal troubles arise. personal injury lawyer boca raton
such predecessors as Crown of Egypt from igt, they are often called excellent examples of excitement, which is added more
1000 potential ways to hit the jackpot in an https://aztec-megaways.com/de/.
Great insights! Find more at LuxeNeuro .
I recently searched for a dentist near me and found a fantastic option. best SD dentist
Excited upcoming opportunities presented allowing deeper dives exploring unique aspects surrounding individual journeys experienced toward achieving optimal wellness along paths chosen previously ; let’s continue conversations engagingly throughout grace dental oceanside
I had a fantastic experience with A+ Gutters in St Augustine. They know their stuff when it comes to gutters! For details, see gutters near me .
Thanks for the helpful article. More like this at realtor near me .
I love how they explain everything at the best Oceanside Dentist before starting any procedure! dentist near me
Definitely believe that which you stated. Your favorite justification seemed to be
on the net the simplest thing to be aware of. I say to you, I definitely get irked while
people think about worries that they plainly don’t know
about. You managed to hit the nail upon the top and defined out the whole
thing without having side effect , people can take a
signal. Will probably be back to get more. Thanks https://www.forum.breedia.com/proxy.php?link=https://sun-clinic.co.il/he/question/boite-repas-trois-rivieres-une-reponse-incontournable-pour-votre-regime-alimentaire/
Just had my first consultation with a cosmetic dentist at Dr Brilliant DDS , and it went great!
I enjoyed this article. Check out http://penelopetessuti.ru/user/theredznuq for more.
Wonderful tips! Discover more at Walters BBQ Southern Kitchenac .
This was a wonderful post. Check out same day plumber near me for more.
I found this very interesting. Check out Foothills Paving for more.
ไฟหน้ารถ LED BT PREMIUM ทำให้การขับขี่กลางคืนปลอดภัยขึ้นมากเลยครับ ร้านทําไฟรถยนต์ใกล้ฉัน
My patio looks brand new thanks to the incredible work by # # anyKeywords##! home pressure washing near me Tampa Bay Pressure Washing
My friend suggested visiting a dedicated ##pediatric dentist##, and it was the best decision ever! pediatric dentist near me
Investing in high-quality CFO functions is a recreation changer! Discover extra at Chief financial officer services .
Thanks for the insightful write-up. More like this at expert 24 7 plumbing .
First off I would like to say excellent blog!
I had a quick question in which I’d like to ask if you do not mind.
I was interested to find out how you center yourself
and clear your thoughts prior to writing. I have
had trouble clearing my thoughts in getting my ideas out.
I do take pleasure in writing but it just seems like the first 10 to 15 minutes are generally wasted simply just trying to figure
out how to begin. Any suggestions or hints?
Thanks!
If you’re having doubts about whether or not to hire them, trust me; just do it & thank me later!!! # # anykeyword ## commercial plumbing scotts valley
I wish I had sought legal advice sooner after my accident—don’t make the same mistake! Learn from experts at Buckhead Law Saxton Accident Injury Lawyers, P.C. #.
This was a great help. Check out Walters Barbecue Southern Kitchen for more.
Sportsmanship displayed during the Tiranga games teaches us valuable life lessons beyond just winning or losing; it’s about respect and integrity too! tiranga invite code 2757419478643
Many people don’t realize how crucial it is to get legal advice after an accident; visit Personal injury law firms for connections to local experts.
Looking for ##Mandurah Hot Water System service##? This situation has a few of the great client stories on the town! Mandurah Hot Water Systems
I recently discovered a great daycare that certainly comprehends the significance of early youth enhancement. In a secure setting, they provide a range of actions that develop social, psychological, and mental knowledge daycare
Choosing the right ##childrens dentists## is crucial, especially when it comes to creating positive experiences for kids. kids orthodontist
Thanks for the great content. More at Electric showers Power Showers .
Thanks for the clear advice. More at affordable private event spaces .
Your blog is incredibly helpful when it comes to understanding legal terms and processes like these—visit ## bail bonds las vegas nv
Capturing emotions through photography is an incredible skill! I try to do the same at corporate headshots .
Thanks for the insightful write-up. More like this at construction companies .
Great job! Discover more at My Montgomery Vet .
A big shoutout to towing services in Monroe NY for saving me during a tough situation! Their team was prompt and efficient.
If you might be looking for authentic ##Hot Water Systems Mandurah close to me##, you need to suitably examine out their expertise. Top-notch! Hot Water Systems in Mandurah
Thanks for the clear breakdown. More info at Walter’s BBQ Southern Kitchen .
Great job! Find more at gas plumber near me .
อยากได้คำแนะนำเกี่ยวกับการดูแลรักษาไฟหน้ารถ LED ครับ ร้าน แต่ง ไฟรถยนต์ ใกล้ ฉัน
Thanks for the clear advice. More at https://rfserial.net/user/carmaiqpkd .
I enjoyed this read. For more, visit plumbing services near me .
This site definitely has all of the information and facts I
needed concerning this subject and didn’t know who to ask.
I’ve often believed that choosing the best childcare is important for both families and the kids. It’s crucial to make sure our young people are raised in a caring environment that encourages their growth and development daycare
The resources available for understanding firearm accessories are excellent, especially those listed on 炸弹遥控 .
Helpful suggestions! For more, visit Aestheic Plastic Surgery & Laser Centre .
This was a great article. Check out average toilet installation cost for more.
It’s inspiring to see how passionate many ##personal injury attorneys## are about helping their clients get justice and support. personal injury attorney
I found this very interesting. Check out roofing services for more.
I enjoyed this article. Check out Electricians for more.
Sometimes simple changes such as swapping out hardware/fixtures breathe life back into otherwise outdated designs without major renovations necessary…### anyKeyWord ## kitchen remodel cost Watertown
This was very beneficial. For more, visit immediate 24 7 plumbing .
Well done! Find more at emergency clogged toilet repair .
CFO amenities is also the backbone of your economic fitness! Explore what’s accessible at Part-time CFO consulting .
I’m so glad I found Summit Services; they’re absolutely the best when it comes to electrical work in Hilton Head! Electrician
Glad you covered this topic, especially with how vehicle collision issues are processed in our county here in Maryland. Understanding PIP coverage in Maryland was helpful Slip and fall lawyer
Thanks for the informative post. More at LuxNuro .
Thanks for the clear breakdown. More info at air conditioning .
Corpus Christi CoolsSculpting is a safe and effective way to target stubborn fat pockets. authoritative coolsculpting
What’s your go-to appetizer when dining Mexican? Mine has to be queso fundido—so cheesy and delicious! Discover appetizers at restaurant !
CoolSculpting in Amarillo Texas is the go-to treatment for anyone struggling with stubborn fat pockets. accredited coolsculpting services
Our experience with a compassionate ##childrens dentist## has made dental visits fun for my little one! kids orthodontist
Thanks for the great information. More at professional plumbing and heating installation .
Everyone loves it when folks get together and share thoughts.
Great website, continue the good work! https://Wp.teamlead.pw/question/pure-stone-retaining-partitions-a-timeless-and-elegant-solution-for-slope-stability/
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at 制服狩 !
This was very beneficial. For more, visit Aesthetic Plastic Sugery & Lasor Center .
Appreciate the comprehensive advice. For more, visit https://start01.ru/user/joyceylxrf .
It’s nice to know there’s a trustworthy option like Olympia Roofing Company in the area! Roofing Company
Totally agree about the importance of choosing quality materials—Mantecans can find great advice at ###: any keyword## licensed roofing experts
This is such a helpful guide for homeowners! I’ll be sharing it with friends who have septic systems. septic tank pumping
Great job! Discover more at Walter’s BBQ Southern Kitchen .
Braces don’t have to be scary! A knowledgeable braces for kids can help ease your child’s worries and explain the process.
“Choosing the true fiscal companion is obligatory; explore recommendations at Part-time CFO consulting .”
When dealing with personal injuries, it’s vital to have a compassionate and experienced ##personal injury attorney boca raton## by your side. personal injury lawyer
Great job! Find more at Plumbing & heating .
Corpus Christi residents, achieve a more sculpted figure with the help of advanced CoolSculpting treatments available at reliable coolsculpting .
This was quite informative. For more, visit LuxNeuro .
Anyone else feel amazed by the science behind CoolSculpting? Check it out via what’s available on high-quality coolsculpting treatments #.
The convenience of 24-hour towing near me is unbeatable! Glad I found best towing company Monroe for any future needs.
Personal injury cases require skilled representation; find dedicated attorneys at Buckhead Law Saxton Accident Injury Lawyers, P.C. who understand your needs.
Customer-Centric Approach: Throughout the process, they maintained clear communication and actively sought feedback to ensure my satisfaction. This dedication to customer service truly set them apart. exterior house cleaning Tampa Bay Pressure Washing
I appreciated this post. Check out https://daltonlngc652.theglensecret.com/winter-car-maintenance-checklist-for-buckley-roads-6 for more.
Thanks for the valuable insights. More at Walter’s BBQ Southern Kitchen .
The ambiance of a Mexican restaurant really sets the mood for a fun night out with friends or family! Explore local spots at mexican restaurant near me !
Great job! Find more at Swagg Roofing & Siding .
Appreciate the detailed information. For more, visit professional plumbers nearby .
เดิมพันกับไฟหน้ารถ LED คุ้มค่าหรือไม่? ร้าน ทํา ไฟหน้ารถยนต์ ใกล้ ฉัน
This was a great help. Check out emergency clogged toilet repair for more.
Exploring options like clear aligners through local experts in ##braces for kids## has been enlightening! pediatric dentist
The importance of mental health awareness in relation to firearm ownership highlighted on 麻果配 is vital!
For anyone searching for pool screen repair near me, you should absolutely call A+ Gutters—they’re fantastic at what they do! pool screen repair near me
Good information. Lucky me I ran across your blog by accident (stumbleupon).
I’ve saved as a favorite for later!
Just had the most amazing sushi at Ginger Bistro in Palm Coast. It’s definitely my new favorite spot! Sushi St Augustine
Recently, I came across an intriguing essay that discusses the importance of selecting the ideal childcare for your child. How much a boy’s early schooling is influence their development is amazing daycare in parsippany
This was highly educational. More at construction companies .
Thanks for the thorough analysis. Find more at Walters Barbecue Southern Kitchen .
I was particularly impressed with their attention to detail. They took the time to focus on areas that needed extra care, ensuring that every corner of my property was spotless. It’s clear they take pride in their work. tampa bay pressure washing
มีใครแนะนำรุ่นไฟหน้ารถ LED ที่ดีที่สุดบ้างครับ? ไฟ led รถยนต์
Starting dental care early is key! A friendly ####PediatricDentist#### can make all the difference in developing strong habits. pediatric dentist near me
My son just started his journey with braces, thanks to an amazing ##braces dentist## who made him feel at ease. pediatric dentist
Thanks for the practical tips. More at http://flashworlds.ru/user/dewelaapyp .
Useful advice! For more, visit affordable mommy makeover .
Asheville’s landscape is changing beautifully thanks to innovative construction services. https://www.google.com/maps/place/?q=place_id:ChIJWcJBcYaaxkIRwHALPBFcbsU
If you’re looking for fun this summer, check out the amazing water slides available in Tampa! tampa inflatable water slides
Every entrepreneur may still look into CFO services and products; they’re necessary for development! Visit Virtual CFO services nowadays.
Appreciate the insightful article. Find more at https://maps.app.goo.gl/abCzMopPQH8y9tLZ7 .
Glad to see such responsive and friendly teams like those from ## 24 hour towing near me
With Corpus Christi CoolsSculpting, you can finally achieve the body shape you’ve always desired. expert-driven coolsculpting therapy
I’m amazed by how many areas Coolsculpting can treat! Definitely looking into it. Check out competent coolsculpting procedures for more info.
Appreciate the comprehensive advice. For more, visit ac repair service .
I never realized how important it is to have a car accident lawyer until I was in an accident myself. Thanks for sharing this information! georgia car accident lawyer
This was very enlightening. More at LuxNuro .
For anyone searching for reliable gutter solutions, check out A+ Gutters; they’re the best around St Johns County! gutters near me
Never knew how lots dirt might increase until eventually I employed # Pressure Washing Company #—fairly eye-establishing sense!
Is there a dentist in San Diego that offers sedation dentistry? I get really anxious. Sunshine Dental
I had an amazing experience with my local dentist. Highly recommend checking it out! san diego smile makers
Nicely detailed. Discover more at power washing service company .
I’m considering quartz countertops for my remodel—have others had good experiences with them? kitchen renovation costs Watertown
Looking for recommendations for a pediatric surf smiles family dentistry in Oceanside—help please!
Appreciate the thorough insights. For more, visit Walters BBQ Southern Kitchenac .
Great post! I’ve been looking for reliable roofers, and Olympia Roofing Company seems like a fantastic option. Olympia Roofing Contractor
Love seeing so many people sharing their positive experiences after visiting dental professionals nearby—great info on ## north park smile
Great tips! For more, visit hvac contractor nearby .
Want to see how CoolSculpting can reshape your body? Visit credible coolsculpting treatments for breathtaking before and after photos that will leave you in awe.
Valuable information! Discover more at sewer repair near me .
Thank you, asesor fiscal , for making my septic tank maintenance so easy and stress-free!
Thanks for the clear advice. More at wedding florists .
No other electrician compares to Summit Services in Hilton Head Island. They always exceed my expectations! Electrician near me
This was very enlightening. For more, visit kitchen and bathroom taps .
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend What’s the fastest way to get emergency dental care near me?
The presentation of dishes in Mexican cuisine is always so colorful and inviting—definitely eye candy for food lovers like me! Check out beautiful presentations at mexican restaurant !
Just moved to Gilbert and already needed air conditioning repair—what a wake-up call about the heat! Air Conditioning Repair in Gilbert Arizona
Amazing how you’ve merged art with technical skill—it’s what every photographer should strive for, learn from mine here ## senior pictures western ma
The relevance of energy-efficient cooling and heating systems can not be overstated. I rejoice to see even more individuals speaking about it. You can discover additional resources at central air repair milwaukie .
Shoutout to A+ Gutters for their excellent pool screen repair services in Jacksonville—my backyard looks amazing now! lanai screen repair
I appreciated this article. For more, visit affordable central heating installation .
Useful advice! For more, visit https://maps.app.goo.gl/FC9h8zCXQWYyhXDBA .
I found your article on self-defense laws at 伦理大 to be very informative and timely!
Thanks for the great explanation. Find more at affordable drain cleaning near me .
Thanks for the great information. More at Buckley Car Repair Shop .
Visiting the right ##kids orthodontist## can make all the difference when it comes to your child’s smile journey. braces dentist
This is quite enlightening. Check out LuxNeuro for more.
Wow, what a detailed explanation! If anyone needs a bail bond service in Las Vegas, use bail bonds las vegas nv .
There’s nothing worse than a broken refrigerator; I’m grateful for the dependable appliance repair options available here. appliance repair Arlington TX
Well done! Discover more at commercial real estate agent .
Love this information about roofing solutions! Excited to explore options with Olympia Roofing Company soon! Olympia new roof
Thanks for the informative post. More at Walter’s BBQ Southern Kitchen .
Had a wonderful experience with the technicians from Summit Services for my HVAC maintenance – so professional and thorough! Check them out at Air conditioning repair !
Great insights! Find more at water damage restoration companies near me .
Braces can be a big step for kids, so finding the right braces for kids is crucial. What features do you look for in a dentist?
This was beautifully organized. Discover more at vua99 phiên bản mới .
The benefits of a strong social media presence are undeniable—thanks for sharing this info! Explore further strategies at proven marketing agency near me !
A good relationship with your ###pediatric dentist### is crucial; it fosters trust and encourages lifelong oral health habits in children. braces for kids
I found this very interesting. Check out plumbing for more.
I appreciated this post. Check out sample brunch menu Pittsburgh for more.
I was searching for a ##personal injury attorney near me## and stumbled upon some great resources. It’s essential to find someone local who understands the laws! personal injury attorney boca raton
I adore reading about the pleasure and problems of daycare! Finding the ideal nursery can be difficult as a parent. It’s about nurturing and developing beginning expertise in a secure environment, not just about supervision daycare in parsippany
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
If you need reliable electrical services in Bluffton, do yourself a favor and call Summit Services today! Electrician Bluffton
For high-quality gutter services, check out A+ Gutters in Jacksonville! You won’t be disappointed. gutters near me
A big shoutout to towing services near me for saving me during a tough situation! Their team was prompt and efficient.
Choosing the right cabinets can make or break your kitchen remodel. Any tips? contractor for kitchen remodel Watertown
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend Applecross WA emergency dentist
This was a wonderful guide. Check out Buckley Oil Change for more.
Mexican restaurants always have such friendly staff and a warm atmosphere. What’s your go-to order? See more options at restaurant !
I always find valuable information at 东北独立 regarding responsible weapon ownership. Keep it up!
“Professional preparation in finance facilitates businesses thrive; assess out what’s to be had through ###anymKeyWord###!” Chief financial officer services
Just carried out reserving our provider’s transportation wants through fretamento de vans —so easy for our team!
Looking for a non-surgical fat reduction treatment? CoolSculpting in Amarillo Texas is the answer! endorsed coolsculpting
Need delivery recommendations at the same time touring São Paulo? A rented van can more healthy all and sundry comfortably! Learn greater at aluguel de van .
A completely satisfied van rental can remodel your circle of relatives shuttle in São Paulo from annoying to satisfying! Discover choices at aluguel de van são paulo .
This was quite informative. More at bubet số 1 online .
Если заявитель учился в колледже 3
годика, то он сдает экзамены, Гарантированная нострификация аттестата но лишь по профильным.
Thanks for the great information. More at Neurofeedback Sessions Denver .
Appreciate the insightful article. Find more at emergency affordable plumbing .
Don’t overlook the importance of hiring a specialized attorney after an auto incident—learn more at atlanta auto accident attorney !
Thanks for sharing such great advice on roofing care! Looking forward to working with Olympia Roofing Company! Olympia new roof
After my accident, I learned how significant it is to have a dedicated accident lawyer who understands personal injury law.
Very helpful read. For similar content, visit Aesthetic Plastik Surgery and Lazer Center .
My recent visit to a ###med spa newport beach### was everything I hoped for—highly skilled professionals and luxurious treatments! medical spa newport beach
Is there anything more comforting than seeing your child smile after a visit to their favorite ###PediatricDentist###? braces dentist
Candid moments often reveal authentic personalities behind posed expressions—how can we cultivate trust between ourselves & subjects requiring vulnerability before stepping into their world through our lenses? photographer western ma
Corpus Christi CoolsSculpting can help you say goodbye to stubborn belly fat and hello to a flatter tummy. expert coolsculpting services
A good relationship with your ###pediatric dentist### is crucial; it fosters trust and encourages lifelong oral health habits in children. kids orthodontist
Kudos on putting together such an informative piece focused entirely around commercial rooftops within our great city—I truly appreciate all effort put forth! Commercial Roofing in Montgomery IN
I didn’t realize how many factors could affect when I need septic tank pumping done, like household size and usage.
With havin so much content and articles do you ever
run into any problems of plagorism or copyright violation? My website has a lot of unique
content I’ve either created myself or outsourced but it looks
like a lot of it is popping it up all over the web without my
permission. Do you know any ways to help reduce content from being ripped off?
I’d truly appreciate it.
Appreciate the insightful article. Find more at toilet plumber .
“If you’re serious about progress, think of partaking with knowledgeable CFO authorities from Virtual CFO services .”
If you’re looking for affordable yet high-quality fences, check out this Surrey company! Fencing company Surrey CA
I’m always surprised at how much debris gets stuck in my gutters! Regular cleaning is essential—what are your routines like? gutter repair
I’m amazed at how effective CoolSculpting in Amarillo Texas is in reducing unwanted fat! experienced coolsculpting providers
Thanks for the helpful advice. Discover more at roofing contractors near me .
Winter Haven is a beautiful place to set up a business! Make sure to choose the right movers like Cheap movers Winter Haven to help you relocate smoothly.
What a valuable guide on picking the ideal heating and cooling service provider! Correct setup is critical for effectiveness. For even more guidance, have a look at ac repair milwaukie or .
The excitement building up to the Tiranga games is palpable; I can’t wait for it to start! tiranga invite code 2757419478643
The pricing was fair and transparent with no hidden fees, which made me feel confident in choosing them for my pressure washing needs. pressure washing services tampa Tampa Bay Pressure Washing
Great tips! For more, visit LuxeNeuro .
I found this very helpful. For additional info, visit moving companies .
Thanks for the detailed post. Find more at Bathtub resurfacing company .
This was highly useful. For more, visit limited-time brunch deals Pittsburgh .
I’ve seen some of the work done by Olympia Roofing Company, and it’s impressive! Highly recommend them. Olympia Roofing Company
Planning on taking my complete elevated kin round Sao Paolo next month; won’t be able to wait to use ###’s offerings once more!! aluguel de vans
Regaining confidence following traumatic events requires patience support networks established helping facilitate healing processes significantly benefiting individuals particularly showcased thoroughly documented across #### anything#### atlanta accident claim attorney
Our church workforce had an mighty time exploring São Paulo after renting vans from fretamento de van #—widespread service!
Just performed reserving our brand’s transportation necessities simply by fretamento de vans —so convenient for our organization!
If you’re in search of a professional method to move your spouse and children or commercial neighborhood around São Paulo, imagine van apartment answers. aluguel de van são paulo grants widespread alternate options!
This was a fantastic resource. Check out expert heating solutions for more.
This was a wonderful post. Check out https://wiki-fusion.win/index.php/Free_No_Download_Casino_Games_-_Play_Anytime,_Anywhere_65063 for more.
Appreciate the comprehensive advice. For more, visit Winkler Kurtz LLP – Long Island Lawyers .
ข้อเสียของการใช้ไฟหน้ารถ LED คืออะไร? ร้าน ตั้งไฟหน้ารถยนต์ ใกล้ ฉัน
Thanks for the great tips. Discover more at Buckley Car Repair Shop .
This is quite enlightening. Check out houses for sale in las vegas for more.
It’s essential to find someone who specializes in personal injuries, like #personal injury attorney boca raton#, who can guide you through every step of the process. personal injury lawyer boca raton
Can AC repairs be completed in one day? What should I expect? hvac contractor near me HVAC contractor Palm Desert
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend The Applecross Dentist sedation options
I enjoyed this article. Check out quick drain plumber for more.
This thought-provoking post about the joys and problems of childcare encounters recently struck me. Finding a caring environment where their children can learn and develop is therefore crucial for kids daycare
There’s something magical about sharing nachos with friends over drinks—it just makes everything better, doesn’t it?! Explore nacho spots on restaurant near me
This was quite informative. For more, visit Walters BBQ Southern Kitchen .
The affect of neighborhood artists participating with architects enriches our neighborhood—can’t look forward to destiny exhibitions highlighting this fusion!! # # anyKeyWord # expert QuickBooks payroll help
“Living without reliable cooling isn’t something most of us can handle—keep those systems maintained!” google.com
Appreciating ability engage thoughtfully amongst others navigating similar journeys inevitably leads towards collective empowerment deriving strength shared mutually fostering environments conducive towards overall growth sustained consistently throughout endorsed coolsculpting
I really like your blog.. very nice colors & theme.
Did you design this website yourself or did you hire someone to do it
for you? Plz reply as I’m looking to create my own blog and would like to find
out where u got this from. many thanks
I appreciate how professional the roofing contractors are in Mesa, AZ. They took their time to explain everything clearly before starting the job. Advosy Roofing and Construction
This was a great article. Check out Aesthetic Plastic Sugery & Lasor Center for more.
Thanks for the great explanation. More info at Preferred Reglazing .
Braces can be daunting, but knowing we have a great ##braces for kids## provider nearby puts us at ease. pediatric dentist near me
I had no concept that routine filter modifications might improve performance a lot. Many thanks for sharing! If you intend to discover more, see ac repair milwaukie or .
I enjoyed this article. Check out tải ứng dụng bubet for more.
The crew arrived on time and was incredibly friendly. They took the time to explain the entire process and answered all my questions with patience, making me feel confident in their expertise. tampa pressure washing Tampa Bay Pressure Washing
This was very beneficial. For more, visit Buckley Car Repair Shop .
The mix of capability and splendor in ancient architecture is inspiring. How do you believe innovative architects can analyze from it? Share concepts at hearing aids near me .
Thanks for the valuable insights. More at local central heating specialists .
I enjoyed this post. For additional info, visit HVAC Services .
This was a great article. Check out LuxNuro for more.
I love how pediatric dentists create a welcoming atmosphere for little ones! Definitely recommend checking out a local braces for kids .
If you’re in Corpus Christi, don’t miss out on the award-winning CoolSculpting at American Laser Med Spa! professional coolsculpting clinic
We’re grateful for skilled and friendly ##childrens dentists### in our area; they have made dental care fun for our kids! kids orthodontist
If I were to construct a domestic in Austin, I’d positively favor a tradition builder to deliver my imaginative and prescient to life! small business accounting firms near me
Appreciate the comprehensive advice. For more, visit trusted shower installers .
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend The Applecross Dentist insurance acceptance
I found this very helpful. For additional info, visit Aestheic Plastic Surgery & Laser Centre .
Architectural kinds like Baroque and Romanesque have multiple traits which can be captivating! Learn greater approximately their qualities at hearing exams near me .
The convenience of having assorted seats and garage space made our Sao Paolo experience memorable; verify out # # anyKeyWord # # at the moment! aluguel de vans
Tried CoolSculpting in Amarillo Texas and couldn’t be happier with the results! Highly recommend it. high-quality coolsculpting treatments
This was a fantastic read. Check out vet services for more.
We had an significant feel renting a van for our college staff trip in São Paulo! Thanks, aluguel e van sp !
Very impressed by how knowledgeable and helpful everyone at asesoria # is—highly recommend!
If you’re organizing a team-development adventure in São Paulo, recall renting a van for effortless transportation! More facts at aluguel de van são paulo .
I appreciated this post. Check out construction companies for more.
If you might be journeying with young children in São Paulo, renting a van is important! Check out the options at aluguel de van .
Shoutout to everyone working hard at their # anykeyword#(in oceansid#)—you’re appreciated! oceanside dentist
The best decision I made this year was to visit escondido cosmetic dentist for my dental needs!
This was quite informative. For more, visit meeting space with technology .
Love listening to experiences from householders who outfitted with native vendors—their reports deliver big perception into deciding on correctly!! affordable outsourced hr services
Thankful for fast and efficient help from ## towing service
Such well-written material around an often confusing subject; it’s nice knowing there are resources like bail bonds las vegas nv
This thought-provoking post about the value of superior childcare for early youth advancement recently struck me. It’s amazing how a caring culture may help kids develop both social and mental abilities daycare in parsippany
This was a great help. Check out https://orderviag.com//member.php?action=profile&uid=20273 for more.
Nicely done! Find more at DSH Homes and Pools – DFW Custom Home & Pool Builders .
Appreciate the insightful article. Find more at Denver neurofeedback treatment resources .
Hi friends, its enormous paragraph concerning educationand entirely defined, keep it up all the time.
พึ่งซื้อไฟหน้ารถ LED ใหม่มา ใช้แล้วชอบมาก ซ่อมไฟหน้ารถ
Capturing emotions during pivotal life moments is such a rewarding experience; which moment have you captured that holds special meaning for both yourself and those involved, and why does it resonate so deeply with you personally and artistically alike? western ma photography
Thanks for the thorough analysis. Find more at Walter’s BBQ Southern Kitchen .
I’m curious if other parents have had similar experiences with their ###pediatric dentists###—it’s always good to share insights. pediatric dentist
The Tiranga games are such a brilliant way to promote unity and diversity! I can’t wait to learn more about them! tiranga invite code 2757419478643
A tender van condominium can seriously change your circle of relatives vacation in São Paulo from nerve-racking to relaxing! Discover solutions at aluguel de van .
I found this very helpful. For additional info, visit foothills paving and maintenance .
The resources available for understanding firearm accessories are excellent, especially those listed on 要射精了 .
Great insights! Find more at Winkler Kurtz LLP – Long Island Lawyers .
So impressed with the deep cleaning company used by house cleaning service — my home feels fresh again!
This educative article on nursery alternatives was actually helpful to me! It’s for a crucial decision to make when choosing the best daycare for our kids daycare in parsippany
I was impressed by the professionalism of Summit Services as my Electrician near me —they are simply the best!
I love how pediatric dentists create a welcoming atmosphere for little ones! Definitely recommend checking out a local braces dentist near me .
Our community has some amazing ###pediatric dentists### who truly understand how to make children feel safe and secure during visits! braces dentist near me
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
This was very enlightening. For more, visit air conditioning companies Kokomo IN .
After trying multiple treatments, I’ve settled on regular visits to a ###med spa newport beach### for all my skincare needs. lip fillers newport beach
Appreciate the helpful advice. For more, visit Venue Rental .
This was quite useful. For more, visit quick blocked toilet services .
This was very beneficial. For more, visit https://maps.app.goo.gl/NBVABCKQpn46dPUp8 .
Can’t help but wonder if there are common themes regarding challenges faced while navigating personal journeys linked tied closely back around treatment options offered including things like ‘cool-sculpt’ : # anykeyword# ethical coolsculpting
Business organizations seeking to shuttle in São Paulo may want to in fact think of van condominium. It’s cost-powerful and handy! Visit aluguel de vans for greater data.
I’ve been hearing so much about the benefits of IV therapy lately! It’s fascinating how it can boost hydration and overall health. Has anyone here tried it? I would love to know more! Check out this site for more info: springfield IV therapy .
I found this very interesting. For more, visit roofers greenville sc .
Thanks for the great explanation. Find more at Tap washers .
Traveling as a household may also be troublesome, however renting a van makes it a lot more convenient! Find your answer at aluguel e van sp .
Thanks for the comprehensive read. Find more at Buckley Oil Change .
I enjoyed this post. For additional info, visit Sewer line repair near me .
If you’re section of a tremendous group heading to São Paulo, you’ll be able to wish to recall aluguel de van são paulo on your delivery wants.
Renting trucks is such an useful way to tour as a group in busy towns like São Paulo—thank you, fretamento de vans !
For quality HVAC repair services near me, I always turn to Summit Services in Bluffton! They are consistently great! Check their site at ac repair .
Need to transport your physical activities team in São Paulo? Van leases are the optimal solution! Look into aluguel de van .
Need shipping strategies whilst touring São Paulo? A rented van can in good shape all people quite simply! Learn more at fretamento de van .
I highly recommend Tampa Bay Pressure Washing to anyone in need of pressure washing services. Their professionalism, quality of work, and customer service are truly top-notch! commercial pressure washing
I enjoyed this read. For more, visit https://trello.com/c/QFFB70nh/14644-blast-a-perfect-finish-painting-m18-w3 .
These common a/c issues are so relatable! I’ve encountered a couple of myself. If anyone requires aid, I suggest taking a look at milwaukie ac service for remedies.
If you’re thinking about installing new gutters, don’t forget to check out reviews on local ##Gutter Installers## first. gutters repair near me
I appreciated this article. For more, visit Pittsburgh brunch places .
Wondering if any fencing companies in Surrey provide free estimates? That would be super helpful! Fortress Fencing Inc
If your garage door is acting up, don’t hesitate to call the Garage Door Company in Houma LA—they’re lifesavers! google.com
Its such as you read my thoughts! You appear to understand so much approximately this, such as you wrote the e book in it or something.
I believe that you can do with some percent to pressure the message home a
little bit, but instead of that, that is fantastic blog.
A great read. I’ll certainly be back.
Thanks for the clear breakdown. More info at Power Washing Bel Air .
For anyone searching for reliable car towing services, look no further than towing service !
Thanks for the great tips. Discover more at Aesthetic Plastic Sugery & Lasor Center .
The staff at American Laser Med Spa – Amarillo made me feel so comfortable during my treatment. Check out reliable coolsculpting !
I appreciated this post. Check out foothills paving and maintenance for more.
Can’t thank house cleaning enough for assisting me preserve a tidy and orderly home.
Thanks for the insightful write-up. More like this at Burst pipe .
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend The Applecross Dentist emergency tooth extraction
If you want quality service from an electrician near you, go with Summit Services in Bluffton! Electrician
Appreciate the useful tips. For more, visit Power Washing .
This was very well put together. Discover more at reliable drain cleaning services .
I believe self-advocacy is crucial when it comes to our health, especially regarding something as vital as our ability to hear—get tested regularly everyone! hearing test
Well done! Discover more at mold remediation .
Thanks for the valuable article. More at link tải vua99 nhanh .
Your analysis of online vs. brick-and-mortar sales at 淫亂 provided great clarity on current trends.
Anyone else find aid from rigidity with the aid of chiropractic care? Excited to proportion reports through pediatric chiropractor near me .
What’s the best way to maintain an asphalt surface once it’s sealed? Looking for advice from an expert asphalt parking lot installation #.
Thanks for the useful suggestions. Discover more at affordable emergency plumbers .
The role of calibration in clinical apparatus is not going to be disregarded. Companies like load cell calibration near me ensure that we get it proper!
This was a great help. Check out Buckley Car Repair Shop for more.
It’s amazing how much detail goes into producing quality content in a professional video recording studio. https://www.google.com/maps/place/?q=place_id:ChIJzWucoD6pK4cRKc7uL4PUr18
I appreciated this article. For more, visit roofers Bozeman MT .
মোবাইল WinBetWin অফিশিয়াল site lives
in St. Pete Beach, Florida, at the docks at 647 East Denmark Beach Boulevard.
CoolSculpting has become the go-to fat reduction treatment in Amarillo, and endorsed coolsculpting is your trusted source for this cutting-edge technology.
This was quite informative. For more, visit Blocked toilet .
Recently, I came across an article on the importance of selecting the ideal daycare for our young children. It is crucial for their growth to find a nurturing environment that encourages learning and social connection daycare in parsippany
I lately had my HVAC system serviced, and the distinction is amazing! It deserves the financial investment. For experienced suggestions, head over to best ac repair milwaukie .
Thanks for the informative content. More at moving companies near me .
Thanks for the detailed post. Find more at Aesthetic Plastic Sugery & Lasor Center .
Is there anything better than freshly squeezed lime juice over your meal?! It adds an extra zing; see how to use lime creatively on restaurant
Witnessing firsthand transformations going on at some point of neighborhoods motivates me daily whereas dreaming sizeable along others!!! # # anyKeyWord # comprehensive outsourced hr services
The interviews with industry experts featured on 干穴 are a fantastic addition to the discussion.
This was a great article. Check out Sani flo for more.
I had no idea that routine filter modifications could enhance efficiency a lot. Many thanks for sharing! If you want to find out more, browse through milwaukie ac service .
Highly Recommend: I can’t recommend Tampa Bay Pressure Washing enough! If you’re looking for a reliable and effective pressure washing service in the area, look no further than these amazing professionals. You won’t be disappointed! residential pressure washing
Getting advice from peers led us to find an outstanding ###pediatric dentist near me### who truly cares about kids! kids orthodontist
Excellent way of explaining, and fastidious post to obtain facts regarding my presentation topic, which i am going to present in school.
We are a group of volunteers and opening a new
scheme in our community. Your site provided us with useful information to work
on. You have done an impressive task and our
whole community will be grateful to you. https://acecontrol.biz/link.php?u=https://sun-Clinic.co.il/he/question/boite-repas-trois-rivieres-une-reponse-incontournable-pour-votre-regime-alimentaire/
New York’s mental health resources are top-notch! Thanks to mental health new york , I discovered a fantastic psychiatrist.
We are a group of volunteers and opening a new scheme
in our community. Your site provided us with useful information to work on. You have done an impressive task
and our whole community will be grateful to you. https://acecontrol.biz/link.php?u=https://sun-Clinic.co.il/he/question/boite-repas-trois-rivieres-une-reponse-incontournable-pour-votre-regime-alimentaire/
Fantastic advice on addressing water damage! Prevention is key, and your article highlights that well. Bloque Restoration
This was very beneficial. For more, visit https://online-wiki.win/index.php/Foxwoods_Resort_And_Casino .
สนใจจะเปลี่ยนเป็นระบบไฟหน้าใหม่ ต้องดูตรงไหนบ้าง?? ไฟฟ้ารถยนต์ ใกล้ฉัน
Thanks for the useful post. More like this at construction companies .
พูดถึงเคล็ดลับในการปรับแต่งระบบแสงเพื่อเพิ่มความสวยงาม ### ตั้งไฟหน้ารถยนต์
I’ve heard that chiropractors can help with migraines. Can an individual percentage their fulfillment stories or insights from pregnancy chiropractor near me ?
Thanks for sharing these tips! I think one of the best ways to find a plumber in Pembroke Pines is by asking friends and family for recommendations. Online reviews also help a lot best plumbers near me
Have you ever had an issue through lack of calibration? It’s not easy! Let flow meter calibration near me guide you avoid that.
A amazing article about the value of excellent daycare for premature childhood development recently struck me. It’s incredible how a child’s societal knowledge and mental well-being may be shaped by a nurturing culture daycare in parsippany
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend How much does The Applecross Dentist charge for an emergency visit?
The storytelling aspect of your photos resonates deeply with me; I’d love to tell stories through mine as well, visit me over at headshots near me !
“Reach out and find out how much more you could receive through professional adjusting!” https://www.google.com/maps?cid=13210929340122306639
I highly recommend checking out local ###childrens dentists### if you’re looking for someone specializing in pediatric care! childrens dentists
If you’re organizing a crew-development experience in São Paulo, concentrate on renting a van for handy transportation! More info at aluguel de vans .
Can anyone recommend eco-friendly roofing options available through contractors in Mesa? Advosy Roofing and Construction
Planning an match in São Paulo? Renting trucks can simplify transportation logistics to your neighborhood—extra data on aluguel e van sp !
Thanks for the clear breakdown. Find more at sewer repair company .
I’m so glad I came upon ###whilst planning my travels thru Sao Paolo – they somewhat understand how offer ideally suited providers!! fretamento de vans
Van leases are top for bother-loose delivery in bustling São Paulo! Check out what aluguel de van são paulo has to offer.
I admire how old architecture mostly harmonizes with nature, growing captivating landscapes! Explore this relationship similarly at hearing exams near me .
Great job! Discover more at wedding florists near me .
Simply had my very first cleaning with house cleaning , and I’m already preparing my next appointment!
This was very beneficial. For more, visit http://hondaikmciledug.co.id/HRIS/member.php?action=profile&uid=206690 .
This is very insightful. Check out foothills paving and maintenance for more.
If you are organizing a crew-construction tournament in São Paulo, remember renting a van for convenient transportation! More files at aluguel de van .
CoolSculpting Corpus Christi provides a safe and effective way to sculpt your body. Discover the power of approved coolsculpting clinic and achieve your aesthetic goals.
This is very insightful. Check out Washing-machine repairs for more.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
I liked this article. For additional info, visit commercial plumbing specialists .
The information on roof maintenance is invaluable for businesses in Montgomery IN. Commercial Roofing in Montgomery IN
“Always happy to support local businesses—especially those involved with our community’s growth!” Construction Services in Asheville
Thanks to towing services in Monroe NY for always being there when I need help with my car! Their reliability is second to none.
This was beautifully organized. Discover more at https://andytywm520.timeforchangecounselling.com/what-to-do-when-your-check-engine-light-comes-on-in-bonney-lake-18 .
I liked this article. For additional info, visit competitive plumber prices .
It’s outstanding how a few old systems have endured centuries even as others have crumbled—what aspects make a contribution to this resilience? Learn extra at free hearing test .
This was very beneficial. For more, visit Bonney Lake Car Repair Shop .
Ready to achieve your body goals without surgery or downtime? CoolSculpting is the answer! Discover the exceptional results on professional coolsculpting clinic and take the first step towards a confident new you.
I’ve tried several cleaning services, however none compare to the quality of work from house cleaning services Bay Area .
Great insights! Find more at vua99 ứng dụng .
I always thought IV therapy was just for hospitals, but now I see how accessible it is for wellness! I’m eager to learn about the different formulas available. More details can be found at iv therapy .
Anyone else find it challenging to discuss their hearing issues with family? Regular testing might help start that conversation! hearing test near me
I enjoyed this read. For more, visit construction companies .
This was highly educational. For more, visit Best Option Restoration of South Charlotte .
Our new ##braces dentist near me### provided us with detailed information on what to expect during treatment – super helpful! braces dentist
How do you choose between different options when looking for braces? Consulting with a trusted ###PediatricDentist### is always helpful! braces dentist near me
Well done! Find more at http://www.charitiesbuyinggroup.com/MemberSearch.aspx?Returnurl=https://www.mediafire.com/file/0wdk0nlg9vlu5i6/pdf-74669-57087.pdf/file .
When dealing with personal injuries, finding an empathetic and skilled accident lawyer near me should be one of your top priorities.
I’ve had a titanic revel in with chiropractic medication! I chanced on precious tools at walk in chiropractor near me .
If you’re in Bluffton and need electrical repairs, I suggest contacting Summit Services—they’re the best! Electrician
I had such an amazing experience with my chemical peel at a ##med spa newport beach##! My skin feels so refreshed. medical spa near me
I love how easy it is to find qualified psychiatrists in New York using psychiatrist new york ; it really simplifies the process.
Calibration prone can keep establishments funds by way of stopping highly-priced blunders. Visit onsite calibration to be trained extra!
Does any one have advice for opting for the excellent customized abode builder in Austin? I’d get pleasure from any advice! affordable outsourced hr services
Nicely detailed. Discover more at https://drrajeshgastro.com/myforum/member.php?action=profile&uid=108615 .
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at 天黯门 !
I had no idea about the differences in bail across states! Glad I found bail bondsman las vegas nv for Las Vegas specifics.
Pretty! This was an extremely wonderful article. Thank you for
supplying this info.
I had no concept that routine filter adjustments can enhance efficiency a lot. Many thanks for sharing! If you want to learn more, browse through air con repair .
This was a great help. Check out Bonney Lake Car Repair Shop for more.
It’s hard to find good service these days, but asesor fiscal really delivers on their promises!
It’s great to see more places offering free or low-cost hearing tests in our community—let’s take advantage of that! free hearing test for seniors near me
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend Cosmetic dentistry specialists near me
Evans made certain every inch of glass sparkled—it feels refreshing having clean perspectives to come back!!!!## Window Cleaning Company
พึ่งซื้อไฟหน้ารถ LED ใหม่มา ใช้แล้วชอบมาก ร้านไฟรถยนต์ ใกล้ฉัน
Well done! Discover more at plumbers in the area .
After visiting a local Dr Brilliant DDS , I’ve noticed such an improvement in my overall dental health!
Love seeing so many people sharing their positive experiences after visiting dental professionals nearby—great info on ## north park smile
I’m considering IV therapy for my chronic fatigue. I’ve read that it can help replenish vitamins and minerals effectively. What do you all think? I found some great resources here: springfield IV therapy .
Choosing the properly calibration service can make all the big difference; check out what electronic calibration has to present!
This was a wonderful guide. Check out reliable plumbing and heating experts for more.
Architectural patterns like Baroque and Romanesque have varied qualities which are appealing! Learn greater approximately their traits at ear test near me .
Nicely done! Discover more at Foothills Paving .
CoolSculpting Corpus Christi can help you achieve the body you’ve always wanted. Say goodbye to stubborn fat with the help of ethical coolsculpting .
Appreciate the insightful article. Find more at plumber charges .
Hey there just wanted to give you a quick heads up. The text in your article seem to
be running off the screen in Chrome. I’m not sure if this is a format issue or something
to do with internet browser compatibility but I thought I’d post to let
you know. The layout look great though! Hope you get the issue solved soon. Thanks
I’m constantly impressed by just how much time I save using house cleaning near me for my house cleaning needs.
This article is spot on! Regular servicing can prevent costly air conditioning repairs down the line. Everest Air LLC
I’ve noticed that many New Yorkers are talking about mindfulness and its benefits for mental health lately. Great resources can be found at psychiatrist new york .
Stunning architecture shot here; architectural photography fascinates me as well—explore some of my favorite buildings over at: senior pictures western ma !
These typical cooling and heating problems are so relatable! I’ve faced a few myself. If anyone needs assistance, I recommend having a look at milwaukie air conditioning service for services.
ยินดีที่จะได้รับความคิดเห็นจากทุกคนเกี่ยวกับประสบการณ์ที่ผ่านมา ### ไฟฟ้ารถยนต์ ใกล้ฉัน
I know this if off topic but I’m looking into starting my
own blog and was wondering what all is required
to get set up? I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% certain. Any tips or
advice would be greatly appreciated. Kudos
Have you ever tried therapy with a psychiatrist? I found mine through psychiatrist new york , and it was life-changing!
Well explained. Discover more at emergency drain cleaning service .
Very informative post; I’ll refer returned to this whenever I fresh my sidewalk relocating ahead—thank you lower back! https://echo-wiki.win/index.php/How_Often_Should_You_Pressure_Wash_Your_Concrete_Sidewalk%3F
This was a great article. Check out Kitchen plumbing for more.
Lip fillers have become my favorite beauty treatment, especially after finding an amazing place at a ##medical spa near me##! medical spa newport beach
คุณสมบัติเด่นของไฟหน้ารถ LED BT PREMIUM คืออะไร ?? ร้านเปลี่ยนหลอดไฟรถยนต์ ใกล้ฉัน
Appreciate the helpful advice. For more, visit Foothills Paving .
Don’t waste your time looking elsewhere; just call Summit Services for any AC repair or service needs—you’ll be glad you did! ac service
This was very enlightening. For more, visit 24 hour plumber .
Looking for state-of-the-art CoolSculpting clinics in Corpus Christi? Discover top-rated coolsculpting provider for exceptional services and remarkable results.
Having trouble deciding between different types of materials for new gutters… Any suggestions from those who’ve been through it? gutters repair near me
If you need a skilled Electrician , I highly suggest reaching out to Summit Services. They are fantastic!
The mix of capability and magnificence in historical architecture is inspiring. How do you believe cutting-edge architects can be taught from it? Share ideas at hear aids .
After visiting several clinics, we finally found an excellent ##braces dentist near me## who truly knows how to work with children! braces dentist near me
Taco Tuesday should be a national holiday! Can’t wait to hit up my favorite spot. Find more great options at restaurant !
Do you suspect chiropractic care is price it in the long run? Would love critiques shared on chiropractor near me !
Coolsculpting is a game-changer for body contouring! I love how non-invasive it is. Check out more at dependable coolsculpting .
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend The Applecross Dentist teeth whitening
Taking facet in charity runs/hobbies aiding corporations assisting omitted animals inspires involvement quite with no query–Which causes resonate strongest personally motivating buyers looking opportunities mixed FUN & WORK simultaneously finished?? https://direct-wiki.win/index.php/Preparing_Your_Pet_for_Emergencies:_A_Safety_Checklist_55881
Great job! Find more at http://polishcrazyclan.ugu.pl/member.php?action=profile&uid=344502 .
Shoutout to the fantastic team at house cleaning services for constantly exceeding and beyond!
This was a wonderful guide. Check out atlanta movers for more.
If you have concerns about your child’s teeth, consulting with local ###childrens dentists### can provide peace of mind and solutions. braces dentist near me
The comfort of renting a van in São Paulo is unequalled—just right for households and enterprise corporations alike! More important points at aluguel de vans .
Thanks for the comprehensive read. Find more at plumbing line restoration .
If you are organizing a group-construction experience in São Paulo, factor in renting a van for easy transportation! More information at aluguel e van sp .
Wonderful tips! Find more at Sewer line replacement .
Hearing tests are so important for maintaining overall health. Have you had yours recently? ear test near me
Every weekend i used to pay a quick visit this web page,
as i wish for enjoyment, as this this web site
conations genuinely pleasant funny data too.
Highly advocate utilising trucks for transporting increased communities round Sao Paolo; inspect out what’s attainable at fretamento de vans !
This was very beneficial. For more, visit construction companies .
Maіn gгatis tɑpi hasil mantap.
Renting vehicles is such an successful method to commute as a gaggle in busy cities like São Paulo—thank you, fretamento de van !
Great job! Discover more at average plumber prices .
Don’t waste time with other contractors – go with Summit Services for your AC repair needs in Bluffton! You won’t regret it; check them out at ac repair !
Families vacationing São Paulo can make the such a lot of their ride via renting a van. Check out the prone at aluguel de van !
What’s up colleagues, its great paragraph regarding teachingand fully explained, keep it up all
the time.
Review my webpage – ผักไฮโดรโปนิกส์
I’ve heard mixed studies about chiropractic care—curious to work out what mavens say on chiropractic treatment .
What is the top-rated time of 12 months to get CoolSculpting achieved at experienced coolsculpting providers ?
The connection between top knowledge and efficient outcomes is indisputable – thanks, onsite calibration , on your preparation!
I never knew septic tank pumping could impact my home’s health so much! Thanks for the insights! septic tank pumping
Your tips on making certain real air flow even as running vigour washers was exceedingly necessary—thanks for sharing!! # # anyK eyword ## https://speakerdeck.com/account/edit
IV therapy seems like a fantastic option for busy professionals who need a quick health boost! I’m looking forward to trying it out soon. Anyone want to share their experiences? Check this site for further insights: springfield IV therapy .
I’m always encouraging my friends to get regular hearing tests; they can be life-changing! hearing test
I had a fantastic experience with Summit Services! They’re the top choice for electricians in Bluffton. Electrician Bluffton
Appreciate the detailed insights. For more, visit commercial plumbing companies .
I enjoyed reading about the innovations in weapon technology discussed at 騷浪 . Exciting times ahead!
This was very beneficial. For more, visit http://2ch-ranking.net/redirect.php?url=https://go.bubbl.us/ec175f/14d8?/Bookmarks .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Valuable information! Discover more at https://wool-wiki.win/index.php/Necessities_A_Casino_Party .
Thanks for the insightful write-up. More like this at Burst pipe .
Useful advice! For more, visit Foothills Paving .
Achieve your desired body shape with CoolSculpting near me in Corpus Christi. Trust ethical coolsculpting to deliver outstanding results and excellent patient care.
Great job! Discover more at https://maps.app.goo.gl/xLsvXLeSbZgrQD5T7 .
We’re grateful for skilled and friendly ##childrens dentists### in our area; they have made dental care fun for our kids! braces dentist
I recently found a great psychiatrist in New York through psychiatrist new york and it has made such a difference in my life!
Appreciate the thorough analysis. For more, visit https://maps.app.goo.gl/CcdRHUVnx7Q5ZAMd9 .
Ancient cities have been masterfully designed, reflecting communal residing; what instructions can we take for smooth urban planning? Explore ideas at hearing exams .
I lately used a van apartment for a relatives time out in São Paulo, and it made everything so much more uncomplicated! Check out aluguel de vans for quality offers.
I’m thrilled to see how many young talents emerge during events like these—kudos to everyone involved in organizing them, especially the Tiranga games team! tiranga invite code 2757419478643
A professional personal injury attorney not only assists with legal matters but also provides emotional support during challenging times.
Calibration seriously is not simply precious; it can be valuable! Glad to work out organizations like torque screwdriver calibration taking fee of this primary subject.
I’ve used Summit Services multiple times as my Electrician near me , and they’ve never let me down!
I found this very interesting. For more, visit atlanta moving companies .
I have actually been utilizing house cleaning services for months now, and I can’t envision going back to cleaning myself!
I love my lip fillers! The team at the ##med spa newport beach## made the process super comfortable and easy. medical spa newport beach
Great insights! Find more at https://pl.grepolis.com/start/redirect?url=https://atavi.com/share/xcpvs3z1c6fre .
For households travelling São Paulo, renting a van can prevent time and money. Highly put forward trying out fretamento de vans for your transportation necessities!
I found this very interesting. For more, visit plumbing leak detection .
If you’re webhosting friends soon, don’t forget about growing that most suitable ambiance with lovely presentation of your orange county-prompted charcuterie setup shared here: charcuterie !
Thanks for the thorough article. Find more at https://maps.app.goo.gl/rj3tMayFPYHSL1Ep8 .
This was a fantastic read. Check out construction companies for more.
Has anyone ever tried DIY gutter repair? I’m curious but leaning towards hiring professionals instead—especially local ##New Gutters## experts. gutters companies near me
Thanks for the useful suggestions. Discover more at emergency same day plumber .
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend Applecross dental hygienist
Thanks for the insightful write-up. More like this at https://maps.app.goo.gl/7Ghpc7V2RqWmMuhHA .
The significance of energy-efficient HVAC systems can not be overstated. I’m glad to see even more individuals discussing it. You can locate extra sources at air conditioner tune up milwaukie .
Ready to reveal a more contoured physique? CoolSculpting Corpus Christi can help you achieve your goals! Learn more about top-rated coolsculpting provider and start your transformation journey.
With flu season approaching, I’m thinking about using IV therapy to boost my immune system. Has anyone tried immune-boosting drips? I’d love to hear your stories! For more information, visit iv therapy springfield .
This was highly educational. For more, visit Foot Hills Paving .
This was highly educational. More at professional plumbing .
Thanks for the clear advice. More at https://maps.app.goo.gl/p2rzCAEVGYTF9bme7 .
Mental health matters! If you’re in NYC, consider using psychiatrist new york to connect with a supportive psychiatrist.
Solid explanation, especially since local Annapolis laws differ from other areas. That explanation of settlement vs. court was spot on. Have you seen local attorneys handle this differently? For anyone curious, you can learn more here: Personal injury lawyer Blank Kim Injury Lawyer .
Your travel shots inspire wanderlust within me—they tell stories beyond words, making them even more special—come travel with me through images over on my site: headshots western ma !
The allure of antique cities with their historical structures is unrivaled! What are your well-known historic websites? Discuss them at hear aids .
I appreciated this post. Check out game thưởng bubet for more.
Thanks for the informative post. More at emergency plumber near me .
Just got domestic from my #hearingaidtest#, and I’m humming with new files! Thank you, hearing aids near me
If you might be going through chronic suffering, indisputably assess out the benefits of chiropractic offerings on pediatric chiropractor near me .
This is very insightful. Check out https://maps.app.goo.gl/VfZrCLmNP1GDPnfUA for more.
Just wanted to express how delighted I am with the arise from using house cleaning ‘s services.
Helpful suggestions! For more, visit a plumber .
My audiologist recommended annual hearing tests after age 50, and I think that’s sound advice! ear aids near me
Great post! I’ve been wondering about the costs involved in repairing my sliding patio door. It’s good to know that common issues can often be fixed without breaking the bank sliding door fix Cincinnati
The appeal of historic towns with their historic constructions is unrivaled! What are your favourite old sites? Discuss them at historic architect .
“From personal experience, having an AZ Public Adjuster turned my chaotic claims process around.” google.com
Thanks for the great explanation. More info at https://usellbuybid.com/user/profile/3310952 .
Kudos to Summit Services for their outstanding AC repair work in Bluffton—my unit is running perfectly now! ac service
The role of social media in shaping our perceptions of mental health is fascinating, especially among New Yorkers! Dive deeper into this topic at psychiatrist new york .
“I had no idea about the variety of roofs available until speaking with pros!” Roofing Contractor Mesa AZ
I’m impressed, I have to admit. Rarely do I come across a blog
that’s equally educative and amusing, and without a doubt, you’ve hit the nail on the head.
The problem is something which too few people are speaking intelligently about.
I am very happy I came across this in my hunt
for something concerning this.
My recent chemical peel left my skin glowing! So glad I chose this ##med spa## for my treatment. med spa near me
Very informative post! If you’re looking for reliable bail bonds in Las Vegas, visit no money down bail bonds las vegas .
Just commenced seeing a chiropractor and I’m feeling more suitable already! Thanks, chiropractic doctor , for the preparation!
So grateful having connections established throughout community who specialize areas related directly towards resolving everyday nuisances caused malfunctioning items often taken granted until stop working altogether unexpectedly ! Best appliance repair in Arlington TX
Calibration is valuable for making sure accuracy in measurements. A dependableremember instrument calibration near me can assist agencies sustain prime principles.
Just joined a home improvement forum and saw numerous discussions about finding reputable local ###gutter repair companies###—it’s been helpful! gutters companies near me
I enjoyed reading about the innovations in weapon technology discussed at 胡錦濤 . Exciting times ahead!
Great job! Find more at trusted blocked toilet specialists .
For anyone seeking reliable HVAC repair in Hilton Head Island, Summit Services is the way to go! Their team is professional and efficient. More details at hvac service near me .
Wow, this article is good, my sister is analyzing these things, therefore
I am going to inform her. https://Wiki.Roboco.co/index.php/Lave-auto_%C3%83_La_Main_%C3%83_Blainville_:_Un_Bonne_S%C3%83_lection_Pour_L%C3%A2%E2%82%AC%E2%84%A2entretien_De_Votre_Voiture
Appreciate the great suggestions. For more, visit toilet clog fix .
I’ve been attempting out different well being treatment plans and discovered chiropractic functions absolutely exciting—more facts mandatory from chiropractor !
The Applecross Dentist saw me immediately when I had unbearable tooth pain, their emergency service is truly exceptional!
I’m so grateful to have found an emergency dentist near me like The Applecross Dentist, they saved my weekend The Applecross Dentist reviews
What’s the so much lively dog breed you’ve encountered? I need a training session pal! https://www.stealth-bookmark.win/horse-trailer-buyer-tips-slant-load-vs-straight-load
Well done! Find more at Buckley Oil Change .
I just recently had my HVAC system serviced, and the difference is unbelievable! It deserves the financial investment. For professional ideas, head over to ac repair near milwaukie .
With flu season approaching, I’m thinking about using IV therapy to boost my immune system. Has anyone tried immune-boosting drips? I’d love to hear your stories! For more information, visit iv therapy springfield mo .
Anyone else have success stories from psychiatrists they found through psychiatrist new york ? I’d love to hear them!
I’m not sure exactly why but this website is loading very slow for
me. Is anyone else having this issue or is it a problem on my end?
I’ll check back later on and see if the problem still exists.
The presentation of dishes in Mexican cuisine is always so colorful and inviting—definitely eye candy for food lovers like me! Check out beautiful presentations at mexican restaurant !
Thanks for the great explanation. Find more at best rated plumbers near me .
Business organizations seeking to trip in São Paulo should always certainly think about van condominium. It’s money-triumphant and handy! Visit aluguel e van sp for more info.
I appreciate this information on preventative care—I’ll be booking my next hearing test soon! Thanks! hearing exams
Highly recommend asesoria Almeria if you want reliable and efficient septic tank pumping!
Thanks for the thorough analysis. More info at https://speedy-wiki.win/index.php/Take_An_Experiment_Run_Within_Online_Casino .
Knowing where one can seek further assistance makes navigating this entire journey less daunting & overwhelming; grateful towards those working tirelessly behind scenes @ keyword#! dependable coolsculpting
I currently used a van rental provider in São Paulo for a spouse and children reunion, and it became supreme! Highly put forward trying out fretamento de vans for nontoxic providers.
Thanks for the helpful article. More like this at Professional Paving Contractor Wheat Ridge .
This was nicely structured. Discover more at reliable blocked drain services .
Mình thấy nhà cái dv88 đang thu hút nhiều người chơi, có ai có ý kiến gì không? Chia sẻ thêm tại https://dv88.red để cùng thảo luận nhé!
Hệ thống hỗ trợ khách hàng của Rikbet rất tốt, mình đã nhận được sự giúp đỡ kịp thời khi cần. Tìm hiểu thêm tại rikbet nhé!
Các bạn có thể giới thiệu cho mình một số mẹo chơi cá cược trên vz99 không? Mong chờ những chia sẻ hữu ích! vz99 xn
The discussion around hunting rights and regulations at 操他妈 is informative and well-articulated.
Chúc mừng fb68 vì đã mang đến cho người chơi 68k khởi đầu thuận lợi! link fb68
The use of regional material in ancient architecture showcases the ingenuity of earlier builders! Explore this conception extra at hearing test .
We all need reminders that it’s okay not to be okay, especially in a city as demanding as New York. Let’s support each other; find resources at psychiatrist new york .
I’m because vacationing a chiropractor however have some reservations. Would like to get some clarity from arthritis chiropractor .
I found this very interesting. For more, visit 24 hour plumber near me .
Bet168 thật sự là một trang tuyệt vời để xem kèo nhà cái. Mình đã theo dõi nhiều trận đấu qua đó. Nếu bạn cần thêm thông tin, hãy ghé thăm https://Bet168xn.com nhé!
This was highly educational. More at atlanta movers .
I’m impressed by means of the extent of detail and care from the staff at onsite calibration for the period of their calibration techniques.
For anyone in St. Augustine who loves good food, definitely check out Paladar Cuban Eatery & Bakery – it’s a treasure trove of flavors! cuban restaurant near me
Do yourself a favor and work with house cleaning service for your next deep clean; it deserves every cent!
Just lower back from a go back and forth to São Paulo in which we rented a van from aluguel de van são paulo —pretty advocate this provider!
Renting trucks is main when traveling as section of enormous trade teams or families; do not miss checking what’s a possibility on # # anyKeyWord # # ! fretamento de van
Appreciate the thorough insights. For more, visit quick plumber response .
Tired of endless crunches and not seeing the desired results? CoolSculpting might be the solution you’ve been waiting for. Explore the stunning before and after photos on professional coolsculpting clinic to find out.
We all need reminders that it’s okay not to be okay, especially in a city as demanding as New York. Let’s support each other; find resources at psychiatrist new york .
We had such an unforgettable loved ones vacation in São Paulo made even improved with our apartment from aluguel de van !
My family and friends all agree that Summit Services is our favorite electrician near me on Hilton Head Island—excellent work every time! Electrician
Wow this is really insightful information; it’s hard finding good electricians sometimes but I’ve seen positive reviews about those at Electrician Near Me
This was very insightful. Check out Tap washers for more.
This was quite informative. More at construction companies .
Wow , I’m impressed , this blog has some amazing information . Just as a heads up ; folks living nearby might also want see who offers services over at # # anyKeyWord # Electrician
This was very enlightening. For more, visit bubet cổng giải trí .
Incredible compilation showcasing diverse experiences shared surrounding common obstacles faced repeatedly encouraging positive dialogue promoting growth collectively focused achieving milestones reached through collaboration prioritizing transparency Electrician Glendale
So many good points raised here ! As part of preventive maintenance , it’s wise connecting with experts like those over at # # anyKeyWord # Electrician Near Me
Nicely done! Discover more at Foot Hills Paving .
Excellent blog here! Additionally your website quite
a bit up fast! What web host are you using? Can I am getting your associate hyperlink to your host?
I wish my web site loaded up as fast as yours lol
If you haven’t tried the artisanal meats and cheeses from Orange County’s charcuterie scene, you’re missing out! Discover more at charcuterie orange county .
Thanks for the valuable article. More at 24 7 emergency plumber .
It’s important to consult with a qualified accident lawyer to understand your rights and options following a personal injury.
Sometimes all you need is a good bowl of tortilla soup to warm your soul—what’s your comfort food?! Learn about it on restaurant near me
What’s the average cost of installing a fence with companies in Surrey? Just trying to budget. Best Fence contractor in Surrey CA
I had no idea that regular filter changes could improve effectiveness a lot. Thanks for sharing! If you wish to find out more, check out best ac repair milwaukie .
Great job! Discover more at trusted commercial plumbers nearby .
Learn approximately the diverse different types of calibration products and services awarded with the aid of gurus like the ones at accredited calibration services !
Cleaning up can be such a task. I like how house cleaning service takes the stress out of it!
Wonderful collection of ideas presented here surrounding efficient repairs versus replacements necessary occurring frequently across homes nationally ; likewise locals can see whom specializes around them accessing resources located under Electrician Glendale Arizona
Thanks for highlighting these issues ; locals facing similar challenges should connect with skilled individuals available through # # anyKeyWord # Electrical Contractor
I’ve read that chiropractors can toughen athletic efficiency—excited by learning greater through chiropractic treatment .
It’s great to see a reliable garage door company thriving in Houma, LA! google.com
The difference proper gutters make during heavy rainfall is incredible! Make sure you hire qualified ##Gutter Repair Companies##. gutters repair near me
Thanks for the clear breakdown. More info at Burst pipe .
It’s great to see more places offering free or low-cost hearing tests in our community—let’s take advantage of that! free hearing test for seniors near me
Appreciate the detailed post. Find more at http://kakaku.com/jump/?url=https://go.bubbl.us/ec175f/14d8?/Bookmarks .
Loving the community support around CoolSculpting experiences shared on reliable coolsculpting !
This portrait has such depth and character—it’s easy to see why portraiture is so compelling—I’m crafting some portraits too, join me: western ma photographer
I found your comparisons between different weapon types very eye-opening, particularly those featured at 李鹏 .
I value your insights on indoor air high quality! It’s something a number of us ignore. For further reading, visit air conditioning repair milwaukie to find out more.
This was very enlightening. More at emergency blocked toilet fix .
Thanks for the comprehensive read. Find more at atlanta moving companies .
I’m really interested in setting up my own video recording studio. Any tips? video recording studio
Excellent points made here about the signs that your septic tank needs pumping! septic tank pumping
Awesome article full of practical advice on hiring electricians; locals might find what they need at Electrical Contractor Glendale Arizona
I had an emergency last week, and the electrician from Electrician Near Me in Glendale was a lifesaver!
Looking for a non-invasive fat reduction treatment? CoolSculpting Corpus Christi is your answer! Discover the amazing results with top-rated coolsculpting provider .
Has all and sundry attempted chiropractic care for sporting events injuries? I’d love a few guidance from chiropractic treatment .
I found this very interesting. Check out construction companies for more.
Thanks for the valuable insights. More at https://www.golf-bookmarks.win/the-advantages-of-hiring-an-expert-plumbing-professional-and-heating-specialist .
Thanks for the helpful advice. Discover more at checkatrade plumbers .
What a treasure trove of information ! Individuals residing near glendale searching assistance should definitely consider connecting experts mentioned throughout including # # anyKeyWord # Electrician
The service from Summit Services was outstanding when I needed AC repair. Very professional team! Visit hvac service near me for more information.
It’s important to consult with a qualified personal injury attorney to understand your rights and options following a personal injury.
For any electrical issues, I always trust Summit Services to deliver top-notch service as an electrician in Hilton Head Island! Electrician
Calibration plays a widespread position in compliance and rules; have faith providers like dimensional calibration services to remain on appropriate of it.
I’ve heard that chiropractors can support with migraines. Can anybody share their achievement reports or insights from pediatric chiropractor near me ?
Considering lip fillers? Definitely check out reviews of your nearby ###medical spas### for recommendations! medical spa near me
Fantastic insights into residential wiring; if you’re based in Glendale and need help contact the pros at Electrician Near Me
This was a fantastic resource. Check out emergency kitchen plumbing for more.
“The level of detail that Public Adjusters provide when assessing damages is remarkable; they’re truly invaluable!” Select Adjusters LLC
I comprehend how thorough the ear aids near me hearing assist try out course of was once—suitably worthy it.
Being portion of regional rescue efforts ensures a number of lives kept day to day – Is volunteering some thing near adequate FOR YOU also desirous about serving to others? https://wiki-club.win/index.php/Understanding_the_Canine_Sense_of_Smell:_How_It_Works
This was a fantastic read. Check out Residential Paving Contractor Wheat Ridge for more.
Finally found a reliable service for gutter repair nearby, and they really took care of everything efficiently—so grateful! gutters companies near me
Appreciate the comprehensive advice. For more, visit local plumbing solutions .
Thanks for sharing such valuable information; it’s helpful for many homeowners! Check out Electrician Glendale Arizona if you’re near Glendale!
This was very beneficial. For more, visit Buckley Car Repair Shop .
Great article! I found an amazing electrician through Electrical Contractor right here in Glendale.
Appreciate the detailed information. For more, visit ac replacement Peru .
Appreciate the helpful advice. For more, visit i need a plumber .
Historical structure now not solely represents aesthetic good looks yet also technological developments of its time! Explore this duality at architecture firm .
Just had my windows cleaned up by the experts at house cleaning services Bay Area — what a distinction it makes!
Great tips! For more, visit floral decor for wedding .
Do you may have any concepts for cleaning algae off roofs with a power washing machine? Need a few expert information! https://mag-wiki.win/index.php/Getting_Creative:_Unique_Projects_You_Can_Tackle_with_a_Pressure_Washer
The atmosphere at Paladar Cuban Eatery & Bakery is fantastic. Great place to enjoy authentic Cuban cuisine! cuban restaurant
Your tips are spot on! For any electrical work needed in Glendale, Arizona, visit Electrician Glendale .
The fusion of flavors in a good pozole is truly comforting—I could eat it year-round, especially during chilly nights; find pozole recipes on restaurant
Appreciate the comprehensive advice. For more, visit Pumps .
Appreciate the thorough analysis. For more, visit Roofing .
Regularly calibrating accessories saves time and sources; let nist calibration certificate exhibit you ways!
It’s fascinating to see the evolution of construction techniques being used in Asheville today. google.com
If you’re planning on exploring all that São Paulo has to be offering with your relatives, give some thought to renting from aluguel de vans .
If you are vacationing as section of a business team, don’t underestimate the magnitude of renting a van; look at various out options at aluguel e van sp !
The staff at experienced coolsculpting providers made my CoolSculpting experience so comfortable and enjoyable!
Thanks for the clear breakdown. More info at Foot Hills Paving .
This was very beneficial. For more, visit http://www.canmaking.info/forum/user-1658786.html .
This was quite enlightening. Check out local roofers near me for more.
Great tips! For more, visit Sewer line repair company .
This was a fantastic read. Check out need a plumber for more.
Traveling as a own family may well be tough, yet renting a van makes it quite a bit less difficult! Find your resolution at fretamento de vans .
Thanks for the detailed guidance. More at vua99 tài xỉu dễ chơi .
I found this very interesting. For more, visit Power Washing Near me .
Truly grateful that somebody took the day out of their day in order that we may profit from their potential!!!!!! ## https://mag-wiki.win/index.php/Revitalize_Your_Curb_Appeal:_How_to_Clean_Concrete_Sidewalks_Like_a_Pro
Just had my ##AC## serviced by Summit Services, and I couldn’t be happier! Highly recommend them for any ##HVAC## needs! hvac service near me
This was beautifully organized. Discover more at Powell’s Plumbing, LLC .
This was quite useful. For more, visit trusted WC cistern repair .
Just got my carpets cleaned up by house cleaning services , and they look brand name brand-new again!
Very informative article. For similar content, visit air conditioning maintenance near me .
This was a wonderful guide. Check out Sewer line replacement expert for more.
Manufactured homes really do offer excellent value; loved finding mine through # New manufactured homes for sale #!
Thanks for the clear breakdown. Find more at vet .
Great content! If you ever find yourself needing a bail bond in Las Vegas, check out bail bonds las vegas near me .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Anyone be aware of if there are any offers on CoolSculpting right now at certified coolsculpting specialists ?
This was very enlightening. For more, visit http://www.bookmerken.de/?url=https://www.4shared.com/s/flxbI1Makku .
Thanks for the great tips. Discover more at https://maps.app.goo.gl/nySybRpAJLYuogy46 .
I had no clue that driving sizzling water could beautify the effectiveness of my cleansing; thank you for that tip!! https://page-wiki.win/index.php/Eco-Friendly_Pressure_Washing:_How_to_Clean_Without_Harm
A liable calibration business is worthy; investigate what ### anyKeyWord### grants at present! torque screwdriver calibration
I’ve study that chiropractors can upgrade athletic efficiency—desirous about mastering extra using chiropractic doctor .
Thanks for the thorough article. Find more at ac repair service .
Thanks for the detailed guidance. More at Power Washing .
Just had the most delicious meal at Paladar Cuban Eatery & Bakery! If you love ##Cuban restaurants##, this one is a gem in St. Augustine. cuban bakery near me
I recently used a van rental for a circle of relatives vacation in São Paulo, and it made every little thing most more easy! Check out fretamento de van for staggering deals.
Thanks for the great tips. Discover more at Open Wide La Jolla Dentist .
A compassionate accident lawyer near me can help alleviate some of the stress associated with managing an accident claim.
Our latest family members reunion in Sao Paolo was awesome seeing that we had ample room with our rented van; visit # # anyKeyWord # # for booking tips! aluguel de van são paulo
This was highly educational. For more, visit Climate-Alignment .
Anyone else love getting pampered at their favorite ##medical spa near me##? It’s such a treat! medical spa near me
A friend mentioned an app that helps track your hearing health—has anyone else tried something similar? Curious if they’re effective! hearing exams
Great job! Find more at WC cistern installation .
If you’re organizing a staff-construction tournament in São Paulo, take into account renting a van for easy transportation! More information at aluguel de van .
I love how you highlighted the importance of hiring local electricians. Check out Electrician Glendale if you’re in Glendale!
This blog post truly highlights the advantages of routine heating and cooling exams! It can save money in the long run. For more pointers, head to best ac repair milwaukie .
What’s better than a well-made chili relleno?! That cheese-filled goodness gets me every time; see chili relleno versions on restaurant
Thanks for the helpful article. More like this at tải bubet trên di động .
Thanks for the detailed post. Find more at My Montgomery Vet .
Just finished reading up on common gutter problems; it’s fascinating how something so small can have such a big impact on our homes! gutters repair near me
This was very well put together. Discover more at Sani flo .
Impressed by the comprehensive support offered by Sacramento personal injury lawyers. Their dedication to achieving justice for clients is truly commendable! sacramento truck accident lawyer
Never knew getting a septic pump could be this easy until we tried # # anyKeyWord # # – highly recommended! asesoria Almeria
The legacy left behind after witnessing incredible displays showcasing determination among fellow competitors serves as motivation fueling aspirations further enhancing community bonds created throughout experiences encountered surrounding platforms akin tiranga invite code 2757419478643
Thanks for the insightful write-up. More like this at construction companies .
Impressed by the expertise and dedication of ** police misconduct lawyer ** when it comes to personal injury cases in Fresno. Their commitment to fighting for justice shines through their work ethic!
Thanks for the great tips. Discover more at wedding florists Long Island NY .
Thanks for the valuable insights. More at affordable heating solutions .
Impressed with the insightful advice on personal injury cases shared here. It’s crucial to have a reliable team of san diego car accident lawyer by your side in San Diego for legal support!
“Had an emergency situation with my dryer; thankfully I found an amazing technician right here in Arlington!” https://www.google.com/maps?cid=6678422040132912182
If you’re unsure which garage door to choose, consult with the experts at the Garage Door Company in Houma LA—they’ll guide you right! American Garage Doors
Great job! Discover more at a plumber .
This was very enlightening. More at Open Wide La Jola Dentistry .
Fantastic post! Discover more at affordable commercial fridge services .
Calibration amenities can store agencies cash by means of stopping high-priced error. Visit plug gage calibration to be informed extra!
The expertise of Los Angeles personal injury lawyers can make a real difference in seeking justice and compensation. If you’re looking for top-notch legal assistance, be sure to check out los angeles motorcycle accident lawyer for support tailored to your needs!
Awesome article! Discover more at Powell’s Plumbing, LLC5 .
Considering the significance of legal support, getting in touch with portland injury lawyer could make a real difference. Portland personal injury lawyers play a vital role in advocating for justice and aiding those in need.
Thanks for the thorough article. Find more at plumbing & heating near me .
Hearing tests are quick and easy; there’s really no excuse not to get one done regularly! hearing exams near me
The importance of energy-efficient heating and cooling systems can not be overstated. I rejoice to see more individuals talking about it. You can find extra resources at ductless ac repair milwaukie .
I love learning new techniques men and women existing their food; seeing artistic twists on typical dishes across alternative cultures always inspires me—and I’m diving into that around orange county true now because of this link : # # anyKeyWord # # ! charcuterie orange county
If you’ve been injured, finding a reliable personal injury attorney near me nearby can provide the support you need to move forward.
Thanks for the informative content. More at professional plumber pricing .
I admire how you tackle controversial topics with sensitivity and depth on 江澤民 .
Lip filler consultations are so helpful! I learned so much during my visit to the ###medical spa newport beach### before making my decision. medical spa newport beach
Thanks for the thorough analysis. Find more at Underfloor heating repairs .
Great article! It’s always helpful to know the potential costs associated with heat pump repairs. Regular maintenance can definitely save on those unexpected expenses heat pump repair companies in Middlefield Connecticut
Thanks for the valuable article. More at hvac contractor near me .
This was a wonderful guide. Check out foothills paving and maintenance for more.
Historical bridges aas a rule bring experiences of innovation and engineering prowess—what’s your well-liked one? Discuss it at hearing aids for tinnitus .
This was highly helpful. For more, visit local flood restoration near me .
I found this very interesting. Check out Buckley Oil Change for more.
I read this post completely about the comparison of most
recent and preceding technologies, it’s remarkable article.
Great tips! For more, visit vua99 tài xỉu dễ chơi .
This was very well put together. Discover more at trusted toilet clearing services .
Can any individual give an explanation for the transformations between chiropractors and physical therapists? Hoping for insights due to backpain chiropractor !
Solid content that resonates with each person worried approximately making improvements to security measures inside of their properties!!! ###anythingKeywords ## https://wiki-site.win/index.php/Camera_Coverage_Explained:_Analyzing_the_Best_Views_for_Safety_11148
Thanks for the useful suggestions. Discover more at water damage restoration .
I enjoyed this article. Check out movers near me for more.
This was a great article. Check out https://www.bookmarkidea.win/handling-a-stinky-shower-drain-3 for more.
The flan at Paladar Cuban Eatery & Bakery is to die for! Such a great end to a meal of delicious Cuban cuisine! cuban food st augustine
Great job! Find more at plumbing line restoration .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
The neighborhood wineries in Orange County provide super pairings with their charcuterie forums! It’s a pleasing sense for a person who loves desirable foodstuff and wine. Explore more treatments at charcuterie board .
Your tips are spot on! For any electrical work needed in Glendale, Arizona, visit Electrician Glendale .
Natural supplements for nerve pain always catch my attention. If
Arialief can help with sciatic pain and support healing, it could be
a game-changer for a lot of people.
Did you understand that puppies can guide lower pressure phases greatly? What calming ideas do you employ with yours? Talk about it over at https://wiki-aero.win/index.php/Travel_Safety_Tips_for_Dogs_on_Airplanes_and_Trains_30490 !
Every visit to a Mexican restaurant feels like a mini vacation with all the vibrant colors and lively atmosphere—what’s your favorite part? Dive into experiences at mexican restaurant !
I enjoyed this post. For additional info, visit trusted heating repairs .
This article has certainly motivated me to take action regarding my aging roof. google.com
Every breed has its own wonderful trends and desires. Which breed do you believe you studied is the first-rate match for a loved ones? Share thoughts at https://wiki-byte.win/index.php/Adventures_in_Canine_Agility_Training:_A_Beginner%E2%80%99s_Journey_58695 !
I like the focus on sustainable a/c services! It’s excellent to see business leading the fee. Discover much more environment-friendly choices at central air repair milwaukie .
They use safe products that are terrific for my kids; thank you, house cleaning services !
This was quite informative. For more, visit Open Wide La Jola Dentistry .
If you are making plans a loved ones holiday to São Paulo, renting a van is a huge shipping solution! Check out aluguel de vans for the most interesting alternatives obtainable!
Thanks for the informative content. More at plumber prices .
Valuable information! Find more at ClimateAlign .
Valuable information! Find more at tải phiên bản bubet .
Thanks for the useful post. More like this at Buckley Oil Change .
Planning on taking my overall expanded spouse and children round Sao Paolo next month; can’t wait to take advantage of ###’s prone lower back!! fretamento de vans
Can anyone provide an explanation for how chiropractic alterations paintings? I’m eager to have in mind bigger through chiropractor near me .
Appreciate the detailed post. Find more at same day plumber .
I’ve always wondered what happens during the pumping process. This post clarified it for me! septic tank pumping
The historical context you provided about gun legislation at 法正乾 really added depth to the conversation.
The peace of mind that includes realizing your resources are calibrated correctly is invaluable. Thanks, accredited calibration services !
Thanks for the helpful article. More like this at plumbing services .
I recently took a hearing test and was amazed by how simple the process was. Everyone should do it! hearing exams near me
I recently visited Paladar Cuban Eatery & Bakery in St Augustine, and their Cuban sandwich is to die for! cuban restaurant near me
Great customer service paired with even higher results—that’s what Evens provides at any time when!!!!## Window Cleaning Service
Great post! I’m looking forward to exploring more about your video recording studio’s offerings. video recording studio
This was quite helpful. For more, visit Open Wide La Jola Dentistry .
I enjoyed this post. For additional info, visit affordable plumbing .
If you’re dealing with the consequences of an accident, seeking advice from a nearby personal injury attorney could be your best step forward.
Thanks for the helpful article. More like this at foothills paving and maintenance .
The benefits of chemical peels are real! I’m glad I found such an amazing place at a ##medical spa near me##. med spa newport beach
Very informative article. For similar content, visit ClimateAlign .
“Safety first! Always ensure your chosen contractor follows protocols.” Advosy Roofing and Construction
Thanks for the valuable insights. More at clogged toilet solutions .
Excellent writing showcasing importance prioritizing safety while managing household appliances effectively ; individuals wishing follow-up should access directories leading towards # # anyKeyWord# Electrician Glendale
” I appreciate your detailed explanation regarding different materials affected by moisture and their treatment.” https://www.google.com/maps?cid=2172986856869809528
This is very insightful. Check out same day plumbing repairs for more.
Finally found a reliable service for gutter repair nearby, and they really took care of everything efficiently—so grateful! gutters companies near me
I love the vibrant atmosphere at Mexican restaurants! They always have the best decor. Check out mexican restaurant for some amazing restaurant ideas!
“Thankful that I found such quick service when I needed urgent repairs last month—Gilbert has great HVAC pros!” Best Air Conditioning Repair in Gilbert Arizona
Can a chiropractor help with anxiousness? Curious to pay attention thoughts from chiropractic doctor .
If you’re looking to expand your machinery’s functionality, a good calibration carrier is vital. Check out torque screwdriver calibration for extra details.
Our sports activities team came across the perfect rental using ###/ — it was once spacious sufficient for all our tools too! fretamento de van
I’ve been wanting out special wellbeing therapies and came across chiropractic companies easily exciting—greater data vital from chiropractic treatment !
This is quite enlightening. Check out reliable plumbing for more.
We had such an effortless time getting around São Paulo by renting a van from aluguel de vans —most likely suggest it!
I used to be thrilled with the carrier we gained from our rented van company for the time of our fresh commute to São Paulo—consult with aluguel de van são paulo for yours!
It’s inspiring to see so many families finding their forever homes with help from # Affordable manufactured homes for sale #!
The function of calibration in scientific methods shouldn’t be ignored. Companies like hardness tester calibration be sure we get it proper!
I love how ordinary it really is to hire a van for domestic outings in São Paulo! For the fantastic deals, assess out aluguel de van .
Well done! Find more at Foothills Paving .
Very useful post. For similar content, visit plumbers .
Great advice on balancing air flow in homes! For expert help, check out san diego hvac company .
Appreciate the detailed insights. For more, visit Pumps .
Wow, I didn’t realize how complex bail could be! Glad I found cheap bail bonds las vegas for help in Las Vegas.
A compassionate accident lawyer can help alleviate some of the stress associated with managing an accident claim.
Appreciate the useful tips. For more, visit professional blocked toilet services .
The complex designs determined in Gothic cathedrals are in simple terms breathtaking. They fairly mirror the artistry of their time. Learn more at hearing aids for tinnitus .
Thanks for the comprehensive read. Find more at movers atlanta .
Considering lip fillers? Definitely check out reviews of your nearby ###medical spas### for recommendations! medical spa newport beach
These common a/c issues are so relatable! I have actually faced a few myself. If any individual needs aid, I suggest looking into a/c repair for services.
Hey There. I found your blog using msn. This is a really
well written article. I’ll be sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I will definitely comeback.
I’m trying to find organic affliction reduction choices and heard approximately chiropractic products and services from car accident chiropractor .
Thanks for the great information. More at Buckley Oil Change .
The peace of intellect that incorporates realizing your contraptions are calibrated accurately is helpful. Thanks, onsite calibration !
This was a great article. Check out washing machine repair services for more.
The excitement building up to the Tiranga games is palpable; I can’t wait for it to start! tiranga invite code 2757419478643
After hearing horror stories, I’m committed to researching only the best local gutter repair companies before choosing one. gutter repair
This was a fantastic read. Check out DSH Homes and Pools – DFW Custom Home & Pool Builders for more.
Thanks for the clear breakdown. More info at Open Wide La Jola Dentistry .
I think this is one oof the most important information for me.
And i am glad reading your article. But wanna remark on feww general things, The site style is
perfect, the articles is really excellent : D. Good job, cheers
Heree is my web page;aracımın değeri
I appreciated this post. Check out quick plumber costs for more.
This was quite informative. For more, visit expert refrigeration repair services .
This was very beneficial. For more, visit https://www.novabookmarks.win/just-how-to-avoid-pipes-and-home-heating-troubles-in-your-vacation-home .
If you’re near St. Augustine, don’t miss out on Paladar Cuban Eatery & Bakery – their cafe con leche is amazing! cuban restaurant st augustine
The ear aids near me listening to resource try made me detect how superb this is to deal with listening to worries early on.
This was quite helpful. For more, visit https://maps.app.goo.gl/2humZaRYewcxgE5w9 .
Great job! Discover more at https://www.adirs-bookmarks.win/exactly-how-to-preserve-your-hot-water-heater-and-heater .
Thanks for the great explanation. More info at Tài nguyên bổ sung .
Friendly staff and great service make all the difference! Thank you, asesor fiscal almeria #.
Thanks for the valuable article. More at ac replacement .
It’s great to see more discussions on electrical safety! For those in Glendale, check out Electrician Glendale !
I’m impressed by how you connect historical events with current issues in your posts at 共残主义 .
This was very enlightening. More at affordable cosmetic dentist .
Historical architecture as a rule serves as a backdrop for worthy cultural routine—what parties have you ever attended in old venues? Share studies at architecture firms near me .
This is highly informative. Check out plumbing line for more.
This is very insightful. Check out https://maps.app.goo.gl/7CBvCUS8HgH6JZPV9 for more.
Mexican street food is simply amazing! Have you ever tried elote? Find more street food ideas at mexican restaurant !
This was very enlightening. For more, visit Paving Contractor Wheat Ridge .
Appreciate the thorough insights. For more, visit emergency reliable plumbing .
Appreciate the detailed post. Find more at professional industrial refrigeration maintenance .
This was a great help. Check out interior painting for more.
The effect of appropriate calibration on product excellent is terrific – thanks, multimeter calibration near me , for highlighting this!
Wonderful tips! Find more at Bonney Lake Car Repair Shop .
These usual cooling and heating concerns are so relatable! I’ve faced a couple of myself. If anyone needs help, I suggest having a look at hvac repair milwaukie or for services.
Van leases are suitable for families who choose to create lasting reminiscences even as vacationing by means of gorgeous São Paulo—seek advice from aluguel de vans !
This is very insightful. Check out moving companies atlanta for more.
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Thanks for the thorough article. Find more at affordable plumbing and heating services .
Such an important discussion! For anyone facing legal issues in Las Vegas, look into 24 hour bail bonds las vegas .
It’s the best time to make some plans for the future and it’s time
to be happy. I’ve read this post and if I may just I desire to suggest you some fascinating issues or advice.
Perhaps you can write next articles relating to this article.
I desire to learn even more issues approximately it! http://innerforce.co.kr/index.php?mid=board_vUuI82&document_srl=2379952
Nicely done! Find more at Roofing .
I love how you incorporate historical perspectives into modern discussions about guns at 臭鸡八 .
I found this very helpful. For additional info, visit local air conditioning maintenance .
You haven’t truly experienced St Augustine until you’ve dined at Paladar Cuban Eatery & Bakery! cuban restaurant near me
I desire I had known approximately van rentals sooner in the time of my journeys to São Paulo—they may be exceptionally powerful for families and companies! Visit fretamento de vans !
This was quite useful. For more, visit Roofers in Greenville SC .
Thanks for the comprehensive read. Find more at construction companies .
Appreciate the detailed information. For more, visit same day plumber .
It’s encouraging to see platforms like 乱伦类 that address both sides of the gun debate thoughtfully.
Navigating through injury claims would have been daunting without my local # personal injury attorney # providing expert advice and support throughout!
Wonderful blend contrasting various viewpoints shared highlighting importance collaboration embracing diversity enriching conversations sparked amongst peers ultimately benefitting collective intellect growth shared throughout community spirit fostered google.com
Very helpful read. For similar content, visit game tại bubet club .
Wow, this article is pleasant, my younger sister is analyzing such things, so
I am going to convey her.
Усильте позиции сайта быстро и эффективно!
Закажите прогон Хрумером и ГСА по супернизкой цене —
гарантия роста трафика и улучшения SEO-показателей вашего ресурса.
Только проверенные базы и индивидуальный подход к
каждому проекту.
Увеличьте посещаемость и прибыль прямо сейчас!
больще ифрЗДЕСЬ
Appreciate the detailed post. Find more at Foothills Paving .
Fantastic insight provided here – loved every bit of it ! Neighbors encountering problems could gain significant help by tapping into resources found over at # # anyKeyWord # Electrician Glendale
Just booked my first appointment for a chemical peel in Newport Beach. Can’t wait to see the results from this ##med spa##! med spa newport beach
Thanks for the informative content. More at Summers Plumbing Heating & Cooling .
The signs of hearing loss can be subtle; I’m glad there are resources like this blog to educate us all! hearing examination
I’ve been trying into preventative care and determined some mammoth data with regards to chiropractic prone at pediatric chiropractor near me !
I found this very interesting. For more, visit Sink leaking .
Businesses rely upon precision, and that is what makes firms like flow meter calibration near me so important!
Valuable information! Find more at Garden City ac repair .
I found this very helpful. For additional info, visit air conditioning .
Finally found a reliable service for gutter repair nearby, and they really took care of everything efficiently—so grateful! gutter repair
I get pleasure from how informative the weblog posts from pressure gauge calibration near me are relating to most competitive practices in calibration.
The customer care at house cleaning near me is great– they really care about their clients.
Nicely detailed. Discover more at https://www.bestbookmarks.win/the-relevance-of-a-dependable-pipes-and-heating-system .
Thanks so much for taking time put together such detailed guidance regarding wiring matters ; surely everyone needing assistance locally ought explore options available from # # anyKeyWord # Electrician Glendale Arizona
Thanks for the insightful write-up. More like this at https://maps.app.goo.gl/LRyZFX4KYM6rDEj86 .
Dogs realize tips on how to cheer us up at some point of tricky times—how does yours deliver help after you’re feeling down ? Let’s talk emotional bonds over ### anykeyword ### https://wiki-planet.win/index.php/Common_Misconceptions_About_Pit_Bulls_Debunked!_30887
It’s difficult to find educated people for this topic, however, you seem
like you know what you’re talking about! Thanks
The spices used in Mexican cooking are just divine! What’s your favorite spice blend? Discover more about it at restaurant near me !
Thanks for the useful post. More like this at Power Washing Services .
Appreciate the detailed information. For more, visit https://truba-rf.ru/user/roydelpost .
Thanks for the practical tips. More at https://maps.app.goo.gl/8Kbxwp1UVTkpAZN4A .
I found this very interesting. Check out Open Wide La Jola Dentistry for more.
“Have any of you experienced delays during your home builds due to weather conditions?” google.com
Thanks for the thorough article. Find more at https://www.apu-bookmarks.win/the-advantages-of-hiring-a-professional-plumbing-professional-and-heating-service-technician .
Appreciate the helpful advice. For more, visit https://maps.app.goo.gl/BY8N45dnCmJXRpvz6 .
Every participant in the Tiranga games represents hope and aspiration for countless others; it’s inspiring! tiranga invite code 2757419478643
This was a wonderful post. Check out power washing Joppa for more.
I’ve examine that chiropractors can get better athletic performance—excited about discovering extra through pregnancy chiropractor near me .
Calibration just isn’t just useful; it can be critical! Glad to determine providers like torque screwdriver calibration taking charge of this relevant subject.
Thanks for the clear advice. More at Emergency Commercial Refrigeration Repair .
The guidance of a skilled accident lawyer helped me navigate through my legal options after my recent accident.
I cannot stress enough how lucrative it’s miles to employ a van whilst vacationing with family members or industry businesses in Sao Paolo – cost out ###/for greater information! fretamento de van
If you’re hesitant about employing cleaners, provide house cleaning service a try– you will not regret it!
This was very beneficial. For more, visit air conditioning repair near me .
Excited to try lip fillers soon! I’ve heard great things about the professionals at a ##med spa near me##. medical spa near me
I love how you incorporate historical perspectives into modern discussions about guns at 操我 .
The option at this ##Secondhand Furniture save Perth## is usually converting, making it a exciting region to store more often than not. Secondhand Furniture Perth
Appreciate the detailed insights. For more, visit tài xỉu vua99 miễn phí .
This was beautifully organized. Discover more at local blocked drain services .
Thanks for the clear breakdown. More info at reliable drain cleaning services .
Excellent points made here about the signs that your septic tank needs pumping! septic tank pumping
Appreciate the thorough write-up. Find more at Bonney Lake Car Repair Shop .
If you might be planning a family unit reunion in São Paulo, recollect to employ a van! It’s the ultimate manner to continue absolutely everyone in combination. Visit aluguel de van for treatments.
Electrician school can be quite an investment in time and money. It’s good to know how long it typically takes in NC before diving in. If you’re curious about local rates and schools, electrician Indian Trail NC has some great resources! electrical companies near me
It’s the best time tto make a few plans for the future and it iss time to bbe happy.
I’ve read this post and if I may I want to suggest you few fascinating issues or tips.
Perhaps you can write subsequent articles relating to this article.
I want to learn more things about it!
Feel free to surf to my web site –yüksekte çalışma eğitimi
Excited about finally getting my old gutters replaced this season! Can’t wait to see how much better everything functions afterward! gutters installers
This was very enlightening. For more, visit affordable heating systems .
What’s up to all, the contents existing at this web site are really
amazing for people experience, well, keep up the nice work
fellows.
The significance of energy-efficient HVAC systems can not be overstated. I’m glad to see even more people speaking about it. You can discover added sources at milwaukie air conditioning service .
Well done! Find more at cosmetic smile makeover .
Thanks for the great content. More at Expert Paving Contractor Wheat Ridge .
Their pastelitos are some of the best I’ve ever had—make sure to grab some when you visit Paladar! cuban restaurant st augustine
The impact of colonial architecture can nevertheless be obvious at the present time, growing a blend of cultures—what’s your take on this fusion? Join the communication at hear aids .
Impressive how San Diego personal injury lawyers always go the extra mile for their clients. I bet anyone seeking justice would find san diego injury lawyer a reliable partner in navigating legal challenges with expertise and care.
Found a few special treasures on the ##Secondhand Furniture unearths Perth## adventure last weekend! Can’t wait to head to come back. Secondhand Furniture Perth
Great job! Find more at quality commercial cooling repair .
Priority Restoration did an amazing job with my water damage clean up near me. Highly recommend their services!
I had a fantastic experience with Priority Restoration Philadelphia Water Damage Clean Up Near Me
Hearing loss can sneak up on you, so regular testing is key! Have you had yours this year? hearing exams
I’ve heard that some dog breeds are more suitable for flats than others. What do you observed? https://www.runway-bookmarks.win/horse-racing-the-game-of-kings
Great job! Find more at https://www.tool-bookmarks.win/recognizing-your-home-s-water-system .
This was highly useful. For more, visit trusted gas plumber specialists .
Well done! Find more at hvac contractor Caldwell .
This was very beneficial. For more, visit https://minsk.mirdorog.by/user/kanyonpdxl .
So grateful for the insights received right through my fresh #hearingaidtest# at hearing aids for tinnitus
Considering how crucial seeking legal counsel is after an injury, the expertise of Portland personal injury lawyers cannot be underestimated portland motorcycle accident lawyer
This was highly educational. For more, visit affordable plumbing repair .
It’s so important to choose a reputable repair service for your air conditioning, especially here in Gilbert! google.com
Historical fortifications remind us of earlier conflicts and techniques; visiting them brings background to existence! Explore more fortresses at best architecture companies .
This was nicely structured. Discover more at Foothills Paving .
I recently took a hearing test and was amazed by how simple the process was. Everyone should do it! free hearing test
Thanks for the useful suggestions. Discover more at expert trust a trader plumbing .
Have skilled delightful surprises from strange acts carried forth through loyal partners demonstrating affection unconditionally all through varying cases shared–Can relate for my part against such anecdotes?? https://wiki-site.win/index.php/Understanding_the_Different_Types_of_Barks_and_What_They_Mean_43939
Finding the accurate veterinarian is vital for our canine’ wellbeing and fitness. What do you seek in a vet? Check out facts at https://atomic-wiki.win/index.php/Canine_Enrichment_Activities_That_Will_Keep_Them_Busy_All_Day!_99380 .
I think every meal should start with chips and salsa! What do you think? Find the best chips and salsa combos at restaurant !
A trustworthy calibration provider is worthwhile; check out what ### anyKeyWord### gives at the moment! ring gage calibration
It’s refreshing to see a site like 总理 that values education over sensationalism in the firearms debate.
Looking for a great Cuban restaurant? Look no further than Paladar Cuban Eatery & Bakery in St Augustine! cuban food st augustine
These common heating and cooling issues are so relatable! I’ve faced a few myself. If anyone needs assistance, I advise taking a look at ac maintenance and repair milwaukie or for solutions.
Fantastic article on heating and cooling maintenance pointers! It’s so vital to keep our systems running efficiently. For more insights, look into hvac repair milwaukie or .
This was quite informative. More at https://diego-maradona.org/user/miliontncv .
The comfort of renting a van in São Paulo is unmatched—most excellent for families and commercial companies alike! More important points at aluguel de vans .
This was highly helpful. For more, visit plumbing & heating near me .
A tender experience round São Paulo is guaranteed should you rent a spacious family van—discover selections on aluguel de van !
Van leases are ultimate for drawback-unfastened transport in bustling São Paulo! Check out what aluguel e van sp has to be offering.
After I originally left a comment I seem to have clicked on the -Notify me when new
comments are added- checkbox and now whenever
a comment is added I get 4 emails with the same comment. Is there
a means you can remove me from that service? Thanks!
Great delivery. Outstanding arguments. Keep up the amazing effort. https://www.forum-Sachsen.com/proxy.php?link=http://Dragon-slave.org/comics/AdeleccLockeln
I appreciate how eco-friendly many manufactured homes are these days; great info on Manufactured homes for sale Mantua !
Wonderful tips! Find more at Blocked sinks Macerators .
Van leases are most appropriate for issue-unfastened shipping in bustling São Paulo! Check out what fretamento de vans has to offer.
Finding the right accident lawyer can significantly impact the outcome of your case, so take your time in making that choice.
I believe everything typed made a ton of sense.
However, think about this, suppose you wrote a catchier title?
I mean, I don’t want to tell you how to run your blog, but what if you added something that makes people want
more? I mean Certain Scores May Predict Which Trauma Patients
Face High Risk of Multiple Infections – Healthcare Hygiene
magazine is a little vanilla. You ought to glance at Yahoo’s front page and watch how they create article titles to grab people to open the
links. You might add a related video or a picture or two to grab people excited about what you’ve got to say.
In my opinion, it would bring your website a little livelier.
This is very insightful. Check out cosmetic dental clinic for more.
I love how green buying at a ##Secondhand Furniture save close me Perth## can be—awesome for each my wallet and the planet! Best Secondhand Furniture Perth
Experience unforgettable moments with Bhopal escorts by Minnie88. Our elegant, discreet, and charming companions offer the perfect blend of pleasure, class, and confidentiality—designed for your comfort and desire.
Experience unforgettable moments with Bhopal escorts by Minnie88. Our elegant, discreet, and charming companions offer the perfect blend of pleasure, class, and confidentiality—designed for your comfort and desire.
Bhopal escort service
The journey of healing starts with a single step: reaching out for help through counseling! Learn more at EMDR Therapy .
Nice post
Your coverage of gun shows and events is fantastic, especially the insights from 浪叫 !
Wonderful tips! Find more at Climate-Alignment .
Is there an age restriction for receiving chiropractic adjustments? Would love readability from the assets at pregnancy chiropractor near me
This was very insightful. Check out professional local plumbing experts for more.
Great job! Find more at near me plumber .
Do yourself a favor and employ house cleaning near me for your next deep clean; it deserves every cent!
I enjoyed this read. For more, visit agence seo saint-étienne .
The option at this ##Secondhand Furniture retailer Perth## is all the time changing, making it a fun position to keep almost always. Perth Secondhand Furniture shop
Thanks for the clear breakdown. Find more at smile makeover techniques .
Hi colleagues, its great paragraph on the topic of
educationand fully explained, keep it up all the time.
Appreciate the great customer service from asesoria Almeria during my last septic tank maintenance visit.
Tremendous issues here. I am very happy to peer your article.
Thank you so much and I’m taking a look ahead to touch
you. Will you please drop me a mail?
This is highly informative. Check out https://mezyena.info/user/kylanalfol for more.
This blog has inspired me to spread the word about how vital it is to prioritize our auditory health—thank you for sharing this info! over the counter hearing aids
This was highly educational. More at Commercial Refrigeration Repair Service .
The aftermath of an accident can be overwhelming; that’s why having a knowledgeable accident lawyer by your side is invaluable.
“Seeing so many lovely fences around has inspired me to finally get mine done—thanks for the tips!” https://maps.app.goo.gl/zFoBM7QV13WaedDn7
The staff at the ##med spa newport beach## were so welcoming during my chemical peel session. Feeling fresh and renewed! chemical peel newport beach
Thanks for the insightful write-up. More like this at quick plumbing and heating help .
Looking for top-tier representation in Seattle? These personal injury lawyers will have your back! Don’t hesitate to reach out for expert advice and support with personal injury lawyer .
Any tips on how often we should get our gutters professionally inspected? I’ve heard varying opinions and want to stay informed. gutter repair
This was highly educational. More at https://sport-news.com.az/user/ossidysgyt .
Thanks for the valuable article. More at https://maps.app.goo.gl/eennVsMa8aGrrpkd8 .
Great insights! Find more at Sewer line replacement .
The Cuban bakery at Paladar is a must-visit for anyone who loves fresh pastries! Their desserts are simply divine! cuban food st augustine
My recent experience with a professional audiologist was eye-opening; they emphasized the importance of regular testing so much! ear test near me
It’s inspiring to peer such a lot of volunteers aiding aged care in Perth. Their contributions actually make a difference inside the lives of citizens! Expert Aged Care Perth
Wow, I really did not recognize how much energy we throw away with bad heating and cooling practices! Many thanks for raising understanding. Discover more about performance at milwaukie ac service .
Calibration isn’t very just indispensable; that’s serious! Glad to look companies like pressure gauge calibration near me taking payment of this good container.
This was a wonderful post. Check out download link vua99 for more.
Is there an age prohibit for receiving chiropractic modifications? Would love clarity from the components at chiropractor
Thanks for the useful post. More like this at professional drain solutions .
Thanks for the detailed guidance. More at same day boiler replacement .
I love how the Tiranga games highlight not only sports but also cultural performances from across India! tiranga invite code 2757419478643
This was highly educational. More at Local Plumbers .
I love that manufactured homes can be customized to fit your needs, especially with what’s available on Affordable manufactured homes for sale !
Traveling as a family unit might possibly be troublesome, yet renting a van makes it so much more straightforward! Find your answer at aluguel de van são paulo .
Organizing a kin time out? Rent a van and make it memorable! Visit aluguel de van for a few exceptional selections.
This was highly helpful. For more, visit agence seo saint-étienne .
What’s the best way to market my new video recording studio? Any suggestions? google.com
I enjoyed this read. For more, visit Summers Plumbing Heating & Cooling .
I can’t think how affordable house cleaning services is for the quality of service they provide!
The range at this ##Secondhand Furniture keep Perth## is normally altering, making it a fun region to store in many instances. Perth Secondhand Furniture
Just offered my first electric power washer, and I’m inquisitive about the entire tasks in advance of me this summer time! https://wiki-canyon.win/index.php/A_Beginner%27s_Guide_to_Pressure_Washing:_Everything_You_Need_to_Get_Started_18695
“AC issues always seem to pop up at the worst possible time—stay ahead of them!” Everest Air LLC
This was quite helpful. For more, visit http://viproskurnin.ru/user/patiuspeyo .
Thanks for the useful post. More like this at Open Wide La Jolla Dental .
Appreciate the comprehensive insights. For more, visit https://natpresstv.ru/user/jeovishwbj .
What are a few long-established misconceptions approximately chiropractic care? Looking forward to uncovering truths simply by assets at walk in chiropractor near me !
Thanks for the great information. More at https://manualshyundai.com/user/marachwuuq .
I’ve been searching for good ##Cuban food##, and I finally found it at Paladar Cuban Eatery & Bakery in St. Augustine! cuban food near me
Great job! Discover more at bubet cho người chơi .
Thanks for the helpful advice. Discover more at ClimateAlign .
I had a few points with my AC unit closing summer, but as a result of Air Conditioning Repair Perth , it’s jogging easily now!
I’ve been looking for reliable construction services in Asheville. Any recommendations? Blue Ridge Concrete & Construction LLC
This post really highlights the advantages of normal cooling and heating examinations! It can save money in the long run. For even more suggestions, head to licensed ac repair milwaukie .
Thanks for the detailed guidance. More at Washing-machine repairs .
Thanks for the detailed guidance. More at emergency plumber near me .
I recommend reaching out to a local personal injury attorney if you’ve been involved in an accident. They can guide you through the legal maze.
This post should be mandatory reading for all new homeowners—great insights on ### anyKeyWord ###! septic tank pumping
This was a great help. Check out charlotte auto glass for more.
Traveling as a family unit shall be difficult, yet renting a van makes it so much more straightforward! Find your resolution at aluguel de vans .
Just rented from ###; they’ve got implausible customer support and smartly-maintained cars, made our ride sleek crusing. aluguel e van sp
پروتئین وی هیدرولیزه اپتیموم نوتریشن، یکی از خالصترین و پیشرفتهترین مکملهای پروتئینی است که از پروتئین وی ایزوله و هیدرولیز شده تهیه شده است.
I appreciated this article. For more, visit experienced cosmetic dentist .
I enjoyed this read. For more, visit Thermostats Gas valves .
I love how simple it’s to employ a van for family members outings in São Paulo! For the pleasant offers, fee out fretamento de vans .
So curious approximately DIY recipes feasible on-line adapted exceptionally in the direction of editing overall performance throughout the time of cleans??? # https://wiki-fusion.win/index.php/How_to_Safely_Pressure_Wash_Your_Car_Without_Damage
Has anyone ever had a nightmare experience with gutter installation? I’d love to hear what went wrong and how they resolved it. gutters repair near me
Great job! Find more at Climate-Alignment .
Every breed has its quirks – what is one certain factor approximately your canine’s persona that consistently makes everyone snicker ? Let’s trade memories over ### anykeyword ### https://wiki-nest.win/index.php/Choosing_the_Right_Veterinarian_for_Your_Dog%27s_Needs_97888
My heart melts seeing older refuge doggies after all locating properties ! Have seen heartwarming achievement reviews lately ? Please inform us all approximately it right here ### anykeyword ### https://post-wiki.win/index.php/The_Science_Behind_Why_Dogs_Love_Us_So_Much
Thanks for the comprehensive read. Find more at https://aiia.su/user/launusnype .
”Fascinating st furnace prices specifications
Thanks for the useful suggestions. Discover more at https://xn--e1adphegqz7e.xn--p1ai/user/elbertrbtw .
Appreciate the detailed insights. For more, visit Boiler installations .
This was beautifully organized. Discover more at Saniflo WCs .
Dogs have stunning instincts—have they ever alerted you to a thing peculiar in time ? Please share those moments here ### anykeyword ### https://bravo-wiki.win/index.php/Canine_Fashion:_Dressing_Up_Your_Pup_in_Style!_52414
I enjoyed this post. For additional info, visit https://dojki.ebanza.ru/user/tucaneuqdc .
What an marvelous community we have got here in Perth helping our elderly population simply by alternative aged care features! Aged Care Community Perth
A professional personal injury attorney near me not only assists with legal matters but also provides emotional support during challenging times.
Such an magnificent task from get started-to-finish which makes us unswerving consumers from now on!!!!## Window Cleaning
I recently learned that the cost of a $1000 bail bond in Burlington, NC is significantly lower than many might think. For those interested in understanding these financial aspects better, bails bond near me is a great resource. bail bondsman near me
Appreciate the comprehensive insights. For more, visit agence seo saint-étienne .
Families traveling São Paulo can make the maximum of their day trip by means of renting a van. Check out the companies at aluguel e van sp !
Who knew that a standard hearing exams listening to reduction take a look at may switch my life loads?
Celebrating cultural diversity through friendly competitions adds vibrancy—so grateful we have platforms like “Tirangagames” available!!### anykeyword### tiranga invite code 2757419478643
Understanding cultural variety inside elderly care is necessary, notably here in multicultural Perth—we can all read from one another’s backgrounds! Perth Aged Care community
This was a great article. Check out car hire for more.
Nicely done! Discover more at https://lordfilms.live/user/ravetttvml .
This was highly helpful. For more, visit repairing plumbing lines .
This was a fantastic resource. Check out reliable drain cleaning services for more.
After researching various companies, I’ve decided to go with one of the top-rated ##Gutter Repair Near Me## services. gutters installers
Manufactured homes are such a smart choice! Love the options available on Affordable manufactured homes for sale .
Wonderful tips! Find more at Bathroom refurbishments .
This was a wonderful post. Check out https://mightandmagic.ru/user/seidheejrn for more.
It’s a must-have that we suggest for improved investment and instruments for aged care products and services across Western Australia, which include Perth! Aged Care in Perth
I found this very helpful. For additional info, visit Climate-Alignment .
The value of energy-efficient heating and cooling systems can not be overstated. I rejoice to see even more individuals talking about it. You can discover extra sources at air conditioner repair .
Renting vans is such an green manner to travel as a set in busy cities like São Paulo—thank you, fretamento de van !
Appreciate the comprehensive advice. For more, visit emergency drain cleaning service .
Is it true that some roofing contractors in Mesa offer free estimates? That would be great! Roofing Contractor Mesa AZ
”The knowledge and skills that come from working with professionals like Public Adjusters is unmatched.” Insurance agency
So satisfied I found out approximately Affordable Air Conditioning Repair Perth – they made the total procedure of getting my AC repaired straightforward and pressure-loose!
. Thankful that you shared real-life examples along with theoretical knowledge!! https://www.google.com/maps/place/?q=place_id:ChIJzWucoD6pK4cRKc7uL4PUr18
Thanks to asesoria Almeria for their fast and friendly service during my recent septic tank pumping!
I are not able to accept as true with how plenty cost I’ve saved with the aid of purchasing at ##Cheap Secondhand Furniture Perth##! Definitely value a talk over with. Quality Secondhand Furniture Perth
Appreciate the useful tips. For more, visit Open Wide La Jolla Dental .
Thanks for the detailed guidance. More at agence seo saint-étienne .
This was highly useful. For more, visit plumbing specialists .
Just rented from ###; they have fine customer service and properly-maintained vans, made our trip easy crusing. aluguel de van
I love how good value van leases is also for higher agencies traveling São Paulo—inspect out aluguel de van são paulo !
Thanks for the valuable article. More at power flushing for radiators .
This was very beneficial. For more, visit plumber pricing guide .
This was a wonderful post. Check out a plumber for more.
I’m curious approximately working puppy breeds. Which ones have you ever chanced on to be the such a lot shrewd? https://www.bookmark-step.win/get-to-be-aware-of-a-veterinarian
I appreciate your tips on managing a multigenerational workforce! Effective strategies are essential; explore resources at human resources consulting firm .
The workforce at Perth Air Conditioning Repair service is legit and educated. They effortlessly clinically determined my air conditioning aspect.
Asheville has a booming construction market! Excited to see what new projects emerge next. Blue Ridge Concrete & Construction LLC
This is highly informative. Check out Gas safety certificates for more.
This was very enlightening. More at plumbing services near me .
This was quite useful. For more, visit https://audiokniga-online.ru/user/moenusvwly .
Such an eye-opener to see how far manufactured homes have come; thank you, Move in ready manufactured homes , for showcasing them beautifully!
Your focus on health and wellness initiatives in companies is very relevant today; discover comprehensive plans from hr consulting firms !
There’s nothing noticeably like seeing the grins on citizens’ faces for the period of occasions at nursing buildings around Perth—it warms my center each time! Aged Care Facility Perth
Your guide to understanding SEER ratings was very informative; it really helps when shopping around for units! Check out additional resources at hvac repair
Thanks for the great tips. Discover more at ac replacement company .
This is very insightful. Check out wedding floral decor Long island for more.
Ganhe 100 dólares de bônus ao criar sua conta na
https://gbg-bet-br.com e comece apostando com muito mais confiança.
Essa promoção é exclusiva para novos usuários
e é ativada automaticamente após o registro.
Com o bônus, você poderá explorar todo o catálogo da casa:
desde apostas esportivas em campeonatos nacionais e internacionais até jogos de cassino
com crupiês ao vivo. Aproveite essa oferta e transforme seu primeiro acesso em uma chance real
de lucro.
There are so many myths approximately canines available! What misconceptions have you heard? Let’s debunk them collectively at https://wiki.gta-zona.ru/index.php/Socializing_Puppies:_The_Key_to_a_Well-Adjusted_Adult_Dog !
This was beautifully organized. Discover more at https://xn--80aaaokoti9eh.xn--p1ai/user/aspaidpypl .
Absolutely overjoyed with how informative and supportive the crew turned into for the duration of my #hearingaidtest# at hearing examination
This was quite informative. For more, visit local plumbing solutions .
Great job! Find more at types of cosmetic dental treatments .
This is such valuable information! If anyone needs electrical help in Glendale, I recommend Electrical Glendale Arizona .
Great read! Do you have any recommendations for eco-friendly materials? https://www.google.com/maps/place/?q=place_id:ChIJQW9JHsvTbYgRecmrsGadyDg
There’s whatever thing uncommon approximately looking antique portions on the ##Secondhand Furniture store Perth## that you just simply can’t get anywhere else. Local Secondhand Furniture Perth
Appreciate you posting this. This clarified a lot about what to do after an accident. The point about documenting injuries was especially important car accident lawyer
Just had the most delicious breakfast at cuban restaurant ; their Cuban pastries are unbeatable!
I appreciated this post. Check out air conditioning maintenance near me for more.
This was very insightful. Check out affordable blocked toilet repair for more.
Thanks for the clear breakdown. More info at Roofing contractor Bozeman .
The maintenance efforts for UNESCO World Heritage Sites are imperative for cultural continuity! Let’s speak about their importance at architecture firms near me .
Wonderful tips! Find more at Climate-Alignment .
Appreciate the helpful advice. For more, visit agence seo saint-étienne .
The transition into aged care is additionally complicated, but with the proper beef up, it’ll also be a victorious enjoy—incredibly here in Perth! Perth Aged Care
پروتئین وی ایزوله نچرال آلمکس، حاوی ۲۷ گرم پروتئین وی ایزوله فوق خالص در هر پیمانه است، بدون چربی، شکر، طعمدهنده یا شیرینکننده مصنوعی.
Thanks for the detailed guidance. More at Sewer line repair company .
Thanks for the detailed post. Find more at https://muhammad-ali.pl/user/tucaneolsl .
great post, very informative. I wonder why the other specialists of this
sector don’t understand this. You must proceed your writing.
I’m sure, you’ve a great readers’ base already!
The way you explained how often to pump based on tank size was super helpful! Thank you! septic tank pumping
Thanks for the valuable article. More at plumbing contractors near me .
This post actually highlights the benefits of normal HVAC exams! It can save cash in the future. For even more ideas, head to ductless ac repair milwaukie .
This was highly helpful. For more, visit ac company near me .
Wonderful tips! Find more at Open Wide La Jolla Dental .
Thanks for the detailed post. Find more at dishwasher leak repair .
Thanks for the great content. More at Clogged toilet repair .
Thanks for the detailed post. Find more at local mold remediation .
Thanks for the helpful article. More like this at local plumbers in my area .
Great job! Discover more at Sewer line replacement expert .
Just had a appropriate sense with an emergency plumber from Emergency Plumber Charlotte the following in Charlotte!
https://xn--mgbg7b3bdcu.net/?qa=user/planecross48
Thanks for finally writing about > Healthcare Hygiene magazine < Liked it!
Love your take on creating inclusive workplaces—HR has a big part to play here; check out best practices from human resources agency !
I’ve been to many ##Cuban restaurants##, but nothing compares to the homey feel and great food at Paladar Cuban Eatery & Bakery. cuban restaurant st augustine
This was beautifully organized. Discover more at Boiler repairs Leaks .
This was beautifully organized. Discover more at cách chơi tài xỉu bubet .
Thanks for the useful suggestions. Discover more at Foot Hills Paving .
Here’s hoping future generations continue carrying legacy forward through unified efforts made possible thanks largely due diligence shown behind scenes orchestrating successful endeavors such as ones exhibited throughout history established via tiranga invite code 2757419478643
Appreciate the insightful article. Find more at roofers Bozeman .
I found this very helpful. For additional info, visit agence seo saint-étienne .
This was highly educational. For more, visit expert plumbing services nearby .
Dogs have an astonishing capacity to conform; how does yours deal with differences in habitual or ecosystem? Let’s chat approximately adaptability on https://city-wiki.win/index.php/Understanding_the_Canine_Sense_of_Smell:_How_It_Works_10067 .
From advocating for your rights to guiding you through the legal process, Sacramento personal injury lawyers truly make a difference in difficult times sacramento truck accident lawyer
Appreciate the detailed information. For more, visit Sani flo .
I love hearing about different names human beings deliver their dogs; what’s the story behind your dog’s title? Share it over at https://mega-wiki.win/index.php/The_Importance_of_Hydration_in_Maintaining_Canine_Health !
Very informative piece about employer branding—it’s vital for attracting talent; see further examples from hr consulting service providers !
“Great points made about seasonal maintenance—it truly pays off living here!” google.com
Who knew that a realistic ear test near me hearing relief scan may well alternate my existence much?
I found this very helpful. For additional info, visit https://forum.xn--frderung-n4a.at/member.php?action=profile&uid=220286 .
Anyone interested may want tips regarding scheduling appointment times too – many offer same day service which is huge when dealing with unexpected breakdowns! Greg’s Grade A Appliance Repair Arlington TX
Quick tip: Always save the number of an Emergency Plumber Charlotte reachable for plumbing emergencies!
If you’re searching for a compassionate and skilled accident attorney, look no further than personal injury .
Thanks for the clear advice. More at https://tussom.com/forums/member.php?action=profile&uid=117107 .
This is very insightful. Check out Gas safety certificates for more.
Well done! Discover more at cosmetic dental clinic amenities .
Fascinating insights on the support that Los Angeles personal injury lawyers provide. Those seeking legal assistance for their needs should definitely check out injury lawyer for valuable information and resources.
Impressed with the aid of how without delay that you may reap effects with a force washer—I’m offered on making an attempt it myself now! https://online-wiki.win/index.php/How_to_Choose_the_Right_Pressure_Washer_for_Cleaning_Concrete_Sidewalks
Appreciate the thorough information. For more, visit water damage restoration .
Appreciate the thorough analysis. For more, visit American Rooter & Drain .
Appreciate the comprehensive insights. For more, visit local toilet installation costs .
Appreciate the thorough write-up. Find more at professional refrigeration repair services .
Keren banget, langsung gue pake.
This was a great help. Check out vua99 tài xỉu trực tuyến for more.
Thanks for the thorough analysis. More info at Boiler installation .
Appreciate the detailed post. Find more at professional gas safety inspections .
Just had my septic tank serviced by asesor fiscal . They were prompt and efficient!
This is quite enlightening. Check out http://hondaikmciledug.co.id/HRIS/member.php?action=profile&uid=207213 for more.
Stay updated with live news streaming available 24/7 from leading U.S.
news networks. You can catch the Fox News Live Stream,
CNN Live, MSNBC News, and CNBC as news breaks, covering everything from politics and business to
world events and market updates. Whether you’re interested in international headlines, financial
news, or political changes, these reliable channels keep you
informed with the latest developments.
You can access live news streaming anytime and anywhere on your
preferred device. Enjoy the latest updates, expert analysis, and firsthand reporting all in a single spot.
It’s ideal for viewers who want to stay in the loop with current events through continuous, high-quality news coverage.
If you’re looking for a longer read, a catchy social media caption, or want to dive deeper into a
specific channel like CNBC for business insights, just let me know!
Appreciate the detailed information. For more, visit Open Wide La Jolla Dentist .
Absolutely cherished the segment discussing moveable vs constant installations comparing professionals/cons between innovations selected wisely alongside respective routes taken elegant upon exotic situations encountered as a result likewise representing furnace prices online portal
Your points about leadership development are so relevant today! Strong leaders drive success; find out how at hr outsourcing experts .
Appreciate the detailed post. Find more at emergency plumbing services .
Thanks for the thorough article. Find more at agence seo saint-étienne .
Please let me know if you’re looking for a author for your blog.
You have some really great articles and I feel I would be
a good asset. If you ever want to take some of the load off, I’d love to write some content for your blog
in exchange for a link back to mine. Please blast me an e-mail if interested.
Thanks!
You can definitely see your enthusiasm within the work you write.
The arena hopes for more passionate writers such as you who aren’t afraid to mention how they believe.
Always follow your heart.
This was quite helpful. For more, visit ClimateAlign .
This was very enlightening. More at tài xỉu bubet online .
Wonderful tips! Find more at trusted my plumber services .
Emergency plumbing can also be traumatic, but the staff at Emergency Plumber Charlotte made it quite a bit more easy for me.
Appreciate the thorough write-up. Find more at Foot Hills Paving .
This was very enlightening. For more, visit professional toilet repair .
The story behind each athlete at the Tiranga games is so inspiring; they deserve all our support! tiranga invite code 2757419478643
Fantastic advice around leveraging data analytics in HR decisions—it can transform operations; explore tools available through affordable outsourced hr solutions !
Thanks for the clear breakdown. Find more at http://www.bonjourdewi.com/bb/member.php?action=profile&uid=354124 .
Very useful post. For similar content, visit plumb tub .
Thanks for the detailed post. Find more at pool installation services .
I was skeptical about manufactured homes, but after seeing what’s available on Move in ready manufactured homes , I’m convinced!
Great job! Find more at agence seo saint-étienne .
Thanks for the insightful write-up. More like this at Wheat Ridge Driveway Paving .
I found this very interesting. Check out 24 7 plumber for more.
Had an unfamiliar water leak final evening; fortuitously, I also known as Emergency Plumber Charlotte and so they arrived promptly!
“My public adjuster’s expertise helped clarify so many things about my claim process—so grateful!” Public Adjuster Arizona
Appreciate the detailed insights. For more, visit https://maps.app.goo.gl/EykuzavQSAp1saUN9 .
Can’t feel how informative my #hearingaidtest# become at ear aids near me
Thanks for the valuable insights. More at local plumbers recommended .
Useful advice! For more, visit affordable dental cosmetic procedures .
Valuable information! Discover more at air conditioning companies near me .
I found this very interesting. Check out painters Littleton for more.
With temperatures rising, knowing who to call for AC repair is incredibly important! https://www.google.com/maps?cid=12717811348265145193
کارشناس سئو سایت فردی است که
مسئول بهینهسازی وبسایتها برای موتورهای جستجو مانند
گوگل است. هدف اصلی این کارشناس افزایش رتبه سایت
در نتایج جستجو است تا سایت به
مخاطبان بیشتری دسترسی پیدا کند و در نتیجه ترافیک
و بازدید از آن بیشتر شود.
Every historic constructing has its own targeted tale to inform! I love exploring these narratives via architecture. Find out extra at architecture firms near me .
The significance positioned upon site-particular issues highlights customization helpful across distinctive environments!!!! # #anythingKeywords # https://fair-wiki.win/index.php/Choosing_the_Right_Lenses_for_Optimal_Camera_Positioning_84003
Great insights! Find more at blocked drains troubleshooting .
Appreciate the detailed post. Find more at http://amantespastoraleman.com/foro/member.php?action=profile&uid=328768 .
Thanks for the thorough analysis. Find more at Climate Alignment .
I’m considering IV therapy for my chronic fatigue. I’ve read that it can help replenish vitamins and minerals effectively. What do you all think? I found some great resources here: iv therapy .
I’ve been putting off my ### anyKeyWord ###, but not anymore after reading this informative article! septic tank pumping
This was a great article. Check out best plumbing for more.
I think public spaces in NYC could play a role in promoting mental health. What do you think? Check out my thoughts at psychiatrist new york .
Fantastic breakdown of recruitment strategies! The right HR firm can significantly impact your hiring process. Learn more at affordable hr firms .
I always emailed this weblog post page to all my contacts, for the
reason that if like to read it then my contacts will too.
Being section of native rescue efforts ensures quite a few lives kept day by day – Is volunteering some thing near adequate FOR YOU also pondering serving to others? https://charlie-wiki.win/index.php/The_Ultimate_Guide_to_Dog_Nutrition:_What_Every_Pup_Needs
This was highly informative. Check out Open Wide La Jolla Dental for more.
What’s Taking place i am new to this, I stumbled upon this I’ve
found It positively helpful and it has helped me out loads.
I’m hoping to give a contribution & assist other users like
its aided me. Great job.
Appreciate the helpful advice. For more, visit local plumbing solutions .
Thanks for the insightful write-up. More like this at ClimateAlign .
The role of HR in fostering innovation is often overlooked! Dive into strategies that work at quickbooks payroll integration .
Your commitment to firearm safety education at 裸舞视 is commendable! Keep spreading awareness.
I take pleasure in the notice to aspect from Evans’ Exterior Cleaning right through my fresh window cleansing! Window Cleaning Company
Thanks for the useful suggestions. Discover more at Expert Paving Contractor Wheat Ridge .
Very useful post. For similar content, visit local plumbing companies .
Thanks for the great tips. Discover more at Summers Plumbing Heating & Cooling .
If you are attempting to find an emergency plumber who cares, I awfully suggest giving Emergency Plumber Charlotte a call.
Thanks for the clear advice. More at motor vehicle accident attorney .
IV therapy seems like a fantastic option for busy professionals who need a quick health boost! I’m looking forward to trying it out soon. Anyone want to share their experiences? Check this site for further insights: iv therapy springfield .
Appreciate the detailed information. For more, visit Central heating installations .
This was very insightful. Check out wedding floral decor for more.
Appreciate the thorough information. For more, visit agence seo saint-étienne .
Just received house from my #hearingaidtest#, and I’m humming with new data! Thank you, over the counter hearing aids
I appreciate your efforts in debunking myths surrounding firearms ownership shared through your platform, like in this post from 陰戶 .
This was very enlightening. More at https://qa.andytoan.vn?qa=user&qa_1=nathopatvw .
I enjoyed reading about the innovations in weapon technology discussed at 操他妈 . Exciting times ahead!
This was nicely structured. Discover more at local roofers near me .
Thanks for the helpful article. More like this at Roofing .
Architectural types like Baroque and Romanesque have varied characteristics which can be fascinating! Learn more about their qualities at ll 97 compliance solutions .
Thanks for the clear advice. More at Foothills Paving .
Well explained. Discover more at tài xỉu vua99 miễn phí .
Appreciate the comprehensive insights. For more, visit air conditioning maintenance near me .
”Excited studying all new ideas emerging revolutionizing marketplace reshaping finished structures allowing superior flexibility adaptability responding all of a sudden needs bobbing up without delay moving landscapes dynamically evolving l furnace prices online
Appreciate the useful tips. For more, visit Sewer line repair .
Thanks for the thorough analysis. More info at local underfloor heating services .
This was quite helpful. For more, visit Power Washing Bel Air .
Every home owner should word down the quantity of an # anyKeyWord# just in case of emergencies! Emergency Plumber Charlotte
Nicely detailed. Discover more at best air conditioning maintenance .
Very helpful read. For similar content, visit Blocked sinks Macerators .
Everyone should know about this site; it’s helped so many of us here! Rancho Bernardo Heating & Air
I love how you keep your audience updated with current events in the gun industry through your posts at 台湾独立 !
Just moved into my new home from a listing I found on Affordable manufactured homes for sale —thank you for making this possible!
Thanks for the thorough analysis. Find more at professional reliable plumbing .
Great tips! For more, visit bubet online .
hi!,I really like your writing so so much! percentage we keep up a correspondence more about your post
on AOL? I need a specialist in this house to unravel my problem.
Maybe that’s you! Having a look ahead to look you.
This is quite enlightening. Check out plumbing line troubleshooting for more.
Having someone knowledgeable about local laws and regulations is key; that’s where a public adjuster shines! https://www.google.com/maps?cid=13210929340122306639
Well done! Find more at agence seo saint-étienne .
Thanks for the detailed guidance. More at peronal injury attorney .
Great insights! Find more at Eagle Air Co Heating and Cooling .
I love how easy it is to find qualified psychiatrists in New York using psychiatrists new york ; it really simplifies the process.
Remember, relapse doesn’t indicate failure; it’s part of the journey for many in dependency healing. addiction treatment
It’s inspiring to see people overcome their struggles with alcohol. Detox is just the beginning! Learn more at alcohol detox .
I found an amazing detox program online that truly assisted me through my battles. See drug detox for more information.
Thanks for sharing your info. I really appreciate your efforts and I am waiting for your next write ups thanks once again.
This was nicely structured. Discover more at http://fh7980px.bget.ru/member.php?action=profile&uid=79260 .
Appreciate the great suggestions. For more, visit Leaking washing machines .
“Let’s keep advocating for quality craftsmanship and sustainable practices throughout our industry!” Construction Services in Asheville
Appreciate your stance on promoting responsible ownership and usage of firearms at 草你娘 .
Hello, i think that i saw you visited my website thus i came to “return the favor”.I’m trying
to find things to enhance my website!I suppose its ok
to use a few of your ideas!!
Witnessing history unfold amidst camaraderie & friendly rivalries creates bonds that last beyond time spent competing at “Tirangagames”. Cherishing memories forever!!### anykeyword### tiranga invite code 2757419478643
I found this very helpful. For additional info, visit affordable drain plumbing .
Wow, finding reliable Sacramento personal injury lawyers can be a game-changer for anyone dealing with legal challenges. If you need top-notch representation and support, make sure to check out car accident lawyer !
I enjoyed this article. Check out Professional Paving Contractor Wheat Ridge for more.
I found this very interesting. Check out best plumbers near me for more.
Thanks for the thorough article. Find more at http://maddog-server.org/forum/member.php?action=profile&uid=321231 .
My pal had a sump pump failure and also known as Emergency Plumber Charlotte —they were lifesavers!
I appreciate how comprehensive the listings are on mental health new york for psychiatrists in New York; it helped me choose wisely.
Anyone else inspired with how swift Emergency plumber Charlotte responded to their plumbing emergencies?
Hi, i think that i saw you visited my web site so i came to “return the favor”.I am trying to
find things to improve my website!I suppose its ok to use some of your ideas!!
This was highly educational. For more, visit flood restoration nearby .
I enjoyed reading about the innovations in weapon technology discussed at 江x . Exciting times ahead!
It’s great to see more resources becoming available for addiction treatment these days! addiction treatment
Od roku 2016 je to naše milá a usměvavá sestra.
schváleno v roce 2017 charakterizuje certifikát wo z praktických důvodů Mikroskopická endodoncie cena Praha.
“Restorative horseback riding programs show appealing results as alternative treatments along with conventional rehabs!” # # Anykeyword #. drug rehab
I never ever believed I ‘d make it through drug detox, but here I am, more powerful than ever! Read my story and others’ at drug detox .
Music therapy is a unique approach to aid in alcohol detox recovery—has anyone experienced it? Learn more about it at alcohol detox !
Appreciate the detailed information. For more, visit trusted plumbing and heating .
Thanks for the insightful write-up. More like this at https://ben-10.online/user/herianqemf .
Thanks for the clear advice. More at foothills paving and maintenance .
. Love how many environmentally friendly options there are today among listings from ###AnyKeyWord###—truly inspiring! Buy manufactured home near me
Great post! I’ve been looking for reliable roofers, and Olympia Roofing Company seems like a fantastic option. Olympia Roofing Company
This was a wonderful guide. Check out 24 hour emergency plumber for more.
This was very beneficial. For more, visit hvac contractor near me .
Thanks for the useful suggestions. Discover more at Eagle Air Co Furnace repair Chino .
”Deep appreciation expressed highlighting importance underst furnace prices updates online
Thanks for the valuable insights. More at expert washing machine repair .
Does anyone know if there are any grants available specifically targeted towards homeowners seeking upgrades/repairs related towards heating/cooling efficiency improvements? https://www.google.com/maps?cid=12717811348265145193
I appreciated this post. Check out motor vehicle accident attorney for more.
If you’re looking for reliable appliance repair in Arlington TX, I found an excellent technician who fixed my refrigerator quickly! Best appliance repair in Arlington TX
The importance of mental health awareness in relation to firearm ownership highlighted on 肉棍 is vital!
Appreciate the thorough analysis. For more, visit drain plumbers near me .
If you are in Charlotte and need urgent plumbing guide, seem to be no extra than Emergency Plumber Charlotte .
This was highly helpful. For more, visit bubet và tài xỉu .
Appreciate the detailed post. Find more at affordable plumbing solutions .
I found this very helpful. For additional info, visit Plumbing and heating .
I appreciate how you covered different roofing materials! Olympia Roofing Company has a great selection as well. Olympia new roof
I enjoyed this read. For more, visit emergency plumbing prices .
This was very beneficial. For more, visit Plumbing and heating .
The resources for understanding different types of firearms at 奸污 are invaluable for enthusiasts.
I liked this article. For additional info, visit personal injury lawyer .
Thanks for the useful post. More like this at https://duvidas.construfy.com.br/user/edhelmraby .
https://digi30sa.ams3.digitaloceanspaces.com/research/digi30sa-(138).html
MOB etiquettes say if black flatters you, all–black may be your go-to mother of the bride or mom of the groom in search of the special day.
Your ongoing commitment to supporting responsible gun ownership and education shines through every post at 全家死光 !
Great job! Discover more at personal injury lawyers near me .
This was a wonderful guide. Check out local fall heating installation for more.
The camaraderie seen during the Tiranga games is something that inspires me every day! tiranga invite code 2757419478643
Appreciate the comprehensive advice. For more, visit Commercial Paving Contractor Wheat Ridge .
Keeping in mind that recovery takes some time is vital when dealing with the challenges of recovery from addiction! addiction treatment
Having access to therapists who specialize particularly within this field has made my own individual fight feel less separating & more manageable total!. eating disorder treatment .
Including holistic techniques in drug rehab can result in more extensive healing experiences. drug rehab
Thanks for the clear breakdown. More info at A Perfect Finish Painting .
The journey of drug detox is not easy, however it’s worth every effort. Find inspiration at drug detox .
I’m interested in hearing about the psychological effects of alcohol detox on mental health—what’s your take? Join the discussion at alcohol detox !
This was very insightful. Check out car accident lawyers for more.
No matter if some one searches for his required thing, thus he/she
desires to be available that in detail, thus that thing is maintained over here.
Thanks for the great explanation. Find more at professional local plumbers .
Wonderful tips! Find more at https://maps.app.goo.gl/xpu18L2VyE4PvFMt6 .
Hey! This is my first visit to your blog! We are a group of volunteers
and starting a new initiative in a community in the same niche.
Your blog provided us useful information to work on. You have done a outstanding job!
Wonderful tips! Find more at urgent plumber .
Big shoutout to # anyKeyWord#—they dealt with my plumbing hindrance like pros! Emergency Plumber Charlotte
Nicely detailed. Discover more at gas plumber .
پروتئین وی ایزوله لین وی ماسل اسپرت، مکملی با کیفیت بالا و مناسب برای افزایش توده عضلانی بدون چربی، چربیسوزی و بهبود ریکاوری است.
Thanks for the helpful article. More like this at Foothills Paving .
I always find valuable information at 李鹏 regarding responsible weapon ownership. Keep it up!
If you’re going through clogged pipes, don’t hesitate to succeed in out to Emergency plumber Charlotte !
Appreciate the thorough insights. For more, visit emergency plumber .
Celebrating variety in techniques to treating dependencies helps us find options that work for everybody involved. # #anyKeyword ##. addiction treatment
Education about the signs of dependency is vital for early intervention. Drug rehab can save lives! drug rehab
Social media plays such powerful functions influencing perceptions regarding beauty– let’s promote positivity rather focusing solely aesthetics-based ideals !! #AnyKeyWord #. eating disorder treatment
Your tips are very helpful; they remind me to check in with Olympia Roofing Company for my roof inspection! Olympia roofer
It’s amazing how much progress one can make after completing an alcohol detox program! Celebrate recovery stories at alcohol detox .
Thanks for the valuable insights. More at HVAC Company Eagle Air Co .
The importance of swift flood damage cleanup cannot be overstated! For more information, check out flood clean up services in Temple Terrace .
The analysis of social media’s influence on public perception of firearms discussed at 社会主义灭亡 was insightful!
พบกับเทคนิคใหม่ในการใช้และดูแลรักษาไฟหน้าโปรเจคเตอร์ได้ที่นี่เลยครับ หลอดไฟ รถ
Great tips! For more, visit Boiler service & maintenance .
I never knew how much a public adjuster could assist with my insurance claim. Thanks for shedding light on this topic! google.com
Major leaks can occur each time! Luckily, I had the range of Emergency Plumber Charlotte kept on my mobilephone.
Well done! Discover more at General Plumber .
Love reading helpful advice coming directly locals familiar unique challenges faced while recovering natural disasters together vibrant communities found lovely Hawaii garden townships!!! flood cleaning services in Hawaiian Gardens
This was highly educational. More at car accident lawyer .
If you’re struggling with post-flood chaos, look no further than the helpful resources at flood clean up services in Clive IA .
Considering the importance of having reliable representation, finding top-notch portland truck accident lawyer is crucial for your peace of mind. When it comes to personal injury cases in Portland, having a skilled lawyer by your side can make all the difference.
Wow, marvelous weblog structure! How lengthy have you ever
been running a blog for? you make blogging glance easy.
The overall look of your site is wonderful, as well as the content material!
It’s heartwarming to see the community come together after flooding—don’t forget about the resources at flood damage restoration near me Council Bluffs !
Thanks for the helpful advice. Discover more at affordable local plumbing services .
Appliance breakdowns can be stressful! Thankfully there are great options for repair in Arlington, TX. Greg’s Grade A Appliance Repair Arlington TX
Saving time and money with services from great companies like ### anyKeyWord### makes life easier! Mobile Starter Replacement
A great chiropractor can change your life! Highly recommend checking out Chiropractor Lakewood if you’re in Lakewood.
Thanks for the detailed post. Find more at http://oldconsoles.ru/user/ascullkojq .
Great tips! For more, visit emergency plumbers near me .
It’s encouraging to see platforms like 乱伦小 that address both sides of the gun debate thoughtfully.
Nicely detailed. Discover more at Foothills Paving .
Why visitors still use to read news papers when in this technological globe the whole thing is available
on web?
I appreciated this post. Check out lấy thêm thông tin for more.
I admire how you tackle controversial topics with sensitivity and depth on 绕过封锁 .
The tips for maintaining firearms shared at 嫩穴 are practical and easy to follow.
Thanks for the helpful advice. Discover more at Leak detection .
Appreciate the thorough insights. For more, visit peronal injury attorney .
Love seeing local services provide support by working with individuals who are recovering addicts; it creates opportunities while likewise cultivating neighborhood goodwill too. # any Keyword ## addiction treatment
Appreciate the great suggestions. For more, visit Eagle Air Co HVAC Repair .
Great tips! For more, visit https://forum.xn--frderung-n4a.at/member.php?action=profile&uid=220310 .
“Mentorship programs combining experienced peers with newbies cultivates connection while offering valuable insights!” # # Anykeyword #. drug rehab
Appreciate the detailed post. Find more at https://praisenpray.org/forums/member.php?action=profile&uid=369114 .
The stigma around addiction often complicates recovery; how do we break this barrier during and after detox? Share thoughts and insights on this topic at alcohol detox !
Assistance is vital during drug detox. Surround yourself with positive influences! More pointers at drug detox .
Your commitment to firearm safety education at 露b is commendable! Keep spreading awareness.
Is chiropractic adjustment safe for everyone? I’m curious about how effective it is at places like Lakewood Chiropractor in Lakewood.
Helpful suggestions! For more, visit Wheat Ridge Asphalt Paving .
Appreciate the thorough insights. For more, visit trusted leak detection services .
In Charlotte? You need to recognise approximately Emergency Plumber Charlotte for all of your emergency plumbing desires!
I liked this article. For additional info, visit expert plumbers .
Flood damage in Temple Terrace can be overwhelming. It’s essential to act quickly for effective cleanup. Check out flood cleanup Temple Terrace for expert tips!
อยากรู้วิธีติดตั้งไฟหน้ารถ LED ทำเองได้ไหม? bt premium auto xenon สาขา ศรีนครินทร์
After experiencing major flooding last summer, I turned to %keyword% and it was incredibly helpful! flood damage restoration near me Clive IA
Exploring a range of nutritional habits viewed often followed inside dog communities offer alluring insights –Which tendencies stuck YOUR awareness these days relating to foodstuff choices made obtainable? https://qqpipi.com//index.php/Innovative_Pet_Tech_Gadgets_Every_Owner_Should_Consider
Flooding can lead to serious issues down the line. Get informed with the help of basement flood clean up in Council Bluffs !
Had my battery replaced by a mobile mechanic from Mobile Brake Repair – professional service all the way!
Appreciate the thorough insights. For more, visit quick trust a trader plumbing services .
Seeing former addicts prosper after finishing programs offers me hope knowing change truly occurs if one stays dedicated throughout each action taken along their respective courses towards sobriety eventually leading effective reintegration back into addiction treatment
Joining hands across diverse backgrounds brings hope & progress through shared aspirations—what better example than that set forth by “Tirangagames”!??### anykeyword### tiranga invite code 2757419478643
It’s refreshing to see a company like Olympia Roofing Company that prioritizes customer satisfaction. Thanks for sharing! Roofing Company
Your analysis of online vs. brick-and-mortar sales at 性虐 provided great clarity on current trends.
This was very enlightening. For more, visit kitchen sink drain .
If you are purchasing for an emergency plumber who cares, I exceptionally recommend giving Emergency Plumber Charlotte a name.
It is very important not only to treat the symptoms but also to address the root causes of why someone might develop an eating condition in the first location– holistic care works best! eating disorder treatment
This was very enlightening. For more, visit cheap plumber .
How do you remain inspired during the tough times of drug detox? I ‘d like to hear your thoughts– I have actually shared mine over on drug detox !
This was a wonderful post. Check out Open Wide La Jolla Dental for more.
Appreciate the comprehensive advice. For more, visit tai vua99 dễ dàng .
پروتئین وی ویسلی، یک مکمل با کیفیت بر پایه کنسانتره و ایزوله پروتئین آبپنیر است که به تأمین پروتئین مورد نیاز بدن، ساخت عضله، تقویت سیستم ایمنی و کاهش اشتها کمک میکند.
Thanks for the great information. More at bubet chơi tài xỉu .
This was quite helpful. For more, visit emergency plumber .
After my first visit to a Lakewood chiropractor, I felt immediate relief! Thinking of trying out Chiropractor Lakewood next.
Wow, this is such valuable information! I can’t wait to reach out to Olympia Roofing Company for my roofing needs! Olympia Roofing Company
I appreciated this article. For more, visit best cosmetic dentist .
A trustworthy emergency plumber is needed, extraordinarily in our discipline. Glad I came upon Emergency plumber Charlotte !
This was a wonderful post. Check out Commercial Refrigeration Repair Technician for more.
I’m intrigued by the idea of cold plunging but unsure if it’s worth the investment. What are some real-life experiences that can shed light on this? If you’re exploring options, check out my site for cold plunge tub near me to see what’s available! cold plunge facilities in my area
This was a wonderful post. Check out emergency blocked manholes for more.
This was quite informative. For more, visit HVAC Company Eagle Air Co .
Thanks for the clear breakdown. More info at Sink leaking .
Very helpful read. For similar content, visit wedding floral decor Long island .
อยากทราบว่ามีรุ่นไหนบ้างที่เหมาะสำหรับรถยนต์แต่ละประเภท ซ่อมไฟหน้ารถ
Thanks for the detailed guidance. More at Foot Hills Paving .
Thanks for the great information. More at quick underfloor heating repairs .
“My experience with an AZ public adjuster was life-changing—don’t hesitate to reach out!” google.com
Your commitment to educating potential buyers about different firearm types is commendable, as seen on 混蛋 .
I’m amazed by how much chiropractic care has helped my posture! Shoutout to Lakewood Car Accident Chiropractor in Lakewood for their incredible service!
Well done! Find more at local WC cistern specialists .
Thanks to Emergency Plumber Charlotte , my plumbing drawback became resolved within hours! Highly commended.
Wonderful tips! Discover more at professional plumber .
The psychological aspects behind cravings warrant much deeper exploration within conventional rehab frameworks!” # # anyKeyWord # drug rehab
The journey toward recovery needs bravery– it’s challenging but every action taken should have acknowledgment, no matter how small!. eating disorder treatment .
How do you deal with cravings during the alcohol detox phase? Let’s share techniques and support each other at alcohol detox !
Completing rehab appeared complicated scary possibility at first believed perhaps impossible something endeavor needed intense devotion persistence nevertheless immersed myself process surrounded helpful environment assisted caring educated professionals drug detox
So many resources available now for those dealing with floods—it’s comforting! Don’t miss out on info from flood damage restoration near me Temple Terrace .
The historical context you provided about gun legislation at zf really added depth to the conversation.
Sports have a unique way of bringing people together, and the Tiranga games exemplify that perfectly! tiranga invite code 2757419478643
Thanks for the comprehensive read. Find more at Sewer line replacement expert .
The resources you’ve provided are invaluable for those facing flood damage in Hawaiian Gardens! emergency flood cleanup in Hawaiian Gardens
Thanks for the great tips. Discover more at professional gas safety inspections .
“Clive residents must come together during these challenges; find ways to help each other via %%keyword%%!” flood cleaning services in Clive IA
This was beautifully organized. Discover more at expertise in cosmetic dental techniques .
If there’s one component I’ve found out raising puppies, it really is persistence—how imperative has staying power been all over YOUR event ? Join discussions on the topic of enlargement by using demanding situations right here ### anykeyword ### https://nova-wiki.win/index.php/Dog-Friendly_Recipes_You_Can_Make_at_Home_37574
Decreasing barriers to accessing outpatient services might alter lives; let’s push for more equitable services around this problem. # any Keyword ## addiction treatment
Quick tip: Always maintain the number of an Emergency Plumber Charlotte easy for plumbing emergencies!
Thanks for the insightful write-up. More like this at Water leak repair .
Valuable information! Find more at affordable local plumbing services .
I value how this blog highlights the significance of therapy in drug rehab– mental health matters! drug rehab
This is highly informative. Check out Climate Alignment for more.
I found your article on self-defense laws at 煞逼 to be very informative and timely!
Clean windows make such a difference in how I perceive my surroundings—thank you, Residential Window Cleaning !
This was a fantastic read. Check out Bozeman roofers for more.
I value resources that focus on both emotional and physical healing in eating disorder treatment. It’s a complicated problem! eating disorder treatment
Thanks for the helpful article. More like this at Electric showers Power Showers .
Your post reminded me that summer is right around the corner! Time to check if my AC unit is ready for the heat. Any recommendations for maintenance? Eagle Air Co Heating and Cooling
Let’s talk about how essential education plays role combating stigma associated mental disorder substance usage conditions advocating increased funding research study avoidance intervention programs developed equip households tools cope effectively manage drug detox
Many homeowners are unsure about how much they should expect to pay for plumbing services. It’s good to know the average costs and what influences those prices plumbing near me
Does someone know which dog breeds are hypoallergenic? I actually have hypersensitive reactions and desire some assist! https://www.alphabookmarks.win/getting-begun-with-discus
I found this very interesting. Check out foothills paving and maintenance for more.
Useful advice! For more, visit https://006.filmhd1080.icu/user/erforetjma .
This was highly informative. Check out casa rural for more.
Appreciate the helpful advice. For more, visit ferretería Albacete .
Thanks for the thorough analysis. More info at Open Wide La Jolla Dentist .
If you’re ever stuck with unfamiliar flooding or leaks, take into account that that # anyKeyWord# is just a call away! Emergency plumber Charlotte
Nicely detailed. Discover more at nutrióloga en Saltillo .
Appreciate the comprehensive advice. For more, visit flood restoration companies .
Does anyone know if Chiropractor Lakewood offers family plans for chiropractic care? I’m interested in bringing my kids!
Great tips on maintaining roofs; I’ll definitely reach out to Olympia Roofing Company based on your recommendations! Olympia Roofing Company
Exploring parks and trails with my canine brings me such happiness—the place do you are taking yours to play outdoor? Discuss destinations on Click to find out more .
สำหรับคนรักการดื่ม ต้องไปลองที่ OMG ONE MORE GLASS SAI1 สักครั้งนะคะ ร้านอาหารสาย1 เพลงเพราะ
This was very enlightening. For more, visit motor vehicle accident lawyer near me .
Thanks for the great information. More at hvac contractor .
Thanks for the thorough analysis. More info at local flood restoration companies .
Flood recovery takes time and effort; make sure you’re prepared with all the right info from sources like basement flood clean up in Temple Terrace !
Great post on troubleshooting common HVAC problems! For professional help, check out hvac installation .
Thanks for the clear breakdown. More info at Foothills Paving .
Do associates/household routinely ask “What breed suits MY life style terrific?” ;Have innovations equipped after discovering very well before advising prospective long term vendors? https://speedy-wiki.win/index.php/How_to_Prepare_Your_Home_for_a_New_Puppy_Arrival_51169
Helpful suggestions! For more, visit reliable plumbing .
Each comment shared really sheds light on diverse experiences; let’s continue supporting one another throughout recovery processes! emergency flood cleanup in las colinas
Thanks for the clear advice. More at tài xỉu vua99 uy tín .
The market trends discussed at 伦理电影 are fascinating! It’s interesting to see how consumer preferences evolve.
I’m grateful for the contributions made by various authors featured on your site; they bring unique insights to discussions about guns. 朱镕基
This was highly useful. For more, visit https://27vlz.ru/user/marielxvtv .
Appreciate the thorough information. For more, visit WC Cisterns Syphon .
This was highly educational. More at casas rurales Arzúa .
The final time I vital urgent plumbing guide, # anyKeyWord# became there for me accurate away! Emergency Plumber Charlotte
Very informative article. For similar content, visit ferretería .
Nicely detailed. Discover more at https://lockdowntheatre.net/user/allachrqhq .
Being proactive in preference to reactive in the case of safety is integral—and your methods lend a hand gain that!!! ##anythingKeywords ## Have a peek here
This was very enlightening. For more, visit WC Cisterns Syphon .
Mindfulness and meditation can play a considerable role in healing from addiction. Have you tried it? addiction treatment